When no organic cause for dyspepsia is found, the condition generally is considered to be functional, or idiopathic. Nonulcer dyspepsia can cause a variety of symptoms, including abdominal pain, bloating, nausea, and vomiting. Many patients with non-ulcer dyspepsia have multiple somatic complaints, as well as symptoms of anxiety and depression. Extensive diagnostic testing is not recommended, except in patients with serious risk factors such as dysphagia, protracted vomiting, anorexia, melena, anemia, or a palpable mass. In these patients, endoscopy should be considered to exclude gastroesophageal reflux disease, peptic or duodenal ulcer, and gastric cancer. In patients without risk factors, consideration should be given to empiric therapy with a prokinetic agent (e.g., metoclopramide), an acid suppressant (histamine-H2 receptor antagonist), or an antimicrobial agent with activity against Helicobacter pylori. Treatment of patients with H. pylori infection and nonulcer dyspepsia (rather than peptic ulcer) is controversial and should be undertaken only when the pathogen has been identified. Psychotropic agents should be used in patients with comorbid anxiety or depression. Treatment of nonulcer dyspepsia can be challenging because of the need to balance medical management strategies with treatments for psychologic or functional disease.
Family physicians frequently encounter patients with dyspepsia. An organic cause, such as duodenal ulcer, is found in only about 40 percent of these patients.1 Hence, dyspepsia is considered to be functional, or idiopathic, in as many as 60 percent of patients (Table 1).2–4 The Rome II criteria provide an updated definition of nonulcer dyspepsia (Table 2).5 Symptoms usually are categorized as ulcer-like (i.e., burning sensation, relief with antacids and histamine-H2 blockers or proton pump inhibitors), dysmotility-like (i.e., nausea, bloating, early satiety, anorexia), or unspecified.5
TABLE 1 Differential Diagnosis of Dyspepsia
| Diagnostic category | Approximate prevalence* | |
|---|---|---|
| Functional or nonulcer dyspepsia† | Up to 60 percent | |
| Dyspepsia caused by structural or biochemical disease | ||
| Peptic ulcer disease | 15 to 25 percent | |
| Reflux esophagitis | 5 to 15 percent | |
| Gastric or esophageal cancer | < 2 percent | |
| Biliary tract disease | Rare | |
| Gastroparesis | Rare | |
| Pancreatitis | Rare | |
| Carbohydrate malabsorption (lactose, sorbitol, fructose, mannitol) | Rare | |
| Medication effects (see Table 3) | Rare | |
| Infiltrative diseases of the stomach (Crohn’s disease, sarcoidosis) | Rare | |
| Metabolic disturbances (hypercalcemia, hyperkalemia) | Rare | |
| Hepatoma | Rare | |
| Ischemic bowel disease | Rare | |
| Systemic disorders (diabetes mellitus, thyroid and parathyroid disorders, connective tissue disease) | Rare | |
| Intestinal parasites (Giardia species, Strongyloides species) | Rare | |
| Abdominal cancer, especially pancreatic cancer | Rare | |
*— Prevalence figures are based on the occurrence of the disorders in patients with dyspepsia who are investigated with endoscopy.
†— Functional or nonulcer dyspepsia is defined as a history of at least three months of dyspepsia with no definite structural or biochemical explanation.
Adapted with permission from Bazaldua OV, Schneider FD. Evaluation and management of dyspepsia. Am Fam Physician 1999;60:1774; Talley NJ, Silverstein MD, Agreus L, Nyren O, Sonnenberg A, Holtmann G. AGA technical review: evaluation of dyspepsia. Gastroenterology 1998;114:582–95; and Fisher RS, Parkman HP. Management of non-ulcer dyspepsia. N Engl J Med 1998;339:1376–81.
TABLE 2 Rome II Diagnostic Criteria for Functional Dyspepsia
| Patient meets the following criteria for at least 12 weeks (which need not be consecutive) within the preceding 12 months: |
| Persistent or recurrent symptoms (pain or discomfort centered in the upper abdomen) |
| No evidence of organic disease (including on upper endoscopy) that is likely to explain the symptoms |
| No evidence that dyspepsia is relieved exclusively by defecation or associated with the onset of a change in stool frequency or stool form (i.e., not irritable bowel syndrome) |
Adapted with permission from Drossman DA, et al., eds. Rome II: the functional gastrointestinal disorders: diagnosis, pathophysiology, and treatment: a multinational consensus. 2d ed. McLean, Va.: Degnon Associates, 2000. Accessed March 2, 2004, at: http://www.romecriteria.org/documents/Rome_II_App_A.pdf.
Many patients seek medical help for an ulcer-like pain syndrome that cannot be explained easily. Notably, symptoms and physical findings are unreliable in distinguishing between ulcer and nonulcer dyspepsia. Furthermore, treatment of patients with nonulcer dyspepsia can be challenging because of the need to balance medical management strategies (e.g., eradication of Helicobacter pylori) with treatments for psychologic or functional disease.
