Syncope is an abrupt and transient loss of consciousness caused by cerebral hypoperfusion. It accounts for 1% to 1.5% of emergency department visits, resulting in high hospital admission rates and significant medical costs. Syncope is classified as neurally mediated, cardiac, and orthostatic hypotension. Neurally mediated syncope is the most common type and has a benign course, whereas cardiac syncope is associated with increased morbidity and mortality. Patients with presyncope have similar prognoses to those with syncope and should undergo a similar evaluation. A standardized approach to syncope evaluation reduces hospital admissions and medical costs, and increases diagnostic accuracy. The initial assessment for all patients presenting with syncope includes a detailed history, physical examination, and electrocardiography. The initial evaluation may diagnose up to 50% of patients and allows immediate short-term risk stratification. Laboratory testing and neuroimaging have a low diagnostic yield and should be ordered only if clinically indicated. Several comparable clinical decision rules can be used to assess the short-term risk of death and the need for hospital admission. Low-risk patients with a single episode of syncope can often be reassured with no further investigation. High-risk patients with cardiovascular or structural heart disease, history concerning for arrhythmia, abnormal electrocardiographic findings, or severe comorbidities should be admitted to the hospital for further evaluation. In cases of unexplained syncope, provocative testing and prolonged electrocardiographic monitoring strategies can be diagnostic. The treatment of neurally mediated and orthostatic hypotension syncope is largely supportive, although severe cases may require pharmacotherapy. Cardiac syncope may require cardiac device placement or ablation.
Syncope is a sudden, brief, and transient loss of consciousness caused by cerebral hypoperfusion.1 Other nontraumatic loss of consciousness syndromes include seizures, cataplexy, metabolic disorders, acute intoxications, vertebrobasilar insufficiency, transient ischemic attack, cerebrovascular accident, and psychogenic pseudosyncope.2,3
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Patients who present with presyncope should be evaluated similarly to those who present with syncope. | C | 20, 21 |
| Patients with syncope and evidence of congestive heart failure or structural heart disease, abnormal electrocardiographic findings, or a family history of sudden death should be admitted to the hospital for emergent evaluation. | C | 1, 25, 27, 29 |
| Patients presenting with syncope should have orthostatic blood pressure measurements and standard 12-lead electrocardiography. | C | 1, 2, 25, 27, 29 |
| Laboratory and imaging studies should be ordered for patients with syncope only if clinically indicated by the history and physical examination. | C | 1, 27, 39, 40, 42, 43, 50, 51 |
| Implantable loop recorders increase diagnostic yield, reduce time to diagnosis, and are cost-effective for suspected cardiac syncope and unexplained syncope. | C | 1, 39, 44–48 |
| Patients with syncope who are at low risk of adverse events (e.g., those with symptoms consistent with vasovagal or orthostatic hypotension syncope, no history of heart disease, no family history of sudden cardiac death, and normal electrocardiographic findings) may be safely followed without further intervention or treatment. | C | 1, 25, 27, 29 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
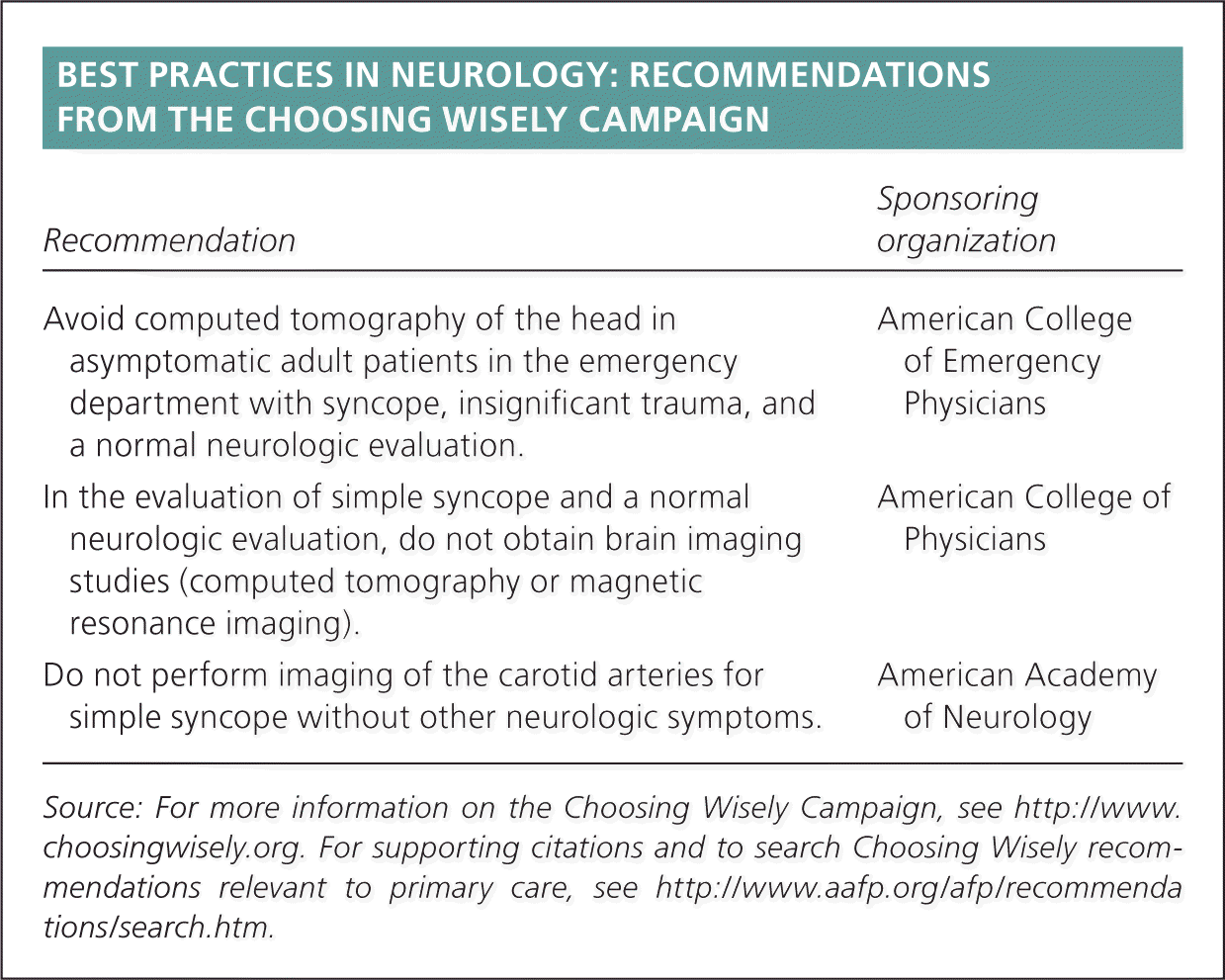
BEST PRACTICES IN NEUROLOGY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN
| Recommendation | Sponsoring organization |
|---|---|
| Avoid computed tomography of the head in asymptomatic adult patients in the emergency department with syncope, insignificant trauma, and a normal neurologic evaluation. | American College of Emergency Physicians |
| In the evaluation of simple syncope and a normal neurologic evaluation, do not obtain brain imaging studies (computed tomography or magnetic resonance imaging). | American College of Physicians |
| Do not perform imaging of the carotid arteries for simple syncope without other neurologic symptoms. | American Academy of Neurology |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Syncope accounts for 1% to 1.5% of all emergency department visits, 250,000 annual hospital admissions, and a median hospital cost of $8,500.4,5 Approximately 40% of the U.S. population will experience a syncopal episode in their lifetimes, and 30% to 50% will be admitted to the hospital for further evaluation.6,7 The etiology is unexplained in up to one-third of cases.8
Although syncope is associated with serious risks, short-term mortality is low (i.e., 0.7% at 10 days and 1.6% at 30 days). At one year, the mortality rate is 8.4%; one-third of these are attributed to cardiovascular causes. Approximately 25% of patients with syncope will experience another event within two years.8,9 Historically, neurally mediated and orthostatic hypotension syncope have not conferred an increased risk of death10; however, in a recent study, healthy adults with a diagnosis of syncope had higher rates of all-cause mortality, recurrent syncope, cardiovascular events, and pacemaker or implantable cardioverter-defibrillator placement compared with matched controls. Patients 44 to 75 years of age had the highest risk.11,12
