The prevalence of hearing loss varies with age, affecting at least 25 percent of patients older than 50 years and more than 50 percent of those older than 80 years. Adolescents and young adults represent groups in which the prevalence of hearing loss is increasing and may therefore benefit from screening. If offered, screening can be performed periodically by asking the patient or family if there are perceived hearing problems, or by using clinical office tests such as whispered voice, finger rub, or audiometry. Audiometry in the family medicine clinic setting is a relatively simple procedure that can be interpreted by a trained health care professional. Pure-tone testing presents tones across the speech spectrum (500 to 4,000 Hz) to determine if the patient's hearing levels fall within normal limits. A quiet testing environment, calibrated audiometric equipment, and appropriately trained personnel are required for in-office testing. Pure-tone audiometry may help physicians appropriately refer patients to an audiologist or otolaryngologist. Unilateral or asymmetrical hearing loss can be symptomatic of a central nervous system lesion and requires additional evaluation.
Nearly 30 million American adults have some degree of hearing loss.1 The prevalence of hearing loss varies with age; at least 25 percent of patients between 51 and 65 years of age, and more than 50 percent of patients older than 80 years, have objective evidence of hearing loss.2,3 Particularly concerning is the increasing prevalence of hearing loss in adolescents and young adults, which affects between 8 and 19 percent of this population.1,4 The U.S. Preventive Services Task Force (USPSTF) finds insufficient evidence for or against screening for hearing loss in asymptomatic adults 50 years or older.3 However, the USPSTF does affirm the effectiveness of screening questionnaires and clinical techniques such as the whispered voice, finger rub, and watch tick tests, all of which can be performed in the primary care clinic.3,5,6 Other guidelines list subjective hearing screening as a preventive service that should be offered to adults starting at 40 years of age.7
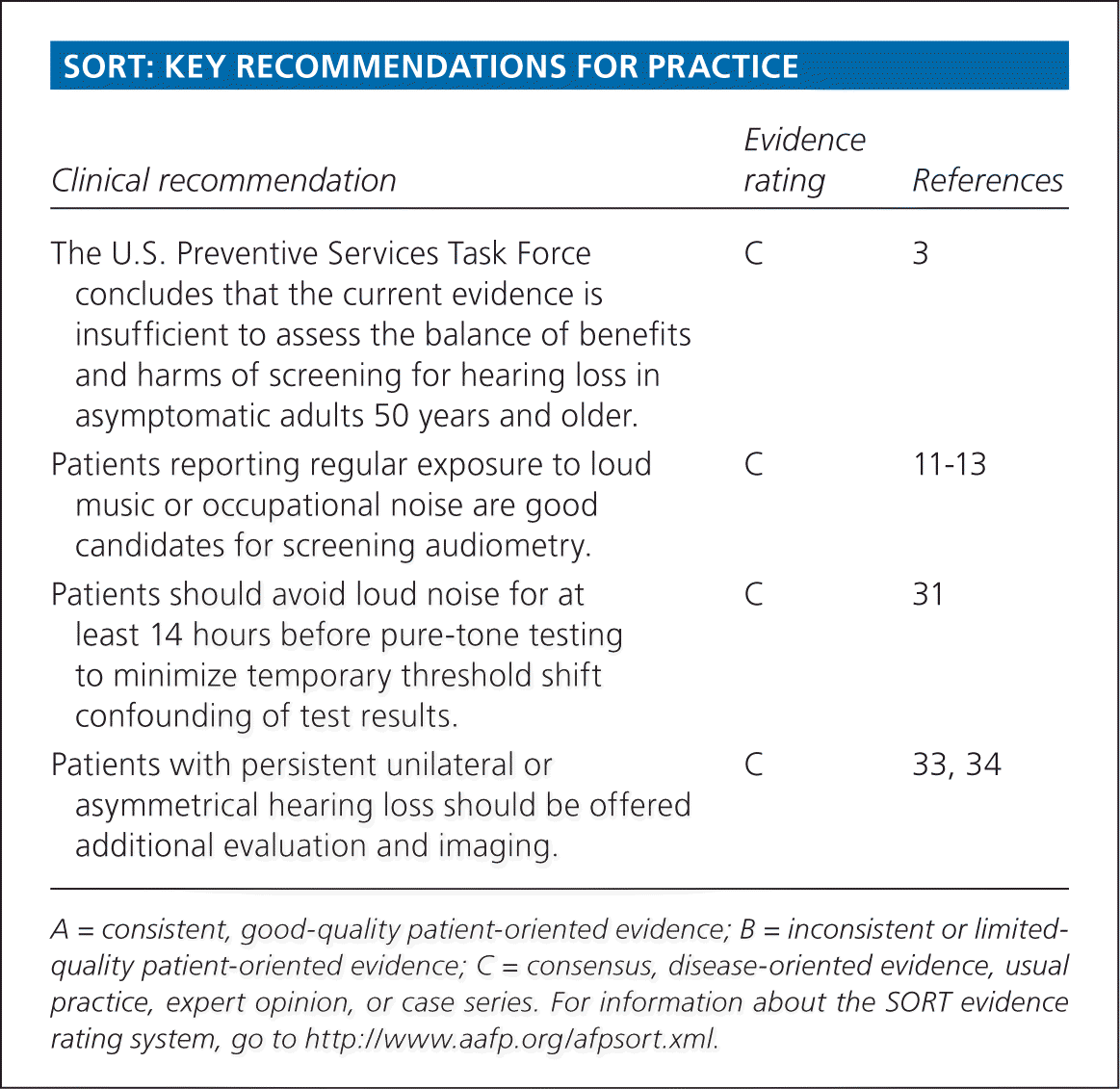
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The U.S. Preventive Services Task Force concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for hearing loss in asymptomatic adults 50 years and older. | C | 3 |
| Patients reporting regular exposure to loud music or occupational noise are good candidates for screening audiometry. | C | 11–13 |
| Patients should avoid loud noise for at least 14 hours before pure-tone testing to minimize temporary threshold shift confounding of test results. | C | 31 |
| Patients with persistent unilateral or asymmetrical hearing loss should be offered additional evaluation and imaging. | C | 33, 34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Audiometry is a relatively simple procedure that can be performed and interpreted by a trained health care professional. Family physicians should feel comfortable performing this testing on adults and cooperative children. Physicians may consider performing audiometry when a patient reports a subjective sense of diminished hearing, or when a family member reports a patient's decreased conversational interaction.8
Although the USPSTF also found insufficient evidence to recommend for or against routinely screening asymptomatic working-age adolescents and adults younger than 50 years for hearing impairment,3 other organizations have recommended regular periodic objective testing throughout childhood and adolescence.9,10 One survey of adolescents and young adults (mean age 19.2 years) revealed that 43 percent of respondents experienced hearing loss associated with exposure to loud music within the past six months.11 Adolescents often listen to music through headphones at maximum volume, and underestimate their vulnerability to music-induced hearing loss.12 Therefore, patients reporting exposure to loud music or occupational noise are good candidates for audiometry.13
