In 2018, approximately 2.8 million passengers flew in and out of U.S. airports per day. Twenty-four to 130 in-flight medical emergencies are estimated to occur per 1 million passengers; however, there is no internationally agreed-upon recording or classification system. Up to 70% of in-flight emergencies are managed by the cabin crew without additional assistance. If a health care volunteer is requested, medical professionals should consider if they are in an appropriate condition to render aid, and then identify themselves to cabin crew, perform a history and physical examination, and inform the cabin crew of clinical impressions and recommendations. An aircraft in flight is a physically constrained and resource-limited environment. When needed, an emergency medical kit and automated external defibrillator are available on all U.S. aircraft with at least one flight attendant and a capacity for 30 or more passengers. Coordinated communication with the pilot, any available ground-based medical resources, and flight dispatch is needed if aircraft diversion is recommended. In the United States, medical volunteers are generally protected by the Aviation Medical Assistance Act of 1998. There is no equivalent law governing international travel, and legal jurisdiction depends on the patient's and medical professional's countries of citizenship and the country in which the aircraft is registered.
Approximately 2.8 million passengers flew in and out of U.S. airports per day in 2018.1 An overhead announcement requesting medical assistance at cruising altitude presents a unique situation for any health care professional given the physically constrained, resource-limited environment. The term “in-flight medical event” is often used interchangeably with “in-flight medical emergency” and includes a spectrum of conditions, ranging from minor to serious.2 There is no internationally agreed-upon recording and classification system for in-flight medical emergencies, and prevalence estimates vary between 24 and 130 emergencies per 1 million passengers.3–5
SORT: KEY RECOMMENDATIONS FOR PRACTICE
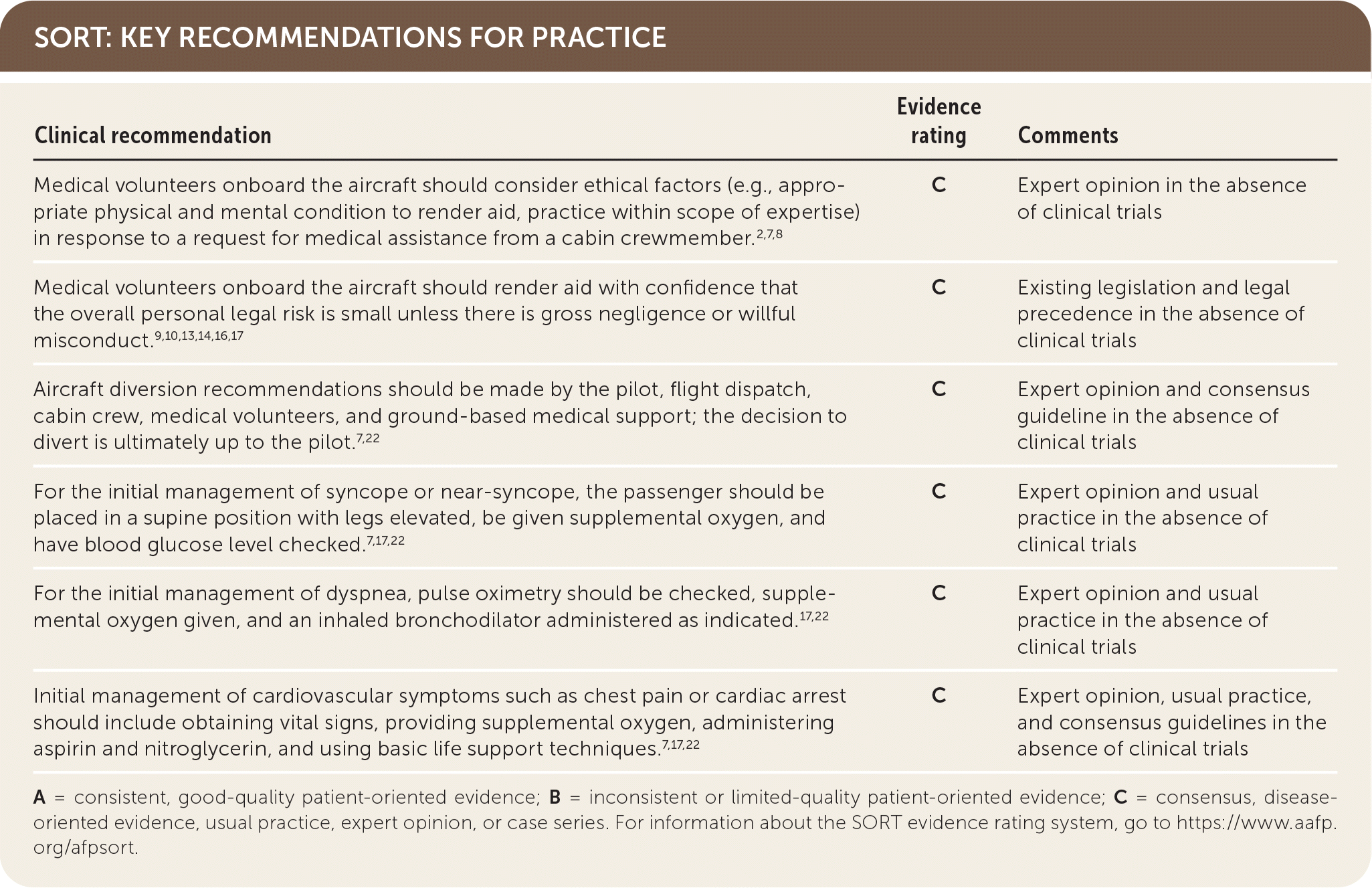
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
In-flight Medical Emergency Basics
Up to 65% to 70% of in-flight medical emergencies are managed by a cabin crew without the assistance of a health care professional.3,6 Crewmembers are trained in individual airline operating protocols, cardiopulmonary resuscitation (CPR), and the use of emergency and lifesaving equipment (e.g., automated external defibrillators [AEDs]) carried onboard.2 If a crewmember requests assistance from a volunteer medical professional, the volunteer should first consider if he or she is in a suitable condition to render aid (e.g., no recent use of alcohol or sleep aids, not fatigued).2 Table 1 summarizes a general approach to in-flight emergencies for volunteer medical professionals.2,7,8 Volunteers should understand that an aircraft in flight is a medically austere environment. For example, aircraft noise may render a stethoscope ineffective for auscultating a manual blood pressure; alternative systolic blood pressure can be measured by the first palpable radial pulse when slowly releasing the pressure in the sphygmomanometer.7
TABLE 1. In-flight Medical Emergency Treatment Approach for Volunteer Medical Professionals

