The health maintenance examination is an opportunity to focus on disease prevention and health promotion. The patient history should include screening for tobacco use, alcohol misuse, intimate partner violence, and depression. Premenopausal women should receive preconception counseling and contraception as needed, and all women planning or capable of pregnancy should take 400 to 800 mcg of folic acid per day. High-risk sexually active women should be counseled on reducing the risk of sexually transmitted infections, and screened for chlamydia, gonorrhea, and syphilis. All women should be screened for human immunodeficiency virus. Adults should be screened for obesity and elevated blood pressure. Women 20 years and older should be screened for dyslipidemia if they are at increased risk of coronary heart disease. Those with sustained blood pressure greater than 135/80 mm Hg should be screened for type 2 diabetes mellitus. Women 55 to 79 years of age should take 75 mg of aspirin per day when the benefits of stroke reduction outweigh the increased risk of gastrointestinal hemorrhage. Women should begin cervical cancer screening by Papanicolaou test at 21 years of age, and if results have been normal, screening may be discontinued at 65 years of age or after total hysterectomy. Breast cancer screening with mammography may be considered in women 40 to 49 years of age based on patients' values, and potential benefits and harms. Mammography is recommended biennially in women 50 to 74 years of age. Women should be screened for colorectal cancer from 50 to 75 years of age. Osteoporosis screening is recommended in women 65 years and older, and in younger women with a similar risk of fracture. Adults should be immunized at recommended intervals according to guidelines from the Centers for Disease Control and Prevention.
The health maintenance examination is an opportunity to spend focused time with patients on disease prevention and health promotion. There is no consensus on the optimal frequency, though most patients and physicians think that a yearly physical examination is important and necessary.1,2 One review found that an annual examination improves delivery of recommended preventive services, and may lessen patient worry.3 It is also a chance for physicians to strengthen their relationship with patients and to provide a medical home. Physicians may use this time to discuss issues such as family relationships or end-of-life care.
This article reviews several evidence-based recommendations to help physicians select services that best promote health in asymptomatic women. These recommendations come primarily from the U.S. Preventive Services Task Force (USPSTF) and are supported by the American Academy of Family Physicians (AAFP). Other professional societies may publish guidelines that agree or conflict with USPSTF recommendations; the most relevant are described here.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References | |
|---|---|---|---|
| Physicians should ask all adults about tobacco use and provide tobacco cessation interventions for those who use tobacco products. | A | 4 | |
| Physicians should screen all adults for alcohol misuse and provide behavioral counseling interventions to reduce alcohol misuse in individuals who engage in risky or hazardous drinking. | B | 5 | |
| Physicians should screen women of childbearing age for intimate partner violence, and those who screen positive should be provided with or referred to intervention services. | B | 9 | |
| Physicians should screen adults for depression when staff-assisted depression care supports are in place to ensure accurate diagnosis, effective treatment, and follow-up. | B | 10 | |
| All women planning or capable of pregnancy should take a daily folic acid supplement of 400 to 800 mcg. | A | 14 | |
| High-risk sexually active adults should be counseled on risk reduction for sexually transmitted infections. | B | 15, 16 | |
| High-risk women should be screened for: | |||
| Chlamydia (including all sexually active women 24 years and younger) | A | 17 | |
| Gonorrhea | B | 18 | |
| Syphilis | A | 19 | |
| All adults 65 years and younger should be screened for human immunodeficiency virus. | A | 20, 21 | |
| Adults should be screened for elevated body mass index. Patients with obesity should be offered intensive counseling and behavioral interventions to promote sustained weight loss. | B | 25 | |
| Adults should be screened for high blood pressure. | A | 27, 28 | |
| Women 45 years and older should be screened for dyslipidemia if at increased risk of CHD. | A | 32, 33 | |
| Women 20 to 45 years of age should be screened for dyslipidemia if at increased risk of CHD. | B | 32, 33 | |
| Asymptomatic adults with sustained blood pressure greater than 135/80 mm Hg (treated or untreated) should be screened for type 2 diabetes mellitus. | B | 36 | |
| Women 55 to 79 years of age should take approximately 75 mg of aspirin per day when the net benefit of ischemic stroke reduction outweighs the increased risk of gastrointestinal hemorrhage. | A | 38 | |
| Women should be screened for cervical cancer with Pap tests beginning at 21 years of age. Low-risk women should receive Pap testing every three years. Co-testing for human papillomavirus is an option beginning at 30 years of age, and can extend the screening interval to five years. Cervical cancer screening should be discontinued at 65 years of age or after total hysterectomy if the woman has a benign gynecologic history. | A | 40–43 | |
| Women 50 to 74 years of age should be screened for breast cancer with mammography biennially. | B | 44, 45 | |
| Mammography should be considered in women 40 to 49 years of age based on each patient's values and the potential benefits and harms. | C | 44, 45 | |
| Adults 50 to 75 years of age should be screened for colorectal cancer with an FOBT annually, sigmoidoscopy every five years with an FOBT every three years, or colonoscopy every 10 years. | A | 48, 49 | |
| Routine screening for ovarian cancer with bimanual examination, transvaginal ultrasonography, or cancer antigen 125 testing is not recommended. | B | 52, 53 | |
| Women 65 years and older should be screened for osteoporosis. Women younger than 65 years should be screened if the risk of fracture is greater than or equal to that of a 65-year-old white woman without additional risk factors. | B | 55, 56 | |
CHD = coronary heart disease; FOBT = fecal occult blood test; Pap = Papanicolaou.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
History
During the health maintenance examination, the patient's medical, social, and family histories should be discussed, in addition to a comprehensive review of systems to find pertinent risk factors that will guide screening and counseling recommendations. Medications should be reconciled and allergies reviewed.
