Psoriasis is a common dermatosis, affecting from 1 to 3 percent of the population. Until recently, the mainstays of topical therapy have been corticosteroids, tars, anthralins and keratolytics. Recently, however, vitamin D analogs, a new anthralin preparation and topical retinoids have expanded physicians' therapeutic armamentarium. These new topical therapies offer increased hope and convenience to the large patient population with psoriasis.
Psoriasis, one of the most common dermatoses, occurs in 1 to 3 percent of the population.1 Although it is rarely life-threatening, psoriasis can cause significant morbidity, social embarrassment, financial cost and disruption in patients' lives. While patients with extensive and severe disease may require potent oral therapy, less severe psoriasis is typically treated with topical medications. This article reviews both the power and the limitations of topical therapies in the treatment of psoriasis.
Pathophysiology
For many years, the mechanism of disease in psoriasis was believed to be epidermal hyperproliferation, since the disease manifests as thick plaques (Figure 1). Laboratory research has shown that patients with psoriasis have a shortened epidermal cell cycle. Normally, keratinocytes require 28 to 44 days to migrate from the basal cell layer of the epidermis to the stratum corneum. In patients with psoriasis, however, this migration takes only four days.2 The dramatic response of patients who are treated with methotrexate (Rheumatrex), an agent that inhibits cellular mitosis, provides additional support for this hypothesis. However, since lymphocytes are found within the psoriatic epidermis and since the disease can be successfully treated with immunosuppressive medications, psoriasis may be a primary immunologic disorder that leads to secondary epidermal hyper-proliferation.
FIGURE 1.
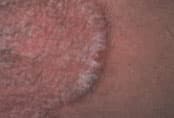
Well-demarcated plaque with superficial scale, typical of psoriasis.
Corticosteroid Therapy
Topical corticosteroids remain one of the most widely used treatment modalities for psoriasis. Corticosteroids have anti-inflammatory, immunosuppressive and antiproliferative properties.3 They bind to a receptor in the cytoplasm of cells and are transported to the nucleus, where they affect gene transcription. The efficacy of an individual topical corticosteroid is related to its potency (Table 1) and its ability to be absorbed into the skin. Absorption can be enhanced by the use of plastic occlusion or by the type of corticosteroid chosen.
TABLE 1 Corticosteroid Potency Chart*
| Generic name | Trade name and strength |
|---|---|
| Class 1—superpotent | |
| Betamethasone dipropionate | Diprolene gel/ointment, 0.05% |
| Diflorasone diacetate | Psorcon ointment, 0.05% |
| Clobetasol propionate | Temovate cream/ointment, 0.05% |
| Halobetasol propionate | Ultravate cream/ointment, 0.05% |
| Class 2—potent | |
| Amcinonide | Cyclocort ointment, 0.1% |
| Betamethasone dipropionate | Diprosone ointment, 0.05% |
| Desoximetasone | Topicort cream/ointment, 0.25%; gel 0.05% |
| Diflorasone diacetate | Florone ointment, 0.05%; Maxiflor ointment, 0.05% |
| Fluocinonide | Lidex cream/ointment, 0.05% |
| Halcinonide | Halog cream, 0.1% |
| Class 3—upper mid-strength | |
| Betamethasone dipropionate | Diprosone cream, 0.05% |
| Betamethasone valerate | Valisone ointment, 0.1% |
| Diflorasone diacetate | Florone, Maxiflor creams, 0.05% |
| Mometasone furoate | Elocon ointment, 0.1% |
| Triamcinolone acetonide | Aristocort cream, 0.5% |
| Class 4—mid-strength | |
| Desoximetasone | Topicort LP cream, 0.05% |
| Fluocinolone acetonide | Synalar-HP cream, 0.2%; Synalar ointment, 0.025% |
| Flurandrenolide | Cordran ointment, 0.05% |
| Triamcinolone acetonide | Aristocort, Kenalog ointments, 0.1% |
| Class 5—lower mid-strength | |
| Betamethasone dipropionate | Diprosone lotion, 0.05% |
| Betamethasone valerate | Valisone cream/lotion, 0.1% |
| Fluocinolone acetonide | Synalar cream, 0.025% |
| Flurandrenolide | Cordran cream, 0.05% |
| Hydrocortisone butyrate | Locoid cream, 0.1% |
| Hydrocortisone valerate | Westcort cream, 0.2% |
| Prednicarbate | Dermatop emollient cream, 0.1% |
| Triamcinolone acetonide | Kenalog cream/lotion, 0.1% |
| Class 6—mild | |
| Alclometasone dipropionate | Aclovate cream/ointment, 0.05% |
| Triamcinolone acetonide | Aristocort cream, 0.1% |
| Desonide | DesOwen cream, 0.05% |
| Fluocinolone acetonide | Synalar cream/solution, 0.01% |
| Desonide | Tridesilon cream, 0.05% |
| Betamethasone valerate | Valisone lotion, 0.1% |
| Class 7—least potent | |
| Topicals with hydrocortisone, dexamethasone, flumethasone, methyprednisolone and prednisolone | |
*—These categories are defined by a vasoconstrictor assay.