Testing may be expanded to include patients who are exposed to excessive noise while at work or at play who have not used adequate hearing protection. Unilateral or asymmetrical hearing loss is common in hunters and military veterans exposed to acoustic trauma from prolonged use of firearms.14
Pure-Tone Audiometry
When hearing loss is suspected, pure-tone audiometry may be used to evaluate hearing deficits by spot-checking certain frequencies, or to evaluate deficits more completely.15 Pure-tone audiometry is performed with the use of an audiometer. Handheld audiometers have a sensitivity of 92 percent and a specificity of 94 percent in detecting sensorineural hearing impairment.16 There are several types of audiometers available, but all function similarly by allowing the tester to increase and decrease the intensity (loudness, in decibels [dB]) and frequency (pitch, in cycles per second or Hz) of the signal as desired.
Pure-tone audiometry is broadly defined as either screening or threshold search. Screening audiometry presents tones across the speech spectrum (500 to 4,000 Hz) at the upper limits of normal hearing (25 to 30 dB for adults, and 15 to 20 dB for children).17 Results are recorded as pass, indicating that the patient's hearing levels are within normal limits, or refer, indicating that hearing loss is possible and a repeat screening test or a threshold search test is recommended.
Threshold search audiometry determines the softest sound a patient can hear at each frequency 50 percent of the time. This testing requires more time and expertise than screening audiometry. The American Speech-Language-Hearing Association has a recommended procedure for pure-tone threshold search tests known as the modified Hughson-Westlake method.18 Testing begins with the ear in which the patient perceives to have better hearing. The tester presents a pure tone at a clearly audible level. After the patient responds to the pure-tone signal, the tester decreases intensity by 10 dB and presents the tone again. If the patient responds to this tone, a “down 10” pattern is employed, with the tester decreasing the intensity of the tone by 10 dB and presenting a tone until the patient no longer responds.18 The tester then increases tone intensity by 5 dB until the patient responds. This is the patient's initial ascending response.
To check for accuracy, the tester should decrease the intensity of the tone by 10 dB one more time to check for no response, then increase the intensity of the signal in 5 dB increments until the patient responds again to the signal. If the patient responds consistently (minimum two out of three responses in ascending order), the tester records the dB level at which the patient responds as the air conduction threshold. After testing the ear that is perceived to have better hearing, the tester then performs the same tests on the patient's other ear.
Testing should begin at 1,000 Hz, because this frequency is easily heard by most patients and has the greatest test-retest reliability.18 A common frequency sequence for pure-tone threshold search testing is to test at 1,000, 2,000, 3,000, 4,000, 8,000, 1,000 (repeat), 500, and 250 Hz.15
Sound frequency (ranging from low to high pitch) is recorded on the audiogram's horizontal axis. Sound intensity is recorded on the vertical axis. Right ear thresholds are manually recorded as a red circle on the audiogram. Left ear thresholds are manually recorded as a blue X (Figures 1 to 4B).
Figure 1.
