Lichen sclerosus, lichen planus, and lichen simplex chronicus are three of the most common non-neoplastic epithelial disorders of the vulva. Lichen sclerosus is characterized by intense vulvar itching and can affect men and women of all ages, but it manifests most commonly in postmenopausal women. Patients with lichen sclerosus have an increased risk of developing squamous cell carcinoma, and they should be monitored for malignancy. Lichen planus is an inflammatory autoimmune disorder that can affect the vulva and the vagina; it peaks in incidence between ages 30 and 60. There are three clinical variants of lichen planus affecting the vulva: erosive, papulosquamous, and hypertrophic. Lichen simplex chronicus is caused by persistent itching and scratching of the vulvar skin, which results in a thickened, leathery appearance. It is thought to be an atopic disorder in many cases and may arise in normal skin as a result of psychological stress or environmental factors. Definitive diagnosis of non-neoplastic disorders depends on the histology of biopsied tissue. All three disorders are treated with topical corticosteroid ointments of varying potency. Lichen sclerosus and lichen planus are not routinely treated with surgery, which is necessary only in patients who have a malignancy or advanced scarring that causes dyspareunia or clitoral phimosis. Educational counseling teaches patients that even though these chronic disorders cannot be cured, they can be effectively managed.
Family physicians are in an ideal position to identify and treat non-neoplastic epithelial disorders of the vulva, which include lichen sclerosus, lichen planus, and lichen simplex chronicus. In addition to recognizing conditions specific to the vulva, family physicians are familiar with dermatologic conditions that affect all parts of the body, and should be able to recognize manifestations of these conditions on the vulva. Moreover, patients with vulvar symptoms often approach their family physician first; therefore, the prompt diagnosis of these conditions is key for successful treatment.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Patients with lichen sclerosus should be evaluated for vulvar malignancy because they are at higher risk for squamous cell carcinoma. | C | 9, 10 | Studies of large groups of women |
| Lichen sclerosus should be treated with a high-potency steroid ointment, such as clobetasol propionate 0.05% (Temovate), to alleviate symptoms, prevent architectural damage, and reverse histologic changes. | B | 31–33 | Consistent findings from randomized controlled trial and descriptive cohort study |
| Vaginal hydrocortisone suppositories are effective for treating erosive vulvovaginal lichen planus. | B | 42 | Prospective observational trial |
| Breaking the itch-scratch cycle is fundamental to the treatment of lichen simplex chronicus. | C | 20,22 | Expert consensus |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see https://www.aafp.org/afpsort.xml.
Lichen Sclerosus
Lichen sclerosus is a chronic, progressive, inflammatory skin condition found most often in the anogenital region.1 Although the exact incidence of lichen sclerosus is unknown, one study showed that this disease affects 1.7 percent of patients presenting to a general gynecology practice.2 Lichen sclerosus can affect women of all ages, although it manifests more often in postmenopausal women.2 Patients with this condition primarily present with intense vulvar itching, which may disrupt sleep and cause dyspareunia.1 Patients may also experience painful defecation and anal fissures if lesions are present in the anal area.1 Some patients with lichen sclerosus may be asymptomatic; one study showed that at least one third of patients may have no symptoms.2 The cause of lichen sclerosus is still under investigation. Some studies have suggested that there may be an autoimmune mechanism,3,4 and others have found a genetic susceptibility in some persons.5–7 Patients with lichen sclerosus have an increased incidence of autoimmune disorders, such as alopecia areata, vitiligo, thyroid disease, and pernicious anemia. In a study of 350 British women with lichen sclerosus, 21.5 percent were found to have an autoimmune-related disease.4
Physical examination is important for differentiating lichen sclerosus from other causes of vulvar pruritus. The appearance of the anogenital skin depends on the degree of disease progression.1 Initially, the skin may appear white, thickened, and excoriated, with edema and resorption of the labia minora.1 As the disease progresses, the skin loses pigmentation and becomes very thin and wrinkled, classically referred to as a “cigarette paper” appearance1 (Figure 1). This fragile skin can easily bruise or form purpura.1 Skin anywhere on the body may be affected with the white papules or plaques, but less than one third of patients with vulvar lichen sclerosus manifest extragenital disease.1 With further progression, anatomic features may become severely distorted as the clitoris becomes buried under the clitoral hood, the labia minora disappear, and the introitus narrows1 (Figure 2). This architectural distortion can be partly responsible for dyspareunia and dysuria. Despite this classic description of disease progression, it is possible for clitoral phimosis to be present even in early lichen sclerosus. The vagina is not involved in lichen sclerosus.