Physicians should ask all adults about tobacco use and provide cessation interventions for those who use tobacco products.4 Patients should be screened for alcohol misuse; the CAGE questionnaire and AUDIT-C screening test are tools that have been validated in a primary care setting.5–7 Behavioral counseling interventions to reduce alcohol misuse should be provided to those who engage in risky or hazardous drinking.5 There is insufficient evidence to recommend routine screening for illicit drug use, although physicians should be alert to suggestive signs or symptoms.8 The USPSTF has provisionally recommended that physicians screen women of childbearing age for intimate partner violence, based on evidence that effective interventions can reduce violence, abuse, and physical and mental harms.9 Women who screen positive should be provided with or referred to intervention services.9
Adults should be screened for depression when the office has support to ensure accurate diagnosis, effective treatment, and follow-up through care coordination, case management, or mental health treatment.10 Asking patients “Over the past two weeks, have you felt down, depressed, or hopeless?” and “Over the past two weeks, have you felt little interest or pleasure in doing things?” has been found to be an effective way to screen for depression. An affirmative response to either question should prompt further evaluation for depression.11
Family Planning
Premenopausal women should be asked about their reproductive plans. If the patient does not currently want to get pregnant, options for contraception should be reviewed. For those who are attempting to conceive, medical history, family history, weight, nutrition, immunization status, environmental exposures, sexually transmitted infection (STI) risk, and substance use should be reviewed and appropriate counseling provided.12,13 To reduce the incidence of neural tube defects, all women planning or capable of pregnancy should take a folic acid supplement of 400 to 800 mcg per day.14 Physicians may choose to counsel women on expectations of perimenopause and menopause, when relevant.
Sexually Transmitted Infections
High-risk sexually active adults include those with multiple partners, those who have an STI or have had one within the past year, and those in a nonmonogamous relationship living in an area with a high rate of STIs. These patients should receive intensive behavioral counseling (more than 30 minutes in one session or delivered in multiple sessions in a health care or community setting) focused on abstinence, condom use, limiting the number of sex partners, modification of sexual practices, and vaccination to reduce transmission of STIs.15,16 According to the USPSTF, high-risk women should be screened at least annually for chlamydia, gonorrhea, and syphilis, and all sexually active women 24 years and younger should be screened annually for chlamydia.17–19 The USPSTF and Centers for Disease Control and Prevention (CDC) recommend screening all adolescents and adults through 65 years of age for human immunodeficiency virus.20,21
Coronary Heart Disease
