Obstructive sleep apnea is a common disorder that causes patients to temporarily stop or decrease their breathing repeatedly during sleep. This results in fragmented, nonrestful sleep that can lead to symptoms such as morning headache and daytime sleepiness. Obstructive sleep apnea affects persons of all ages, with an increasing prevalence in those older than 60 years. The exact prevalence is unknown but is estimated to be between 2% and 14%. There are many health conditions associated with obstructive sleep apnea, including hypertension, coronary artery disease, cardiac arrhythmias, and depression. Loud snoring, gasping during sleep, obesity, and enlarged neck circumference are predictive clinical features. Screening questionnaires can be used to assess for sleep apnea, although their accuracy is limited. The diagnostic standard for obstructive sleep apnea is nocturnal polysomnography in a sleep laboratory. Home sleep apnea tests can be performed for certain patients but are generally considered less accurate. Continuous positive airway pressure is the first-line treatment; adherence rates are variable and seem to improve with early patient education and support. Other treatment modalities include weight reduction, oral appliance therapy, and surgery to correct anatomic obstructions, although there is insufficient evidence to support these types of surgeries. Bariatric surgery can improve sleep parameters and symptoms in obese patients with obstructive sleep apnea and can result in remission in many patients.
Obstructive sleep apnea (OSA) is a common, chronic disorder that disrupts breathing during sleep. It affects persons of all ages but especially those middle-aged and older.1 Patients with OSA temporarily stop or decrease their breathing (apnea or hypopnea, respectively) repeatedly during sleep.2–5 This cessation or decrease in breathing is the result of repetitive partial or complete obstruction of the airway caused by narrowing of the respiratory passages.4,6–8 These breathing disruptions can awaken a person or prevent deep, restful sleep. The effects of fragmented sleep on daytime fatigue and sleepiness are widely recognized.3,6
WHAT IS NEW ON THIS TOPIC: OBSTRUCTIVE SLEEP APNEA
In patients with obstructive sleep apnea, continuous positive airway pressure lowers blood pressure and rates of arrhythmia and stroke, improves left ventricular ejection fraction in patients with heart failure, and reduces fatal and nonfatal cardiovascular events.
A recent meta-analysis demonstrated similar rates of blood pressure lowering between continuous positive airway pressure and mandibular advancement devices.
BEST PRACTICES IN SLEEP MEDICINE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not perform positive airway pressure retitration studies in asymptomatic, adherent patients with sleep apnea and stable weight. | American Academy of Sleep Medicine |
| Do not routinely order sleep studies (polysomnogram) to screen for/diagnose sleep disorders in workers with chronic fatigue/insomnia. | American College of Occupational and Environmental Medicine |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Although the American Academy of Sleep Medicine advocates for physicians to ask all patients about signs and symptoms of OSA, the U.S. Preventive Services Task Force has no position on this issue, and there are no good outcome studies of net benefit for screening unselected populations. | C | 6 |
| Overnight polysomnography performed in a sleep laboratory in the presence of an attendant is considered the diagnostic standard for OSA. | C | 4, 6, 7, 11, 22–24 |
| In obese patients with OSA, bariatric surgery can result in improvement and remission. | A | 57, 58 |
