The preparticipation physical evaluation (PPE) is a common reason for young athletes to see a primary care physician. An annual PPE is required by most state high school athletic associations for participation in school-based sports, although there is limited evidence to support its effectiveness for detecting conditions that predispose athletes to injury or illness. In 2019, the American Academy of Pediatrics, with representatives from the American Academy of Family Physicians and other organizations, published updated PPE recommendations (PPE5). According to the guideline, the general goals of the PPE are determining general physical and psychological health; evaluating for life-threatening or disabling conditions, including risk of sudden cardiac arrest and other conditions that may predispose the athlete to illness or injury; and serving as an entry point into the health care system for those without a medical home or primary care physician. The guideline recommends that the evaluation take place in the physician's office rather than in a group setting. The PPE should include a structured physical examination that focuses on the cardiovascular, musculoskeletal, and neurologic systems. Screening for depression, anxiety disorders, and attention-deficit/hyperactivity disorder is also recommended. Clinicians should recognize any findings suggestive of the relative energy deficiency in sport syndrome. Additional consideration is required to address the needs and concerns of transgender athletes and athletes with physical and intellectual disabilities. Finally, guidelines have been published regarding return to play for athletes who have had COVID-19.
Approximately 60 million children and adolescents, including 7.9 million high school students, participate in some form of sports in the United States.1,2 The preparticipation physical evaluation (PPE) has long been used to determine medical eligibility for youth sports in the United States, with the first PPE recommendations published in 1992 by a task force of five physician organizations.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
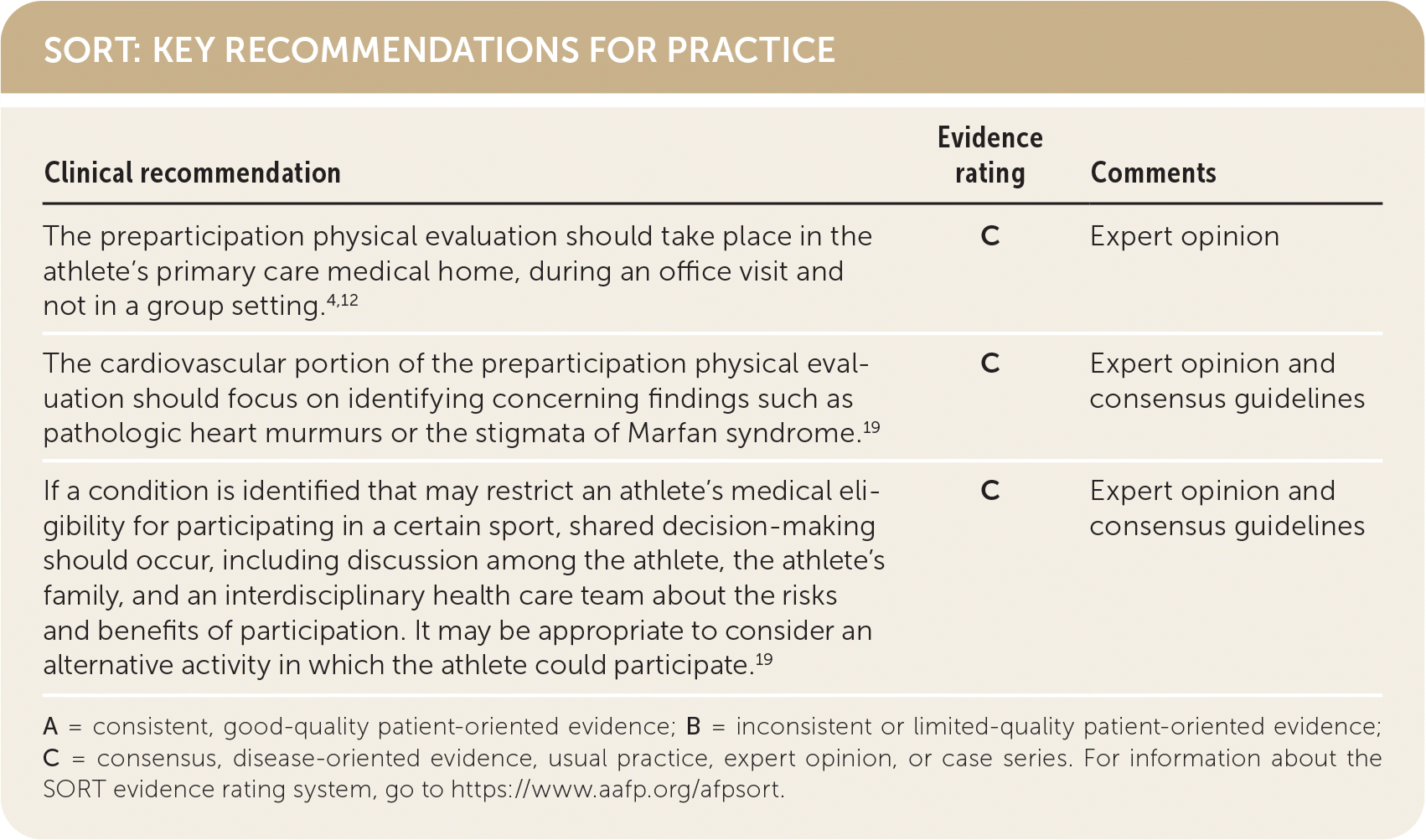
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN PREVENTIVE MEDICINE

| Recommendation | Sponsoring organization |
|---|---|
| Do not order annual electrocardiography or any other cardiac screening for asymptomatic, low-risk patients. | American Academy of Family Physicians and American College of Physicians |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
The intent of the PPE is to promote the health and safety of young athletes participating in training and competition and to identify those who may need additional evaluation before participation or, rarely, exclusion from sports. The American Academy of Pediatrics has published the fifth edition of the most comprehensive, up-to-date guideline on the PPE, referred to as PPE5.4 It contains consensus recommendations from representatives of multiple stakeholder medical societies, including the American Academy of Family Physicians, American Academy of Pediatrics, American College of Sports Medicine, American Medical Society for Sports Medicine, American Orthopaedic Society for Sports Medicine, and American Osteopathic Academy of Sports Medicine.4 In addition to information about physical examinations, the PPE5 contains new recommendations regarding mental health in athletes. It also addresses the specific needs of certain groups, including athletes experiencing relative energy deficiency, transgender athletes, and athletes with disabilities.4