Heart disease is the leading cause of death in U.S. women.22 In addition to a review of medical and family history and tobacco use status, adults should receive targeted screening for other coronary heart disease (CHD) risk factors, including overweight or obesity, hypertension, dyslipidemia, and diabetes mellitus. In adults without preexisting cardiovascular disease or risk factors, medium- to high-intensity behavioral counseling to promote a healthful diet and physical activity for cardiovascular disease prevention has demonstrated only a small health benefit.23 Therefore, the USPSTF advises physicians to consider selective rather than routine counseling, depending on other health care and preventive service priorities.23
OVERWEIGHT AND OBESITY
The disease burden associated with obesity has grown in proportion to the increasing weight of the U.S. population; in 2009 to 2010, approximately one-third of U.S. adults were obese.24 Elevated body mass index (BMI) is a marker of unhealthy weight, and all adults should be screened for elevated BMI. A BMI between 25 and 29.9 kg per m2 is defined as overweight, and a BMI of 30 kg per m2 or greater indicates obesity.25 A BMI calculator is available at http://www.nhlbisupport.com/bmi/.26 The USPSTF recommends that physicians refer patients who are obese to intensive, multicomponent behavioral interventions. Components of such interventions include setting weight-loss goals, improving diet or nutrition, participating in physical activity sessions, addressing barriers to change, actively self-monitoring, and strategizing how to maintain lifestyle changes.25
HYPERTENSION
The risks of uncontrolled hypertension include premature death, heart attack, renal insufficiency, and stroke. The USPSTF recommends screening for elevated blood pressure (greater than 140/90 mm Hg) in all adults 18 years and older.27 The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure recommends screening every other year in adults with normal blood pressure (less than 120/80 mm Hg) and yearly in those with prehypertension (systolic of 120 to 139 mm Hg; diastolic of 81 to 90 mm Hg).28
DYSLIPIDEMIA
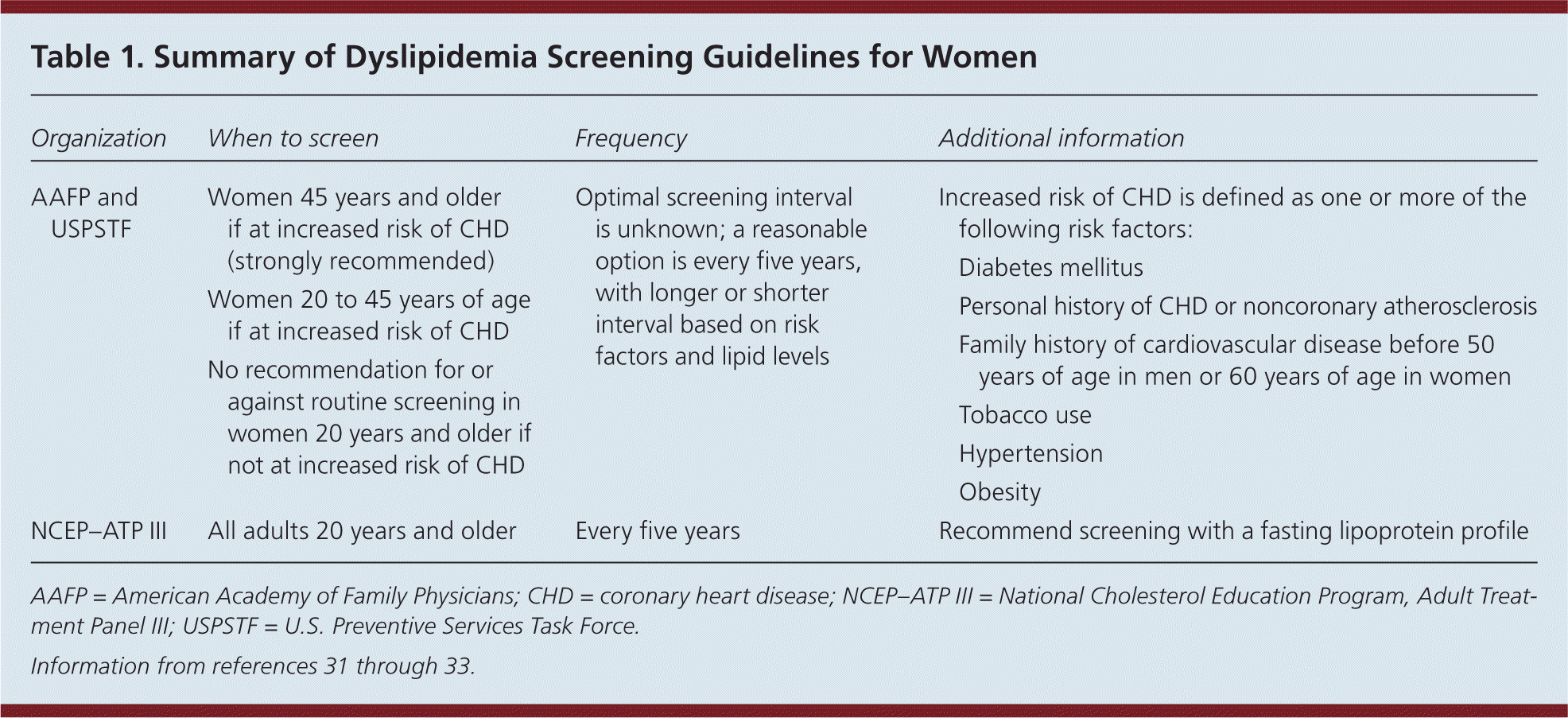
Dyslipidemias, including high levels of low-density lipoprotein cholesterol and low levels of high-density lipoprotein cholesterol, are known risk factors for CHD. There is evidence that lipid-lowering therapy reduces the risk of developing CHD, though there is ongoing debate on the benefit of primary prevention.29–31 The AAFP and USPSTF recommend screening women 20 years and older for dyslipidemia only if they are at increased risk of CHD.32,33 Screening guidelines from the USPSTF and AAFP, and from the National Cholesterol Education Program, Adult Treatment Panel III are outlined in Table 1.31–33
Table 1. Summary of Dyslipidemia Screening Guidelines for Women
| Organization | When to screen | Frequency | Additional information | |
|---|---|---|---|---|
| AAFP and USPSTF |
| Optimal screening interval is unknown; a reasonable option is every five years, with longer or shorter interval based on risk factors and lipid levels | Increased risk of CHD is defined as one or more of the following risk factors:
| |
| NCEP–ATP III |
| Every five years | Recommend screening with a fasting lipoprotein profile | |
AAFP = American Academy of Family Physicians; CHD = coronary heart disease; NCEP–ATP III = National Cholesterol Education Program, Adult Treatment Panel III; USPSTF = U.S. Preventive Services Task Force.
