Clinic and community resources combine to support patients in this unique group-visit model.

Physicians face many complications when helping patients manage their chronic conditions, including limited time and resources. The group-visit model helps deal with those conflicting demands by allowing physicians to offer extensive education and self-management instruction to patients with similar conditions in a group setting while still providing individual evaluation. With skillful planning and community support, you can use group visits to improve care for patients with a wide range of chronic medical conditions. Our clinic used group visits to help adult patients with obesity and found that they significantly improved their weight, quality of life, mental health, and healthy lifestyle behaviors.
TARGETING OBESITY WITH GROUP VISITS
Obesity has become dramatically more prevalent in the past 20 years. More than 35 percent of U.S. adults are now considered obese.1 Conditions connected to obesity account for almost 10 percent of national health care expenditures, and per-capita medical spending by patients with obesity is 42 percent greater than for patients of normal weight.2 The U.S. Preventive Services Task Force recommends that clinicians offer or provide a referral for intensive multicomponent behavioral interventions to manage obesity for adults with a body mass index (BMI) of 30 or higher.3
Group visits are one option, providing high-quality care that may be more accessible to patients and increase patients' ownership of their conditions.4 In a group setting, physicians can refer clinical questions back to the group for discussion and feedback, which in turn can build confidence in self-care. Group visits can also reduce patients' emergency department and subspecialty visits, hospital readmissions, and phone calls to physicians (although phone calls to nurses may increase) while providing greater overall satisfaction with care.5
Primary care has begun to embrace the group-visit model for managing chronic disease, and evidence suggests that group visits reliably improve intermediate clinical outcomes for patients with type 2 diabetes6 and the management of blood pressure.7 However, there is little research nationally on using group visits for weight management.8 Group visits have been shown to improve childhood overweight and inactivity levels, however.4
Implementing group visits may initially require significant planning. This may include identifying and recruiting patients with chronic conditions, enlisting clinic resources for support, and developing a general format for longitudinal visits.9 Over time, you can easily apply these steps to different medical conditions and across different patient ages and locations. (See “Starting a group visit program.”)
KEY POINTS
- Starting a group-visit program requires significant planning, such as identifying and recruiting patients and enlisting clinical support.
- Community partnerships can add value to a group-visit program.
- Group visits that incorporate a one-on-one encounter between a patient and physician or other eligible clinician are billable with an E/M office-visit code based on the key components and appropriate diagnosis codes for the individual portion of the visit.
STARTING A GROUP VISIT PROGRAM
Choose your focus. The most effective group visits involve high-volume, costly patients with chronic diseases, older patients with numerous comorbidities, or patients with frequent visits.
Determine group visit frequency. Group visits can be ongoing, meeting once or twice a month, or can meet for a limited period. Drop-out rates increase in proportion to the length of the program or the interval between group meetings. Communicating by e-mail or telephone between group sessions may help.
Enlist clinic support. For a group of 15 to 20 patients, you generally will need one administrative person available for check-in and up to two medical assistants or registered nurses to take vital signs or obtain history or key information at the outset of the visit. Consider scheduling groups in the evenings or afternoons, and allow staff to leave after completing their tasks, minimizing overhead expenses. Early evening sessions are most likely to appeal to working adult patients or families. Afternoons might be a better option for seniors.
Identify potential patients. You can use ICD-10 codes, disease registries, or prescription data to create a list of patients to target.
Develop a message to recruit patients. You can extend invitations during regular office visits or by phone, mail, or email. Explain to the patient the benefits of participating, such as peer support, education, improved self-care, and the potential for improved clinical outcomes. You should obtain HIPAA and confidentiality releases in which patients agree not to reveal any personal information disclosed by other patients in the group setting.
Consider involving community partners. Local resources or businesses that share your goals to improve chronic conditions or have similar public health interests may want to partner with you.
OUR GROUP-VISIT MODEL
The University of Wisconsin Health clinic in Verona, Wis., decided in 2013 to start a group visit series to address the high obesity rates in our community. We reached out to local businesses, organizations, and insurers to get their input and cooperation. We felt that using community partners for a common goal would have a greater potential to affect a public health problem.
