Obesity is a common condition that is associated with numerous medical problems such as cardiovascular disease, pulmonary disease, and diabetes mellitus. Primary care physicians have an important role in helping patients develop a successful weight loss plan to improve their overall health. Dietary strategies emphasizing reduced caloric intake, regardless of the nutrient composition, are important for weight loss. Behavioral interventions such as motivational interviewing and encouraging physical activity lead to additional weight loss when combined with dietary changes. Medication regimens for concomitant medical problems should take into account the effect of specific agents on the patient's weight. Persons with a body mass index of 30 kg per m2 or greater or 27 kg per m2 or greater with comorbidities who do not succeed in losing weight with diet and activity modifications may consider medication to assist with weight loss. Medications approved for long-term treatment of obesity include orlistat, lorcaserin, liraglutide, phentermine/topiramate, and naltrexone/bupropion. Physicians should consider referring patients for bariatric surgery if they have a body mass index of 40 kg per m2 or greater. For those with obesity-related comorbid conditions, patients should be considered for adjustable gastric banding or other bariatric surgical approaches if they have a body mass index of 30 to 39.9 kg per m2. The most commonly performed procedures for weight loss are Roux-en-Y gastric bypass, sleeve gastrectomy, and adjustable gastric banding. Bariatric surgery is the most effective intervention for weight loss in obese patients, and it leads to improvement in multiple obesity-related conditions, including remission of diabetes.
Obesity is a pervasive problem confronting patients and their physicians. From 2011 to 2012, 69% of U.S. adults were overweight or obese.1 Many common medical problems, such as diabetes mellitus, pulmonary disease, and cardiovascular disease, are related to obesity and can improve with weight loss.2 The management of obesity continues to evolve with the approval of new treatments. This review will provide answers to some of the common clinical questions that physicians encounter when managing obesity in the outpatient setting.
WHAT IS NEW ON THIS TOPIC: OBESITY
Using a single dietary adjustment may produce weight loss similar to more complex plans. For example, encouraging a patient to increase dietary fiber intake produces comparable adherence and weight loss to encouraging compliance with the many goals of the American Heart Association diet.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| BMI should be calculated for all patients 18 years and older, and those with obesity should be referred for intensive, multicomponent behavioral interventions. | B | 2 |
| Increased physical activity should be recommended for weight loss in combination with diet and behavioral modifications. | B | 20 |
| Physicians should consider medications for weight loss in patients with a BMI of 30 kg per m2 or greater, or 27 kg per m2 or greater who also have comorbidities and have unsuccessfully tried diet and lifestyle modification first. | C | 26 |
| Patients with a BMI of 40 kg per m2 or greater and those with a BMI greater than 35 kg per m2 who also have obesity-related comorbidities should be referred for consideration of bariatric surgery. Patients with a BMI greater than 30 kg per m2 who also have obesity-related comorbidities may be candidates for adjustable gastric banding. | B | 36 |
BMI = body mass index.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
What Is the Family Physician's Role in Screening for and Managing Obesity?
Physicians should screen all patients for obesity with measurement of body mass index (BMI) or waist circumference. Diet and behavioral interventions should be initiated in patients who are obese.