| Identify yourself and state your medical qualifications. The airline may require proof of credentials (e.g., business card, licensure documents). |
| Perform as much of a complete history as possible. |
| This may require an interpreter, involvement from family members, or other nearby passengers. |
| Identify high-risk symptoms (e.g., chest pain, shortness of breath, focal neurologic deficits). |
| Obtain vital signs and perform an appropriate physical examination. |
| Inform the cabin crew of your clinical impression and recommendations. |
| Initiate ground-based consultation if not already initiated by the flight crew. |
| The airline may require consultation before using the emergency medical kit. |
| Aircraft diversion and ground-based medical assistance require coordination with the ground-based consultant and pilot. |
| Administer supplemental oxygen or use an automated external defibrillator as indicated. |
| Document the clinical presentation and care rendered; the airline may have specific forms to complete. |
Note: Do not attempt to practice beyond your level of expertise, but remember that your assistance is valuable and better than that of a nonmedical professional.
Physicians assist in 46% to 48% of in-flight medical emergency requests6,7; other skilled medical professionals who respond include nurses (20.1%) and emergency medical services personnel (4.4%).7 Medical volunteers are generally protected when providing medical care during an in-flight medical emergency on U.S. commercial aircraft by the Aviation Medical Assistance Act of 1998, which releases volunteers from liability unless there is gross negligence or willful misconduct.9 There is no equivalent law governing international travel; legal jurisdiction depends on the patient's and volunteer's countries of citizenship and the country in which the aircraft is registered.8,10–13 The United States, England, and Canada do not mandate physicians to render emergency medical services in flight,13–15 but a legal obligation to assist exists in Australia and many other European countries.10,14 Experts in aviation medicine support the use of medical volunteers for in-flight medical emergencies because the overall personal legal risk is small.16,17 There has yet to be a U.S. case heard in court against a physician-passenger providing medical care during an in-flight medical emergency.10,14
Onboard Medical Equipment
The Federal Aviation Administration (FAA) has mandated that certain medical supplies be available on U.S. commercial aircraft (Table 2)18; similarly, the European Union Aviation Safety Agency and International Civil Aviation Organization have established minimum recommendations for emergency medical kit contents.18–20 The FAA requires an AED on aircraft with at least one flight attendant and a capacity for 30 or more passengers.18 No such mandate exists for European airlines; however, many carry an AED onboard.21 Non-U.S. airlines may carry additional controlled substances for analgesia and sedation.19,21 Some U.S. and international airlines have opted to expand their emergency medical kits with additional medications or equipment (Table 3).19,22 If the desired item is not available in the kit, the flight crew can make an overhead announcement requesting the item from other passengers.