Reprinted with permission from Steroids. Portland, Ore.: National Psoriasis Foundation, 1998:6–7.
In general, mid-potency corticosteroids are used for lesions on the torso (Figure 2) and extremities, while low-potency corticosteroids are used for areas with delicate skin, such as that on the face, genitals or flexures. These delicate areas are at increased risk for cutaneous atrophy, one of the side effects of topical corticosteroids. High-potency corticosteroids are usually reserved for use on recalcitrant plaques or lesions on the palms of the hands and soles of the feet. Even then, they should only be used for about two weeks. Ointments are the best choice for dry, scaly, hyperkeratotic plaques; however, they feel oily to the touch and are difficult to wash away from hair. Lotions and gels are best suited for the treatment of the scalp; creams can be used on all areas.
FIGURE 2.
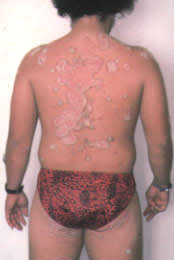
Multiple confluent psoriasis plaques on the back and extremities.
One of the drawbacks of corticosteroid therapy is associated tachyphylaxis, leading to decreased efficacy with continued use and sometimes culminating in an acute flare-up when therapy is terminated. Tachyphylaxis can be minimized by switching patients to less potent corticosteroids and having them apply the medication less frequently once the lesions have improved. Another strategy is the use of corticosteroid-free periods. Potential local side effects of topical corticosteroid therapy include acne and localized hypertrichosis.
Skin atrophy can also occur and may lead to striae, telangiectasia and purpura. The use of very potent topical corticosteroids or weaker ones under occlusion may lead to suppression of the pituitary-adrenal axis.4 In addition, one mortality from Cushing's syndrome has been reported as a result of the use of a topical corticosteroid.5 In general, in order to minimize systemic absorption, a patient should not use more than 40 to 50 g per week of a potent topical corticosteroid and not more than 90 to 100 g per week of a moderately potent topical corticosteroid. Corticosteroids may be used in combination with other treatments (Table 2).
TABLE 2 Topical Agents for the Treatment of Psoriasis
| Drug | Advantages | Disadvantages | Comment | Cost* |
|---|---|---|---|---|
| Corticosteroids | Easy to use, rapid onset | Tachyphylaxis, atrophy, telangiectasia and adrenal suppression possible | Can be used in combination with calcipotriene (Dovonex) or tazarotene (Tazorac) | † |
| Calcipotriene | Well-tolerated | Expensive, may cause skin irritation | Potential for hypercalcemia with excessive use | $78.00 per 60 g |
| Anthralin (Anthra-Derm) | Once-daily administration, well-tolerated | May stain and/or cause skin irritation | Microencapsulated form may be less staining and irritating | 25.00 to 30.00 |
| Tars | Effective with UV light therapy | May cause skin staining, folliculitis, contact allergy; malodorous | Commonly used for psoriasis of the scalp | † |
| Tazarotene | Expensive, may be teratogenic; irritating to uninvolved skin | First topical retinoid indicated by the FDA for treatment of psoriasis | 60.00 to 212.00† |
UV = ultraviolet; FDA = U.S. Food and Drug Administration.