EVIDENCE SUMMARY
The U.S. Preventive Services Task Force (USPSTF) recommends that all persons 18 years and older be screened for obesity (Table 11,3), and that those with a BMI of 30 kg per m2 or greater be offered intensive, multicomponent behavioral interventions.2 The American Academy of Family Physicians recommends screening for obesity followed by intensive counseling and behavioral interventions, with at least one session per month for at least three months.4 Waist circumference may be an acceptable alternative in some persons because BMI may not account for the cardiovascular risk of central adiposity. Family physicians can assist patients in setting weight loss goals, improving nutrition, increasing physical activity, addressing barriers to change, and developing strategies to maintain long-term lifestyle changes. Behavior modifications can lead to clinically important weight loss of 5%, improved glucose tolerance, and reduction in other cardiovascular risk factors.2
Table 1. Weight Classifications
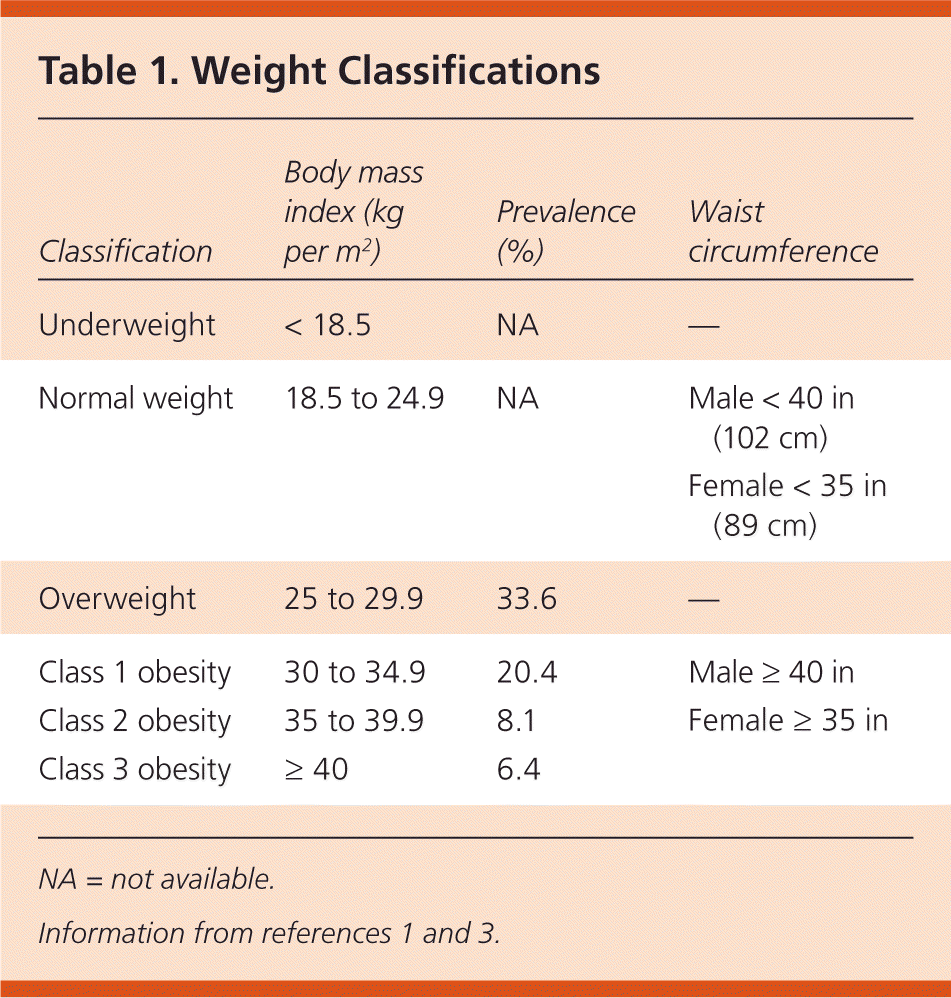
| Classification | Body mass index (kg per m2) | Prevalence (%) | Waist circumference |
|---|---|---|---|
| Underweight | < 18.5 | NA | — |
| Normal weight | 18.5 to 24.9 | NA | Male < 40 in (102 cm) |
| Female < 35 in (89 cm) | |||
| Overweight | 25 to 29.9 | 33.6 | — |
| Class 1 obesity | 30 to 34.9 | 20.4 | Male ≥ 40 in |
| Class 2 obesity | 35 to 39.9 | 8.1 | Female ≥ 35 in |
| Class 3 obesity | ≥ 40 | 6.4 |
NA = not available.
Which Dietary Approaches Have Been Shown to Be Most Effective for Weight Loss?
Adherence to a diet with a deficit of 500 kcal per day, regardless of macronutrient composition, is most effective for weight loss. Simple and realistic diet modifications have the highest likelihood of success.