Not surprisingly, nonulcer dyspepsia is responsible for substantial costs to the U.S. health care system (direct medical costs) and to society (e.g., lost time from work, diminished work productivity).6 A better understanding of this condition and its management can improve patient care and decrease unnecessary medical expenditures.
Pathophysiology
The pathophysiology of dyspepsia is not well understood. To explain the symptoms of nonulcer dyspepsia more fully, researchers have focused on several key factors: motility disorders, nonmotility disorders (including H. pylori infection), and psychosocial factors.
MOTILITY DISORDERS
Some patients with symptoms of nonulcer dyspepsia have a history of gastroesophageal reflux. Up to 25 percent also report heartburn.7 Therefore, researchers have attempted to evaluate the role of motility dysfunction in nonulcer dyspepsia by conducting scintigraphic studies of gastric emptying, manometry, and electrogastrography. On these tests, 25 to 60 percent of patients with nonulcer dyspepsia exhibit motility dysfunction.8,9
Symptoms of nonulcer dyspepsia correlate poorly with regional gastric-emptying problems such as decreased compliance in the proximal stomach and relaxation of the distal end.10 Patients may or may not improve when they are given promotility agents; sometimes motility improves, but the symptoms of nonulcer dyspepsia do not.11
Motor dysfunction involving the gall-bladder and biliary tract may play a role in nonulcer dyspepsia. Both delayed emptying of the gallbladder and dysfunction of the sphincter of Oddi have been implicated, but no solid conclusions can be drawn from research conducted thus far.3
NONMOTILITY DISORDERS
Some patients with nonulcer dyspepsia exhibit evidence of hyperemic, mottled gastric or duodenal mucosa on upper endoscopy, which suggests that the symptoms of dyspepsia are caused by duodenitis.12 However, as with motility disorders, there is little correlation between symptoms and severity of duodenitis, and no relationship between treatment and improvement of mucosal appearance on endoscopy.13
One of the most prevalent theories currently being evaluated is the possible involvement of H. pylori infection in nonulcer dyspepsia (as in ulcer disease).3,14 Although some investigators have found a higher prevalence of H. pylori infection in patients with non-ulcer dyspepsia, study results have not been consistent.15,16 The fact that dyspepsia occurs after intentional H. pylori infection supports involvement of this pathogen.17 However, treatment results have been inconsistent, and the role of H. pylori infection in nonulcer dyspepsia remains controversial.18,19
Other possible pathophysiologic mechanisms for nonulcer dyspepsia include bile reflux into the stomach, viral-induced gastritis, malabsorption of carbohydrates, parasitic infections, and augmented visceral pain perception. Little objective evidence supports a large role for any of these factors, and purported involvement for many of them is based on case reports.3
PSYCHOSOCIAL FACTORS
Patients with nonulcer dyspepsia are more likely to have symptoms of anxiety and depression than are healthy persons or patients with ulcers. Multiple somatic complaints also are more common in patients who have nonulcer dyspepsia.20
A history of child abuse has been linked to the symptoms of nonulcer dyspepsia. Stress from life events also has been correlated with these symptoms and has been linked to exacerbations of nonulcer dyspepsia.1 In addition, the condition has been linked to the symptoms of irritable bowel syndrome (despite the emphasis on lower versus upper gastrointestinal tract symptoms), an illness known to be connected to stress.21
COMBINED EFFECT
The combination of psychologic symptoms, motility dysfunction, infection, and nonulcer dyspepsia may be best understood as a complex interaction of factors. Addressing only one factor, such as H. pylori infection or motility dysfunction, is unlikely to be successful and may be frustrating for the patient and the physician. The best management approach would seem to be consideration of both the psychologic and physiologic factors that may underlie nonulcer dyspepsia, although this strategy has not been tested in randomized clinical trials.
Diagnosis
The diagnosis of dyspepsia is challenging because patients often exhibit changing symptoms, and because characterization of the symptoms provides little information about the nature of the underlying physiologic abnormality.22,23
HISTORY
A thorough history may help to clarify the underlying disorder and determine the initial approach to management. Peptic ulcer disease, gastroesophageal reflux disease, and gastric cancer must be excluded. Use of medications and herbal products associated with dyspepsia should be explored (Table 3).2,5,24 Other conditions to consider include celiac sprue and lactose or fructose intolerance.
