Determining whether the visit you've just finished should be coded as a level 4 could be as simple as asking yourself three questions.

Performing level 4 evaluation and management (E/M) outpatient visits but coding them as level 3 visits is a costly mistake for family physicians. It can result in $30,000 or more in lost revenue in a year, depending on practice volume. Some doctors choose to report a level 3 instead of a level 4 because of fear of over-coding.1 Some do level 4 work but their documentation is lacking and doesn't support a level 4 code. But the most common reason I've seen for under-coding level 4 visits is that the coding criteria are complex and time-consuming.
“Coding is complicated and boring,” I often hear physicians say. “I have better things to do, like take care of my patients.”
New rules for coding and documenting outpatient E/M office visits should simplify things, clear up confusion, and help you code more confidently and accurately.
The rules, which took effect Jan. 1, are the most significant changes to E/M coding since 1997 (for more details, see “Countdown to the E/M Coding Changes” in the September/October 2020 issue of FPM). Coding for outpatient E/M office visits is now based solely on either the level of medical decision making (MDM) required or the total time you spend on the visit on the date of service. (See “E/M coding changes series.”) The history and exam components are no longer used for coding purposes. (Note: these changes apply only to regular office visits and not to nursing home or hospital E/M visits.)
The 2021 E/M coding changes should help ensure you're not leaving money on the table, especially when it comes to coding level 4 visits, which is not as straightforward as coding other levels.
KEY POINTS
- Doing level 4 evaluation and management (E/M) work but coding it as a level 3 office visit is a common mistake that can cost a family physician thousands of dollars each year.
- Rule changes that eliminated the history and exam portions from coding requirements should make it easier to identify level 4 office visits and code them for appropriate reimbursement.
- Answering three basic questions can help you identify whether you've performed a level 4 visit.
E/M CODING CHANGES SERIES
- September/October 2020 — Countdown to the E/M Coding Changes
- November/December 2020 — The 2021 Office Visit Coding Changes: Putting the Pieces Together
- January/February 2021 — Coding Level 4 Office Visits Using the New E/M Guidelines
CODING LEVEL 4 VISITS: THE BASICS
These are the basic parameters for coding a level 4 visit based on total time or MDM under the new rules.
Total time includes all time the physician or other qualified health professional (QHP) spends on that patient on the day of the encounter. This includes time spent reviewing the patient's chart before the visit, face-to-face time during the visit, and time spent after the visit documenting the encounter. It may also include discussing the patient's care with other health professionals or family members, calling the patient later in the day, or ordering medications, studies, procedures, or referrals, as long as those actions happen before midnight on the date of service. Total time does not include time spent performing separately billed procedures or time spent by your nurse or other office staff caring for the patient.
The total time needed for a level 4 visit with an established patient (CPT code 99214) is 30–39 minutes. The total time needed for a level 4 visit with a new patient (CPT 99204) is 45–59 minutes.
Many EHRs have time calculators that will show the amount of time you have had the patient's chart open. This will help you keep track of time while you're reviewing the chart before the visit, performing the exam (if you always open the chart at the beginning of the visit and close it at the end of the encounter), and making notes after the visit. It will be less helpful for physicians who open the computer only when needed during the patient visit.
Documentation of total time is fairly straightforward: just note how much time you spent on the visit that day. You aren't required to break down how much time you spent before, during, and after the visit, though that may be helpful supportive detail in the event of an audit. You may want to include a short definition of total time so that patients who read their notes don't confuse it with face-to-face time and think, “My doctor only spent 20 minutes with me, not the 40 minutes listed here.” For example, your documentation could say, “Total time: 40 minutes. This includes time spent with the patient during the visit as well as time spent before and after the visit reviewing the chart, documenting the encounter, making phone calls, reviewing studies, etc.” In addition to preventing misunderstandings, this gives patients a better idea of all the time we spend on them outside of the actual visit. Another way to accomplish it without “note bloat” is to have a pop-up message with this information that appears in the EHR whenever patients access their notes.