EVIDENCE SUMMARY
Various commonly used diet plans result in a similar degree of weight loss, regardless of the specific dietary composition of macronutrients (carbohydrate, protein, and fat).5 Adherence to calorie reduction is the most important factor; any diet in which caloric intake is less than caloric expenditure will lead to weight loss.6 A deficit of at least 500 kcal per day can be achieved with intake of 1,200 to 1,500 kcal for women and 1,500 to 1,800 kcal for men. Very low-calorie diets (800 kcal or less per day) should be avoided unless the patient is under close supervision with high-intensity lifestyle interventions.7
Diet plans with multiple components can be overwhelming and lead to poor adherence. A simpler approach using a single dietary adjustment may produce weight loss similar to more complex plans. For example, encouraging a patient to increase dietary fiber intake produces comparable adherence and weight loss to encouraging compliance with the many goals of the American Heart Association diet. Similarly, more permissive goals, such as adding more vegetables and standing more, lead to greater improvement in life-style behaviors than restrictive approaches that instruct patients to avoid certain foods.8 Although different diets with similar caloric intake can result in comparable weight loss, a higher-quality diet of nutrient-dense foods (e.g., vegetables, fruits, whole grains) that are rich in fiber, vitamins, and minerals will produce greater results.9 The 2015–2020 Dietary Guidelines for Americans reinforce the need to make healthier food and beverage choices by consuming nutrient-dense foods from all food groups and limiting intake of added sugars, saturated fats, and sodium.10
Which Behavioral Interventions Are Helpful for Weight Loss?
The USPSTF recommends that patients who are obese be referred to intensive, multicomponent behavioral interventions with 12 to 26 sessions per year.2 Interventions that have been proven effective include motivational interviewing, worksite interventions, and exercise.
EVIDENCE SUMMARY