Figure 1.
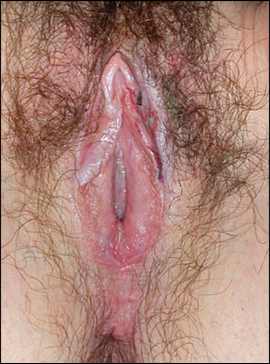
Cigarette-paper appearance of lichen sclerosus of the vulva.
Definitive diagnosis of lichen sclerosus depends on the histology of biopsied tissue. Moreover, it is important to identify and biopsy any thickened areas of epithelium in patients with lichen sclerosus because such acanthotic epidermal areas can be suggestive of squamous cell hyperplasia.1 Patients with lichen sclerosus—especially those with squamous cell hyperplasia—have an increased risk of vulvar malignancy and should be monitored accordingly.8 The increased risk of developing squamous cell carcinoma is approximately 5 percent in patients with lichen sclerosus.9,10 Patients with lichen sclerosus are also at a higher risk for autoimmune disorders and should be screened appropriately.
Figure 2.
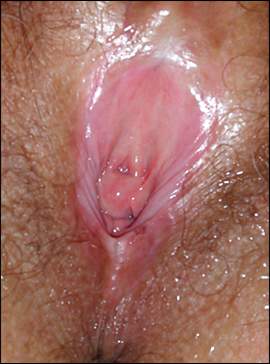
Architectural destruction of the vulva secondary to lichen sclerosus.
Lichen Planus
Lichen planus is an inflammatory autoimmune disorder involving keratinized and mucosal surfaces. There are three clinical variants that affect the vulva: erosive lichen planus, papulosquamous lichen planus, and hypertrophic lichen planus.11 The cause of lichen planus is not known, but the most widely accepted theory is that an autoimmune mechanism results in activated T cells attacking basal keratinocytes.11 The incidence of lichen planus peaks between the ages of 30 and 60, and this disease is rare compared with lichen sclerosus.11
Patients with vulvar lichen planus present most often with itching, burning, postcoital bleeding, dyspareunia, and pain.11 The most common variant of this disease is erosive lichen planus.11 This severe form is characterized by violaceous erosions that look like glassy, reticulated, white papules and plaques (Figure 3), and, if allowed to progress, can lead to extensive erosion and ulceration (Figure 4) with destruction of the vulvar architecture.12 In contrast with lichen sclerosus, erosive lichen planus involves the vagina in up to 70 percent of patients.11,13,14 This vaginitis can result in friable, hemorrhagic tissue, adhesions, and desquamation, causing yellow discharge. Speculum examination can be painful or even impossible in these patients. On examination, the presence of bacterial or fungal superinfection of the affected tissue should be assessed and treated.15 Punch biopsy with direct immunofluorescence can be performed at the border of the eroded area to confirm a diagnosis of erosive lichen planus and rule out an autoimmune blistering disease, which may appear similar to erosive lichen planus.11 The differential diagnosis includes lichen sclerosus, mucous membrane pemphigoid, pemphigus vulgaris, Behçet's syndrome, desquamative inflammatory vaginitis, lichenoid drug reactions, and graft-versus-host disease.11 Of note, erosive lichen planus can affect gingival tissue as well, resulting in vulvovaginal-gingival syndrome.13 The lesions at each site may present at different times, making the diagnosis more difficult.
Figure 3.
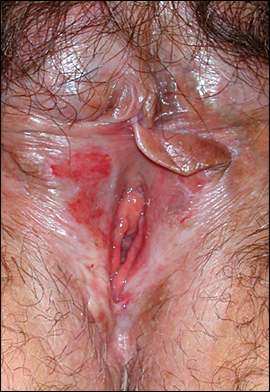
Lichen planus of the vulva.
Figure 4.