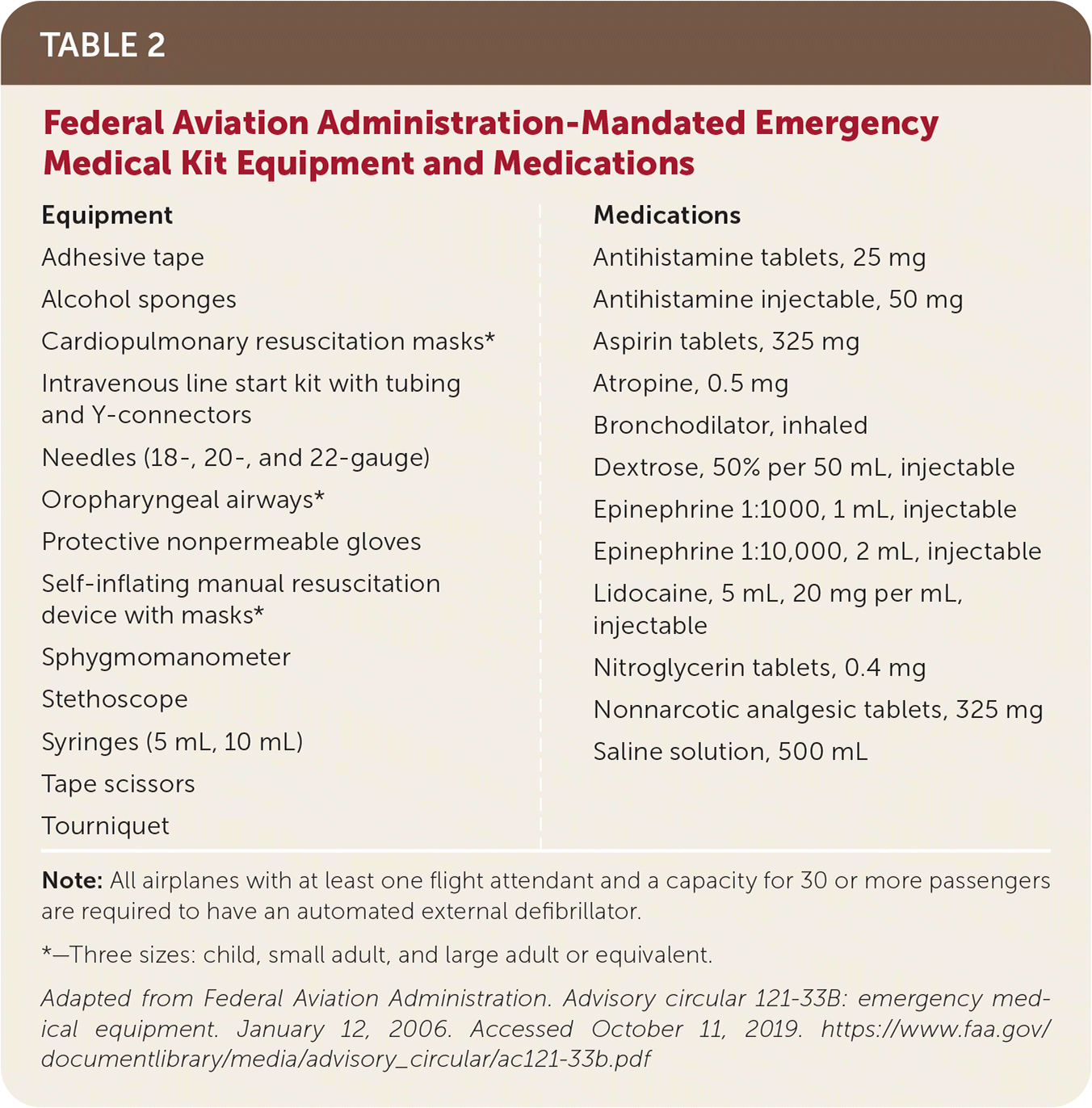
TABLE 2. Federal Aviation Administration-Mandated Emergency Medical Kit Equipment and Medications
| Equipment | |
|---|---|
| Adhesive tape Alcohol sponges Cardiopulmonary resuscitation masks* Intravenous line start kit with tubing and Y-connectors Needles (18-, 20-, and 22-gauge) Oropharyngeal airways* Protective nonpermeable gloves Self-inflating manual resuscitation device with masks* Sphygmomanometer Stethoscope Syringes (5 mL, 10 mL) Tape scissors Tourniquet | |
| Medications | |
| Antihistamine tablets, 25 mg Antihistamine injectable, 50 mg Aspirin tablets, 325 mg Atropine, 0.5 mg Bronchodilator, inhaled Dextrose, 50% per 50 mL, injectable Epinephrine 1: 1000, 1 mL, injectable Epinephrine 1: 10,000, 2 mL, injectable Lidocaine, 5 mL, 20 mg per mL, injectable Nitroglycerin tablets, 0.4 mg Nonnarcotic analgesic tablets, 325 mg Saline solution, 500 mL |
Note: All airplanes with at least one flight attendant and a capacity for 30 or more passengers are required to have an automated external defibrillator.
*—Three sizes: child, small adult, and large adult or equivalent.
Adapted from Federal Aviation Administration. Advisory circular 121-33B: emergency medical equipment. January 12, 2006. Accessed October 11, 2019. https://www.faa.gov/documentlibrary/media/advisory_circular/ac121-33b.pdf
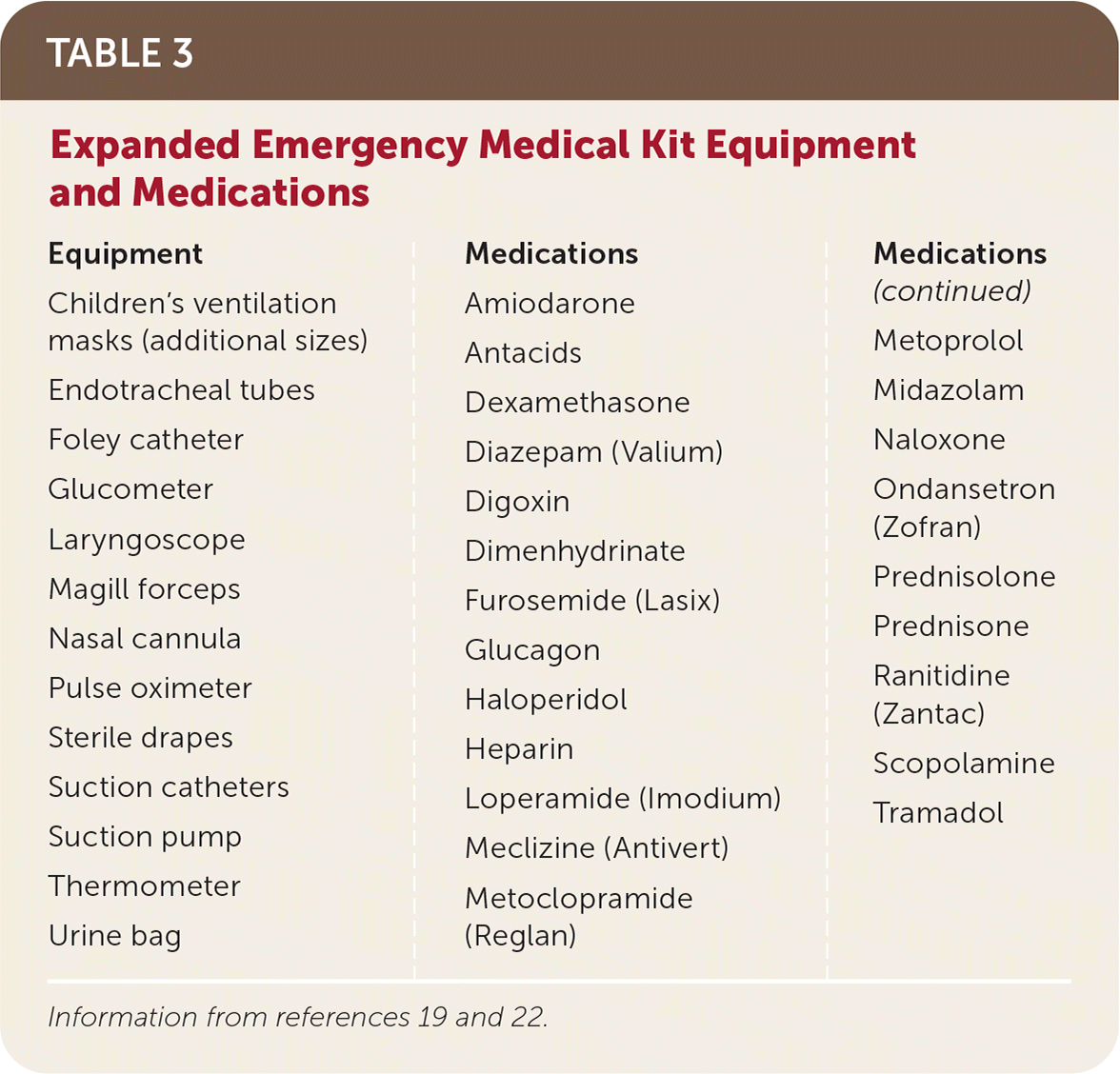
TABLE 3. Expanded Emergency Medical Kit Equipment and Medications
| Equipment | ||
|---|---|---|
| Children's ventilation masks (additional sizes) Endotracheal tubes Foley catheter Glucometer Laryngoscope Magill forceps Nasal cannula Pulse oximeter Sterile drapes Suction catheters Suction pump Thermometer Urine bag | ||
| Medications | ||
| Amiodarone Antacids Dexamethasone Diazepam (Valium) Digoxin Dimenhydrinate Furosemide (Lasix) Glucagon Haloperidol Heparin Loperamide (Imodium) Meclizine (Antivert) Metoclopramide (Reglan) Metoprolol Midazolam Naloxone Ondansetron (Zofran) Prednisolone Prednisone Ranitidine (Zantac) Scopolamine Tramadol |