Management of syncope remains a challenge, particularly in identifying patients with potentially life-threatening etiologies. Lack of physician knowledge, a desire to reassure the patient or clinician, and the fear of medicolegal ramifications result in overuse of diagnostic tests.13 A standardized approach for evaluating patients with syncope reduces admissions, hospital costs, and number of tests performed, and increases accuracy of diagnosis.14 Only 10% to 15% of patients will remain undiagnosed after a comprehensive evaluation using current guidelines.15,16
Classification and Etiology
Syncope is classified as cardiac, neurally mediated (reflex), and orthostatic hypotension (Table 1).1,17 The differential diagnosis should include nontraumatic causes of transient loss of consciousness. Rare causes include subclavian steal syndrome, pulmonary embolism, acute myocardial infarction, acute aortic dissection, leaking aortic aneurysm, subarachnoid hemorrhage, and cardiac tamponade.2,3
Table 1. Classification of Syncope

| Syncope type | Scenario | Clinical features |
|---|---|---|
| Cardiac syncope | ||
| Arrhythmia (e.g., bradyarrhythmias, ventricular tachyarrhythmias, supraventricular tachyarrhythmias), pacemaker dysfunction, channelopathies | Generally abrupt and unprovoked; palpitations may precede symptoms | Abnormal electrocardiographic findings, family history of sudden death, personal history of heart disease, sudden onset of palpitations, symptoms during or after exertion while in supine or prone position |
| Obstructive cardiomyopathy | Hypertrophic cardiomyopathy or exertional syncope in persons with a family history of sudden cardiac death | Often asymptomatic; may cause arrhythmias, chest pain, shortness of breath, or syncope; dynamic systolic murmur that intensifies from squatting to standing or during Valsalva maneuver |
| Structural cardiac disease | Acute myocardial infarction or ischemia | Diaphoresis, exertional chest pain, nausea, shortness of breath; rare cause of syncope |
| Arrhythmogenic right ventricular cardiomyopathy | Asymptomatic, atypical chest pain, dizziness, exertional syncope, family history of sudden cardiac death, palpitations, right ventricular structural abnormalities | |
| Infiltrative (e.g., amyloidosis, hemochromatosis, sarcoidosis) | Arrhythmias, heart block, heart failure | |
| Valvular disease (e.g., aortic stenosis, mitral stenosis, pulmonary stenosis) | Symptoms dependent on severity; severe aortic stenosis can manifest with congestive heart failure, exertional angina, or syncope | |
| Other structural disease | Acute aortic dissection | Hypotension or shock, severe sharp chest pain with or without radiation to the back, history of hypertension |
| Cardiac masses (e.g., atrial myxoma, cardiac tumors) | Arrhythmia via direct invasion, embolization, heart failure, systemic symptoms, valvular regurgitation | |
| Cardiac tamponade | Elevated jugular venous pressure, hypotension, pulsus paradoxus, sinus tachycardia | |
| Pulmonary hypertension | Often asymptomatic; may cause fatigue and shortness of breath | |
| Saddle pulmonary embolus | Acute shortness of breath, chest pain, hypoxia, right heart strain, sinus tachycardia | |
| Neurally mediated (reflex) syncope | ||
| Carotid sinus syndrome/hypersensitivity | Head rotation or pressure on the carotid sinus (e.g., from shaving or tight collar) can reproduce symptoms; consider in patients with unexplained falls | Ventricular pause or decreased systolic blood pressure after carotid sinus massage; may coincide with syncope |
| Situational | Brought on by coughing, defecation, gastrointestinal stimulation, or urination; may occur after exercise or meals | Absence of heart disease; history of similar syncope; prolonged standing, eating, or voiding |
| Vasovagal | Mediated by fear, heat exposure, noxious stimuli, pain, or stress | Prodromal symptoms (e.g., diaphoresis, dizziness, nausea), precipitating factors |
| Orthostatic hypotension syncope | ||
| Drug induced | Alcohol, antianginal agents, antidepressants, antidiabetic agents, antihypertensives, antiparkinsonian agents, diuretics, flibanserin (Addyi), insulin | Initiation or change in dosage |
| Postural tachycardia syndrome | Young adults (predominantly female); associated with chronic fatigue syndrome and mitral valve prolapse | Severe orthostatic intolerance with marked tachycardia |
| Primary autonomic failure | Multiple sclerosis, multiple system atrophy (e.g., Shy-Drager syndrome), Parkinson disease/parkinsonism, Wernicke encephalopathy | Orthostatic hypotension with postural change |
| Secondary autonomic failure | Amyloidosis, chronic inflammatory demyelinating polyneuropathy, connective tissue diseases, diabetes mellitus, Lewy body dementia, older age, spinal cord injury, uremia | Orthostatic hypotension with postural change |
| Volume depletion | Acute blood loss (e.g., gastrointestinal bleeding, ectopic pregnancy), diarrhea, inadequate fluid intake, vomiting | Hypotension, tachycardia, history of volume/blood loss, dehydration on examination |
Neurally mediated syncope is the most common type, comprising approximately 45% of cases.6,10,18 It can be vasovagal, situational, or secondary to carotid sinus hypersensitivity. The pathophysiology is complex, consisting of an interaction between autonomic systems paradoxically favoring parasympathetic or vagal tone, which causes bradycardia and hypotension.