Controversies and Concerns
A long-standing debate has surrounded the use of the PPE. This is primarily because there is limited evidence to support its effectiveness for detecting conditions that predispose athletes to injury or illness.5,6
Another concern is that requiring a PPE may be a barrier to sports participation, especially in socioeconomically or medically disadvantaged communities in which PPEs may not be readily available.4 Even for individuals with medical insurance, PPEs may be an out-of-pocket expense (Z02.5 is the current International Classification of Diseases [ICD] code for a sports-related PPE7). Billing for the PPE as though it is a routine health maintenance visit may allow for coverage; however, doing so may preclude additional covered preventive visits for the patient during the calendar year. It may also be difficult to incorporate a PPE into a routine wellness visit because of time limitations, lack of a standardized approach, and gaps in physician knowledge related to appropriate questions and recommended examinations.8
Despite these ongoing debates, PPEs are widely performed. The Special Olympics requires a PPE for all athletes before participation.4 PPEs are recommended by the National Federation of State High School Associations and the National Collegiate Athletic Association.9,10 Most state high school athletic associations require an annual PPE for participation in school-based athletics11; however, the PPE5 recommends a full evaluation every two to three years with annual updates only as needed to address potential areas of concern.4 Clinicians should be aware of their own state's recommendations regarding the required frequency of PPEs.4
General Goals and Recommendations
The general goals of a PPE are determining the general physical and psychological health of the athlete; evaluating for life-threatening or disabling conditions, including risk of sudden cardiac arrest and other conditions that may predispose the athlete to illness or injury; and serving as an entry point into the health care system for those without a medical home or primary care physician.4
The PPE5 and the American Academy of Family Physicians recommend that the PPE take place in the athlete's primary care medical home, during an office visit and not in a group setting.4,12 Despite the insurance coverage limitations noted previously, the PPE may be an athlete's only contact with a physician in any given year, allowing an opportunity for the physician to incorporate routine preventive health care into the visit when possible.5,13
Medical History
The medical history is an important component of the PPE. The history alone can detect up to 88% of general medical conditions and 67% to 75% of musculoskeletal conditions pertinent to sports participation.14 Providing history forms before evaluation allows the athlete and family time to complete an accurate medical history and to reduce errors. The PPE5 recommends using forms that are simpler and shorter than those previously recommended4 (Table 115 ).