*—Estimated cost to the pharmacist based on average wholesale prices at the mid-range, rounded to the nearest dollar, in Red book.
Montvale, N.J.: Medical Economics Data, 1998. Cost to the patient will be higher, depending on prescription filling fee.
†—Price varies according to product and strength used; generic preparations available.
Keratolytics
Keratolytic agents assist in removing scale or hyperkeratosis in patients with psoriasis or other dermatoses. A commonly used keratolytic agent is salicylic acid. It is usually prescribed in concentrations between 2 and 10 percent and should not be applied extensively on the body, especially in children, for fear of inducing salicylism (e.g., toxic effects marked by tinnitus, nausea and vomiting). Salicylic acid in concentrations of 5 to 10 percent compounded in petrolatum, acid mantle cream or even mid-strength topical corticosteroids can be used twice daily for several weeks at a time on thick keratotic plaques. Stronger concentrations of keratolytics (20 percent salicylic acid) can be applied for about two weeks to remove the thick scale to enable other topical therapies to better penetrate the skin. Urea-containing preparations and alphahydroxy acids, such as glycolic and lactic acids, are also effective keratolytic agents.
Anthralin
Anthralin (Anthra-Derm) derives its origin from the herbal remedy Goa powder, which was used for refractory skin diseases in India and Brazil.6 Anthralin is presently available in ointment, cream and paste forms. Although its mechanism of action is not well defined, anthralin has been demonstrated to inhibit cell growth and restore cell differentiation. It is traditionally applied once daily at night. The initial concentration of 0.05 percent or 0.1 percent is gradually increased to no more than 3 to 5 percent.
Although anthralin is an effective antipsoriatic agent without systemic side effects, it can stain hair, skin, nails, clothing and bedding a brownish to purplish color. To minimize staining, patients should be advised to apply the medication wearing plastic gloves and to use old sheets and nightclothes. Furthermore, anthralin can be very irritating to normal skin and must be applied only to affected skin. Contact with the face, eyes or mucous membranes must be avoided. Applying petroleum or zinc oxide ointment around the psoriatic lesion may help prevent anthralin from causing perilesional irritation. A 0.5 to 1 percent preparation applied for at least 10 minutes can be washed off with soap and water; this application has been shown to be as effective as the longer conventional application.7–9
Because of its inconvenience and its tendency to irritate unaffected skin, anthralin has for the most part been supplanted by newer agents, although many patients still derive benefit from its use.
Coal Tar
Coal tar for treatment of cutaneous conditions was described by the Greek philosopher Dioscorides nearly 2,000 years ago,10 and it continues to be used today in the treatment of psoriasis (Table 2). Coal tar is produced by heating coal in the absence of air and removing ammonia from the resulting dark residue. Because coal tar contains as many as 10,000 different chemical compounds, its precise mechanism of action is not clear. However, it appears to have antiproliferative and anti-inflammatory actions, and clinical use has demonstrated its efficacy. Not only is coal tar beneficial when used alone in patients with mild to moderate psoriasis, it is also useful in combination with ultraviolet B radiation and has been successful in cases that were refractory to other treatment modalities.11
The use of coal tar, like anthralin, is limited by its inconvenience. In addition to its unpleasant odor, it can also stain clothing and bedding. Crude coal tar is particularly difficult to use. Some of the purified preparations are more acceptable for outpatient use but may not be as effective. Side effects include folliculitis and contact allergy. If contact allergy is suspected, the patient should undergo patch testing to distinguish between an allergic and an irritant response. If the patient has an irritant response, treatment with coal tar may continue, but with a lower concentration. There has been one report of severe bronchospasm in an atopic patient with asthma after inhalation of coal tar vapor.12 In addition, coal tar has been found to be carcinogenic in animal studies,13 although conclusive evidence linking its use to cancer in humans is lacking.