Cardiac syncope occurs in approximately 20% of syncope presentations. It is most often caused by an arrhythmia, and less often by a structural cardiac abnormality. In a prospective cohort study, patients with cardiac syncope had a twofold increase in mortality over 17 years.10 The presence of cardiovascular disease predicts a cardiac etiology of syncope with 85% to 94% sensitivity and 64% to 83% specificity.16
Orthostatic hypotension syncope has an incidence of approximately 10% and is typically characterized by posturally induced hypotension, most often related to impaired increase in systemic vascular resistance. Associated factors include medication effects, volume depletion, acute hemorrhage, and autonomic dysfunction. Postural tachycardia syndrome is the most prevalent form of orthostatic intolerance, affecting approximately 500,000 persons in the United States. Younger adults, predominantly women who report symptoms of postural presyncope, are more likely to have this condition.19
PRESYNCOPE
Presyncope is poorly studied, and the true incidence is unknown. A study of 881 patients presenting to the emergency department with presyncope showed a 30-day risk of serious outcomes of 5% and a mortality rate of 0.3%.20 Emergency physicians had difficulty stratifying patients at increased risk of adverse outcomes, regardless of presumed etiology. A prospective observational study (n = 244) compared adverse outcomes and hospitalizations in patients who presented with presyncope and syncope.21 Adverse outcomes occurred in 49 of 244 patients (20%) with presyncope compared with 68 of 293 patients (23%) with syncope. Admission rates were 49% and 69%, respectively. Because rates of adverse outcomes are similar in patients with presyncope and syncope, both groups should receive a similar evaluation.
Risk Stratification
The decision to perform an expedited and monitored evaluation of patients presenting with syncope is based on the likelihood of short-term adverse outcomes. Unnecessary admissions for patients meeting low-risk criteria result in high medical costs without improvements in morbidity and mortality, patient safety, or quality of life.22
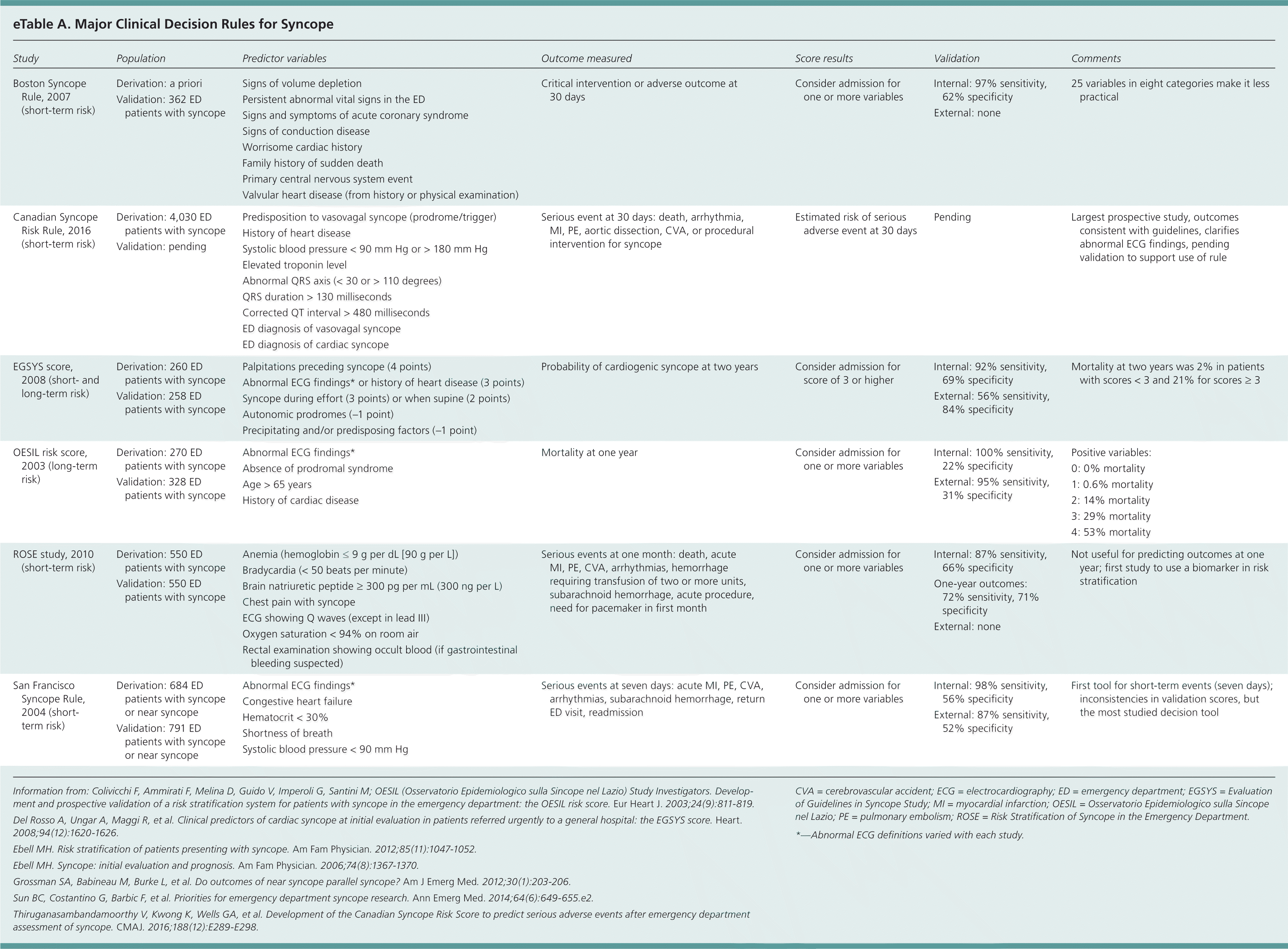
Several clinical decision rules have been developed to risk stratify patients presenting to the emergency department with syncope. Each has differing variables, and no single rule has proved significantly superior 23,24 (eTable A). The San Francisco Syncope Rule, Evaluation of Guidelines in Syncope Study, and Osservatorio Epidemiologico sulla Sincope nel Lazio are the only rules that have been externally validated. High-risk patients should be admitted for further evaluation (Table 2).1,25
eTable A. Major Clinical Decision Rules for Syncope
| Study | Population | Predictor variables | Outcome measured | Score results | Validation | Comments |
|---|---|---|---|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
CVA = cerebrovascular accident; ECG = electrocardiography; ED = emergency department; EGSYS = Evaluation of Guidelines in Syncope Study; MI = myocardial infarction; OESIL = Osservatorio Epidemiologico sulla Sincope nel Lazio; PE = pulmonary embolism; ROSE = Risk Stratification of Syncope in the Emergency Department.