TABLE 1. Preparticipation Physical Evaluation Forms

Adapted with permission from Wise S, Leggit J. Preparticipation physical evaluation: AAFP and others update recommendations. Am Fam Physician. 2020;101(11):693.
A parent or guardian should be involved in completion of the history form. A study of high school athletes undergoing PPEs found that only about 19% of students' answers were in concordance with their parents' responses.16
Of particular importance is personal history of possible cardiovascular symptoms (e.g., exertional chest pain) or family history of premature serious cardiac conditions or sudden death before 50 years of age.4 Other inquiries about potentially disqualifying conditions include a history or symptoms of spinal injuries, brachial plexus injuries, concussions, neurologic disorders, diabetes mellitus, loss of a paired organ (e.g., kidney), skin conditions, asthma or exercise-induced bronchospasm, hematologic disorders, and musculoskeletal injuries.4 Answers to these questions may prompt consideration for further evaluation through a structured examination or additional testing to determine eligibility for sports participation.
The history should also include questions about mental health, substance use, and high-risk behavior. These issues should ideally be discussed with the athlete alone to increase the likelihood of honest answers.17
Physical Examination and Testing
Elevated blood pressure and visual acuity problems are among the most common abnormalities noted during the physical examination portion of the PPE.4,18 The evidence is lacking for performing any other routine screening tests in asymptomatic athletes as part of the PPE, but expert consensus recommends a structured physical examination.4 In particular, the American Heart Association and American College of Cardiology provide recommendations that should be followed with regard to various cardiovascular abnormalities, considering intensity of the sport and disease severity with the potential of sudden cardiac death.19
The cardiovascular portion of the examination should focus on identifying concerning findings, such as pathologic heart murmurs or the stigmata of Marfan syndrome (e.g., long arms and legs, tall and thin body, flexible joints).19 Worldwide, there is considerable debate about whether electrocardiography or echocardiography should be part of the PPE.20,21 The American Heart Association continues to recommend its 14-element cardiovascular history and physical examination as opposed to electrocardiogram screening (Table 2).22 It is unknown whether detection of disease by these screening tests leads to a reduction in sudden cardiac deaths.23
TABLE 2. The 14-Element American Heart Association Recommendations for Preparticipation Cardiovascular Screening of Competitive Athletes

| Medical history* |
| Personal |
| 1. Chest pain, discomfort, tightness, or pressure related to exertion |
| 2. Unexplained syncope or near syncope† |
| 3. Excessive and unexplained dyspnea/fatigue or palpitations associated with exercise |
| 4. Prior recognition of a heart murmur |
| 5. Elevated systemic blood pressure |
| 6. Prior restriction from participation in sports |
| 7. Prior testing for the heart, ordered by a physician |
| Family |
| 8. Premature death (sudden and unexpected, or otherwise) before 50 years of age attributable to heart disease in one or more relatives |
| 9. Disability from heart disease in close relative younger than 50 years |
| 10. Hypertrophic or dilated cardiomyopathy, long QT syndrome, or other ion channelopathies, Marfan syndrome, or clinically significant arrhythmias; specific knowledge of genetic cardiac conditions in family members |
| Physical examination |
| 11. Heart murmur‡ |
| 12. Femoral pulses to exclude coarctation of the aorta |
| 13. Physical stigmata of Marfan syndrome |
| 14. Brachial artery blood pressure (sitting position)§ |
*—Parental verification is recommended for high school and middle school athletes.
†—Judged not to be of neurocardiogenic (vasovagal) origin; of particular concern when occurring during or after physical exertion.
‡—Refers to heart murmurs judged likely to be organic and unlikely to be innocent; auscultation should be performed with the patient in both the supine and standing positions (or with Valsalva maneuver), specifically to identify murmurs of dynamic left ventricular outflow tract obstruction.