OSA = obstructive sleep apnea.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Prevalence
The exact prevalence of OSA is unknown, although estimates range from 2% to 14% in community-screened populations to a much higher prevalence in certain subgroups (i.e., 20% to 90% of persons referred for sleep studies).7,9
Men are three times more likely than women to have OSA. It is particularly uncommon in nonobese, premenopausal women; however, the rates of OSA in postmenopausal women not taking hormone therapy approach the rates of OSA in men of a similar age and body mass index.6,10,11
The prevalence of OSA increases with age, especially in persons older than 60 years. OSA is also more prevalent among persons who are obese. Both an aging population and a growing rate of obesity contribute to the increasing rate of OSA.1,2,4,6
Associated Conditions
OSA is important from a public health perspective because patients with untreated OSA have higher rates of health care use, including more frequent and longer hospitalizations and higher health care costs.2,4,12,13 Furthermore, OSA has been associated with higher rates of unintentional injury, including motor vehicle collisions and work-related injuries, which add to the public health burden.3,4,6,9,14
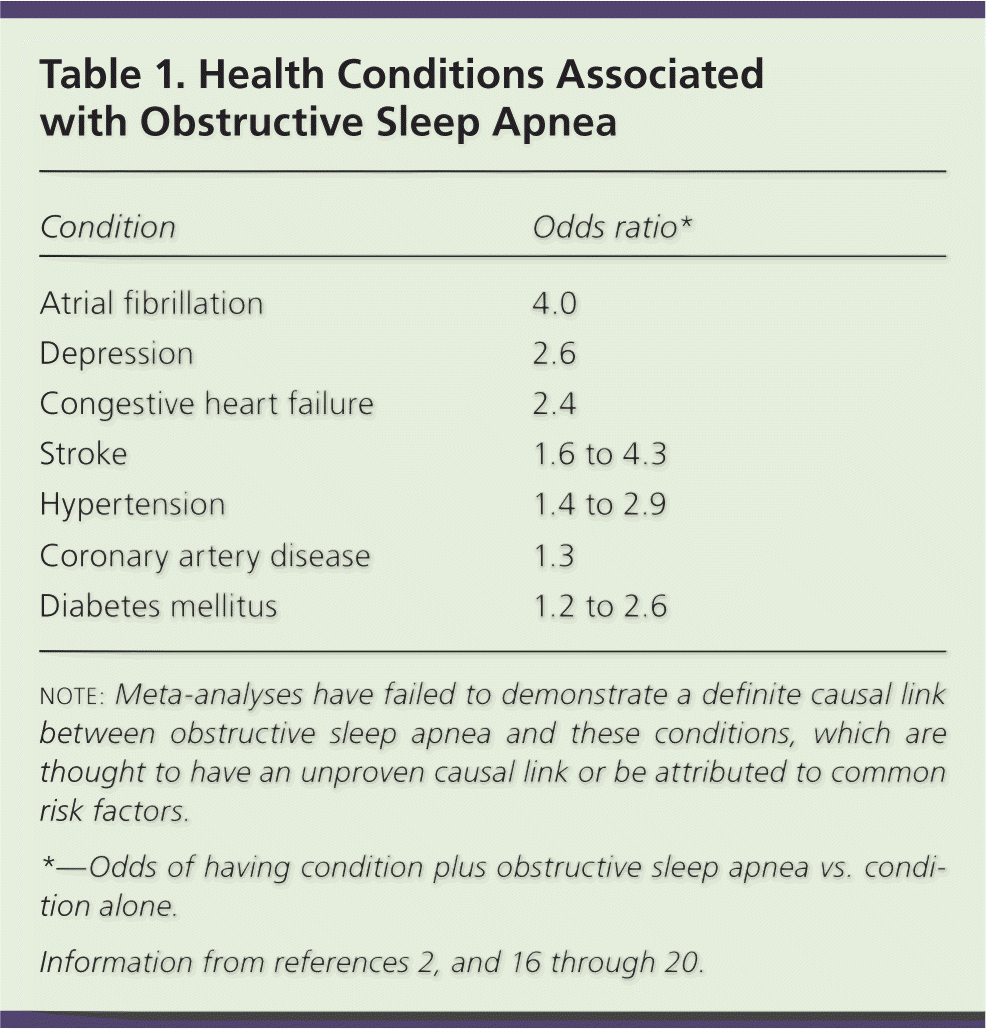
OSA has been associated with increased morbidity and mortality rates2,8,14,15 and decreased quality-of-life scores,6,15 as well as numerous health problems (Table 12,16–20); however, a causal relationship has not been established via randomized controlled trials or large meta-analyses.2,16–21
Table 1. Health Conditions Associated with Obstructive Sleep Apnea
| Condition | Odds ratio* |
|---|---|
| Atrial fibrillation | 4.0 |
| Depression | 2.6 |
| Congestive heart failure | 2.4 |
| Stroke | 1.6 to 4.3 |
| Hypertension | 1.4 to 2.9 |
| Coronary artery disease | 1.3 |
| Diabetes mellitus | 1.2 to 2.6 |
note: Meta-analyses have failed to demonstrate a definite causal link between obstructive sleep apnea and these conditions, which are thought to have an unproven causal link or be attributed to common risk factors.
*—Odds of having condition plus obstructive sleep apnea vs. condition alone.
Screening
There are no outcome data to support the net benefit of screening for OSA in unselected populations. Screening is not recommended by major organizations, including the U.S. Preventive Services Task Force. However, the American Academy of Sleep Medicine advocates for physicians to ask all adult patients about signs and symptoms of OSA as part of a routine health maintenance evaluation.6
Diagnosis
In addition to risk factors, numerous signs and symptoms can suggest OSA, but polysomnography is the diagnostic standard.4,6,7,11,22–26
CLINICAL HISTORY
Predictive clinical features of OSA include observed gasping during sleep, morning headache, excessive daytime sleepiness, loud snoring, and neck circumference of greater than 16 inches (40.6 cm).6,7,11,26
Table 2. Predisposing Risk Factors for Obstructive Sleep Apnea
As previously mentioned, men are three times more likely to have OSA, but they are nine times more likely to be referred for polysomnography, which suggests that the diagnosis of OSA may be overlooked in women.6,11
There are several screening questionnaires for OSA, although the accuracy of many of them is limited.4,6,7,24 The STOP-Bang questionnaire is a validated screening tool, particularly in obese and surgical patients (Figure 1).27 Its sensitivity has consistently been shown to be greater than 85%, with a specificity ranging between 25% and 85%, and a higher specificity in obese men.27–29 The STOP-Bang questionnaire can be easily administered in the primary care setting.
