Case Scenario
Mr. H is an 84-year-old man with well-controlled hypertension and hyperlipidemia. He recently presented to the emergency department with anxiety symptoms, shortness of breath, and palpitations. A clinical examination found an irregular heart rhythm of 140 to 160 beats per minute. An electrocardiogram (ECG) showed atrial fibrillation with no acute ST-T wave changes. After Mr. H received an intravenous dose of a beta blocker, his heart rate quickly decreased to the 80s, and his symptoms resolved. However, a repeat ECG showed that he was in atrial fibrillation. He was admitted for telemetry monitoring, and an oral beta blocker and intravenous heparin were initiated. Laboratory tests showed no evidence of ischemia, anemia, electrolyte imbalance, or thyroid dysfunction. An echocardiogram showed calcification of the aortic and mitral valves but no stenosis or significant regurgitation. A cardiologist recommended prescribing a direct oral anticoagulant to prevent an embolic stroke. However, Mr. H’s primary care physician is concerned about the risks of anticoagulation because of recent functional decline in the patient, including a slowing of his gait without any falls.
Clinical Commentary
Atrial fibrillation is the most common cardiac arrhythmia, occurring in an estimated 2.7 million to 6.1 million people in the United States.1 Approximately 9% of people 65 years and older have this condition, and it occurs more often in men.2 [corrected] Risk factors include hypertension, diabetes mellitus, ischemic heart disease, and older age. Each year atrial fibrillation causes more than 750,000 hospital admissions and more than 130,000 deaths, often associated with strokes.3 An estimated 15% to 20% of strokes occur in patients with underlying atrial fibrillation.4,5
The use of warfarin (Coumadin) and direct oral anticoagulants such as rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa) to prevent strokes is the first-line treatment for younger patients with atrial fibrillation. However, the use of direct oral anticoagulants in older people is problematic because of a higher risk of morbidity and mortality from gastrointestinal and intracerebral bleeding, which can be exacerbated by falls.
Practice guidelines recommend risk stratification with the CHA2DS2-VASc tool (congestive heart failure; hypertension; age 75 years or older [doubled]; diabetes mellitus; prior stroke, transient ischemic attack, or thromboembolism [doubled]; vascular disease; age 65 to 74 years; sex category; https://www.mdcalc.com/cha2ds2-vasc-score-atrial-fibrillation-stroke-risk) to identify patients who could benefit from anticoagulation therapy; however, there is a modest predictive ability for ischemic stroke.6–8 Some physicians use the CHA2DS2-VASc tool to determine whether to initiate anticoagulation therapy without considering the patient’s functional status and bleeding risk, which is not recommended. Bleeding risk scores such as HAS-BLED (hypertension, abnormal renal and liver function, stroke history, bleeding risk, labile international normalized ratio, elderly [older than 65 years], drugs and alcohol use; https://www.mdcalc.com/has-bled-score-major-bleeding-risk) may help assess risk but have limited predictive power.
A 2007 Cochrane review evaluated high-quality placebo-controlled studies comparing the benefits and risks of anticoagulation in atrial fibrillation. Participants were younger (average age 69 years) and had less comorbidity than the general population. After two years, patients taking warfarin experienced 17 out of 1,000 fewer strokes (number needed to treat [NNT] = 59) and five out of 1,000 fewer disabling or fatal strokes (NNT = 200). This distinction is essential because most studies assess only the reduction of all strokes, some of which are mild or quickly resolve. Compared with those who received placebo, participants who were treated with warfarin experienced 40 out of 1,000 more severe bleeds (number needed to harm [NNH] = 25), six of which were fatal, and six out of 1,000 more developed hemorrhagic strokes (NNH = 83 for fatal bleeds and hemorrhagic strokes combined). There was no difference in all-cause mortality.9
Few older people are included in randomized controlled trials of anticoagulation; therefore, there are limited data about risks in this population.10,11 A 2018 cohort study examined the risks and benefits of anticoagulation in people 90 years and older. Fifteen out of 1,000 averted strokes with anticoagulation therapy (NNT = 67), and the rate of averting a stroke was similar between warfarin and direct oral anticoagulants. In the direct oral anticoagulant arm, four out of 1,000 had a hemorrhagic stroke vs. 16 out of 1,000 in the warfarin arm. In each group using anticoagulation therapy, approximately 60 out of 1,000 participants had major bleeds.12
It is unclear how often older people with comorbidities that would increase the risk of bleeding (e.g., prior bleeding events, prior reactions to anticoagulation, falls, use of antiplatelet agents) are included in anticoagulation trials. Results of studies evaluating the effect of these factors are inconsistent; therefore, clinicians must use their judgment about benefits and risks in this population.13 One study of patients who fall often found that patients taking anticoagulants had a similar rate of bleeding as patients not taking anticoagulants; however, patients who did bleed had a higher rate of death if they were taking anticoagulants (146 out of 1,000 excess deaths; NNH = 7).14 It is important to know how well an older patient can tolerate warfarin and whether they can take medication consistently because these factors will affect possible harms.