Coal tar can be applied at night and should be allowed to dry on the skin for 10 to 15 minutes before the patient gets in bed (to minimize staining of bedding and nightclothes) and is showered off in the morning. Alternatively, coal tar can be applied in the morning and showered off after 10 to 15 minutes. A once-daily application of coal tar is often used in conjunction with a topical corticosteroid applied twice daily. Although tars have generally been supplanted by newer, more convenient medications, tar-containing shampoos are effective in the treatment of psoriasis of the scalp (Figure 3).
FIGURE 3.
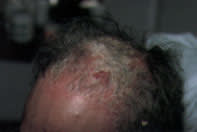
Psoriasis of the scalp.
Vitamin D Analogs
The rationale for the use of vitamin D derivatives in the treatment of psoriasis is based on the observation that patients with hypocalcemia often develop various forms of psoriasis, most notably the pustular form. In one case, a patient who had undergone thyroidectomy developed repeated flares of pustular psoriasis after decreases were made in her dosage of ergocalciferol (Vitamin D2); each episode was related to severe hypocalcemia and resolved after her serum calcium levels normalized.14 Another patient with osteoporosis experienced dramatic improvement in severe psoriasis after receiving an oral form of vitamin D.15 This finding, along with the discovery that the bioactive form of 1,25-dihydroxycholecalciferol has been shown to inhibit keratinocyte proliferation and promote keratinocyte differentiation,16 has led to the development of vitamin D analogs for the treatment of psoriasis.
Calcipotriene (Dovonex), a topical vitamin D analog, has been available in the United States since 1993. Short-term clinical trials have demonstrated that it is at least as effective as betamethasone 17 valerate ointment17,18 and superior to short-contact anthralin cream19 or 15 percent coal tar.20 Long-term studies have also shown that the short-term response to calciprotriene can be maintained for up to 12 months.21
Calcipotriene, applied twice daily, is generally well tolerated, although the face and groin areas should be avoided since it may cause irritant dermatitis.22 Like corticosteroids, calcipotriene can be considered a first-line agent and is available as an ointment, cream or solution. To avoid hypercalcemia, calcipotriene use should not exceed 100 g per week. Calcipotriene is not associated with tachyphylaxis, and it has been shown to result in greater improvement and fewer side effects when combined with the potent corticosteroid halobetosol (Ultravate).23 Use of calcipotriene should be discontinued when a woman becomes pregnant.24
Retinoids
Retinoids mediate cell differentiation and proliferation. Systemic retinoids have been used for the treatment of recalcitrant, severe psoriasis. Oral retinoids, such as etretinate (Tegison), are associated with several adverse effects, such as teratogenicity, serum lipid and transaminase elevations, mucocutaneous toxicity, skeletal changes and hair loss. Topical retinoids were developed to avoid many of these systemic side effects. In June 1997, the U.S. Food and Drug Administration labeled tazarotene (Tazorac) for the treatment of psoriasis involving up to 20 percent of the body surface area. Applied topically, tazarotene is rapidly metabolized in the skin and converted to to the active metabolite, tazarotenic acid.
Clinical studies have demonstrated the efficacy of both 0.05 and 0.1 percent tazarotene gel.25,26 Study results suggest that tazarotene use may lead to an extended response, providing long-term improvement and maintenance therapy.26 The gel formulation is suitable for the treatment of scalp psoriasis. Unlike calcipotriene, tazarotene can be used to treat psoriasis of the face.
Local skin irritation and pruritis are frequent side effects of tazarotene, and care must be used to ensure that the medicine is applied only to lesional skin. Since tazarotene may be teratogenic, women of child-bearing age should be warned of the potential fetal risk and should use adequate birth-control measures. A negative pregnancy test should be confirmed within two weeks of initiating treatment with tazarotene; as an additional precaution, therapy can be started during a normal menstrual period.