*—Abnormal ECG definitions varied with each study.
Information from: Colivicchi F, Ammirati F, Melina D, Guido V, Imperoli G, Santini M; OESIL (Osservatorio Epidemiologico sulla Sincope nel Lazio) Study Investigators. Development and prospective validation of a risk stratification system for patients with syncope in the emergency department: the OESIL risk score. Eur Heart J. 2003;24(9):811-819.
Del Rosso A, Ungar A, Maggi R, et al. Clinical predictors of cardiac syncope at initial evaluation in patients referred urgently to a general hospital: the EGSYS score. Heart. 2008;94(12):1620-1626.
Ebell MH. Risk stratification of patients presenting with syncope. Am Fam Physician . 2012;85(11):1047-1052.
Ebell MH. Syncope: initial evaluation and prognosis. Am Fam Physician . 2006;74(8):1367-1370.
Grossman SA, Babineau M, Burke L, et al. Do outcomes of near syncope parallel syncope? Am J Emerg Med. 2012;30(1):203-206. Sun BC, Costantino G, Barbic F, et al. Priorities for emergency department syncope research. Ann Emerg Med. 2014;64(6):649-655.e2.
Thiruganasambandamoorthy V, Kwong K, Wells GA, et al. Development of the Canadian Syncope Risk Score to predict serious adverse events after emergency department assessment of syncope. CMAJ . 2016;188(12):E289-E298.
Table 2. Risk Stratification in Patients with Syncope

| High risk (hospital admission recommended)* |
| Clinical history suggestive of arrhythmic syncope (e.g., syncope during exercise, palpitations, or syncope without warning or prodrome) |
| Comorbidities (e.g., severe anemia, electrolyte abnormalities) |
| Electrocardiographic history suggestive of arrhythmic syncope (e.g., bifascicular block, sinus bradycardia < 40 beats per minute in absence of sinoatrial block or medication use, QRS preexcitation, abnormal QT interval, ST segment elevation leads V1 through V3 [Brugada pattern], negative T wave in right precordial leads and epsilon wave [arrhythmogenic right ventricular dysplasia/cardiomyopathy]) |
| Family history of sudden death |
| Hypotension (systolic blood pressure < 90 mm Hg) |
| Older age† |
| Severe structural heart disease, congestive heart failure, or coronary artery disease |
| Low risk (outpatient evaluation recommended)‡ |
| Age less than 50 years† |
| No history of cardiovascular disease |
| Normal electrocardiographic findings |
| Symptoms consistent with neurally mediated or orthostatic hypotension syncope |
| Unremarkable cardiovascular findings |
*—Patient is at high risk if any of the criteria are met.
†—Different age thresholds have been used in studies for decision making. Older age largely reflects the patient's cardiovascular health.
‡—Patient is at low risk only if all criteria are met.
Diagnostic Approach
Guidelines from the Canadian Cardiovascular Society, European Society of Cardiology, and the American College of Emergency Physicians recommend obtaining a detailed history and performing a physical examination, standard 12-lead electrocardiography (ECG), and orthostatic blood pressure measurement in patients presenting with syncope.1,25–28 Additional testing should be individualized. Figure 1 provides a general framework, emphasizing classification and risk stratification to standardize the evaluation of syncope.2 High-risk patients should be admitted for monitoring and further workup. Low-risk patients with a first episode of syncope may be reassured without further workup.1,25,27,29
Figure 1. Evaluation of Syncope
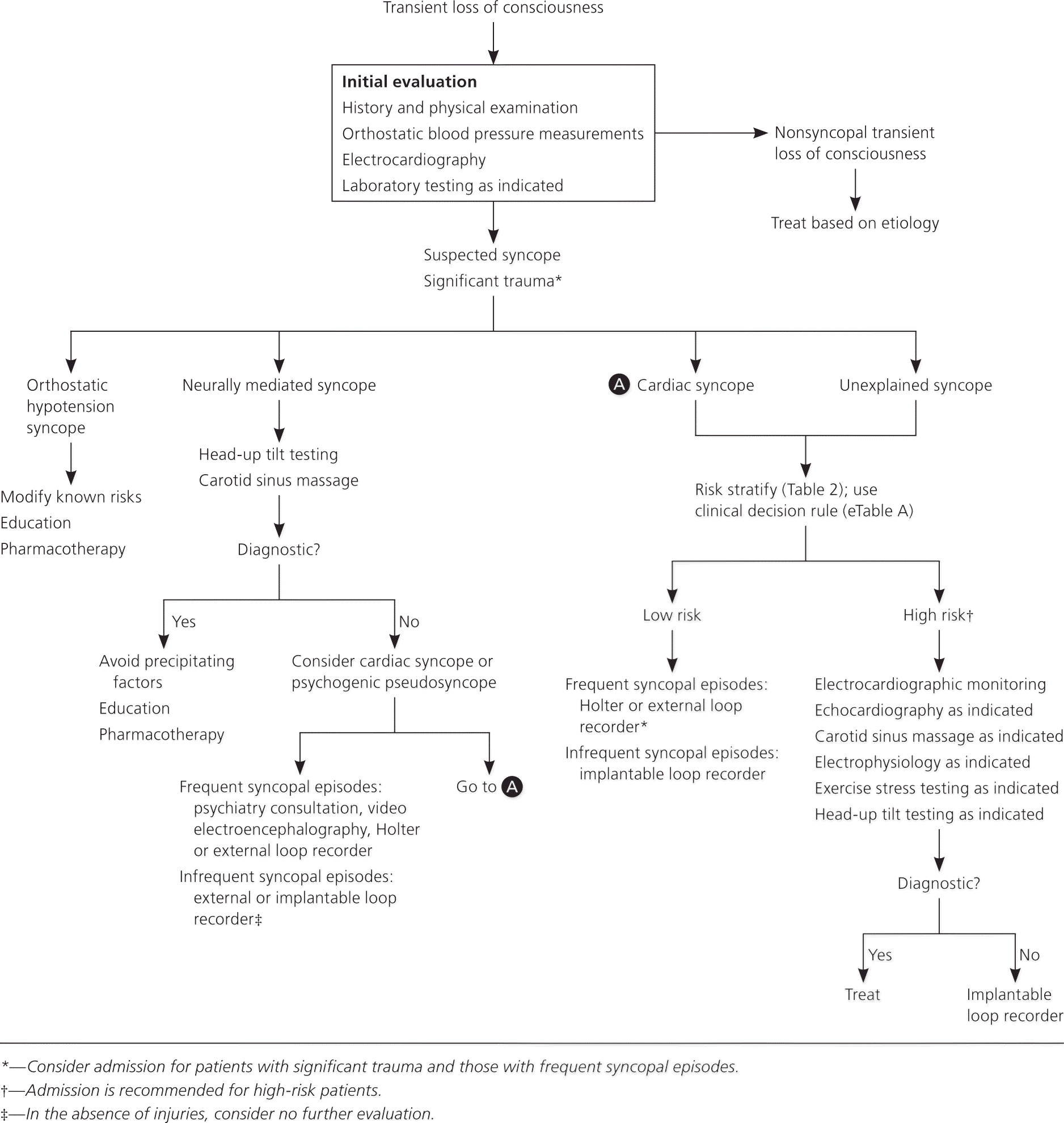
Algorithm for the evaluation of syncope.
Information from reference 2.
HISTORY
A detailed history will suggest a diagnosis in up to 50% of patients and is the most important diagnostic tool in the evaluation of syncope.1 The history should focus on three key elements: (1) Is the loss of consciousness attributable to syncope? (2) Is there a history of cardiovascular disease? (3) Are there clinical features to suggest a specific cause of syncope?30 Pertinent historical elements are listed in Table 3.18,30–33 Medication reconciliation is relevant because medications are contributory in 5% to 15% of syncope cases, typically causing orthostatic hypotension, sedation, symptomatic bradycardia, or QT interval prolongation.34 The history should also assist in classifying patients as low or high risk.
Table 3. Pertinent Historical Information in the Evaluation of Syncope