Motivational interviewing involves assessing a patient's motives for change and acting as a supportive partner to empower them in the process (Table 2).11,12 Multiple studies have shown that motivational interviewing can modestly enhance the effects of a weight-loss program (−3.3 lb [−1.5 kg]; 95% confidence interval [CI], −4.4 to −2.0 lb [−2.0 to −0.9 kg]), and it can be readily used by primary care physicians.13 This technique can also indirectly have beneficial effects on other cardiovascular risk factors, such as activity and cholesterol levels.14
Table 2. Motivational Interviewing Techniques
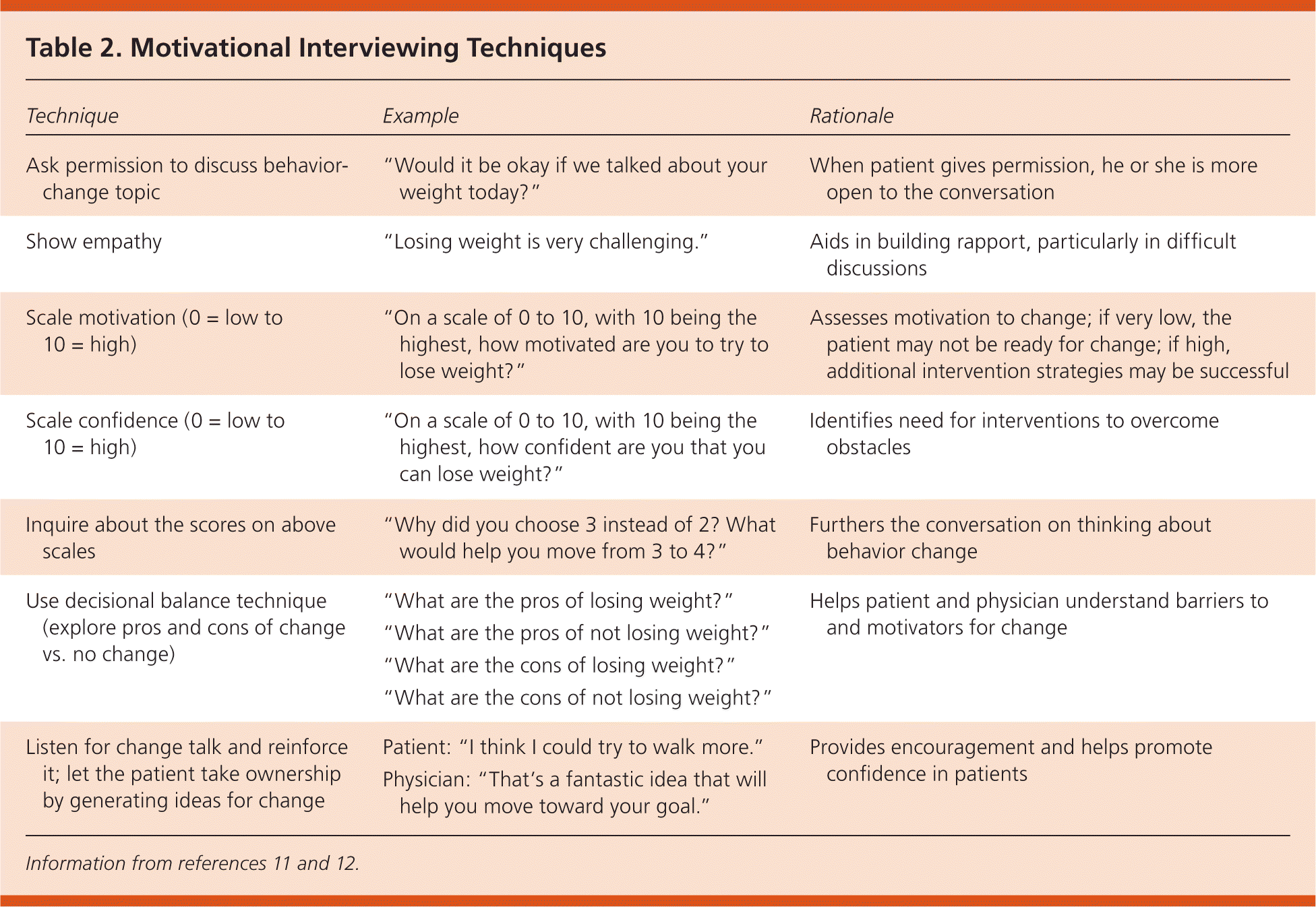
| Technique | Example | Rationale |
|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Worksite interventions are gaining in popularity, and family physicians can encourage patient participation. A systematic review found that worksite nutrition and physical activity programs achieve modest improvements in weight (−2.8 lb [−1.3 kg]; 95% CI, −4.6 to −1.0 lb [−2.1 to −0.5 kg]) over six to 12 months.15 Another study evaluated the effect of worksite incentive programs in which participants received regular education about a healthful diet and exercise.16 Participants received monetary rewards for meeting weight loss goals and lost an average of 2.2 lb (1.0 kg).
Increasing physical activity is an important part of any weight loss plan. The National Institute for Health and Care Excellence recommends 45 to 60 minutes per day of moderate-intensity exercise to prevent obesity and 60 to 90 minutes per day to avoid regaining weight.17 The U.S. Department of Health and Human Services recommends 150 to 300 minutes of moderate-intensity activity or 75 to 150 minutes of vigorous activity per week.18 Exercise alone is not as beneficial for weight loss as it is when combined with a behavioral weight-management program.19 A 2006 Cochrane review showed modest weight loss with exercise alone (−1.1 to −8.8 lb [−0.5 to −4.0 kg]), but the effect was not as significant as when exercise was combined with dietary modification (−7.5 to −39.0 lb [−3.4 to −17.7 kg]).20