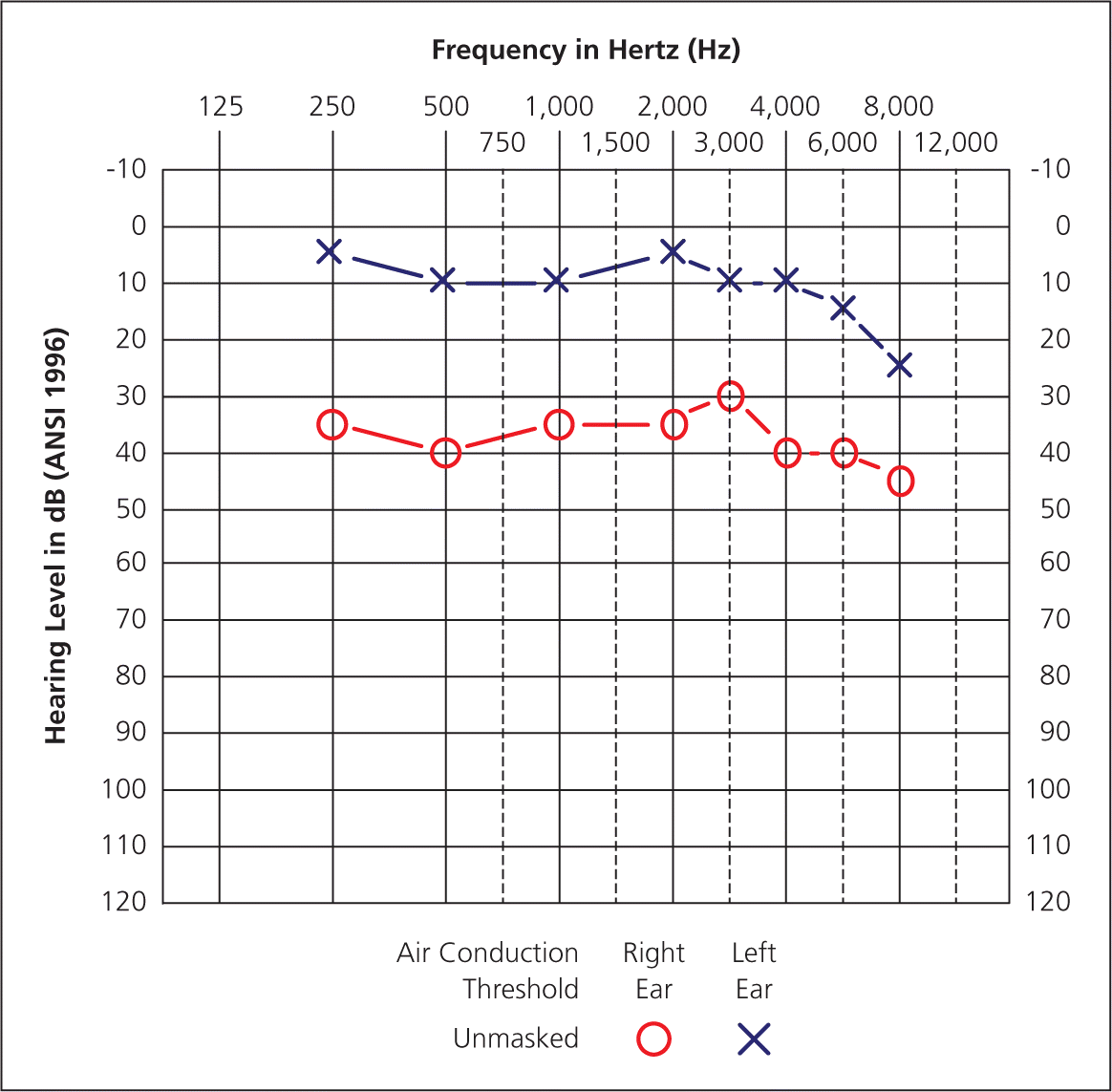
Right ear, flat conductive hearing loss across all frequencies due to complete occlusion of the ear canal with cerumen.
Figures 2A and 2B.
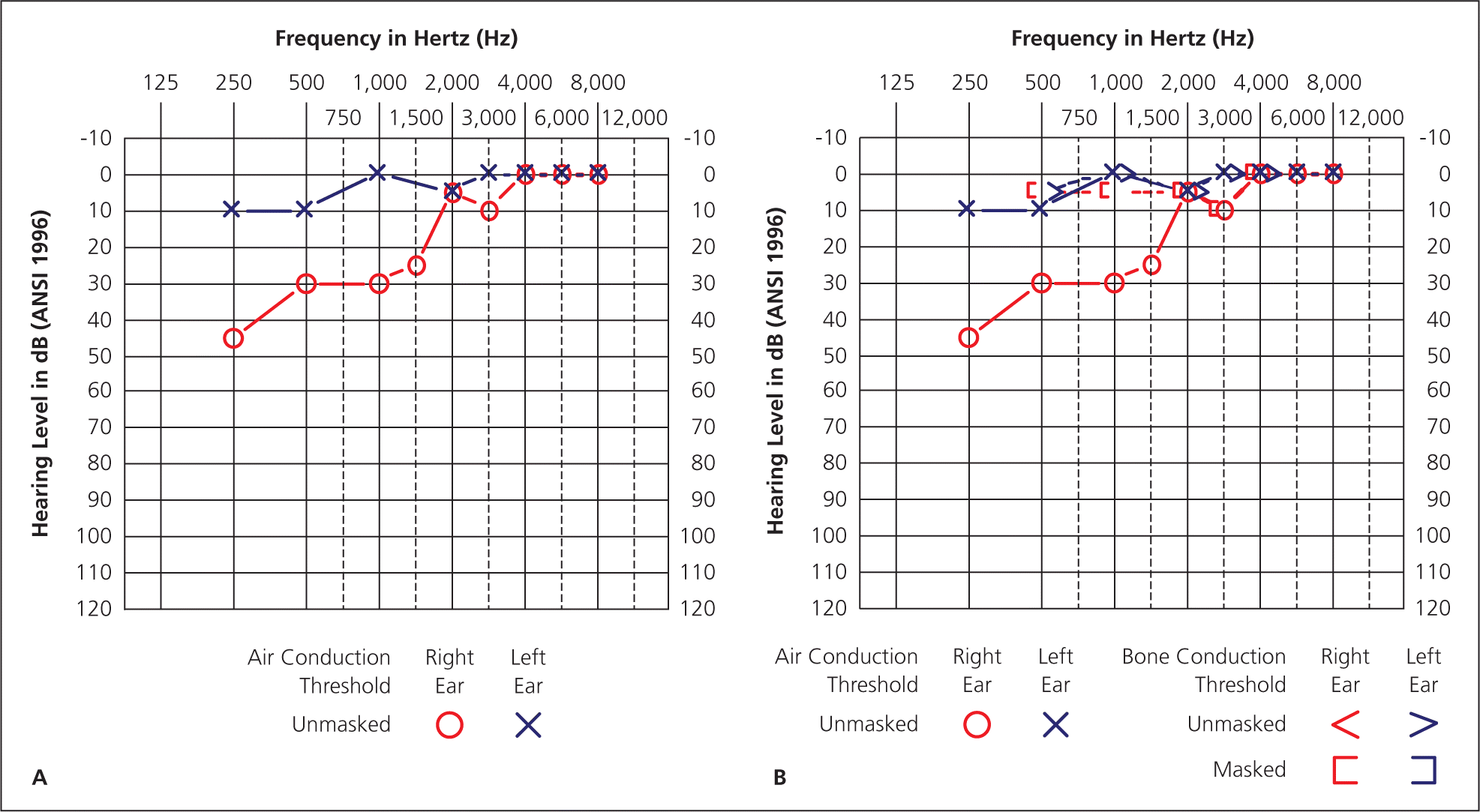
Right ear. Bone conduction is better than air conduction. The patient has low- to mid-frequency conductive hearing loss due to tympanic membrane perforation.