An anonymous survey of 12 European airlines that included full-service and low-cost carriers demonstrated a high degree of variability in emergency medical kit contents. None of the kits complied with International Civil Aviation Organization recommendations; two were found to be insufficiently equipped for in-flight medical emergencies requiring acute care.23 Medical volunteers should know that these kits generally are designed for adults and may not have basic airway equipment and medication dosing for children.24 Multiple medical organizations, including the International Academy of Aviation and Space Medicine, American Osteopathic Association, American College of Emergency Physicians, and American Medical Association have requested the addition of pulse oximeters, naloxone, antiemetics, and sedatives among other items.21 However, the FAA-mandated emergency medical kit is usually sufficient for initiating treatment for most in-flight medical emergencies.7
Ground-Based Medical Resources
The FAA does not require in-flight consultation with ground-based medical support, but many airlines contract with a third party to help manage medical emergencies.6,7 The pilot is notified by a crewmember when a medical emergency occurs. The pilot then establishes contact with the ground-based medical group and the airline operations center to determine the best course of action. Board-certified emergency physicians typically staff ground-based groups and have additional training in aviation and telemedicine.7,8 Crewmembers are often required to contact ground-based medical support before using the emergency medical kit.7 Communication is paramount because of the challenges of radio interference and indirect patient contact. Ground-based medical resources are involved in approximately 16 in-flight medical emergencies per 1 million passengers.7 There are no current studies on the effect of ground-based medical support on patient outcomes.22