What Is the Role of Medications in the Treatment of Obesity?
Medications approved for long-term treatment of obesity include orlistat (Xenical), lorcaserin (Belviq), liraglutide (Saxenda), phentermine/topiramate (Qsymia), and naltrexone/bupropion (Contrave). Medications prescribed for concomitant conditions should be optimized to increase the chance of weight loss.
EVIDENCE SUMMARY
Pharmacotherapeutic options for treating obesity have expanded in recent years. Medications should be considered only for patients who have not achieved weight loss goals with diet and lifestyle changes, and after an extensive discussion of the risks and benefits. All of the agents discussed below have been approved by the U.S. Food and Drug Administration for long-term weight management in conjunction with a reduced-calorie diet and increased physical activity in patients with a BMI of 30 kg per m2 or greater, or 27 kg per m2 or greater who have comorbid conditions such as hypertension, diabetes, or dyslipidemia21–25 (Table 321–32). Despite their indication for long-term therapy, the optimal duration of treatment is unclear; the available evidence was limited to one to two years. Relatively high rates of attrition in studies also raise concern about the utility of these agents in ongoing treatment. Multiple sympathomimetic agents, including phentermine, are approved for short-term treatment (less than 12 weeks), but these agents are not reviewed here. Physicians should consider the effect that medications prescribed for concomitant conditions may have on a patient's weight (Table 4).3,33
Table 3. Medications Approved for the Long-Term Treatment of Obesity
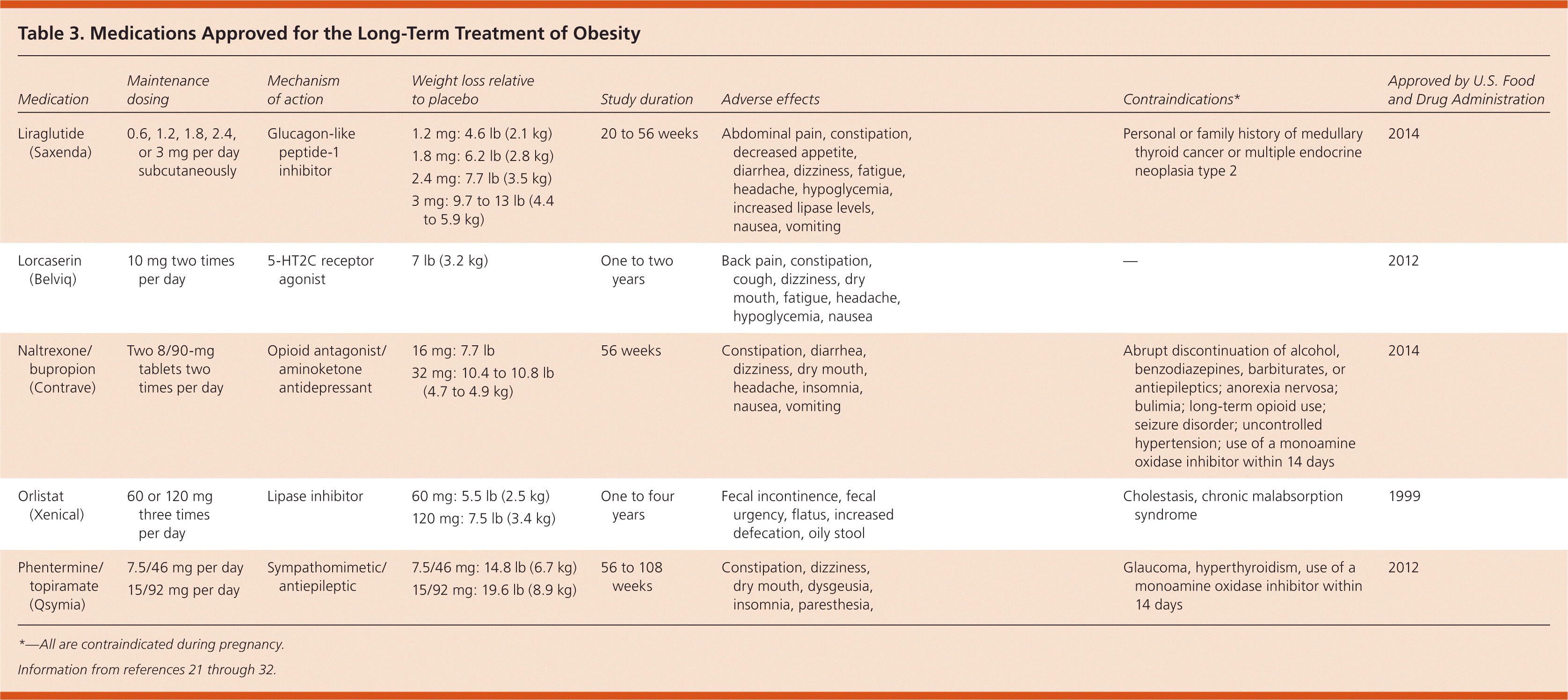
| Medication | Maintenance dosing | Mechanism of action | Weight loss relative to placebo | Study duration | Adverse effects | Contraindications* | Approved by U.S. Food and Drug Administration |
|---|---|---|---|---|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
*—All are contraindicated during pregnancy.