Figures 3A and 3B.
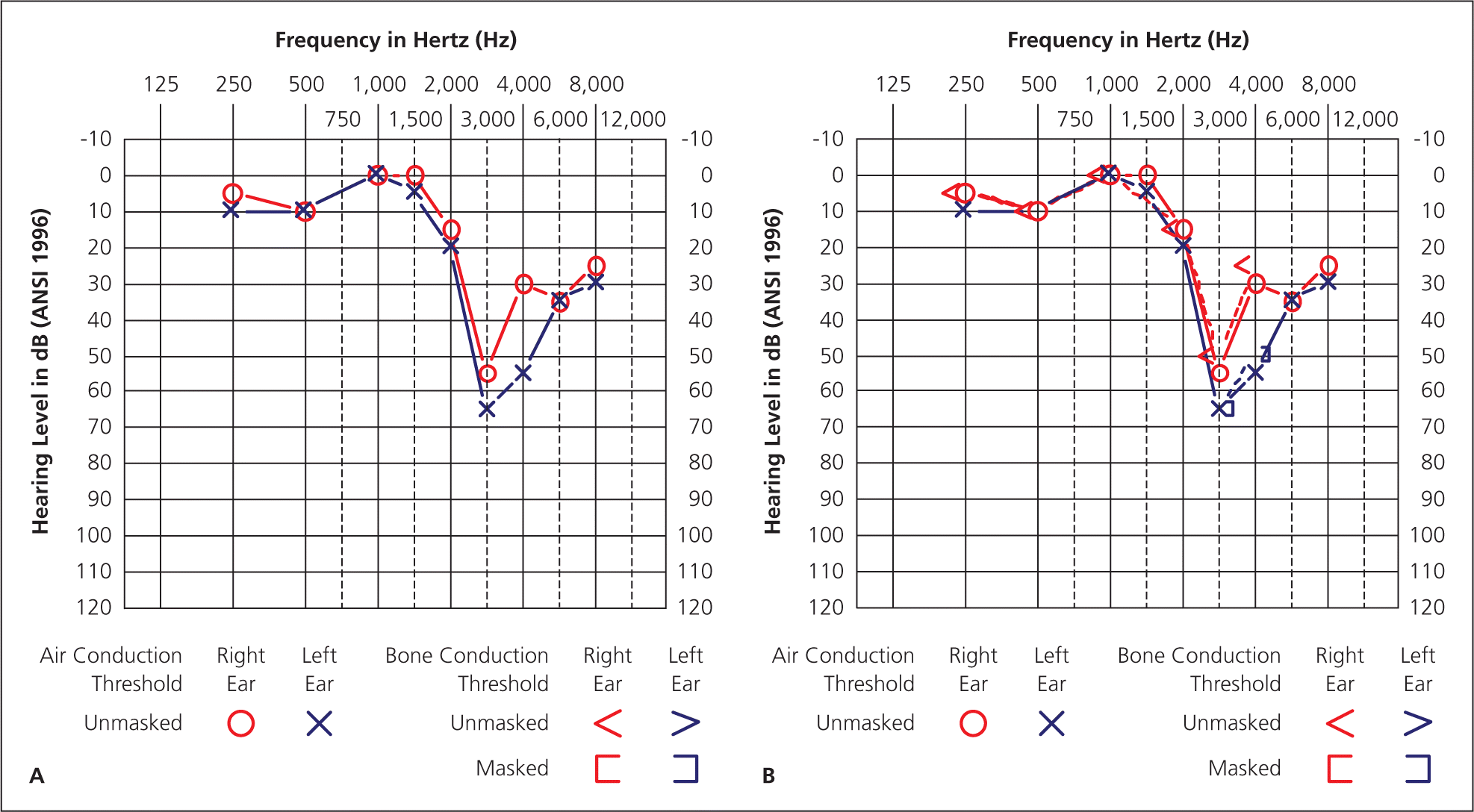
Bilateral, noise-induced sensorineural hearing loss. There are no significant differences between air and bone conduction thresholds. The asymmetry at 3,000 Hz and 4,000 Hz (with the left ear worse than the right) reflects this patient's occupation as a soldier in the infantry and being a right-handed shooter.