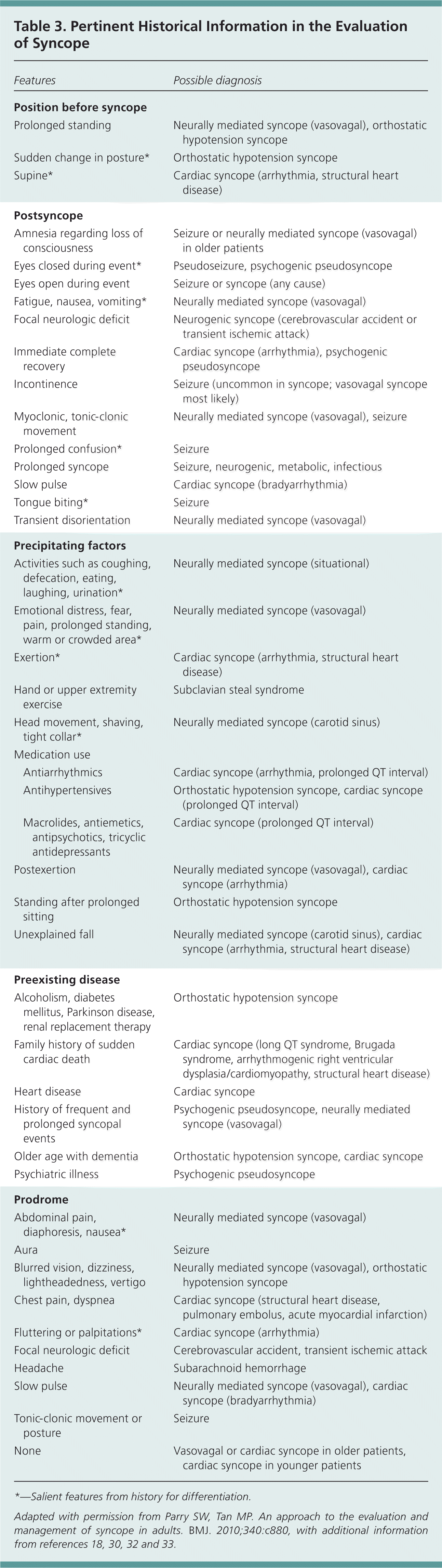
| Features | Possible diagnosis | |
|---|---|---|
| Position before syncope | ||
| Prolonged standing | Neurally mediated syncope (vasovagal), orthostatic hypotension syncope | |
| Sudden change in posture* | Orthostatic hypotension syncope | |
| Supine* | Cardiac syncope (arrhythmia, structural heart disease) | |
| Postsyncope | ||
| Amnesia regarding loss of consciousness | Seizure or neurally mediated syncope (vasovagal) in older patients | |
| Eyes closed during event* | Pseudoseizure, psychogenic pseudosyncope | |
| Eyes open during event | Seizure or syncope (any cause) | |
| Fatigue, nausea, vomiting* | Neurally mediated syncope (vasovagal) | |
| Focal neurologic deficit | Neurogenic syncope (cerebrovascular accident or transient ischemic attack) | |
| Immediate complete recovery | Cardiac syncope (arrhythmia), psychogenic pseudosyncope | |
| Incontinence | Seizure (uncommon in syncope; vasovagal syncope most likely) | |
| Myoclonic, tonic-clonic movement | Neurally mediated syncope (vasovagal), seizure | |
| Prolonged confusion* | Seizure | |
| Prolonged syncope | Seizure, neurogenic, metabolic, infectious | |
| Slow pulse | Cardiac syncope (bradyarrhythmia) | |
| Tongue biting* | Seizure | |
| Transient disorientation | Neurally mediated syncope (vasovagal) | |
| Precipitating factors | ||
| Activities such as coughing, defecation, eating, laughing, urination* | Neurally mediated syncope (situational) | |
| Emotional distress, fear, pain, prolonged standing, warm or crowded area* | Neurally mediated syncope (vasovagal) | |
| Exertion* | Cardiac syncope (arrhythmia, structural heart disease) | |
| Hand or upper extremity exercise | Subclavian steal syndrome | |
| Head movement, shaving, tight collar* | Neurally mediated syncope (carotid sinus) | |
| Medication use | ||
| Antiarrhythmics | Cardiac syncope (arrhythmia, prolonged QT interval) | |
| Antihypertensives | Orthostatic hypotension syncope, cardiac syncope (prolonged QT interval) | |
| Macrolides, antiemetics, antipsychotics, tricyclic antidepressants | Cardiac syncope (prolonged QT interval) | |
| Postexertion | Neurally mediated syncope (vasovagal), cardiac syncope (arrhythmia) | |
| Standing after prolonged sitting | Orthostatic hypotension syncope | |
| Unexplained fall | Neurally mediated syncope (carotid sinus), cardiac syncope (arrhythmia, structural heart disease) | |
| Preexisting disease | ||
| Alcoholism, diabetes mellitus, Parkinson disease, renal replacement therapy | Orthostatic hypotension syncope | |
| Family history of sudden cardiac death | Cardiac syncope (long QT syndrome, Brugada syndrome, arrhythmogenic right ventricular dysplasia/cardiomyopathy, structural heart disease) | |
| Heart disease | Cardiac syncope | |
| History of frequent and prolonged syncopal events | Psychogenic pseudosyncope, neurally mediated syncope (vasovagal) | |
| Older age with dementia | Orthostatic hypotension syncope, cardiac syncope | |
| Psychiatric illness | Psychogenic pseudosyncope | |
| Prodrome | ||
| Abdominal pain, diaphoresis, nausea* | Neurally mediated syncope (vasovagal) | |
| Aura | Seizure | |
| Blurred vision, dizziness, lightheadedness, vertigo | Neurally mediated syncope (vasovagal), orthostatic hypotension syncope | |
| Chest pain, dyspnea | Cardiac syncope (structural heart disease, pulmonary embolus, acute myocardial infarction) | |
| Fluttering or palpitations* | Cardiac syncope (arrhythmia) | |
| Focal neurologic deficit | Cerebrovascular accident, transient ischemic attack | |
| Headache | Subarachnoid hemorrhage | |
| Slow pulse | Neurally mediated syncope (vasovagal), cardiac syncope (bradyarrhythmia) | |
| Tonic-clonic movement or posture | Seizure | |
| None | Vasovagal or cardiac syncope in older patients, cardiac syncope in younger patients | |
*—Salient features from history for differentiation.
Adapted with permission from Parry SW, Tan MP. An approach to the evaluation and management of syncope in adults. BMJ. 2010;340:c880, with additional information from references 18, 30, 32 and 33.
PHYSICAL EXAMINATION