TYPE 2 DIABETES
An estimated 13.3 percent of women older than 20 years have type 2 diabetes, and the prevalence is increasing.34,35 More than one-third of these women are undiagnosed.35 However, the benefit of screening and treating asymptomatic women remains controversial. The USPSTF recommends screening for type 2 diabetes in asymptomatic adults with sustained blood pressure greater than 135/80 mm Hg (treated or untreated), but found insufficient evidence to support routine screening for asymptomatic adults with a blood pressure below this level.36 The American Diabetes Association recommends screening in persons at risk of type 2 diabetes.37 Recommendations from both organizations are summarized in Table 2.36,37 Screening tests include A1C level, fasting plasma glucose level, and two-hour 75-g oral glucose tolerance test.37
Table 2. Summary of Type 2 Diabetes Mellitus Screening Guidelines for Women

| Organization | When to screen | Frequency | |
|---|---|---|---|
| ADA | All adults beginning at 45 years of age |
| |
All adults with body mass index ≥ 25 kg per m2 and one of the following additional risk factors:
| |||
| USPSTF | Asymptomatic adults with sustained blood pressure (treated or untreated) > 135/80 mm Hg |
| |
| Insufficient evidence to recommend for or against screening adults with blood pressure ≤ 135/80 mm Hg | |||
ADA = American Diabetes Association; USPSTF = U.S. Preventive Services Task Force.
Stroke Prevention
The USPSTF recommends that women 55 to 79 years of age take approximately 75 mg of aspirin per day when the net benefit of ischemic stroke reduction outweighs the increased risk of gastrointestinal hemorrhage.38 A tool to help determine an individual's risk of stroke is available at http://www.westernstroke.org/PersonalStrokeRisk1.xls.
Cancer Screening
Cancer is the second leading cause of death in the United States, accounting for nearly one in every four deaths.39 For select cancers, screening can lead to early diagnosis and the greatest chance of survival. Screening for average-risk women is outlined here. Women who have a family history of cancer or other risk factors (i.e., a history of high-dose chest radiation, diethylstilbestrol exposure in utero, or immunosuppression) may require different screening paradigms.
CERVICAL CANCER
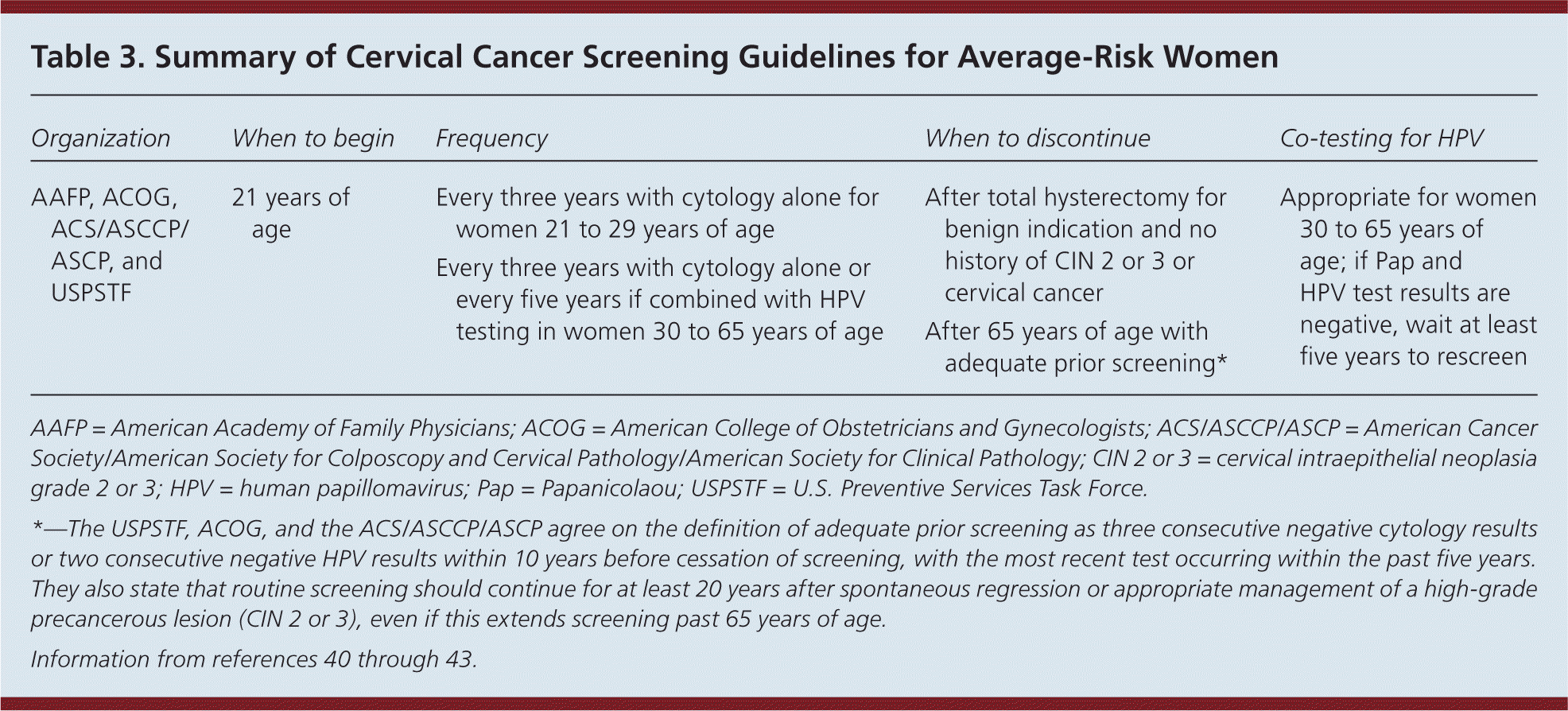
Incidence and mortality rates of cervical cancer have decreased because of prevention and screening with Papanicolaou (Pap) tests.39 Women should be screened for cervical cancer with Pap tests beginning at 21 years of age. Low-risk women should receive Pap testing every three years. Co-testing for human papillomavirus is an option beginning at 30 years of age, and can extend the screening interval to five years. Cervical cancer screening should be discontinued at 65 years of age or after total hysterectomy if the woman has a benign gynecologic history.40,41 Table 3 summarizes clinical recommendations for cervical cancer screening.40–43
Table 3. Summary of Cervical Cancer Screening Guidelines for Average-Risk Women
| Organization | When to begin | Frequency | When to discontinue | Co-testing for HPV |
|---|---|---|---|---|
| AAFP, ACOG, ACS/ASCCP/ASCP, and USPSTF | 21 years of age |
|
| Appropriate for women 30 to 65 years of age; if Pap and HPV test results are negative, wait at least five years to rescreen |