§—Preferably taken in both arms.
Adapted with permission from Maron BJ, Friedman RA, Kligfield P, et al. Assessment of the 12-lead ECG as a screening test for detection of cardiovascular disease in healthy general populations of young people (12–25 years of age): a scientific statement from the American Heart Association and the American College of Cardiology. Circulation. 2014;130(15):305.
When a condition is identified that may restrict an athlete's medical eligibility for participating in a certain sport, consultation with a specialist may be warranted. If it is determined that there is risk to participation, shared decision-making should occur, including a discussion among the athlete, the athlete's family, and an interdisciplinary health care team about the risks and benefits of participation. It may be appropriate to consider an alternative activity in which the athlete could participate.19 It is also important to consider that athletes restricted from participating in their chosen sport may be upset; they should be monitored and provided with appropriate emotional support.
Mental Health Screening
Mental health is increasingly recognized as a major issue for young athletes and is emphasized in the PPE5.4 In addition to screening for and evaluating mental health disorders, the PPE can be used as an opportunity to screen for and educate patients on bullying, hazing, sexual abuse, and sleep disorders, all of which can affect mental health in athletes.17,24
DEPRESSION AND ANXIETY
The PPE5 recommends screening athletes for depression and anxiety disorders and maintaining an awareness of local resources that can assist patients.4 Suggested screening tools include the Patient Health Questionnaire-9 (https://www.mdcalc.com/phq-9-patient-health-questionnaire-9) and the Generalized Anxiety Disorder-7 scale (https://www.mdcalc.com/gad-7-general-anxiety-disorder-7).4
Illness and sports-related injury can cause psychological distress, and conversely, psychological distress may be an independent risk factor for injury.25 Depression is also a risk factor for suicide, which is the second-leading cause of death among all college students but only the fourth-leading cause of death in college athletes, suggesting that sports participation may have a protective effect.26,27 In the absence of suicidal ideation, depression or anxiety should not preclude sports participation, although sports participation should not delay appropriate treatment.
ATTENTION-DEFICIT/HYPERACTIVITY DISORDER
Attention-deficit/hyperactivity disorder is another common condition affecting athletes. It is not a disqualifier for sports participation, but academic accommodations and treatment should be provided as needed after diagnosis. At the collegiate and elite level, a therapeutic use exemption may be required for patients taking attention-deficit/hyperactivity disorder medications at the same time as sports participation.28,29
Substance Abuse Screening
Screening should be performed for substance use disorders, including tobacco, vaping/electronic cigarettes, performance-enhancing supplements, alcohol, marijuana, and prescription analgesics.4 One method for substance abuse screening is the CRAFFT (Car, Relax, Alone, Forget, Friends, Trouble) tool, which is intended for use in individuals 12 to 21 years of age (https://crafft.org/).
Special Considerations
FEMALE ATHLETE TRIAD AND RELATIVE ENERGY DEFICIENCY IN SPORT
The female athlete triad (the triad) and relative energy deficiency in sport (RED-S) are syndromes that occur when energy expenditure is disproportionately high relative to caloric intake. The triad refers to girls and women who have long-term manifestations of low energy availability, disordered eating, decreased bone mineral density, and menstrual dysfunction. The RED-S syndrome is characterized by relative energy deficiency (sometimes due to an eating disorder); low bone mineral density; and impaired cardiovascular, immune, and psychological health.30,31 Although it is more often reported in female athletes, the syndrome also occurs in male athletes.32 There is ongoing discussion about the degree of overlap and differences between RED-S and the triad.33
Endocrine abnormalities may also occur, resulting in menstrual dysfunction in female athletes and low testosterone levels and erectile dysfunction in male athletes.30,31,34–36
Screening for the triad and RED-S is challenging because many of its features are not readily apparent until they have progressed to serious clinical concerns. Consequently, it is important to discuss potential early symptoms during the PPE.
Menstrual dysfunction is an important symptom. It is two to three times more common in athletes than nonathletes, with as many as 10% to 15% of female athletes having amenorrhea or oligomenorrhea.37 Use of hormonal oral contraceptives may mask menstrual dysfunction.