TABLE 3 Agents Commonly Associated with Dyspepsia
| Acarbose (Precose) |
| Alcohol |
| Alendronate (Fosamax) |
| Antibiotics, oral (e.g., erythromycin) |
| Codeine |
| Corticosteroids (e.g., prednisone) |
| Herbs (e.g., garlic, ginkgo, saw palmetto, feverfew, chaste tree berry, white willow)5 |
| Iron |
| Metformin (Glucophage) |
| Miglitol (Glyset) |
| Nonsteroidal anti-inflammatory drugs, including cyclooxygenase-2 enzyme inhibitors |
| Orlistat (Xenical) |
| Potassium chloride |
| Risedronate (Actonel) |
| Theophylline |
Adapted with permission from Bazaldua OV, Schneider FD. Evaluation and management of dyspepsia. Am Fam Physician 1999;60:1776, with additional information from references 5 and 24.
ENDOSCOPY
Establishing the diagnosis of peptic or duodenal ulcer greatly clarifies the treatment approach. Therefore, it is important to determine whether endoscopy is needed (Figure 1).2,4
Figure 1 Dyspepsia
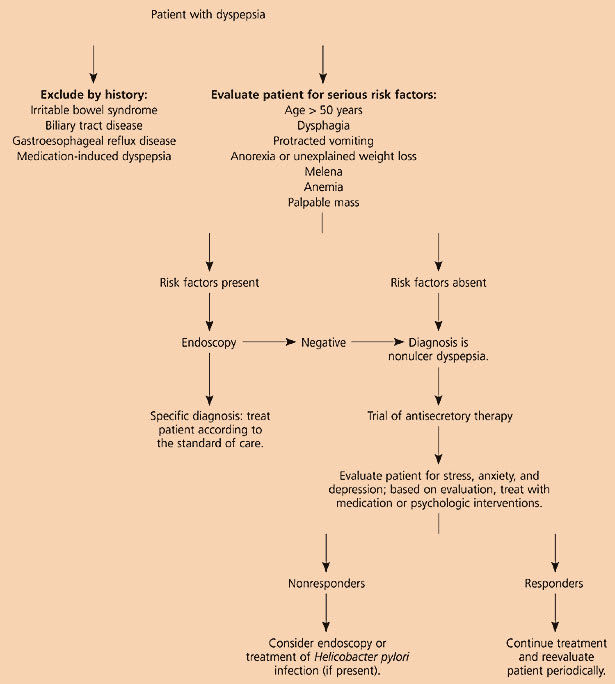
Evaluation and management of nonulcer dyspepsia.
Adapted with permission from Bazaldua OV, Schneider FD. Evaluation and management of dyspepsia. Am Fam Physician 1999;60:1779, with additional information from reference 4.
Although the role of early endoscopy is controversial, some experts4 suggest that endoscopy should be considered in patients with dyspepsia who are older than 55 years, especially if symptoms are not relieved by treatment with a histamine-H2 receptor antagonist (H2RA) or a proton pump inhibitor (PPI). The guidelines outlined in the Maastricht European consensus report25 recommend endoscopy for patients older than 45 years, whereas the American Digestive Health Foundation26 recommends endoscopy for patients with dyspepsia who are older than 50 years. Other experts27 suggest that because of cost, empiric therapy should be used first, even in older patients.
Proponents of endoscopy cite several advantages, including the information that endoscopy provides about reflux, ulcers, and upper gastrointestinal cancers. During endoscopy, samples can be obtained to determine whether a patient has H. pylori infection. However, the cost of endoscopy and the low yield of treatable gastric cancers have dampened enthusiasm for an endoscopy-based approach. If no organic disorder is found on endoscopy, empiric therapy appears to be the most reasonable approach.4
Treatment
Although evidence clearly supports the treatment of peptic ulcer disease, data on the management of nonulcer dyspepsia are conflicting, with treatment sometimes depending on the predominant symptom. Patients with predominant nausea and bloating may have motility dysfunction and may benefit from treatment with a promotility agent. Patients with pain as the predominant symptom may have mucosal disease or H. pylori infection; if H. pylori is identified, a trial of antibiotics may be warranted. Patients with prominent somatic complaints, anxiety, or depression are more likely to have a psychologic basis for their symptoms.
GASTRIC ACID SUPPRESSANTS
Gastric acid suppressants have been evaluated extensively in the treatment of nonulcer dyspepsia, despite lack of evidence for the involvement of acid in the pathophysiology of the condition. While antacids have not been found to be beneficial, bismuth salts have been shown to be somewhat more effective than placebo.28 [Strength of recommendation (SOR) A, systematic review] Because long-term use of bismuth salts is associated with neurotoxicity, these agents should be reserved for second-line therapy.28
A meta-analysis of randomized controlled trials (RCTs) found that H2RAs were more effective than placebo in patients with non-ulcer dyspepsia, although many of the trials had suboptimal study designs.29 [SOR A, meta-analysis] Current evidence does not demonstrate superiority for the PPI omeprazole (Prilosec) over H2RAs. Therefore, H2RAs are preferred, because of their lower cost.28 One review4 noted that most studies have used higher H2RA dosages than those available in over-the-counter formulations, with improvement occurring in approximately 25 percent more patients treated with H2RAs compared with placebo.