AAFP = American Academy of Family Physicians; ACOG = American College of Obstetricians and Gynecologists; ACS/ASCCP/ASCP = American Cancer Society/ American Society for Colposcopy and Cervical Pathology/American Society for Clinical Pathology; CIN 2 or 3 = cervical intraepithelial neoplasia grade 2 or 3; HPV = human papillomavirus; Pap = Papanicolaou; USPSTF = U.S. Preventive Services Task Force.
*—The USPSTF, ACOG, and the ACS/ ASCCP/ ASCP agree on the definition of adequate prior screening as three consecutive negative cytology results or two consecutive negative HPV results within 10 years before cessation of screening, with the most recent test occurring within the past five years. They also state that routine screening should continue for at least 20 years after spontaneous regression or appropriate management of a high-grade precancerous lesion (CIN 2 or 3), even if this extends screening past 65 years of age.
BREAST CANCER
Breast cancer is the second most commonly diagnosed cancer in women.39 Small tumors confined to the breast are more likely to be successfully treated. In women 40 to 49 years of age, the USPSTF recommends shared decision making about whether to start mammography, taking into account patients' values and potential benefits and harms. Compared with older women, screening women 40 to 49 years of age results in a lower absolute reduction in breast cancer mortality and higher rates of false-positive results.44 The USPSTF and AAFP recommend routine biennial screening beginning at 50 years of age with discontinuation at 75 years of age.44,45 The American College of Obstetricians and Gynecologists (ACOG) and the American Cancer Society recommend annual screening beginning at 40 years of age without a specific discontinuation age.46,47 In contrast to ACOG's recommendations, the USPSTF has found insufficient evidence to assess the benefits and harms of clinical breast examination, and recommends against teaching breast self-examination.44,46 eTable A summarizes clinical recommendations for breast cancer screening.
eTable A. Summary of Breast Cancer Screening Guidelines for Average-Risk Women
| Organization | Mammography | Clinical breast examination | Breast self-examination | ||
|---|---|---|---|---|---|
| When to begin | Frequency | When to discontinue | |||
| AAFP and USPSTF | 50 years of age; consider at 40 to 49 years of age based on discussion of values, benefits, and harms | Biennially | Insufficient evidence to recommend for or against screening in women 75 years and older | Insufficient evidence to recommend for or against | Recommend against |
| ACOG | 40 years of age | Yearly | No recommendation; consider medical comorbidity and life expectancy when screening women 75 years and older | Every one to three years for women 20 to 39 years of age | Encourage breast self-awareness, which can include self-examination |
| Yearly for women 40 years and older | |||||
| ACS | 40 years of age | Yearly | Continue as long as the patient is in good health | Every three years for women 20 to 39 years of age | Optional, starting at 20 years of age |
| Yearly for women 40 years and older | |||||
AAFP = American Academy of Family Physicians; ACOG = American College of Obstetricians and Gynecologists; ACS = American Cancer Society; USPSTF = U.S. Preventive Services Task Force.