Figures 4A and 4B.
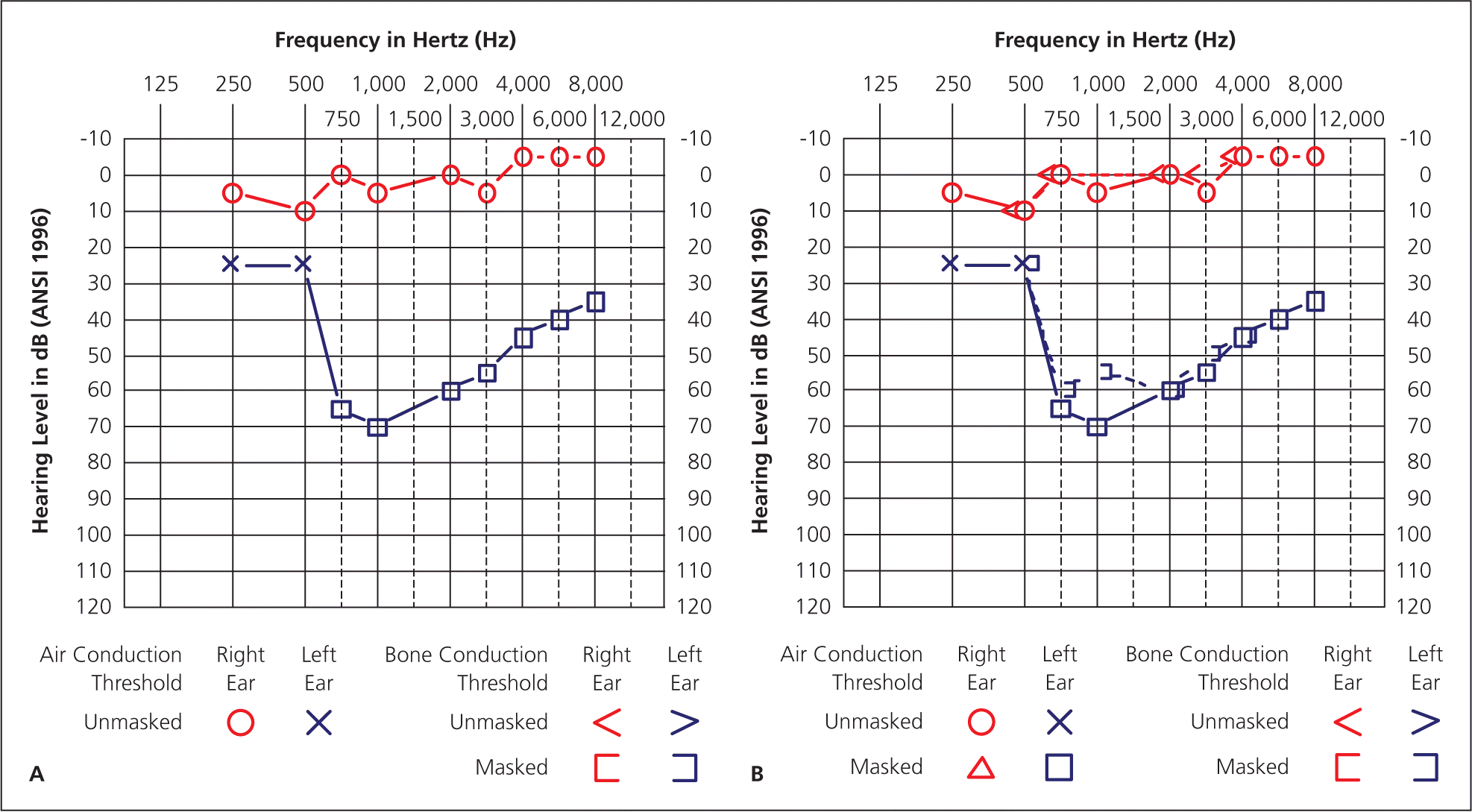
Left ear sensorineural hearing loss due to vestibular schwannoma. With sensorineural hearing loss, there is no significant difference in threshold between air and bone conduction.