Table 4. Common Medications that Contribute to Weight Gain or Loss
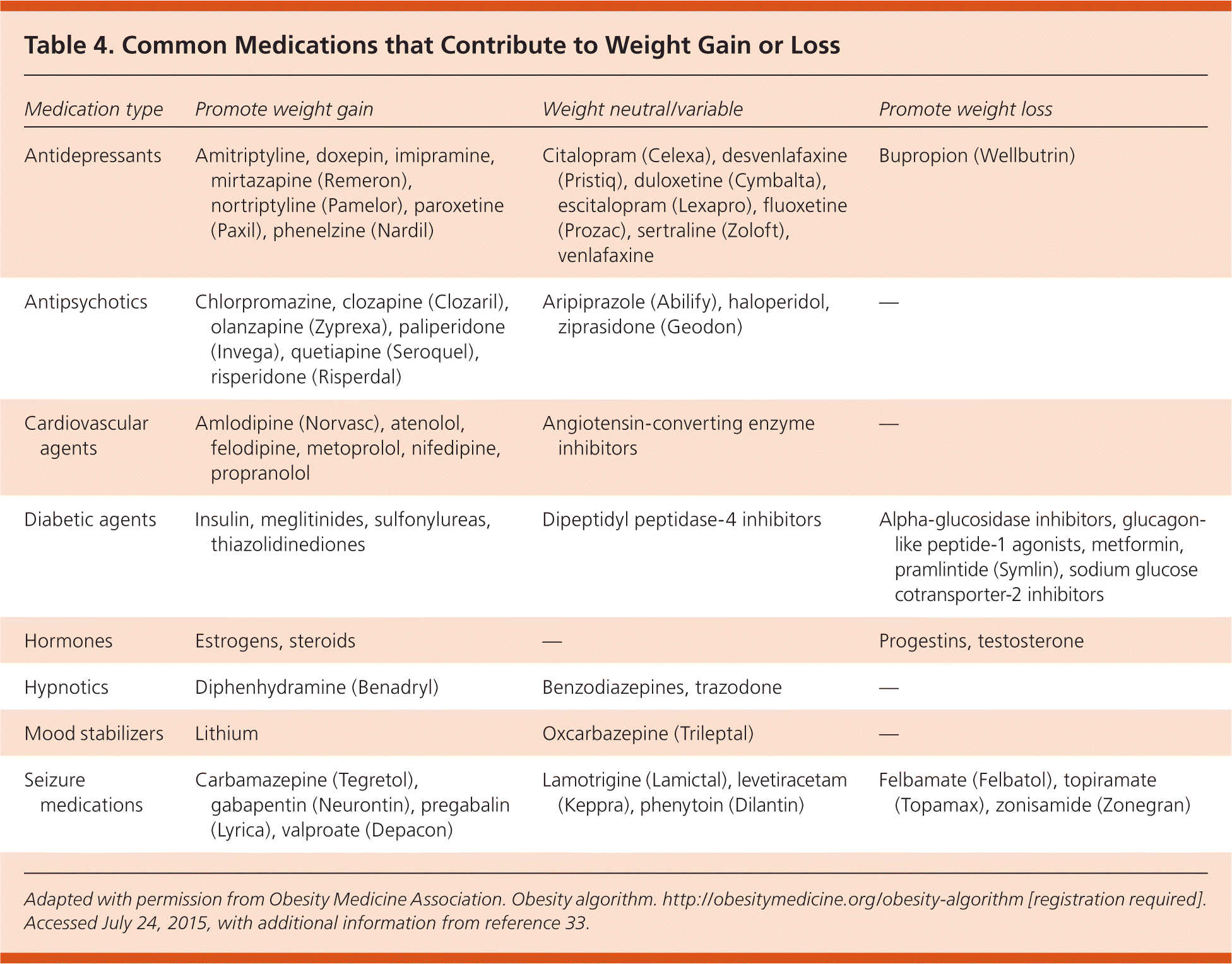
| Medication type | Promote weight gain | Weight neutral/variable | Promote weight loss |
|---|---|---|---|
| Antidepressants | Amitriptyline, doxepin, imipramine, mirtazapine (Remeron), nortriptyline (Pamelor), paroxetine (Paxil), phenelzine (Nardil) | Citalopram (Celexa), desvenlafaxine (Pristiq), duloxetine (Cymbalta), escitalopram (Lexapro), fluoxetine (Prozac), sertraline (Zoloft), venlafaxine | Bupropion (Wellbutrin) |
| Antipsychotics | Chlorpromazine, clozapine (Clozaril), olanzapine (Zyprexa), paliperidone (Invega), quetiapine (Seroquel), risperidone (Risperdal) | Aripiprazole (Abilify), haloperidol, ziprasidone (Geodon) | — |
| Cardiovascular agents | Amlodipine (Norvasc), atenolol, felodipine, metoprolol, nifedipine, propranolol | Angiotensin-converting enzyme inhibitors | — |
| Diabetic agents | Insulin, meglitinides, sulfonylureas, thiazolidinediones | Dipeptidyl peptidase-4 inhibitors | Alpha-glucosidase inhibitors, glucagon-like peptide-1 agonists, metformin, pramlintide (Symlin), sodium glucose cotransporter-2 inhibitors |
| Hormones | Estrogens, steroids | — | Progestins, testosterone |
| Hypnotics | Diphenhydramine (Benadryl) | Benzodiazepines, trazodone | — |
| Mood stabilizers | Lithium | Oxcarbazepine (Trileptal) | — |
| Seizure medications | Carbamazepine (Tegretol), gabapentin (Neurontin), pregabalin (Lyrica), valproate (Depacon) | Lamotrigine (Lamictal), levetiracetam (Keppra), phenytoin (Dilantin) | Felbamate (Felbatol), topiramate (Topamax), zonisamide (Zonegran) |
Adapted with permission from Obesity Medicine Association. Obesity algorithm. http://obesitymedicine.org/obesity-algorithm [registration required]. Accessed July 24, 2015, with additional information from reference 33 .