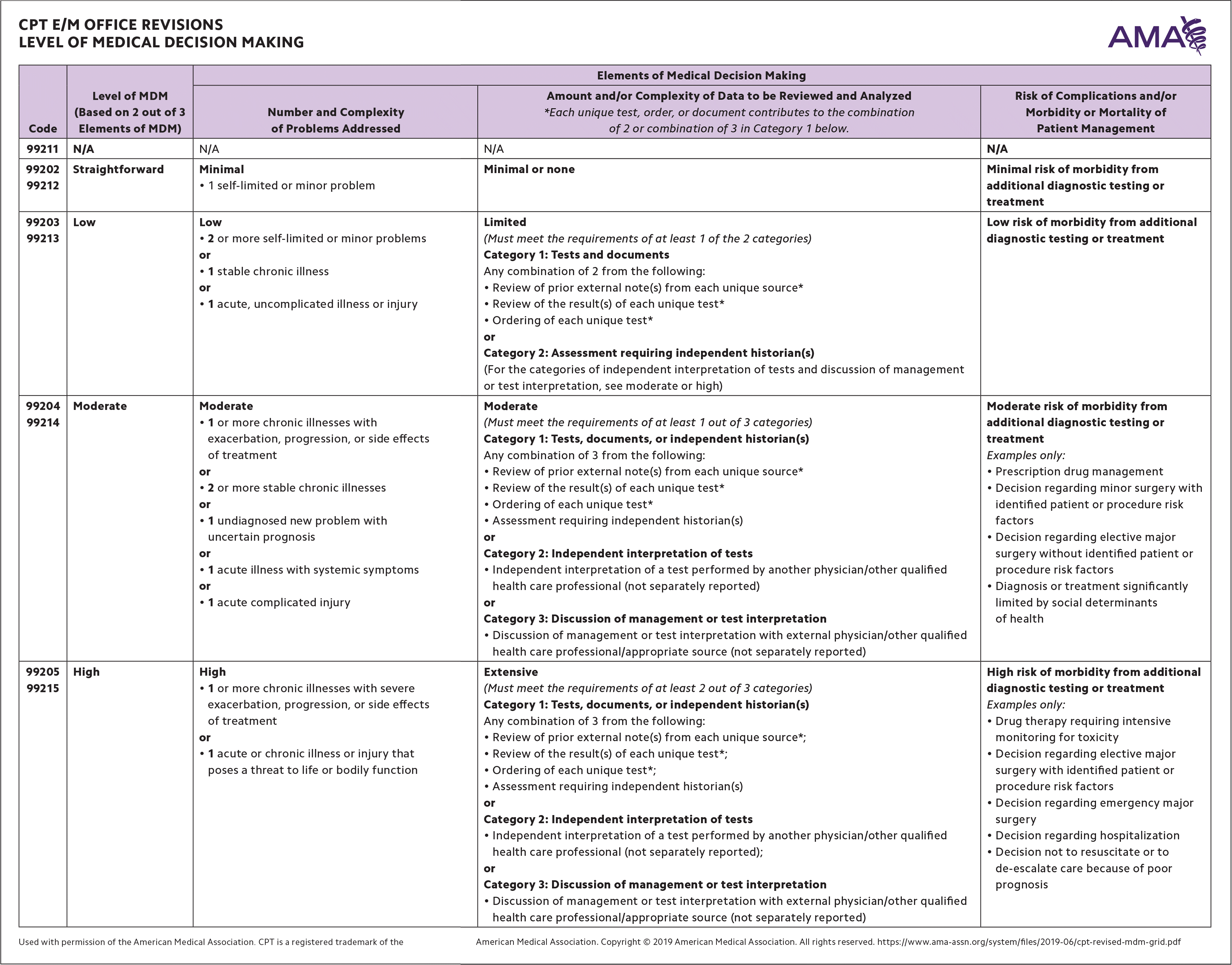
Medical decision making is still made up of three elements: problems, data, and risk. But the definitions have changed somewhat (see “CPT E/M office revisions: level of medical decision making”). The overall level of the visit is determined by the highest levels met in at least two of those three elements. That means that for an outpatient E/M office visit to be coded as a level 4 (for new or established patients), you need at least two of the three elements to reach the “moderate” category — moderate number and complexity of problems addressed; moderate amount and/or complexity of data to be reviewed and analyzed; or moderate risk of complications and/or morbidity or mortality of patient management. An important difference between coding based on MDM versus total time is that you may count MDM that occurs outside of the date of service (e.g., data reviewed or ordered the day after the patient's visit).