TAKE-HOME MESSAGES FOR RIGHT CARE

| Risk stratification is essential to identify patients who may benefit the most from anticoagulation therapy. |
| Evaluate comorbidities, medication use, risk of falls, and risk of bleeding for evidence-based decision-making. |
| Patient-centered, shared decision-making discussions between the physician and patient are essential to evaluate the benefits and risks of anticoagulation. |
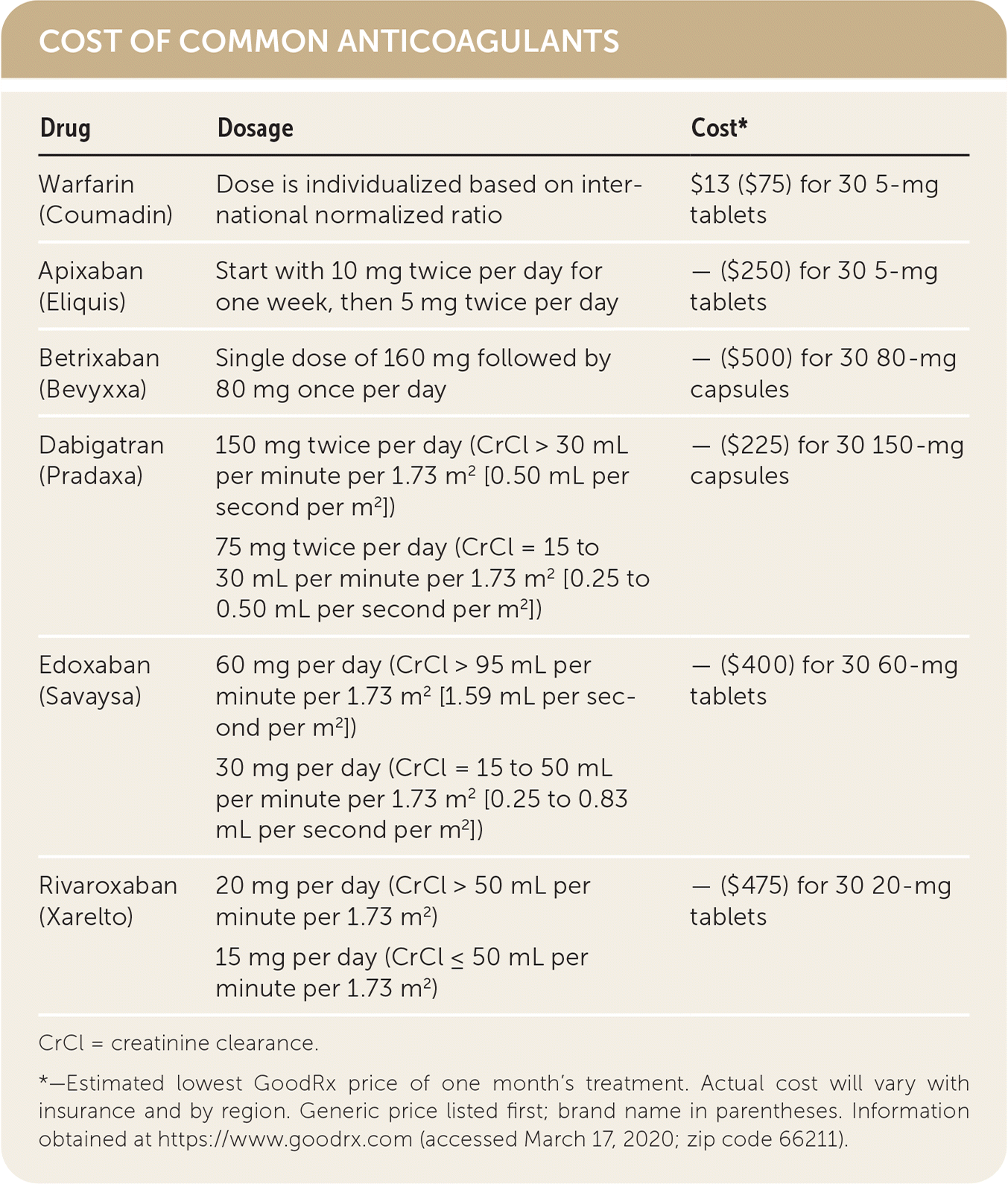
COST OF COMMON ANTICOAGULANTS
| Drug | Dosage | Cost* |
|---|---|---|
| Warfarin (Coumadin) | Dose is individualized based on international normalized ratio | $13 ($75) for 30 5-mg tablets |
| Apixaban (Eliquis) | Start with 10 mg twice per day for one week, then 5 mg twice per day | — ($250) for 30 5-mg tablets |
| Betrixaban (Bevyxxa) | Single dose of 160 mg followed by 80 mg once per day | — ($500) for 30 80-mg capsules |
| Dabigatran (Pradaxa) | 150 mg twice per day (CrCl > 30 mL per minute per 1.73 m2 [0.50 mL per second per m2]) 75 mg twice per day (CrCl = 15 to 30 mL per minute per 1.73 m2 [0.25 to 0.50 mL per second per m2]) | — ($225) for 30 150-mg capsules |
| Edoxaban (Savaysa) | 60 mg per day (CrCl > 95 mL per minute per 1.73 m2 [1.59 mL per second per m2]) 30 mg per day (CrCl = 15 to 50 mL per minute per 1.73 m2 [0.25 to 0.83 mL per second per m2]) | — ($400) for 30 60-mg tablets |
| Rivaroxaban (Xarelto) | 20 mg per day (CrCl > 50 mL per minute per 1.73 m2) 15 mg per day (CrCl ≤ 50 mL per minute per 1.73 m2) | — ($475) for 30 20-mg tablets |
CrCl = creatinine clearance.
*—Estimated lowest GoodRx price of one month’s treatment. Actual cost will vary with insurance and by region. Generic price listed first; brand name in parentheses. Information obtained at https://www.goodrx.com (accessed March 17, 2020; zip code 66211).
Studies have shown that direct oral anticoagulants are at least as effective as warfarin.11 Comparative risks of bleeding complications are mixed, with some studies showing decreased rates of intracerebral hemorrhage and others showing a slightly increased risk of gastrointestinal bleeding in patients taking direct oral anticoagulants.15–21 When necessary, vitamin K can be used to reverse the effects of warfarin. Two medications are U.S. Food and Drug Administration–approved for reversing the effects of direct oral anticoagulants in patients who experience life-threatening bleeding or require emergency surgery. Andexanet alfa (Andexxa) should be used for patients taking apixaban, rivaroxaban, or edoxaban (Savaysa). Idarucizumab (Praxbind) should be used for patients taking dabigatran.22
Patient Perspective