Aircraft Diversion
Approximately 4% to 7% of in-flight medical emergencies result in aircraft diversion, with the most common reasons being cardiac arrest (57.9%), cardiac symptoms (18.4%), obstetric emergencies (18.0%), and possible stroke (16.4%).7,22 The decision to divert an aircraft is made by the pilot in conjunction with flight dispatch and recommendations from the cabin crew, medical volunteers, and ground-based medical support. Factors include patient preference (or by proxy a family member), weather, fuel load, airport capabilities, and proximity of medical resources to specific airports.7,22
Considerations for Specific Conditions
SYNCOPE
A review of 49,000 in-flight medical emergencies found syncope or near-syncope to be the most common emergency category with a prevalence of 32.7%.22 Patients often have initial mild bradycardia and hypotension, and may appear ill, pale, diaphoretic, or have a slightly altered mental status. The passenger should be placed in a supine or Trendelenburg position, which may require movement of the passenger into an aisle or galley with the legs elevated on a seat.7 Providing supplemental oxygen should be considered, and the patient's blood glucose level should be obtained with a finger stick device if available.17 If the passenger does not recover within 15 to 30 minutes of initial interventions, contacting ground-based medical support and recommending an aircraft diversion should be considered because of more serious causes for loss of consciousness such as acute coronary syndrome, arrhythmia, hypoxia, pulmonary embolism or thrombosis, and stroke.22 Patients with persistent hypotension may need intravenous fluids if oral intake is not tolerated.