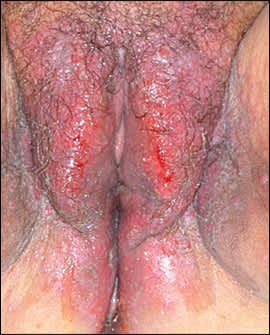
Extensive lichen planus of the vulva.
The less common variants of vulvar lichen planus are papulosquamous lichen planus and hypertrophic lichen planus.11 Though papulosquamous lichen planus is described as small, violaceous, pruritic papules on keratinized skin, the papules more often are poorly demarcated, pink, and opaque.11 Hypertrophic lichen planus presents as hyperkeratotic lesions of the perineum and perianal area, and may appear similar to squamous cell cancer.11
It is still unclear whether vulvovaginal lichen planus leads to an increased risk of squamous cell carcinoma. Several studies16–19 have shown a low incidence of squamous cell carcinoma in patients with lichen planus. As such, patients with lichen planus should be examined regularly, and any nonresolving lesions should be biopsied to rule out malignancy.11,17–19
Lichen Simplex Chronicus
Lichen simplex chronicus is not a specific entity, but rather describes lichenification of the vulva caused by persistent itching and scratching.20 The skin can become leathery and thickened (Figure 5) or, in severe cases, may be excoriated. Lichen simplex chronicus is a fairly common disease, affecting as many as 35 percent of patients seen in clinics specializing in vulvar disorders.21 Patients report intense pruritus with rubbing and scratching that can occur consciously or unconsciously while sleeping. Lichen simplex chronicus is thought to be an atopic disorder in many cases and may arise in normal skin as a result of psychological stress or environmental factors.22 Causative factors include heat, sweat retention, rubbing from clothing, excessive use of cleansers, application of irritating topical products, and irritation from menstrual hygiene products.22 Lichen simplex chronicus can also occur as a secondary process when there is a preexisting condition such as candidiasis, tinea, human papilloma-virus, lichen sclerosus, psoriasis, parasite infestation, or neoplasia.22 Regardless of the cause, the disease is a result of the itch-scratch cycle.
Figure 5.
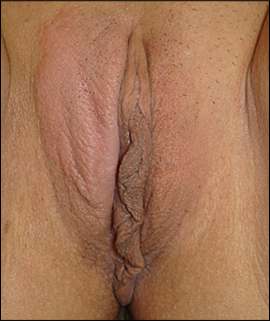
Thickened, leathery skin seen in lichen simplex chronicus of the vulva.
On examination, lichen simplex chronicus presents as erythematous, lichenified plaques with overlying excoriation. Hypopigmentation or hyperpigmentation can occur.22 Linear fissures may be found at the skin folds.
Treatment
Education is an important part of treating patients with vulvar conditions. Patients should be told that these disorders are incurable and the symptoms could be chronic. Symptomatic relief can be achieved with application of topical emollients or viscous lidocaine (Xylocaine) and the use of sitz baths.11,22 Treatment for all three disorders should begin with corticosteroid ointments or creams of varying potency.23
Though not approved by the U.S. Food and Drug Administration for treatment of these conditions, macrolide immunosuppressants (e.g., tacrolimus ointment [Protopic], pimecrolimus cream [Elidel]) have been shown to effectively treat lichen sclerosus, lichen planus, and lichen simplex chronicus.24–28 The use of these drugs is controversial, given some evidence that, at high systemic levels, they may increase the risk of developing skin cancer or lymphoma. However, studies have shown that macrolide immunosuppressants, when used topically for lichen sclerosus and lichen simplex chronicus, do not reach any quantifiable level in the blood, thus making the risk of cancer only theoretical.28,29
Lichen sclerosus and lichen planus are not routinely treated with surgery, which is necessary only in patients who have malignancy or advanced scarring that causes dyspareunia or clitoral phimosis.11,23,30
LICHEN SCLEROSUS
Lichen sclerosus is treated with potent topical steroids to alleviate symptoms, prevent architectural damage, and reverse histologic changes.31–33 The recommended regimen for lichen sclerosus begins with a high-potency corticosteroid (e.g., clobetasol propionate 0.05% ointment [Temovate]) used daily until all active lesions have resolved (usually in two to three months), then tapered to once or twice per week.32,33 A 30-g tube of clobetasol ointment should last three months or longer.33 Alternatively, the patient can use a moderate-potency steroid (e.g., beta-methasone valerate 0.1% cream [Beta-Val]) to maintain remission. Despite known side effects of long-term topical steroid use, one small study showed that treating lichen sclerosus with moderate-potency topical steroids for up to 39 months caused no side effects other than erythema.34
Intralesional steroids and cryotherapy have been used with success in patients with thickened lichen sclerosus lesions; 5 to 20 mg of triamcinolone acetonide (Kenalog) can be injected directly into the area, and cryotherapy can be performed using the contact method, with one freeze-thaw cycle per lesion.35,36 Any lesion that does not resolve with topical or intralesional therapy should be biopsied to confirm the diagnosis and rule out malignancy.