Figure 1. STOP-Bang Questionnaire

STOP-Bang Questionnaire to assess the risk of obstructive sleep apnea.
Adapted with permission from Chung F, Yegneswaran B, Liao P, et al. STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology. 2008;108(5):821.
Nocturia and snoring are sensitive, but not specific, signs of OSA, although the specificity of snoring increases in proportion to the severity.6,11,26 The “elbow sign,” described as being elbowed by one's bed partner, can be suggestive of OSA. In one study, 97% of patients with a positive polysomnography result reported being elbowed by their bed partner because of snoring or apneic episodes.30
PHYSICAL EXAMINATION
In addition to large neck circumference and high body mass index, factors predictive of OSA include posterior chin position (retrognathia), reduced distance and increased angles from the chin to the thyroid cartilage, and a narrow oropharyngeal opening.6,7,11
POLYSOMNOGRAPHY
Sleep studies performed in a sleep laboratory or in the home can quantify the apnea-hypopnea index, which is required to diagnose OSA. Apnea is a complete obstruction of airflow, and hypopnea is a partial obstruction of airflow; both must last a minimum of 10 seconds. Hypopneas are measured by oxygen desaturation of 3% or more or arousal from sleep. The apnea-hypopnea index is calculated by adding all apneas and hypopneas and then dividing by total sleep time. An apnea-hypopnea index of 15 or more events per hour, or five or more events per hour in the presence of symptoms or cardiovascular comorbidities, is diagnostic for OSA (Table 3).4,23,24,29,31
Table 3. Symptoms and Cardiovascular Comorbidities That Assist with the Diagnosis of Obstructive Sleep Apnea

| Symptoms |
| Cognitive impairment |
| Daytime sleepiness |
| Fatigue |
| Insomnia |
| Loud snoring |
| Mood disorders |
| Sleep episodes during wakefulness |
| Waking up gasping for air, choking, or holding one's breath |
| Cardiovascular comorbidities |
| Hypertension |
| Ischemic heart disease |
| Previous stroke |
note: The diagnostic threshold for obstructive sleep apnea is reached when the apnea-hypopnea index reaches five or more events per hour in the presence of symptoms or cardiovascular comorbidities.
There are four types of sleep studies, depending on the number of physiologic parameters, or channels, being monitored4 (eTable A). Overnight polysomnography performed in a sleep laboratory in the presence of an attendant is considered the first-line diagnostic study and is classified as a type-I study.4,6,7,11,22–24 A full-night study is generally indicated for diagnosis, with a follow-up study used for positive airway pressure titration; however, a split-night study, in which diagnosis and positive airway pressure titration occur in the same night, can also be performed.6,23 Split-night studies are most useful in patients who have an apnea-hypopnea index greater than 20 events per hour discovered within the first two hours of the study.23
eTable A. Accuracy of Portable Monitors to Diagnose Obstructive Sleep Apnea
| Type of monitor | Number of channels | Sensitivity (%) at threshold AHI of 15 | Specificity (%) at threshold AHI of 15 | Sensitivity (%) at threshold AHI of 5 | Specificity (%) at threshold AHI of 5 |
|---|---|---|---|---|---|
| II | 7 to 16 | 79 to 100 | 71 to 100 | 88 to 94 | 36 to 77 |
| III | 4 to 6 | 64 to 100 | 41 to 100 | 83 to 97 | 48 to 100 |
| IV | 2 or 3 | 67 to 98 | 50 to 100 | 75 to 100 | 43 to 100 |
AHI = apnea-hypopnea index.
Information from Qaseem A, Dallas P, Owens DK, Starkey M, Holty JE, Shekelle P. Diagnosis of obstructive sleep apnea in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2014;161(3):210–220.