DYSPNEA
Dyspnea accounts for 10.1% of in-flight medical emergencies.22 Cabin pressure is inversely proportional to the altitude of the aircraft, and aircraft cabins are not pressurized to sea level equivalent. Although the barometric pressure at sea level corresponds to an arterial oxygen pressure of 95 to 98 mm Hg, the barometric pressure at 8,000 ft (2,438 m) results in an arterial oxygen pressure of 55 to 56 mm Hg and a corresponding blood oxygen saturation of 90%.8,25 Most healthy travelers can compensate for this degree of hypoxemia; passengers with known hypoxemia (i.e., resting oxygen saturation less than 92% at sea level) are advised to travel with portable oxygen.17 Causes for dyspnea include asthma or chronic obstructive pulmonary disease, allergic reaction, pneumonia, pneumothorax, pulmonary embolism or thrombosis, and toxic exposure.22 In a passenger with dyspnea, pulse oximetry level should be obtained, and supplemental oxygen administered if oxygen saturation is less than 95%. If a passenger uses 4 L per minute of supplemental oxygen or more on the ground, the onboard oxygen supply may not be sufficient to reverse hypoxia; therefore, aircraft diversion may be required.22 Bronchodilators are available in emergency medical kits and should be administered for bronchospasm. If the patient does not improve, ground-based medical support should provide additional recommendations about the best use of available medical resources given airline operational concerns.7
CHEST PAIN
Chest pain or other cardiovascular symptoms have a prevalence of 7% of in-flight medical emergencies and can be secondary to acute coronary syndrome, anxiety, aortic dissection, musculoskeletal pain, or pulmonary causes such as pulmonary embolus, bronchospasm, or pneumothorax.22 Dyspepsia is often a diagnosis of exclusion. Cardiac arrests are reported separately with a prevalence of 0.2% of in-flight medical emergencies but account for up to 86% of emergencies that result in death.7,22 The initial assessment should include performing a focused cardiovascular history and obtaining vital signs. If acute coronary syndrome is suspected, aspirin and nitroglycerin are typically included in FAA-mandated emergency medical kits. Chest pain that subsides with basic interventions is not usually caused by an acute ST-segment elevation myocardial infarction, aortic dissection, or pulmonary embolism warranting diversion; however, the passenger should be offered transport to a hospital by emergency service personnel on landing.17
For a patient with suspected cardiac arrest (i.e., unresponsive, not breathing or agonal gasps, no pulse), the pilot and ground-based medical support should be notified and basic life support initiated, including high-quality CPR and use of an AED. Most aircraft will not have the capability to perform 12-lead electrocardiography. Epinephrine and lidocaine are available in emergency medical kits for volunteers comfortable with advanced life support algorithms and can be administered per ground-based medical support recommendations. CPR should be continued until one of the following occurs: return of spontaneous circulation; it becomes unsafe to continue CPR; all rescuers are too exhausted to continue; the aircraft has landed, and care is transferred to the ground-support medical team; or the patient is presumed dead (i.e., CPR has been maintained for 30 minutes or longer with no signs of life within this period and no shocks advised by the AED).26
OTHER NEUROLOGIC CONDITIONS
Other neurologic conditions make up approximately 5.5% of in-flight medical emergencies, which include strokes and seizures.22 Stroke evaluations should focus on the timing of onset, focal neurologic deficits, and other associated symptoms such as headache. Supplemental oxygen should be initiated to limit further neurologic injury. Although aspirin is available in the emergency medical kit, it should not be given when a stroke is considered because hemorrhagic and ischemic strokes are indistinguishable without radiography.17 A suspected acute stroke should prompt a recommendation for diversion; differential diagnoses include complex migraine and intracranial mass.22 Seizure thresholds are potentially lowered by in-flight hypoxemia and disturbances in passengers' circadian rhythms.17 For a possible seizure, identifying symptoms include event onset, duration, quality of movements, and loss of bowel or bladder function. If the seizure resolves and the patient regains normal mental status, diversion is not usually necessary. Giving an oral benzodiazepine, if available, or an additional dose of the patient's antiepileptic medication if the patient has a history of seizures should be considered. Multiple, ongoing seizures or failure to recover from a postictal state should prompt continued monitoring of the passenger's airway, breathing, and circulation with a recommendation for aircraft diversion.22 Parenteral benzodiazepines are not usually available on U.S. commercial aircraft.