Conventional pure-tone testing is used for adults and older children. Audiometry is more challenging in patients younger than five years, and these patients should be referred to an audiologist with experience treating children.19 In many cases, the accuracy of pure-tone testing during well-child visits is overwhelmingly poor.20
Special Considerations Affecting Audiometry Interpretation
ENVIRONMENT
Pure-tone audiometry requires a quiet testing environment with low levels of background noise. Background noise can cause elevated thresholds, especially in low frequencies (eFigures 1A and 1B). To minimize the number of false-positive results, sound levels in the test environment should not exceed American National Standards Institute (ANSI) requirements.21 A quiet booth that features sound-absorptive materials such as carpeting, acoustic foam, or tiles is considered standard practice. Industrial hygienists, biomedical maintenance technicians, and audiologists can evaluate environmental noise levels in the test area using a sound level meter to ensure that ANSI specifications are met.
eFigure 1A
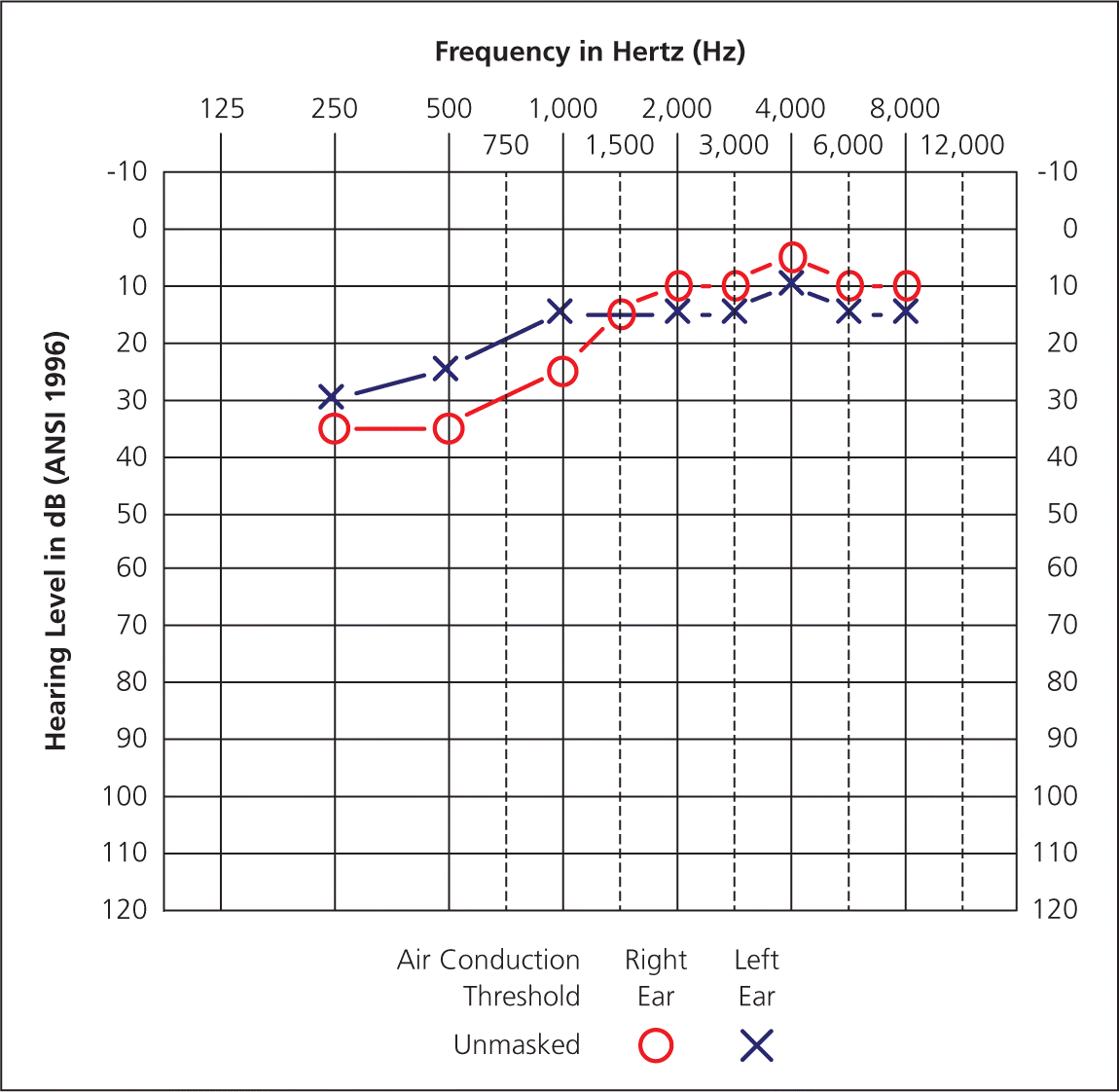
The audiogram shows a false low-frequency hearing loss in both ears because of excessive background noise in the test area.