Information from:
American Academy of Family Physicians. Clinical preventive services. Breast cancer. 2009. https://www.aafp.org/patient-care/clinical-recommendations/all/breast-cancer.html. Accessed February 7, 2012.
U.S. Preventive Services Task Force. Screening for breast cancer. November 2009. http://www.uspreventiveservicestaskforce.org/uspstf/uspsbrca.htm. Accessed January 12, 2012.
American College of Obstetricians-Gynecologists. Practice bulletin no. 122: Breast cancer screening. Obstet Gynecol. 2011;118(2 pt 1):372–382.
American Cancer Society. Breast cancer: early detection. 2011. http://www.cancer.org/Cancer/BreastCancer/MoreInformation/BreastCancerEarlyDetection/breast-cancer-early-detection-toc. Accessed January 11, 2012.
COLORECTAL CANCER
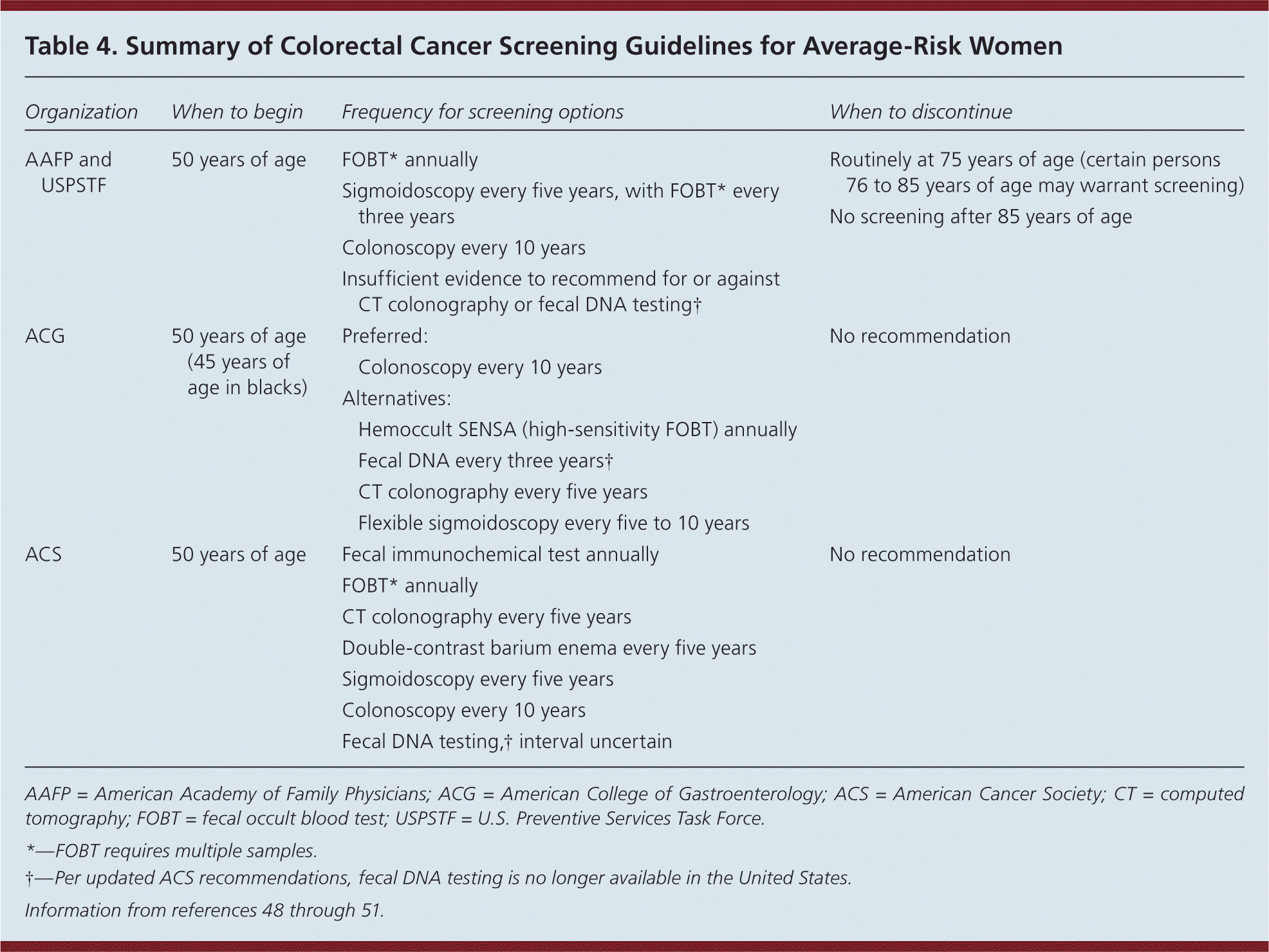
Colorectal cancer mortality rates have decreased in the past 20 years, likely secondary to improved screening and treatment options. Adults 50 to 75 years of age should undergo screening. Per USPSTF recommendations, fecal occult blood test (annually), sigmoidoscopy (every five years) plus fecal occult blood test (every three years), and colonoscopy (every 10 years) are acceptable methods of screening.48,49 Because each method entails different risks, benefits, costs, and availability, the choice should be based on patient preference. When any other initial screening result is positive, colonoscopy is the next recommended step in evaluation. Of note, digital rectal examination is not recommended for colorectal cancer screening. Table 4 summarizes clinical recommendations for colorectal cancer screening.48–51
Table 4. Summary of Colorectal Cancer Screening Guidelines for Average-Risk Women
| Organization | When to begin | Frequency for screening options | When to discontinue | |
|---|---|---|---|---|
| AAFP and USPSTF | 50 years of age | FOBT* annually |
| |
| Sigmoidoscopy every five years, with FOBT* every three years | ||||
| Colonoscopy every 10 years | ||||
| Insufficient evidence to recommend for or against CT colonography or fecal DNA testing† | ||||
| ACG | 50 years of age (45 years of age in blacks) | Preferred: |
| |
| Colonoscopy every 10 years | ||||
| Alternatives: | ||||
| Hemoccult SENSA (high-sensitivity FOBT) annually | ||||
| Fecal DNA every three years† | ||||
| CT colonography every five years | ||||
| Flexible sigmoidoscopy every five to 10 years | ||||
| ACS | 50 years of age | Fecal immunochemical test annually |
| |
| FOBT* annually | ||||
| CT colonography every five years | ||||
| Double-contrast barium enema every five years | ||||