Members of the public are often concerned about the risk of bleeding from anticoagulants by observing the experiences of those around them. Shared decision-making after discussing the pros and cons of different options is essential in a situation in which the answers are not always clear. Patients should be made aware of data that compare the benefits and risks of anticoagulation therapy. The physician should also be prepared to discuss nonpharmacologic strategies or strategies that the patient may have learned about on the internet, such as dietary changes or magnesium supplementation. Also, detailed discussions of the incidence of stroke vs. bleeding or overall mortality are not likely to be readily available online. The same is true of the risks inherent in a bleeding episode and the differences between anticoagulants. What are the benefits of monitored vs. unmonitored anticoagulation? What sort of events (e.g., a fall) can precipitate bleeding? How safe is surgery for a patient taking anticoagulants, and how safe and effective is reversal of the anticoagulant? Even informed patients need an objective and trusted professional to filter and explain their options, keeping in mind that important uncertainties exist.
Primary care physicians can help bridge the gap between theory and reality by conveying a thoughtful assessment of possible outcomes and preventive measures. The pressure to administer anticoagulants to large subpopulations of patients assumes that what is good for the majority is good for all and that reducing a single risk will reduce a patient’s overall risk. The goal of patients is their global well-being, a goal that does not necessarily align with the optimal end point for each of their medical conditions. It is the fundamental role of the primary care physician to balance these conflicting concerns.
Resolution of Case
Mr. H has a CHA2DS8%2-VASc score of 3 because of his hypertension (one point) and age older than 75 years (two points), indicating a high risk of stroke.6 Mr. H and his primary care physician had a shared decision-making conversation. Mr. H has a 3.2% annual risk of stroke, with less than one-half of that being a risk of a disabling or fatal stroke.1,2,9,12 [corrected] They discussed the costs of medications and potential adverse effects and the need for laboratory testing with warfarin. They also considered his age and recent functional decline, which, if complicated by a fall, could result in severe intracranial bleeding. Together they decided that Mr. H would continue to take the beta blocker to control his heart rate, and he would abstain from anticoagulation therapy and consider taking a daily aspirin as an alternative.