It has been debated whether patients with asymptomatic lichen sclerosus should be treated. Treatment has been shown to slow or reverse disease progression, which may prevent malignancy, but these benefits should be weighed against the theoretical, unproven risks of long-term steroid therapy for lichen sclerosus.23,37
Other medications that have been tried with success in treating lichen sclerosus include oral and topical retinoids,38,39 though they are not considered first-line agents because they have many more side effects than corticosteroid ointments. In the past, topical testosterone and progesterone were accepted therapies for lichen sclerosus, but recent clinical trials have shown that clobetasol is more effective than testosterone and that 2% testosterone (Androgel) is no more effective than petrolatum ointment.31,40
LICHEN PLANUS
All three variants of lichen planus are treated with ultra-potent topical corticosteroids applied twice daily until active lesions have resolved11,16 or, in less severe cases, a moderate-potency topical steroid applied at bedtime.41 As in the treatment of lichen sclerosus, the potency and dosage of the steroid ointment can be tapered once active lichen planus lesions have resolved, though there is no evidence or published data on exact tapering regimens.11 Vaginal hydrocortisone suppositories are an effective treatment for vulvovaginal lichen planus.42
If topical medications fail, the next step is to use an oral corticosteroid (e.g., prednisone, 40 to 60 mg daily for two to four weeks),12,15 which will almost always be effective.11 Because lichen planus is a chronic disorder, tapering or discontinuation of topical or oral therapies can result in recurrent lesions.12 Patients with erosive vaginal lichen planus can also be treated with a potent steroid ointment on a vaginal dilator to maintain a patent vagina.11
LICHEN SIMPLEX CHRONICUS
Patients with lichen simplex chronicus should be treated with a moderate-potency topical corticosteroid (e.g., triamcinolone 0.1% ointment [Triderm] applied twice daily), although high-potency steroids have been used for a short course of two to three weeks.22 Oral steroids can also be used if topical steroids are not effective after several weeks of use.
Any underlying disease causing the itching should be identified and treated.22 Diseases such as tinea, candidiasis, and scabies can be identified with scrapings or culture. Other diseases, such as lichen sclerosus, psoriasis, or neoplasia, can be diagnosed with biopsy. However, adequate treatment of the underlying condition does not always cure the itch-scratch cycle. In refractory cases of lichen simplex chronicus, patch testing may be used to identify the irritants each patient should avoid.43,44
Perhaps the most important component of treating lichen simplex chronicus is breaking the itch-scratch cycle.22 Patients should be advised to avoid scratching the affected areas. Nighttime scratching can be effectively treated with a sedating antihistamine (e.g., hydroxyzine [Vistaril]) given two hours before bedtime.22 The dose can be started at 25 mg and increased as needed and tolerated. Amitriptyline (Elavil, brand no longer available in the United States) at a dosage of 25 to 50 mg at bedtime is effective in treating pruritus, whereas nonsedating antihistamines are not effective. Selective serotonin reuptake inhibitors (e.g., citalopram [Celexa], fluoxetine [Prozac], paroxetine [Paxil], sertraline [Zoloft]) have been proven effective in controlling subconscious scratching associated with lichen simplex chronicus.22
Lichen simplex chronicus can have a prolonged course and, if left untreated, can persist indefinitely, although the symptoms may wax and wane.22 Even with therapy, the symptoms can recur, and some patients require intermittent treatment for months to years.