Six community partners agreed to help, providing some in-kind or reduced cost services to either the practice itself or group participants. These incentives are not essential to the group-visit model, but they offer further motivation. (See “Verona 2020 community partners and benefits.”) In return, in addition to helping combat obesity, the community partners raised their profile. Together, we developed the group-visit model known as the 2020 Verona Clinic Fitness and Lifestyle Challenge, which debuted in 2014 and recently completed its sixth annual group.
VERONA 2020 COMMUNITY PARTNERS AND BENEFITS

| Community partner | Benefits |
|---|---|
| Yoga instructors | Provided exercise sessions during group meetings; initially volunteered their time. |
| Local grocery store | Provided $20 gift cards to group members for in-store purchases. |
| National chain grocery store | Provided in-person nutritional services through in-store dietitian, 10 percent discount for group members, store tours, and cooking demonstrations in the store's restaurant. |
| Local fitness center | Provided a fitness class instructor during group meetings, a free tour/demonstration, discounted memberships, and personal trainers with individualized fitness plans. |
| Local insurance companies | Treated the group meetings as a “wellness plan,” reimbursing individuals $100 for completing the program. |
Each group has up to 20 participants. Participants must have a BMI of 30 or more and express motivation to lose weight in the program. Clinicians are encouraged to personally invite patients to participate, and interested patients receive a formal invitation letter followed by a phone call from one of the program leaders.
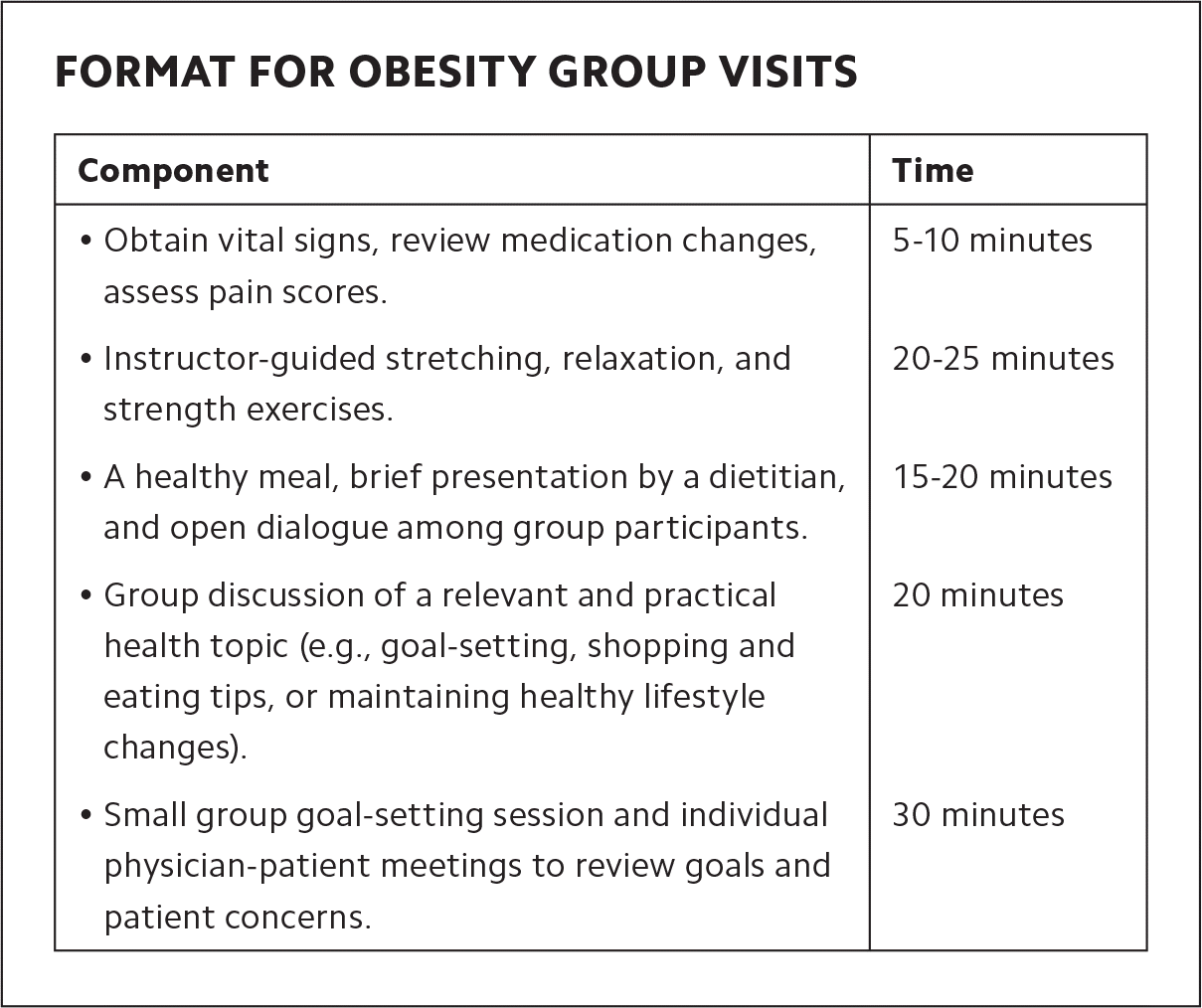
Over 20 weeks, a family physician and a behavioral health specialist conduct six monthly, 90-minute group visits at the clinic in the early evening. (See “Format for obesity group visits.”)