To make this simpler, let's substitute “level 4” for the term “moderate” as we take a look at what qualifies in each category (problems, data, and risk).
Level 4 problems include the following:
- One unstable chronic illness (for coding purposes “unstable” includes hypertension in patients whose blood pressure is not at goal or diabetes in patients whose A1C is not at goal),
- Two stable chronic illnesses (e.g., controlled hypertension, diabetes, chronic kidney disease, or heart disease),
- One acute illness with systemic symptoms (e.g., pyelonephritis or pneumonia),
- One acute complicated injury (e.g., concussion),
- One new problem with uncertain prognosis (e.g., breast lump).
Level 4 data includes the following:
- One x-ray or electrocardiogram (ECG) interpreted by you,
- Discussion of the patient's management or test results with an external physician (one from a different medical group or different specialty/subspecialty),
- A total of three points, earned as follows: a) One point for each unique test ordered or reviewed (panels count as one point each; you cannot count labs you order and perform in-office yourself), b) One point for reviewing note(s) from each external source, and c) One point for using an independent historian.
Level 4 risk includes the following:
- Prescription drug management, which includes ordering, changing, stopping, refilling, or deciding to continue a prescription medication (as long as the physician documents evaluation of the condition for which the medication is being managed),
- The presence of social determinants of health (lack of money, food, or housing) that significantly limit a patient's diagnosis or treatment,
- Decision about major elective surgery without identified risk factors for patient or procedure,
- Decision about minor surgery with identified risk factors for patient or procedure.
CPT E/M OFFICE REVISIONS LEVEL OF MEDICAL DECISION MAKING
| Code | Level of MDM (Based on 2 out of 3Elements of MDM) | Elements of Medical Decision Making | ||
|---|---|---|---|---|
| Number and Complexity of Problems Addressed | Amount and/or Complexity of Data to be Reviewed and Analyzed *Each unique test, order, or document contributes to the combination of 2 or combination of 3 in Category 1 below. | Risk of Complications and/or Morbidity or Mortality of Patient Management | ||
| 99211 | N/A | N/A | N/A | N/A |
| 99202 99212 | Straightforward | Minimal
| Minimal or none | Minimal risk of morbidity from additional diagnostic testing or treatment |
| 99203 99213 | Low | Low
or
or
| Limited (Must meet the requirements of at least 1 of the 2 categories) Category 1: Tests and documents Any combination of 2 from the following:
or Category 2: Assessment requiring independent historian(s) (For the categories of independent interpretation of tests and discussion of management or test interpretation, see moderate or high) | Low risk of morbidity from additional diagnostic testing or treatment |
| 99204 99214 | Moderate | Moderate
or
or
or
or
| Moderate (Must meet the requirements of at least 1 out of 3 categories) Category 1: Tests, documents, or independent historian(s) Any combination of 3 from the following:
or Category 2: Independent interpretation of tests
or Category 3: Discussion of management or test interpretation
| Moderate risk of morbidity from additional diagnostic testing or treatment Examples only:
|
| 99205 99215 | High | High
or
| Extensive (Must meet the requirements of at least 2 out of 3 categories) Category 1: Tests, documents, or independent historian(s) Any combination of 3 from the following:
or Category 2: Independent interpretation of tests
or Category 3: Discussion of management or test interpretation
| High risk of morbidity from additional diagnostic testing or treatment Examples only:
|
Used with permission of the American Medical Association. CPT is a registered trademark of the American Medical Association. Copyright © 2019 American Medical Association. All rights reserved. https://www.ama-assn.org/system/files/2019-06/cpt-revised-mdm-grid.pdf
IDENTIFYING LEVEL 4 VISITS IN THREE QUESTIONS
Here are three questions you can ask yourself to quickly determine whether you've just performed a level 4 visit:
- Was your total time between 30 and 39 minutes for an established patient, or between 45 and 59 minutes for a new patient? If so, then you're done. Code it as a level 4 using total time.