Most patients with syncope will have normal physical examination findings, with the exception of any trauma incurred from the syncopal event. The examination should focus on initial vital signs; orthostatic blood pressure measurements35; and vascular (pulses and carotid bruits), cardiac, pulmonary (evidence of congestive heart failure), abdominal, rectal, and skin/nail (anemia) signs. Any new focal neurologic findings suggest a primary central nervous system lesion.
DIAGNOSTIC TESTING
Carotid sinus massage can be considered in patients older than 40 years to confirm the diagnosis of carotid sinus hypersensitivity. The maneuver is positive when it produces an asystolic or ventricular pause longer than three seconds or a decrease in systolic blood pressure of at least 50 mm Hg. The test is performed while the patient is supine, with five to 10 seconds of massage consecutively to each carotid sinus. It should be performed initially on the right because the maneuver is more often positive on this side. If results are negative, it should be repeated with the patient upright at approximately 60 to 70 degrees.36 This maneuver should be avoided in patients who have had a stroke or transient ischemic attack in the past three months and in patients with carotid bruits. If a positive carotid hypersensitivity test is associated with patient symptoms, then the patient has carotid sinus syndrome.
Routine laboratory studies have low diagnostic yield and should be ordered only if clinically indicated. Laboratory tests can distinguish syncope from other suspected nontraumatic etiologies of loss of consciousness. Elevated troponin and brain natriuretic peptide levels have been shown to predict a higher likelihood of adverse outcomes but should be used only if cardiovascular disease is clinically suspected.26,37,38
ECG generally has a low diagnostic yield (approximately 3% to 5%) but is recommended for all patients with syncope.39,40 Although arrhythmias are unlikely to be detected on a single ECG, ischemic, structural, or conduction abnormalities may be identified. Any ECG abnormality or change from baseline increases the risk of arrhythmia or death within one year of the syncopal event.41
Echocardiography is essential to evaluate suspected structural abnormalities, but it generally has low diagnostic yield. Two studies (n = more than 310) found echocardiography to be clinically useful in patients with syncope if there is a history of cardiac disease, abnormal ECG findings, or suspected significant valvular disease.42,43
Continuous cardiac monitoring is the diagnostic standard to establish a correlation between symptoms and ECG findings. Devices include Holter monitors (generally up to 72 hours), external loop recorders (typically four to six weeks), and implantable loop recorders (up to three years). The diagnostic yield improves with prolonged monitoring. Up to 50% of patients who present with syncope in the absence of heart disease will have an arrhythmia when an implantable loop recorder is placed.44 These devices may increase diagnostic yield, decrease time to diagnosis, and improve cost-effectiveness. Some guidelines recommend them early in the diagnostic workup of unexplained syncope.45–48 Patients most likely to benefit from these devices are those with cardiovascular disease, abnormal baseline ECG findings, cardiac symptoms surrounding the syncopal event, and a family history of sudden cardiac death.39
Provocative testing strategies include head-up tilt testing, exercise testing, and electrophysiologic studies. The head-up tilt test is a safe procedure designed to precipitate hypotension and bradycardia and is used to confirm the diagnosis of neurally mediated syncope in patients with an intermediate pretest probability.11 Persons in high-risk settings with unexplained syncope should also be considered for testing. Protocols using isoproterenol or nitroglycerin have an overall sensitivity of 92% to 94%; however, specificity is low.1,49 Exercise testing is useful in exertional syncope, ischemia, and arrhythmia evaluation. Less than 2% of patients referred to cardiologists for evaluation of unexplained syncope undergo electrophysiologic studies.1 These studies have poor sensitivity and specificity except in the setting of structural heart disease; they have been replaced by noninvasive tools such as prolonged ECG monitoring.1,7 Patients who have an indication for implantable cardioverter-defibrillator placement do not require electrophysiologic studies.