FORMAT FOR OBESITY GROUP VISITS
| Component | Time |
|---|---|
| • Obtain vital signs, review medication changes, assess pain scores. | 5–10 minutes |
| • Instructor-guided stretching, relaxation, and strength exercises. | 20–25 minutes |
| • A healthy meal, brief presentation by a dietitian, and open dialogue among group participants. | 15–20 minutes |
| • Group discussion of a relevant and practical health topic (e.g., goal-setting, shopping and eating tips, or maintaining healthy lifestyle changes). | 20 minutes |
| • Small group goal-setting session and individual physician-patient meetings to review goals and patient concerns. | 30 minutes |
At each group visit, patients individually check in with an administrative staff member, who also collects any necessary copayments. Up to two medical assistants or registered nurses obtain vital signs and briefly review any pertinent changes in medication or pain scores.
The visits begin in our clinic community room, where a yoga instructor from a partnering fitness center leads the group in stretching and relaxation exercises, as well as strength exercises with resistance bands, for approximately 20 to 25 minutes.
The group is served a healthy meal while a dietitian from a partnering grocery store leads a brief discussion of the meal components, nutrition information, and possible meal variations. The dietitian plans these meals, which are prepared offsite, to reflect the patients' dietary needs, preferences, and allergies and to encourage patients to try common foods in different combinations and increase their intake of vegetables, fruit, and whole grains.
Next, the physician leaders, dietitian, or fitness instructor lead a group discussion on a health topic for 20 to 25 minutes. The topics include SMART (specific, measurable, attainable, realistic, and timebound) goal setting, mindful eating, reading nutrition labels, and overcoming obstacles to maintaining healthy lifestyle changes. Patients frequently struggle with making healthy choices when grocery shopping or eating out, so the group also reviews specific examples of how to navigate stores and restaurant menus.
The participants then break into groups of approximately three to six patients led by the physician or behavioral health specialist. They review barriers and successes of that month's goals and set SMART goals for the next month. They may also discuss changes in individual medical conditions, medications, or treatment since the last meeting, either in one-on-one meetings or in front of the small group. Patients sign agreements when they join the group visits that they will not disclose other group members' personal information. Participants receive an after-visit summary that includes topics reviewed, patient resources for nutrition and exercise, and their individual SMART goals.
Between visits, patients receive weekly e-mails from the group leaders that include exercise tips and nutrition information (e.g., recipes and corresponding grocery lists). Group members using mobile apps for exercise or food tracking can share information with the group or the group dietitian, who can suggest modifications.
THE FINANCIAL SIDE OF GROUP VISITS
Providing group visits doesn't have to be expensive. For example, we conduct the group visits in the early evenings to allow clinic support staff to leave after completing their work, which minimizes overhead. Our first group yoga instructor volunteered her time as she was working to achieve certification, but subsequent instructors have received a small fee for each session from the clinic's general funds. To reduce costs further, the exercise portion of the meetings could be recorded and reused to avoid needing an instructor at every session. Serving the group members a meal is not necessary for group visits, but we felt it would be a useful adjunct to our weight management program. It's also not costly, with $50 covering dinner for 20 patients and the dietitian's time for each session. Unpaid interns assist the dietitian with the food preparation as part of their academic training, the meals are self-serve, and clinic staff handle cleanup.