eFigure 1B
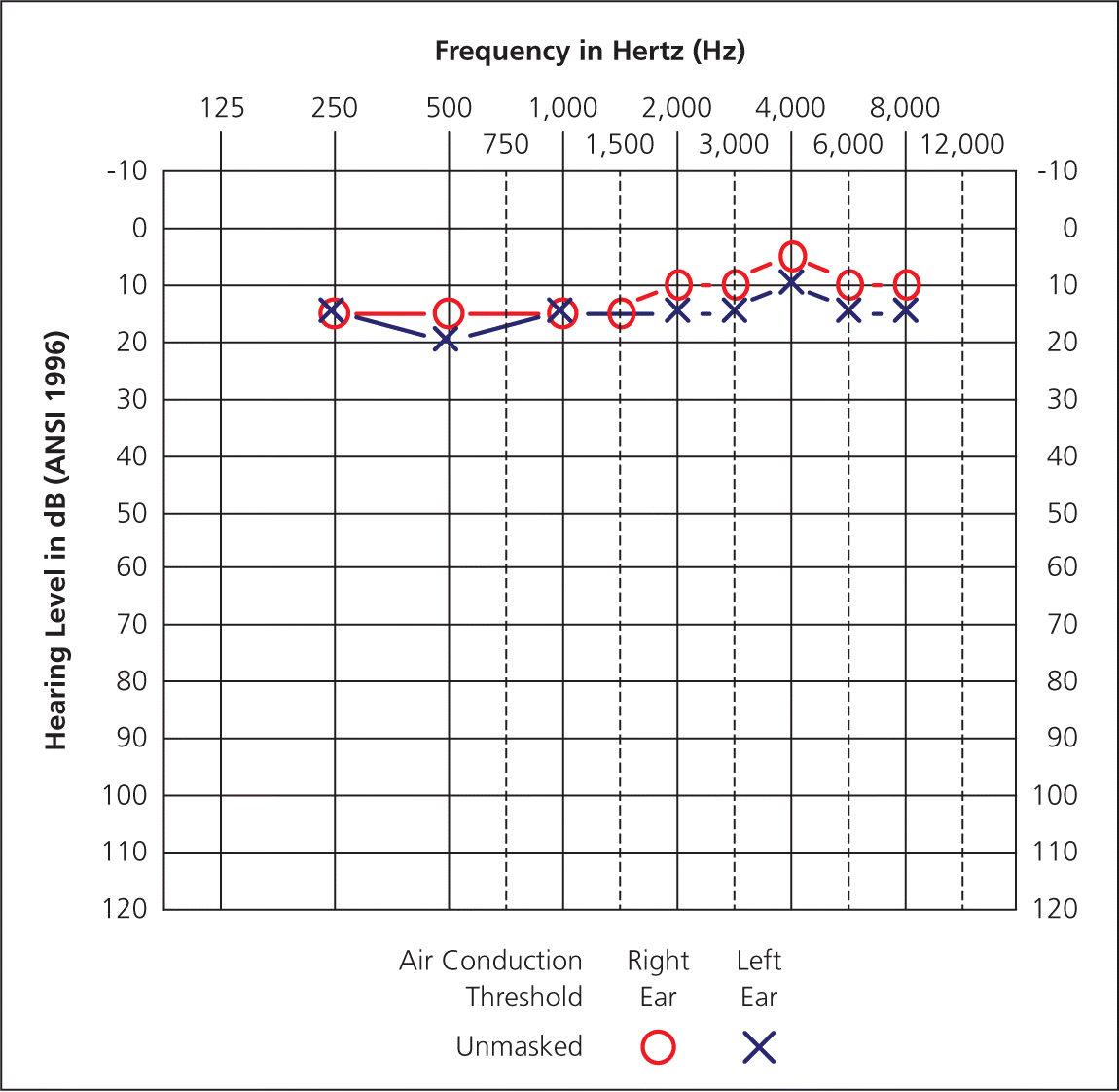
When the patient is retested in a quiet area that meets American National Standards Institute specifications, hearing levels are within normal limits.
EQUIPMENT
Several types of audiometers are available for purchase, ranging from handheld screening audiometers to those with full diagnostic capabilities extending to higher frequencies. Screening audiometers for office use, for example, generally test at frequencies in the speech range of 500 to 4,000 Hz.
There are many purchase options to consider for earphones and transducers. Circumaural headphones have a cushion covering the entire external ear. These help reduce background noise when the testing environment is not ideal. Supra-aural headphones sit directly on the pinna, and are the least effective headphone at attenuating background noise. Insert earphones are inserted directly into the ear canal. They reduce the possibility of collapsing canals, provide some background noise attenuation, and reduce the possibility of sound detection from the opposite ear.
All audiometers and audiometric equipment require annual calibrations to meet ANSI specifications.22 Audiometer supplier information is listed in Table 1.