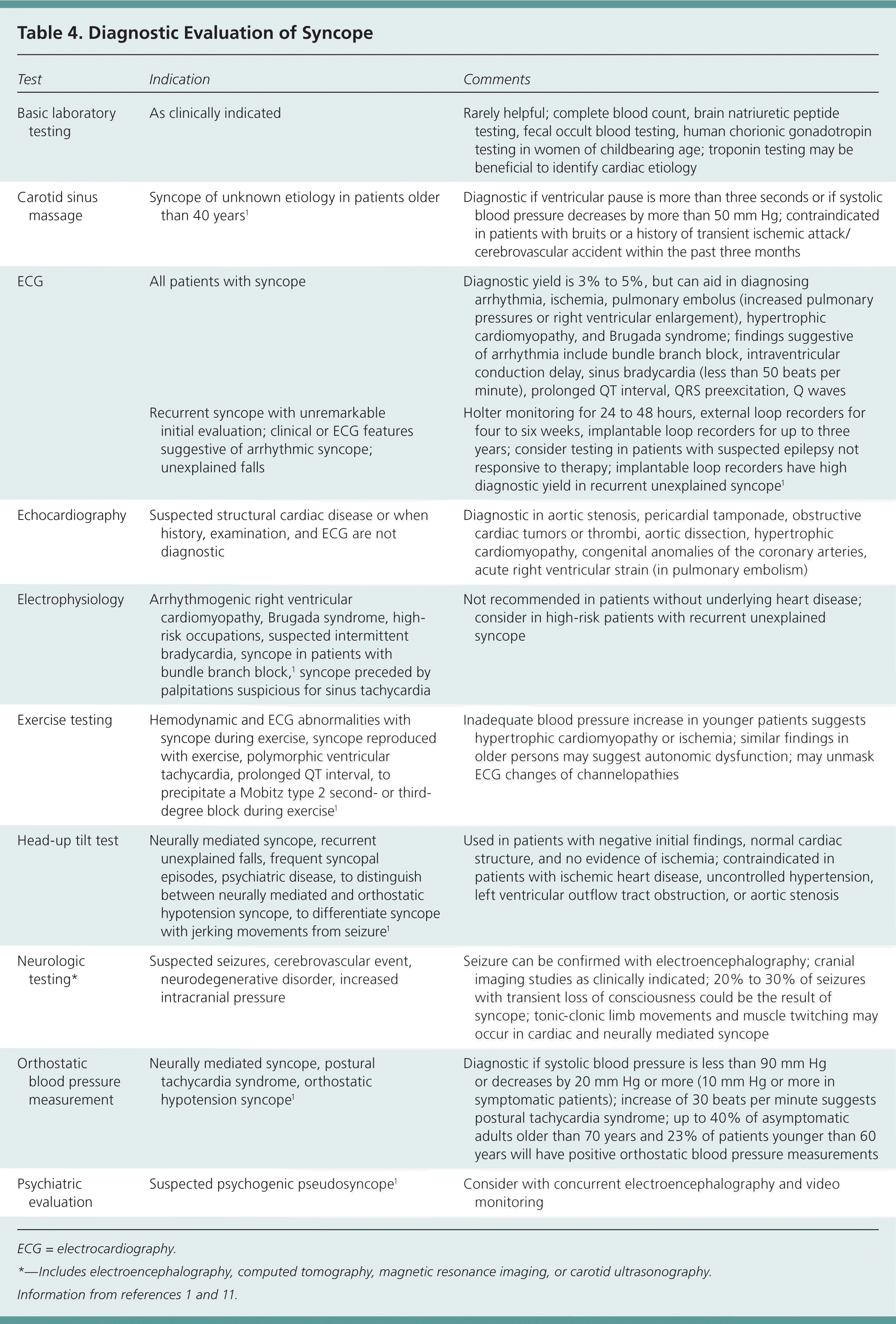
Cranial or cardiac imaging, carotid ultrasonography, electroencephalography, and cardiac enzyme testing are rarely helpful in determining the cause of syncope and should not be ordered routinely. These tests affect diagnosis and management in less than 2% of older patients presenting to the emergency department.40 For most patients with tests results that were significant and affected management, the patient's history indicated the diagnosis.50,51 Table 4 provides an overview of the available testing modalities.1,11
Table 4. Diagnostic Evaluation of Syncope
| Test | Indication | Comments |
|---|---|---|
| Basic laboratory testing | As clinically indicated | Rarely helpful; complete blood count, brain natriuretic peptide testing, fecal occult blood testing, human chorionic gonadotropin testing in women of childbearing age; troponin testing may be beneficial to identify cardiac etiology |
| Carotid sinus massage | Syncope of unknown etiology in patients older than 40 years1 | Diagnostic if ventricular pause is more than three seconds or if systolic blood pressure decreases by more than 50 mm Hg; contraindicated in patients with bruits or a history of transient ischemic attack/cerebrovascular accident within the past three months |
| ECG | All patients with syncope | Diagnostic yield is 3% to 5%, but can aid in diagnosing arrhythmia, ischemia, pulmonary embolus (increased pulmonary pressures or right ventricular enlargement), hypertrophic cardiomyopathy, and Brugada syndrome; findings suggestive of arrhythmia include bundle branch block, intraventricular conduction delay, sinus bradycardia (less than 50 beats per minute), prolonged QT interval, QRS preexcitation, Q waves |
| Recurrent syncope with unremarkable initial evaluation; clinical or ECG features suggestive of arrhythmic syncope; unexplained falls | Holter monitoring for 24 to 48 hours, external loop recorders for four to six weeks, implantable loop recorders for up to three years; consider testing in patients with suspected epilepsy not responsive to therapy; implantable loop recorders have high diagnostic yield in recurrent unexplained syncope1 | |
| Echocardiography | Suspected structural cardiac disease or when history, examination, and ECG are not diagnostic | Diagnostic in aortic stenosis, pericardial tamponade, obstructive cardiac tumors or thrombi, aortic dissection, hypertrophic cardiomyopathy, congenital anomalies of the coronary arteries, acute right ventricular strain (in pulmonary embolism) |
| Electrophysiology | Arrhythmogenic right ventricular cardiomyopathy, Brugada syndrome, high-risk occupations, suspected intermittent bradycardia, syncope in patients with bundle branch block,1 syncope preceded by palpitations suspicious for sinus tachycardia | Not recommended in patients without underlying heart disease; consider in high-risk patients with recurrent unexplained syncope |
| Exercise testing | Hemodynamic and ECG abnormalities with syncope during exercise, syncope reproduced with exercise, polymorphic ventricular tachycardia, prolonged QT interval, to precipitate a Mobitz type 2 second- or third-degree block during exercise1 | Inadequate blood pressure increase in younger patients suggests hypertrophic cardiomyopathy or ischemia; similar findings in older persons may suggest autonomic dysfunction; may unmask ECG changes of channelopathies |
| Head-up tilt test | Neurally mediated syncope, recurrent unexplained falls, frequent syncopal episodes, psychiatric disease, to distinguish between neurally mediated and orthostatic hypotension syncope, to differentiate syncope with jerking movements from seizure1 | Used in patients with negative initial findings, normal cardiac structure, and no evidence of ischemia; contraindicated in patients with ischemic heart disease, uncontrolled hypertension, left ventricular outflow tract obstruction, or aortic stenosis |
| Neurologic testing* | Suspected seizures, cerebrovascular event, neurodegenerative disorder, increased intracranial pressure | Seizure can be confirmed with electroencephalography; cranial imaging studies as clinically indicated; 20% to 30% of seizures with transient loss of consciousness could be the result of syncope; tonic-clonic limb movements and muscle twitching may occur in cardiac and neurally mediated syncope |