| Sigmoidoscopy every five years | ||||
| Colonoscopy every 10 years | ||||
| Fecal DNA testing,† interval uncertain | ||||
AAFP = American Academy of Family Physicians; ACG = American College of Gastroenterology; ACS = American Cancer Society; CT = computed tomography; FOBT = fecal occult blood test; USPSTF = U.S. Preventive Services Task Force.
*—FOBT requires multiple samples.
†—Per updated ACS recommendations, fecal DNA testing is no longer available in the United States.
OVARIAN CANCER
Routine screening for ovarian cancer with bimanual examination, transvaginal ultrasonography, or cancer antigen 125 testing is not recommended. It does not reduce ovarian cancer mortality, and leads to complications from diagnostic evaluation of false-positive results.52,53
Osteoporosis Screening and Prevention
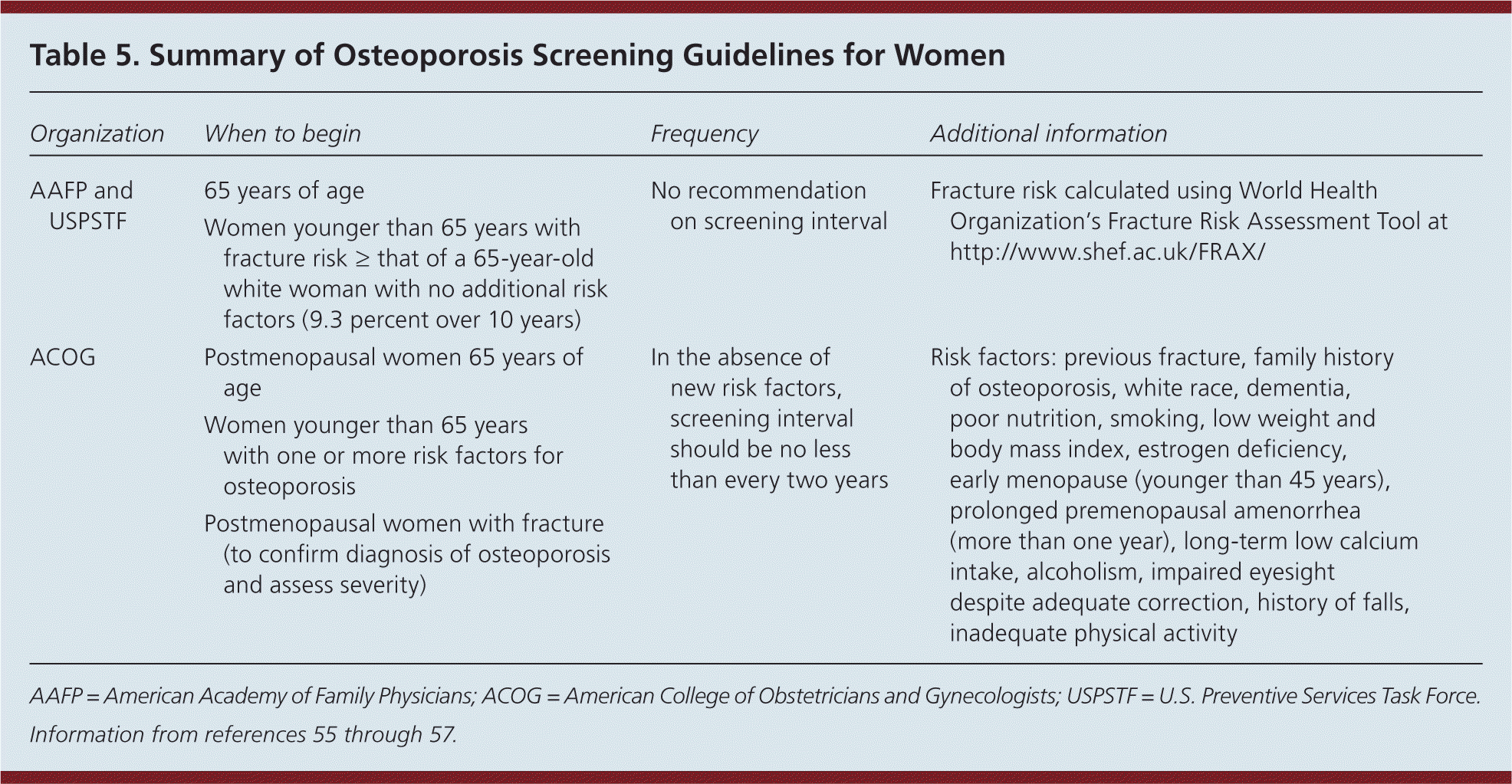
In 2010, osteoporosis and osteopenia affected an estimated 35 million women older than 50 years. This number is expected to increase to 41 million by 2020.54 Screening with dual energy x-ray absorptiometry (DEXA) is recommended for women 65 years and older. Additionally, the USPSTF recommends using the World Health Organization's Fracture Risk Assessment Tool to risk-stratify women younger than 65 years. Screening younger women is recommended if the risk of fracture is greater than or equal to that of a 65-year-old white woman without additional risk factors (9.3 percent over 10 years).55,56 ACOG also recommends that the decision to screen women younger than 65 years be based on specific risk factor assessment.57 Table 5 summarizes recommendations for osteoporosis screening.55–57
Table 5. Summary of Osteoporosis Screening Guidelines for Women
| Organization | When to begin | Frequency | Additional information |
|---|---|---|---|
| AAFP and USPSTF | 65 years of age | No recommendation on screening interval | Fracture risk calculated using World Health Organization's Fracture Risk Assessment Tool at http://www.shef.ac.uk/FRAX/ |
| Women younger than 65 years with fracture risk ≥ that of a 65-year-old white woman with no additional risk factors (9.3 percent over 10 years) | |||
| ACOG | Postmenopausal women 65 years of age | In the absence of new risk factors, screening interval should be no less than every two years | Risk factors: previous fracture, family history of osteoporosis, white race, dementia, poor nutrition, smoking, low weight and body mass index, estrogen deficiency, early menopause (younger than 45 years), prolonged premenopausal amenorrhea (more than one year), long-term low calcium intake, alcoholism, impaired eyesight despite adequate correction, history of falls, inadequate physical activity |