Table 1. Audiometer Suppliers

| Grason-Stadler, Inc. | |
| http://www.grason-stadler.com | |
| 800-700-2282 | |
| Handtronix | |
| http://www.handtronix.com | |
| 866-950-2573 | |
| Maico Diagnostics | |
| http://www.maico-diagnostics.com | |
| 888-941-4201 | |
| Micro Audiometrics | |
| http://www.microaud.com | |
| 800-729-9509 | |
| Welch Allyn, Inc. | |
| http://www.welchallyn.com | |
| 800-535-6663 | |
PERSONNEL
Support personnel can be trained to perform audiometry in formal courses lasting 20 hours.23 Physicians should check with their state and local agencies for licensing requirements of audiometry personnel. In the absence of state or local requirements, guidelines for the use of support personnel to perform audiometry are listed in Table 2.24–26
Table 2. Guidelines for the Use of Support Personnel to Perform Audiometry

| American Academy of Audiology | Support personnel are defined as “people who, after appropriate training, perform tasks that are prescribed, directed, and supervised by an audiologist.”24 |
| American Academy of Otolaryngology–Head and Neck Surgery | “Technicians can only perform diagnostic tests that do not require the skills of an audiologist…. Technicians must be under the direct supervision of a physician.”25 |
| American Speech-Language-Hearing Association (ASHA) | “Regardless of job title, preparation, tasks, and other credentials, all persons who provide support services in audiology and speech-language pathology should be directed and supervised by ASHA-certified audiologists and/or speech-language pathologists.”26 |
PATIENT HISTORY
Patients may feign or exaggerate hearing loss for personal reasons, and may intentionally or unintentionally misreport on testing. Patients with constant, bothersome tinnitus (ringing or buzzing in the ears) often have difficulty discerning pure tones. Many combat veterans have a history of blast exposures, mild concussion, or posttraumatic stress disorder.27–29 These patients may have difficulty completing audiometry for reasons related to headaches, memory problems, irritability, or fatigue. Taking a history before the hearing test will alert the physician to these possibilities. Supplemental, objective tests such as evoked otoacoustic emissions testing (stimulation of hair cells to produce sound) and patient questionnaires can assist with difficult-to-test populations.30
Recent noise exposure before pure-tone testing may affect the validity of the test results. Riding a loud motorcycle or listening to music through headphones may result in a temporary hearing threshold shift, and may not reflect the patient's true hearing thresholds. Patients should minimize or avoid exposure to loud noise for at least 14 hours before pure-tone testing.31
PHYSICAL FINDINGS
Audiometry results may be affected in patients with anatomic anomalies, such as narrow or collapsing ear canals (stenosis of the ear canal), complete canal occlusion, or absence of an ear canal (atresia). Impacted cerumen can cause a conductive hearing loss (Figure 1) that typically resolves following cerumen removal. Collapsed ear canals occur in many older patients whose cartilage has become flaccid. Placing an over-the-ear headphone over already narrow or closed ear canals may add sufficient pressure to collapse the ear canals even further, resulting in a false high-frequency hearing loss. An otoscopic examination should be performed before the hearing test to ensure that the tympanic membrane is at least partially visible.
Differentiating conductive hearing loss from sensorineural hearing loss requires bone conduction testing. Audiometry relies on techniques similar to the Weber and Rinne tests to compare air and bone conduction. Bone conduction audiometry measures pure-tone thresholds using a mechanical device that transmits sounds via vibration through the forehead or mastoid bone. Figures 2A and 2B demonstrate differences in air and bone conduction thresholds (an air-bone gap) for a patient with a tympanic membrane rupture.32 Figures 3A and 3B illustrate no air-bone gap for a patient with bilateral hearing loss. Unilateral or asymmetrical hearing loss (Figures 4A and 4B) can be symptomatic of a central nervous system lesion, including vestibular schwannoma (commonly though incorrectly called an acoustic neuroma), and warrants additional evaluation and imaging.33,34
If the pure-tone threshold difference or asymmetry between ears at any frequency is equal to or greater than 40 dB, the sound energy from the test ear can stimulate the nontest ear, causing the nontest ear to respond to the stimulus. To prevent this crossover of sound from one ear to the other, narrow band noise is presented to the nontest ear and thresholds are recorded as masked.32 Right ear masked air conduction thresholds are manually recorded as a red triangle on the audiogram. Left ear masked air conduction thresholds are manually recorded as a blue box. Right ear masked bone conductions are manually recorded as a red square bracket (open on the right side). Left ear masked bone conduction thresholds are manually recorded as a blue square bracket (open on the left side). Figures 4A and 4B show masked bone conduction thresholds in the left ear.
Table 3. Educational Resources for Hearing Conservation

| Association | Description | |
|---|---|---|
| American Academy of Audiology | Consumer guides including a fact sheet on noise-induced hearing loss; position statement on preventing noise-induced occupational hearing loss | |
| http://www.audiology.org/ | ||
| National Hearing Conservation Association | Practical guides on hearing conservation related to music, firearms, farming, children, and noise; Noise Destroys poster of damaged hair cells within the cochlea | |
| http://www.hearingconservation.org/ | ||
| National Institute for Occupational Safety and Health | Noise and Hearing Loss Prevention: current research, training tools, frequently asked questions, and more | |
| http://www.cdc.gov/niosh/topics/noise/ | ||
| National Institute on Deafness and Other Communication Disorders | Ten Ways to Recognize Hearing Loss patient questionnaire | |
| http://www.nidcd.nih.gov/health/hearing/10ways.aspx | ||
Additional audiometric testing by an audiologist is recommended for patients whose pure-tone thresholds fall outside the range of normal limits.35
Reimbursement Considerations
Pure-tone audiometry threshold diagnostic testing of both ears (interpreted as pass/fail) should be billed under Current Procedural Terminology (CPT) code 92552 (pure tone audiometry [threshold]; air only) or 92553 for Medicare reimbursement.36 The average reimbursement for pure-tone audiometry threshold diagnostic testing of both ears is $28.71. Medicare does not cover the pure-tone audiometry screening test of both ears under CPT code 92551 (screening test, pure tone, air only).36 For non-Medicare claims, testing will be billed under the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) diagnosis code 389.9 (unspecified hearing loss).37,38 Private insurance companies may cover this service as billed under the ICD-9-CM code V72.1 (special investigations and examinations; examination of ears and hearing).39
As part of a preventive approach to hearing loss, physicians may consider placing educational materials on hearing loss prevention, and a dispenser of earplugs for patients to use when anticipating exposure to loud noise, in their office waiting rooms. Table 3 provides a sample of educational resources for hearing conservation.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms audiometry, screening, prevalence, and hearing loss. The search included meta-analyses, cross-sectional studies, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, and the National Guideline Clearinghouse, and Cochrane Database of Systematic Reviews. Search date: September 2011.