In general, home sleep apnea tests are considered to be less accurate than type-I studies because of data loss from detached or malfunctioning monitoring equipment.32 Additionally, home monitors with fewer channels cannot discern between sleep and wakefulness, and therefore can only estimate an apnea-hypopnea index. Home sleep apnea tests can be an alternative to type-I studies in patients who are unable to present to a sleep laboratory. These tests are more accurate in identifying patients with a higher pretest probability of OSA and can rule out OSA in low-risk patients.23,32–34 Home sleep apnea tests are not recommended in patients with comorbidities such as congestive heart failure, chronic lung disease, or neurologic conditions because they have not been verified in these populations.4,6
Treatment
LIFESTYLE CHANGES AND WEIGHT REDUCTION
Obesity results in fatty deposits around the neck, which contribute to pharyngeal collapse.35 Although a decrease in weight has been shown to decrease critical closing pressures of the airway, there are inconsistent findings on the association between weight reduction and overall improvement in sleep and breathing patterns.36 Studies have shown that sleeping in the supine position compared with the lateral position may double the apnea-hypopnea index in patients with OSA. Strategies to avoid the supine position include placing tennis balls in a sock or pocket and pinning or sewing them onto the back of a shirt; wearing vests with posterior bumpers; and using positional alarms, verbal instruction, and pillows.37 Because of poor long-term compliance, positional therapy is not routinely recommended over standard positive airway pressure therapy.38,39
POSITIVE AIRWAY PRESSURE
Positive pressure therapies include continuous positive airway pressure (CPAP), bilevel positive airway pressure, and auto-titrating positive airway pressure. CPAP is effective and remains the first-line treatment for OSA. CPAP works via pneumatic splinting of the upper airways. Airway pressure may be applied through oral, oronasal, and nasal devices.40 A Cochrane review of CPAP interfaces demonstrated that nasal masks are preferred by patients, but further studies are required to assess the comparative benefits of each delivery system.41 CPAP adherence rates range between 17% and 85%, with improved adherence in patients who receive early and continued education and support on the use of CPAP.42–46
CPAP has not only been shown to improve quality-of-life and sleep indices in patients with OSA, but also to lower blood pressure and rates of arrhythmia and stroke, to improve left ventricular ejection fraction in patients with heart failure, and to improve the rates of fatal and nonfatal cardiovascular events.20,47–50 Bilevel positive airway pressure may be considered in patients who need high pressure, who hypoventilate during sleep, and who have difficulty exhaling against a fixed pressure. Auto-titrating positive airway pressure automatically adjusts pressure as needed to maintain airway patency and can be used in lieu of a formal CPAP titration study. These devices can be maintained in continuous self-adjustment mode, or a fixed pressure can be set based on information obtained during titration.51 Auto-titrating positive airway pressure should be used only in patients without significant comorbidities.
ORAL APPLIANCE THERAPY
Although CPAP is the preferred treatment modality for OSA, oral appliances are a reasonable alternative if patients cannot tolerate CPAP. The two main oral appliance therapies are mandibular advancement devices, which keep the patient's jaw forward to maintain an open airway, and tongue-retaining devices, which splint the tongue in place to keep the airway open.52 Mandibular advancement devices are preferred because there is insufficient evidence on the effectiveness of tongue-retaining devices. Newer devices such as oral pressure therapy, which uses a mouthpiece and a vacuum pump to stabilize upper airway tissue, are being studied.53
CPAP has been shown to be superior to oral appliances in reducing apnea-hypopnea indices, arousal indices, and oxygen desaturation, particularly in patients with moderate to severe OSA, although quality-of-life indices appear to be similar to oral appliances.54 A recent meta-analysis, however, demonstrated similar rates of blood pressure lowering between CPAP and mandibular advancement devices.55 Guidelines published in 2015 from the American Academy of Sleep Medicine and the American Academy of Dental Sleep Medicine recommend that a qualified dentist use a custom, titratable appliance vs. noncustom oral devices based on systematic reviews that showed superiority in sleep parameters.54
SURGERY
Numerous surgeries have been proposed and attempted to correct anatomic obstruction in patients with OSA: nasal procedures (e.g., septoplasty), oral procedures (e.g., uvulopalatopharyngoplasty), hypopharyngeal procedures (e.g., tongue reduction and stabilization), laryngeal procedures (e.g., epiglottoplasty), and global airway procedures (e.g., maxillomandibular advancement).23 According to systematic reviews, there is insufficient evidence to support surgery in general or any type of surgery in particular for the treatment of OSA.56 Benefits of bariatric surgery in obese patients with OSA include an improvement in more than 75% of patients and a remission rate of 40% after two years.57,58
OTHER STRATEGIES
Surgical implantation of neurostimulators delivers electrical pulses to the hypoglossal nerve to increase tone to upper airway muscles. A recent study showed that this method may be effective for treating OSA.59 Nasal dilators have been created to decrease nasal airway resistance. They have been shown to be effective in reducing snoring but not effective for other sleep parameters.37 Use of pharmacologic agents has been proposed to increase respiratory drive and upper airway muscle tone; however, these agents have not been shown to successfully treat OSA.37
Data Sources: A PubMed search was performed using the key term obstructive sleep apnea. The search included randomized controlled trials, reviews, clinical trials, and meta-analyses. A search was also done using Essential Evidence Plus, the Cochrane Database of Systematic Reviews, the Agency for Healthcare Research and Quality evidence reports, and the National Guideline Clearinghouse. Search date: January 15, 2016.
The authors thank Marilyn Daniels for her assistance with this manuscript.