Orlistat, a reversible inhibitor of gastrointestinal lipase, is a common first choice for therapy because of its long history and lack of systemic effects due to limited absorption. It is taken as a 60- to 120-mg capsule three times per day during or up to one hour after a fat-containing meal. Patients should take a daily multi-vitamin containing fat-soluble vitamins while using orlistat.21 A systematic review showed an average weight loss of 7.5 lb (3.4 kg; 95% CI, 7.1 to 7.9 lb [3.2 to 3.6 kg]) and 5.5 lb (2.5 kg; 95% CI, 3.3 to 7.7 lb [1.5 to 3.5 kg]) greater than placebo for the 120-mg and 60-mg doses, respectively.26 Benefits also include a reduction in multiple cardiovascular risks, including blood pressure, lipid levels, and blood glucose levels. Gastrointestinal symptoms such as oily stool, flatus, fecal urgency, and fecal incontinence are the most common adverse effects limiting long-term use. These symptoms are more severe in patients consuming greater than the recommended dietary fat intake (30% of total calories).21,26
Lorcaserin is a serotonin 5-HT2C receptor agonist administered as a 10-mg tablet twice per day. It should not be used in combination with other serotonergic medications because of concern for serotonin syndrome, and should be discontinued if 5% weight loss has not been achieved in the first 12 weeks of therapy.22 A systematic review showed a mean weight loss of 7.1 lb (3.2 kg; 95% CI, 6.0 to 8.4 lb [2.7 to 3.8 kg]) greater than placebo.26 Its mechanism of action is more specific to the 5-HT2C receptor to minimize the risk of valvulopathy that occurs with other serotonergic weight-loss medications. Serial echocardiography performed in multiple trials revealed no short-term increase in valvulopathy.34
Liraglutide is a glucagon-like peptide-1 receptor agonist that is administered subcutaneously and leads to weight loss when used for diabetes. Dosing for weight loss starts at 0.6 mg per day and is increased in weekly intervals to the full dosage of 3 mg per day, higher than the 1.8-mg dose used for diabetes. Liraglutide is contraindicated in patients with a personal or family history of medullary thyroid carcinoma or multiple endocrine neoplasia type 2 syndrome, and it may affect the absorption of other medications via delayed gastric emptying.23 Randomized trials of 3 mg of liraglutide have shown weight loss of 9.7 to 13.0 lb (4.4 to 5.9 kg) greater than placebo, with improved maintenance of weight loss.27–29
Phentermine/topiramate is a combination sympathomimetic and antiepileptic that is started at a dosage of 3.75 mg/23 mg per day for 14 days, after which the dose escalates to a maximum of 15 mg/92 mg. It should be discontinued if 5% weight loss is not achieved in the first 12 weeks of use at the maximum dose. When discontinuing, phentermine/topiramate should be tapered gradually because of the risk of seizure. Women of child-bearing age should use contraception and have regular pregnancy testing during treatment because of the risk of fetal toxicity.24 A systematic review showed a mean weight loss of 19.6 lb (8.9 kg; 95% CI, 18.3 to 20.7 lb [8.3 to 9.4 kg]) greater than placebo with the 15-mg dose, and another trial showed sustained weight loss through two years of follow-up.26,30
Naltrexone/bupropion is a combination opioid antagonist and antidepressant. It is given as a single 8-mg/90-mg dose and is titrated from one tablet per day to two tablets two times per day over four weeks. It carries a boxed warning for increased suicidality, and is contraindicated in patients with uncontrolled hypertension or seizure disorder, and in those who are receiving long-term opioid therapy.25 Naltrexone/bupropion has a greater effect on weight loss than either agent alone.35 The Contrave Obesity Research I and II trials showed a weight reduction of 10.4 to 10.8 lb (4.7 to 4.9 kg) greater than placebo.31,32 In the Contrave Obesity Research I trial there was a 50% completion rate, and 29.8% of participants experienced nausea; however, there was no increased risk of depression or suicidality.31
Which Patients Should Be Referred for Bariatric Surgery?