As for revenue, billing codes specifically for group visits have not been established. Some physicians use the evaluation and management (E/M) code 99499, “Unlisted evaluation and management service,” for Medicare patients participating in group visits. However, this is a miscellaneous code without a set value, and insurers may not reimburse for it.10 Instead, as long as the patient is provided a one-on-one encounter during the group visit, you can bill traditional E/M office visit codes 99212–99214 for the individual portion of the visits, based on the history, examination, and medical decision making provided and documented for each patient. We have typically submitted 99213 and been paid appropriately for these visits. Because some insurers may not pay for treatment of overweight or obesity alone, you should be sure to submit diagnosis codes for any conditions that are exacerbated by overweight and obesity, such as diabetes, metabolic syndrome, hypertension, hyperlipidemia, coronary artery disease, osteoarthritis, or obstructive sleep apnea.4
If the group visit includes services led by a dietitian or a behavioral health specialist, that portion of the group visit can be directly billed by the nonphysician – for example, 97804, “Medical nutrition therapy, group, each 30 minutes,” or 96153, “Health and behavior intervention, each 15 minutes, face-to-face, group.” Not all payers will reimburse these codes (Medicare and Medicaid will not), and if payers do, it is sometimes only when diabetes-related education is provided. If physicians provide the group portion of the visit, it might be possible to obtain reimbursement for group education and behavioral-change coaching by billing a code for preventive medicine group counseling, such as 99411 (30 minutes) or 99412 (60 minutes), or for physician educational services in a group visit setting, such as 99078. These codes would be billed in addition to the E/M code for each individual visit, with modifier 25, “Significant, separately identifiable E/M service by the same physician on the same day of the procedure or other service.” Note that individual payers may not consider obesity counseling a preventive service. Check with your payers to determine what will work best in your situation.
ARE YOUR GROUP MEETINGS MEETING YOUR NEEDS?
Once you implement group visits, you must evaluate whether the model is effective. Depending on what health care goals you are trying to address, your key outcome measures might include improvements in A1C, blood pressure control, or pain scores, or changes in how patients use medication for these conditions.
We measured each participant's weight, height, BMI, and blood pressure each month and tracked the data in the clinic's electronic health record. We also conducted pre- and post-program formal assessments that included the Patient Health Questionnaire-9 (PHQ-9), a validated instrument to measure depression severity; the Short Form Survey (SF-36), a validated quality-of-life instrument; and the Fitness and Lifestyle Self-Assessment, a 13-item nonvalidated questionnaire of self-care created by our program coordinators. We mailed the assessments to the patients to complete prior to the initial group visit, and they completed the assessments again at the final session. Physician leaders used Excel spreadsheets to track weight, BMI, and the pre- and post-program formal assessment data.
We are continuing to analyze data collected over the five years of our group-visit program. But during the first two years, the average participant's weight decreased five pounds, from 252.2 to 247.2 pounds during the program. Although overall weight loss was small, it was statistically significant and similar to weight loss seen with diabetes prevention programs. Also during this period, average PHQ-9 scores improved from 6.0 (mild depression) to 3.6 (minimal depression), average SF-36 scores improved from 50.8 to 62.5 (with higher scores equating with better health), and emotional well-being and pain subscales also improved. We also saw improvement in four self-care areas — meal planning, regular weekly exercise, knowledge of pedometer use, and recognition of inexpensive exercise methods — as well as positive trends for reducing systolic and diastolic blood pressure.
Qualitative comments from the program evaluations revealed that many participants said they would have been unable to make changes on their own without participating in the group program, and they were particularly encouraged by the motivation they received from the clinicians.
GROUP VISITS ARE NOT JUST FOR BIG GROUPS
Although our obesity group-visit program used community partners and a multidisciplinary team, this model could be used on a smaller scale. You could involve community partners as you became more experienced with group visits. Patients might also help you identify what community partners may help sustain group visits and achieve long-term goals.
With planning and clinic and community support, we have found group visits are a feasible and useful tool for helping patients better manage chronic medical conditions such as obesity over time. The financial differences between traditional and group visits are minimal, but the potential gains in patient outcomes and satisfaction make group visits a worthwhile model to consider.