Other findings that suggest the possibility of the triad or RED-S include eating disorders, history of bone stress injuries, symptoms of low testosterone in males, and symptoms of low energy (e.g., fatigue, difficulty in recovering from training). Other conditions that may mimic low-energy symptoms should be excluded, notably pregnancy and iron deficiency anemia.
Treatment of the triad or RED-S includes increasing caloric intake and/or decreasing energy expenditure. In female athletes, normalization of menses suggests that the treatment is working. Taking oral contraceptives, however, restores menses without correcting the underlying energy imbalance. This should not preclude the physician from prescribing oral contraceptives to patients with the triad or RED-S if needed for contraception, assuming no contraindications exist. If sports participation would cause serious harm to the athlete's health or compromise appropriate treatment of the syndrome, disqualification may be considered.30
TRANSGENDER ATHLETES
Many sports have traditionally been organized by biologic sex rather than gender identification, and policy on sports participation by transgender athletes has been controversial. A safe and supportive relationship should be established between the athlete and physician, ideally before the PPE. It is important to address patients by their preferred pronoun or gender, which can be identified on a history intake form with a simple question (i.e., What pronouns do you use? or How do you identify your gender?). See a previously published article in American Family Physician on caring for transgender patients for more information.38 An editorial on caring for transgender athletes appears in this issue of American Family Physician.39
As with all athletes, mental health screening and guidance should be thoroughly discussed during the PPE with transgender athletes. However, clinicians should avoid assuming that any concerns are secondary to being transgender.40
As part of the PPE, clinicians should be advocates for transgender athletes to promote inclusivity and to support access to sports participation for all. Clinicians can help improve the health care experience for transgender patients by becoming aware of regulations from local sports governing bodies and by advocating for athletes as they navigate these regulations.41
ATHLETES WITH A DISABILITY
Athletes with a physical or intellectual disability represent a growing number of participants in sports.42 The Americans with Disabilities Act defines disability as an impairment that limits a major life activity.43 Common disabilities in athletes include cerebral palsy, blindness, deafness, paralysis, cognitive impairment, amputation, muscular dystrophy, and multiple sclerosis. Athletes with disabilities derive similar benefits from sports participation as other athletes and should be encouraged to participate.44,45
The PPE of athletes with a disability includes the same components as athletes without a disability but may require closer examination of specific systems. Ocular function should be assessed closely because athletes with a disability commonly have poor visual acuity, refractive errors, astigmatism, or strabismus.46 Assessing the cardiovascular system may require specialty consultation because some underlying disabilities are associated with comorbid congenital heart issues (e.g., patients who have Down syndrome have a high incidence of atrioventricular septal defects).47 Dermatologic abnormalities should be assessed and discussed with athletes who use wheelchairs or who may lie prone during activity. A comprehensive neuromuscular examination is important for athletes with a disability because they may have difficulty with strength, flexibility, or spasticity or may use prosthetic devices.
The PPE of athletes with a disability should ideally use a multidisciplinary approach, with the athlete's medical specialists and service providers available to help assess the athlete's medical condition and functional abilities and the demands of the sport to determine medical eligibility.
COVID-19
The COVID-19 pandemic poses new challenges to conducting PPEs. Adherence to physical distancing guidelines makes it imperative that PPEs are conducted in the patient's medical home as opposed to group settings.7
Another challenge relates to cardiovascular risk after COVID-19. Recommendations for addressing return to play after COVID-19 continue to evolve as new evidence accumulates. The National Federation of State High School Associations, American Medical Society for Sports Medicine, and American Academy of Pediatrics are among several organizations recommending that athletes with COVID-19–related illness be evaluated by a medical professional before returning to participation because potential cardiac and pulmonary risks following the disease can occur.48–50 Specific details of this evaluation are beyond the scope of this review but are addressed in interim guidance from the American Medical Society for Sports Medicine.7
This article updates previous articles by Mirabelli, et al.51; Giese, et al.52; and Kurowski and Chandran.53
Data Sources: A PubMed search was completed using key terms related to the preparticipation physical evaluation. Additionally, the PPE: Preparticipation Physical Evaluation Monograph, 5th ed., was reviewed. Search dates: May 2020 to February 2021.