| Orthostatic blood pressure measurement | Neurally mediated syncope, postural tachycardia syndrome, orthostatic hypotension syncope1 | Diagnostic if systolic blood pressure is less than 90 mm Hg or decreases by 20 mm Hg or more (10 mm Hg or more in symptomatic patients); increase of 30 beats per minute suggests postural tachycardia syndrome; up to 40% of asymptomatic adults older than 70 years and 23% of patients younger than 60 years will have positive orthostatic blood pressure measurements |
| Psychiatric evaluation | Suspected psychogenic pseudosyncope1 | Consider with concurrent electroencephalography and video monitoring |
ECG = electrocardiography.
*—Includes electroencephalography, computed tomography, magnetic resonance imaging, or carotid ultrasonography. Information from references 1 and 11.
Treatment
The treatment of syncope is directed at the underlying cause. Morbidity and mortality are generally low except in cardiac syncope; therefore, patient reassurance is an important part of treatment.
NEURALLY MEDIATED SYNCOPE
Treatment of neurally mediated syncope includes reassurance, education, and physical therapy.1 In situational syncope, it is important to avoid potential triggers. Physical counterpressure maneuvers such as leg crossing, squatting, and tensing the lower extremities are effective at the onset of prodromal symptoms.7 One randomized trial showed that these maneuvers reduce syncope by 39%.52 Tilt training involves standing for prolonged periods, and compliance is generally poor.7
Pharmacologic therapy with beta blockers, alpha agonists, and fludrocortisone has shown no effectiveness or conflicting results in reducing vasovagal syncope.1 In one small randomized trial of patients with a history of recurrent vasovagal syncope, paroxetine (Paxil) prevented additional episodes in 82.4% compared with 47.1% in the placebo group over two years (P < .001), although guidelines recommend its use only in patients with concurrent psychiatric disease.53 In patients with severe asystole from neurally mediated syncope, a double-blind, randomized, placebo-controlled trial showed that the use of permanent dual chamber pacing reduced the risk of recurrent syncope.54
ORTHOSTATIC HYPOTENSION
Treatment of orthostatic hypotension includes education and lifestyle modifications, such as slowly transitioning from a supine or sitting position to standing and increasing fluid and sodium intake.1 Contributing medications should be discontinued or decreased, if possible. Other treatment modalities include elevating the head of the bed by 10 degrees, compression stockings/abdominal binders, and counterpressure maneuvers.1 If these do not mitigate symptoms, midodrine and fludrocortisone are effective treatments.55
CARDIAC SYNCOPE
Management of cardiac syncope is directed at the underlying etiology. Options include antiarrhythmic drugs, cardiac pacing, catheter-directed ablation, and, rarely, implantable cardioverter-defibrillator placement.1
This article updates previous articles on this topic by Gauer,56 and by Miller and Kruse.57
Data Sources: We searched OvidSP, Essential Evidence Plus, the National Guideline Clearinghouse, Cochrane Library, and UpToDate using combinations of the following key words: syncope, transient loss of consciousness, presyncope, clinical decision rules, risk stratification, mortality, morbidity, etiology, incidence, electrocardiographic monitoring, electrophysiologic studies, diagnostic evaluation, hospitalization, brain natriuretic peptide, troponin, cardiac enzymes, implantable loop recorders, cost, quality of life, carotid sinus massage, head-up tilt table, implantable cardioverter defibrillator, guidelines, orthostatic hypotension, diagnostic evaluation, medical cost, postural tachycardia syndrome. Search dates: June 22 to August 6, 2015, and October 15, 2016.
The opinions or assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the Department of Defense.