| Women younger than 65 years with one or more risk factors for osteoporosis | |||
| Postmenopausal women with fracture (to confirm diagnosis of osteoporosis and assess severity) |
AAFP = American Academy of Family Physicians; ACOG = American College of Obstetricians and Gynecologists; USPSTF = U.S. Preventive Services Task Force.
A 2011 meta-analysis conducted for the USPSTF found that calcium and vitamin D supplements may reduce fracture risk in older adults.58 However, a 2012 USPSTF draft recommendation statement concluded that the current evidence is insufficient to assess the risks and benefits of calcium and vitamin D supplementation for prevention of fracture in premenopausal and noninstitutionalized postmenopausal women.59 Formal recommendation is forthcoming. The National Institutes of Health recommends a total daily intake of 1,000 mg of calcium for women 19 to 50 years of age, and 1,200 mg for women older than 50 years, in addition to 600 to 800 IU of vitamin D.60,61 ACOG recommends counseling women on other modifiable osteoporosis risk factors, including regular weight-bearing and muscle-strengthening exercises, smoking cessation, moderation of alcohol intake, and fall-prevention strategies.57
Immunizations
The AAFP recommends immunizing all adults at recommended intervals, unless the vaccine is contraindicated in an individual patient.62 The CDC's Advisory Committee on Immunization Practices releases yearly recommendations for adult immunizations, which are available at http://www.cdc.gov/vaccines/schedules/easy-to-read/adult.html.63 The CDC's annual updates to the immunization schedule will be published February 1, 2013. Immunization status should be reviewed at the health maintenance examination and at visits for routine medical care.
Data Sources: A literature search was performed on health maintenance topics in women that focused on the USPSTF guidelines and the AAFP clinical preventive services policy recommendations. Also reviewed were recommendations from the National Institutes of Health; the CDC's Advisory Committee on Immunization Practices; the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; and the National Cholesterol Education Program, Adult Treatment Panel III. Preventive care guidelines from other specialty groups that were reviewed include ACOG, the American College of Gastroenterology, the American Cancer Society, and the American Diabetes Association. Search dates: between December 2011 and November 2012.