Patients with a BMI of 40 kg per m2 or greater, or 30 kg per m2 or greater who have obesity-related comorbidities should be offered referral for consideration of bariatric surgery. Adjustable gastric banding is most appropriate for patients with a BMI of 30 to 34.9 kg per m2.
EVIDENCE SUMMARY
Family physicians have a key role in identifying and counseling patients who may qualify for bariatric surgery (Table 5).36–38 Patients who have been unsuccessful with extensive lifestyle and medical therapy and who meet criteria for operative intervention based on BMI should be referred for a surgical evaluation. An extensive preoperative assessment of comorbidities and surgical risk, as well as a willingness to comply with the long-term management and follow-up requirements, is crucial. Candidates for bariatric surgery include those with a BMI of 40 kg per m2 or greater, regardless of comorbidities, or a BMI of 30 kg per m2 or greater who have at least one severe obesity-related comorbidity, such as type 2 diabetes, hypertension, hyperlipidemia, obstructive sleep apnea, nonalcoholic fatty liver disease, debilitating arthritis, or impaired quality of life. There is increasing evidence for the use of bariatric surgery in patients with a BMI of less than 35 kg per m2, and the adjustable gastric band system has been approved for use in patients with a BMI of 30 to 34.9 kg per m2 who have obesity-related conditions.36
Table 5. Summary of Common Bariatric Procedures

| Procedure | Percentage of excess weight lost | Indications | Complications | Mechanism |
|---|---|---|---|---|
| Adjustable gastric banding | 44 | BMI ≥ 40 kg per m2, ≥ 35 kg per m2 with comorbidities, or ≥ 30 kg per m2 with diabetes mellitus or metabolic syndrome | Band erosion or slippage, need for revision or removal, reservoir leakage | Restrictive; silicone band placed around gastric fundus, inflates/deflates to adjust |
| Roux-en-Y gastric bypass | 67 | BMI ≥ 40 kg per m2, or ≥ 35 kg per m2 with comorbidities | Anastomotic leak, delayed gastric emptying, dumping syndrome, gastric dilation, hernia, nutritional deficiencies, obstruction, staple line failure, stoma narrowing | Restrictive and malabsorptive; ≤ 50-mL gastric pouch anastomosed to Roux limb 30 to 50 cm distal to bypass a portion of small bowel |
| Sleeve gastrectomy | 56 | BMI ≥ 40 kg per m2, or ≥ 35 kg per m2 with comorbidities | Gastric leakage, vomiting | Restrictive; size of stomach is reduced to 25% with pylorus intact |
BMI = body mass index.
How Effective Is Bariatric Surgery?
Bariatric surgery is more effective than diet, behavioral modifications, and pharmacotherapy in the management of obesity, and it leads to improvement in numerous obesity-related comorbidities.
EVIDENCE SUMMARY
Gastric bypass is the most common weight loss procedure worldwide. However, sleeve gastrectomy is being performed with increasing frequency.39 A 2014 Cochrane review found that surgery, regardless of the procedure, resulted in greater weight loss than nonsurgical treatment.37 However, follow-up was limited to one to two years in most studies. The most weight loss occurs with gastric bypass, followed by sleeve gastrectomy and gastric banding.38 Bariatric surgery is relatively safe, with an overall 30-day mortality rate of 0.08%, a complication rate of 17%, and a reoperation rate of 7%.40 Bariatric procedures have been proven effective in reducing many obesity-related conditions, including all-cause mortality, myocardial infarction, and stroke.41,42 Surgery leads to a greater rate of diabetes remission than medical treatment, and the term metabolic surgery is increasingly used when referring to these procedures.43 Bariatric surgery has also been shown to improve hypertension, dyslipidemia, sleep apnea, and health-related quality of life.37,44,45
Data Sources: A PubMed search was completed in Clinical Queries using the key terms obesity, pharmacotherapy, bariatric surgery, diet, and behavioral modification. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, the Cochrane database, the National Guideline Clearinghouse, Essential Evidence Plus, and UpToDate. Search dates: July 2015 through April 2016.