- Did you see the patient for a level 4 problem and either order/review level 4 data or manage level 4 risk? If so, then code it as a level 4 using MDM.
- Did you order/review level 4 data and manage level 4 risk? If so, code it as a level 4 using MDM.
Another way to simplify coding level 4 visits is to recognize that ordering labs, x-rays, ECGs, and medications (prescription drug management) often signals level 4 work, while using independent historians, discussing care/studies with external physicians, and providing care limited by social determinants of health are not used as often to code level 4 visits. Therefore, questions 2 and 3 could be rephrased or shortened as follows:
- 2. Did you see the patient for a level 4 problem and either prescribe a medication, interpret an x-ray (or ECG), or order/review three tests?
- 3. Did you prescribe a medication and either interpret an x-ray (or ECG) or order/review three tests?
OFFICE VISIT EXAMPLES
Now let's look at three examples of level 4 office visits, documented with the usual SOAP (subjective, objective, assessment, and plan) note. See if you can identify why each is a level 4 before you get to the explanation.
Patient 1
Subjective: 44 yo female presents with 3 day hx of dysuria, frequency, urgency, L mid back pain, fever, chills, and nausea. Has prior hx of UTIs. No hx of pyelo. No hx of resistant infections. Able to keep food down.
Objective: T 100.2, P 96, R 18, BP 110/70. Pt looks ill but not toxic.
EYES: Fundi benign. PERRLA. TMs: Benign. PHARYNX: Benign. NECK: Benign. No cervical adenopathy. HEART: S1 and S2 w/o murmurs. LUNGS: Clear. Breathing is nonlabored. ABDOMEN: soft, nontender, moderate L CVA tenderness. EXTREMITIES no edema.
Laboratory: UA – TNTC, WBCs – 4+ bacteria.
Assessment/Plan: Pyelonephritis N12. Discussed acute pyelo, also ways to prevent bladder infections. Handout given. Push fluids. Discussed fever and pain control. Cipro 500 mg po bid x 7 days with appropriate precautions. RTC 72 hours, RTC or ER sooner if red flags occur.
Explanation: The total time for this visit was 25 minutes (in the range of a level 3 visit), so it can't be coded as a level 4 using total time. The time also was not documented in the note, which would be required to support coding based on total time. However, here's the breakdown for coding the visit based on MDM:
- Was there a level 4 problem? Yes: acute illness with systemic symptoms.
- Was level 4 data ordered/reviewed? No: two lab tests reviewed (three are required).
- Was level 4 risk managed? Yes: prescription drug management.
Two out of three criteria meet the requirements for a level 4, so code it as a level 4.
Patient 2
Subjective: 23 y/o female presents for recheck of depression, also complaining of sore throat and ankle sprain.
Counseling going well. Started on sertraline 50 mg 4 months ago. No new stressors. Pt denies depressed mood, insomnia, anorexia, loss of pleasure, suicidal ideation, poor concentration, or irritability. Anxiety is also well controlled.
Has 2 day hx of L lateral ankle pain. Tripped over dog and turned ankle in. Pt able to walk now with mild limp.
Has a 3 day hx of sore throat, fever, and fatigue. Denies other symptoms.