PPIs other than omeprazole have not been studied in the management of nonulcer dyspepsia. No evidence supports the use of sucralfate (Carafate) and misoprostol (Cytotec) in patients with nonulcer dyspepsia.
PROKINETIC AGENTS
Prokinetic agents often are touted as the most effective medications for the management of nonulcer dyspepsia. Studies have shown that symptomatic improvement is 45 to 50 percent greater with cisapride, domperidone, or metoclopramide therapy than with placebo.4,28 [Reference 28: SOR A, systematic review of limited-quality studies] However, the studies have been of poor quality. In addition, most of the studies evaluated cis-apride and domperidone, and access to these agents is restricted in the United States.
The prokinetic agent metoclopramide (Reglan) is available in this country for the management of nonulcer dyspepsia. This agent should be used with caution, because it occasionally is associated with the development of tardive dyskinesia. Metoclopramide is a low-cost drug, but antidopaminergic side effects limit its use in elderly patients. Studies comparing H2RAs with metoclopramide have not been performed.
ERADICATION OF H. PYLORI
Several systematic reviews and meta-analyses30–32 have evaluated the benefits of eradicating H. pylori infection in patients with nonulcer dyspepsia. In general, the trials included patients with documented H. pylori infection, used typical dual or triple therapy for H. pylori infection (i.e., antisecretory therapy plus antibiotics), and evaluated dyspepsia at three and 12 months. For every 15 patients with nonulcer dyspepsia in whom H. pylori is eradicated, one fewer patient has dyspepsia a year later.32 [SOR B, systematic review of inconsistent or limited-quality studies] Another study found a small increase (7 percent) in the likelihood of treatment success with H. pylori eradication.33 [SOR B, systematic review of inconsistent or limited-quality studies]
More studies are needed to resolve the conflicting study results and to determine whether, as some investigators claim, a modest benefit for H. pylori eradication may be cost-effective.31 Eradication regimens are reviewed elsewhere.34
PSYCHOTROPIC AGENTS
Patients with nonulcer dyspepsia frequently are treated with tricyclic antidepressants, selective serotonin reuptake inhibitors (SSRIs), and anxiolytic agents. One meta-analysis35 of 11 good-quality clinical trials evaluated the use of tricyclic antidepressants in 737 patients with functional gastrointestinal disorders, defined as irritable bowel syndrome or non-ulcer dyspepsia. Improvement of abdominal pain was significant; the number needed to treat was 3.35 [SOR A, meta-analysis] The authors commented that the symptomatic improvement may have been the result of the treatment of depressive symptoms, and that future clinical trials should implement methods to control for this potential confounding variable. Currently, use of tricyclic antidepressants is limited, because of the potential side effects of these agents and the availability of newer antidepressants.
No published studies have evaluated the use of SSRIs in the management of nonulcer dyspepsia. Because these patients often have depression and anxiety, SSRI therapy may be effective.4 Use of benzodiazepines should be avoided because of their addictive potential, although treatment with other anxiolytic agents, such as buspirone (BuSpar), may be considered.4 When treatment with an SSRI or buspirone is considered, it is important to be aware that the serotoninergic effects of these agents might cause gastrointestinal upset, initially worsening the dyspepsia. Therefore, these medications should be initiated at the lowest dosage, and the dosage should be increased slowly.
PSYCHOLOGIC INTERVENTIONS
As reported in a Cochrane review,20 three trials have evaluated the effects of psychologic interventions on dyspepsia symptoms and quality of life in patients with nonulcer dyspepsia. The studied interventions included psychotherapy, psychodrama, cognitive behavior therapy, relaxation therapy, and guided imagery or hypnosis. All three trials reported short-term (12-week) improvement of symptoms, and one study also reported some improvement in psychologic parameters. However, at one year, the improvement in symptoms was not statistically significant in two of the studies.20 [SOR B, inconsistent findings from RCTs] Results from these studies were not combined because the interventions were quite different. Overall, psychotherapy should be reserved for use in patients with a significant comorbid psychiatric condition or as an adjunct to medical management.
MISCELLANEOUS
Agents that alter pain perception have been considered for use in the management of nonulcer dyspepsia, because of some evidence showing augmented pain perception in such patients.4 These agents include tricyclic antidepressants, 5-HT3-receptor antagonists (granisetron [Kytril], ondansetron [Zofran]), and somatostatin analogues (octreotide [Sandostatin]).
Alternative therapies, such as peppermint oil and traditional Chinese medicine, have been reported to improve symptoms in patients with dyspepsia. However, published studies have been of poor quality, and the results should be interpreted with caution.36