TRAUMATIC INJURIES
Traumatic injuries make up 4.8% of in-flight medical emergencies.22 Most injuries are minor, such as from shifting luggage, falls, or burns from hot liquids, but patient-specific factors such as age and use of anticoagulants need to be considered.17 The passenger should be assessed for loss of consciousness or other neurologic symptoms, bleeding, open wounds, or deformities. Bleeding can be controlled by direct pressure and elevation; however, if there is ongoing heavy extremity bleeding, consider applying a tourniquet. If a fracture or dislocation is suspected, a splint may need to be improvised from materials available on the aircraft.17
PSYCHIATRIC SYMPTOMS
Anxiety or agitation and psychosis account for 3% of in-flight medical emergencies.22 Stressors such as lengthy check-in processes, enhanced security measures, delayed flights, cramped cabins, and alcohol consumption can exacerbate underlying psychiatric disorders such as panic disorder or posttraumatic stress disorder.17 Other causes include the misuse of or withdrawal from substances such as opioids, benzodiazepines, or stimulants. Care must be taken to consider organic pathology, because symptoms (e.g., chest pain, dyspnea) may overlap. Verbal calming techniques and establishing rapport should be the first-line treatment. If ineffective, the flight crew should provide individual airline security protocols, which take precedence over attempts at medical management.22 Security protocols may include restraining the passenger or diverting the aircraft for the safety of other passengers and crew. The FAA-mandated emergency medical kit has few medications that can treat agitation, reverse substance intoxication, or aid withdrawal such as benzodiazepines, naloxone, or antiemetic therapy.
ALLERGIC REACTIONS
Allergic reactions have a prevalence of 1.6% of in-flight medical emergencies, most commonly to food (e.g., peanuts, tree nuts) but may include exposure to traveling animals or other environmental allergens.22 Reactions can range from localized hives to anaphylaxis. Treatments available in emergency medical kits include antihistamines (oral or injectable) and epinephrine. When possible, the exposure should be removed.
OBSTETRIC EMERGENCIES
Obstetric emergencies are a small proportion of overall in-flight medical emergencies with a prevalence of 0.7%. However, they are the third most common emergency resulting in aircraft diversion and the second most common emergency resulting in hospital admission.6,22 A focused history includes determining the gestational age, presence of multiple gestations, pregnancy complications, and presence and quality of abdominal or pelvic pain. Physical examination should include vital signs and assessing for any vaginal bleeding, duration, and severity. If vaginal bleeding is less than one pad per hour or the patient has not reached 20 weeks' gestation, consider expectant management and coordination of emergency medical services on arrival. If the patient is past 20 weeks' gestation and there is ongoing or severe vaginal bleeding or abdominal pain, aircraft diversion is recommended, because the differential diagnosis includes active labor, spontaneous abortion, preeclampsia or eclampsia, and placental abruption.22 Intravenous fluids are indicated if there is a concern for hemorrhagic shock.
Data Sources: A PubMed search was completed using the following key terms: in-flight medical emergencies, legal implications of flight medical emergencies, in-flight emergency medical kits, and medical issues in flight. Pertinent United States, European, and international aviation guidelines were also reviewed. Search dates: September through November 2019, and July 2020.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as the official policy or position of the U.S. Army, the Department of Defense, or the U.S. government.