Objective: T 100.4, P 88, R 14, BP 125/70. Pt is NAD, affect is bright, eye contact is good. EYES: Fundi benign. PERRLA. TMs: Benign. PHARYNX: tonsils 2+ red s exudate. NECK: Benign. No cervical adenopathy. HEART: RRR. LUNGS: Clear. Bilateral ankle exam: L ant drawer is negative, inversion testing on L causes pain, focal mild tenderness and swelling just below L lat malleolus.
Laboratory: strep screen – negative, strep culture – pending.
Assessment/Plan: Depression with anxiety F41.8 well controlled. Sertraline 50 mg refilled. Continue counseling. Discussed depression.
Tonsillitis J03.90. Strep screen neg. Discussed symptomatic measures. Will call if strep culture is positive.
Sprain left ankle, initial encounter S93.492A, is mild and improving. Discussed RICE protocol and NSAIDS if needed.
RTC 2 mo to recheck depression. Call or RTC sooner if problems or concerns develop.
Total time: 35 minutes. This includes time spent with the patient, but also time spent before the visit reviewing the chart and time after the visit documenting the visit, etc.
Explanation: The total time for this visit (35 minutes) is in the range of a level 4 (30–39 minutes), so a physician could code it as a level 4 using total time. However, here's the breakdown for MDM:
- Was there a level 4 problem? No: One stable chronic illness, one acute uncomplicated illness, and one acute uncomplicated injury.
- Was level 4 data ordered/reviewed? No: two lab tests.
- Was level 4 risk managed? Yes: prescription drug management.
This visit only meets one out of three criteria, so it can't be coded as a level 4 based on MDM. But because the physician has documented that the visit met the criteria for a level 4 based on total time, it can be coded as a level 4.
Patient 3
Subjective: 47 y/o male presents for a BP recheck. His home blood pressures have been averaging 155/95. He denies chest pain, fast heart rate, headache, flushing, or nose-bleeds. Feels good. Taking losartan every day. Watches his wt and exercises.
Objective: T 97.2, P 72, R 16, BP 160/95. NAD.
EYES: Fundi nl. PERRLA. TMs: nl.
PHARYNX: nl. NECK: Benign. Thyroid is not enlarged. HEART: S1 and S2 no murmurs. LUNGS: Clear. ABDOMEN: No masses or organomegaly. EXTREMITIES: no edema.
Assessment/Plan: Essential hypertension I10. Increase losartan to 100 mg per day. Check BP 3 times a wk, avoid salt, continue to limit alcohol to 2 drinks a day or less. RTC for BP check in 3 wks, sooner if problems arise.
Explanation: Total time for this visit was 20 minutes (but not documented in note). That is in the range of a level 3 visit, not a level 4.
Here's the breakdown for coding the visit based on MDM:
- Was there a level 4 problem? Yes: One chronic, uncontrolled illness.
- Was level 4 data reviewed/ordered? No: No tests were ordered.
- Was level 4 risk managed? Yes: Prescription drug management.
Two out of three criteria were met, so code it as a level 4.
(Templates to help code visits based on total time or MDM are available with “Countdown to the E/M Coding Changes,” FPM September/October 2020.)
HOW DOES YOUR LEVEL 4 CODING COMPARE?
Comparing your coding with national averages is a good way to gauge where you stand in terms of getting the reimbursements you deserve. The national average for family physicians' usage of the level 4 code (99214) is slowly increasing and is approaching 50% of established patient office visits (it's now above 50% for our Medicare patients).2
That's a good benchmark. But all practices are different, and some coding variation is normal. In general, doctors with more elderly patients usually have a higher percentage of level 4 visits. Doctors who address fewer problems per visit, have a high patient volume, or have a younger panel tend to have a lower percentage of level 4 visits.
Coding should be easier with the removal of the history and exam components, allowing us to focus more on treating our patients. By using the three questions presented in this article, as well as the patient examples, you should be able to more confidently code level 4 visits and make sure you're getting paid for the amount of work you're doing.

