Family physicians should be proficient in geriatric assessment because, as society ages, older adults will constitute an increasing proportion of patients. Geriatric assessment evaluates medical, social, and environmental factors that influence overall well-being, and addresses functional status, fall risk, medication review, nutrition, vision, hearing, cognition, mood, and toileting. The Medicare Annual Wellness Visit includes the key elements of geriatric assessment performed by family physicians. Comprehensive geriatric assessment can lead to early recognition of problems that impair quality of life by identifying areas for focused intervention, but a rolling geriatric assessment over several visits can also effectively identify subtle or hidden problems. Assessment should be tailored to patient goals of care and life expectancy. By asking patients and families to self-assess risks using precompleted forms, and by using trained office staff to complete validated assessment tools, family physicians can maximize efficiency by focusing on identified problems. Fall risk can be assessed with a single screening question: “Have you fallen in the past year?” The Beers, STOPP (screening tool of older persons' prescriptions), and START (screening tool to alert doctors to right treatment) criteria are helpful resources for reviewing the appropriateness of medications in older adults. Screening for depression is recommended when depression care supports are available; this can be performed with a brief two-item screen, the Patient Health Questionnaire-2. Older adults should be screened for unintentional weight loss and malnutrition. Although rates of hearing loss and vision loss increase with age, there is insufficient evidence to recommend screening in asymptomatic individuals. The U.S. Preventive Services Task Force advises clinicians to assess cognition when there is suspicion of impairment. Urinary incontinence can impair patients' quality of life, and it can be assessed with a two-question screening tool. Immunizations and advance care planning are also important components of the geriatric assessment.
Older adults with complex chronic conditions will be an increasing proportion of family physicians' patient population. In 2015, patients older than 65 years accounted for 31% of all U.S. office visits, and that proportion will grow.1 Since 2013, every day 10,000 baby boomers turn 65 years of age and enter Medicare.2 By 2030, the population older than 65 years will double to 72 million (20% of the total U.S. population).2 Individuals are living longer, with multiple chronic illnesses, making them vulnerable to disability and diminished quality of life. Although 95% of older patients with complex needs have regular access to care, 58% struggle to navigate the system, and 62% are stressed about their ability to afford housing, utilities, or meals.3 Geriatric assessment, which evaluates medical problems; cognitive, affective, and functional abilities; and social and environmental factors, can identify these unrecognized needs to improve the well-being of older adults.
Evidence Base for Comprehensive Geriatric Assessment
Most of the literature supporting geriatric assessment models involves specialized geriatric team-based assessment. Comprehensive geriatric assessment is a systematic evaluation of frail older persons by a team of health professionals and consists of six core components: data gathering, team discussion, development of a treatment plan, and implementation of a treatment plan, with monitoring and revision as needed.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
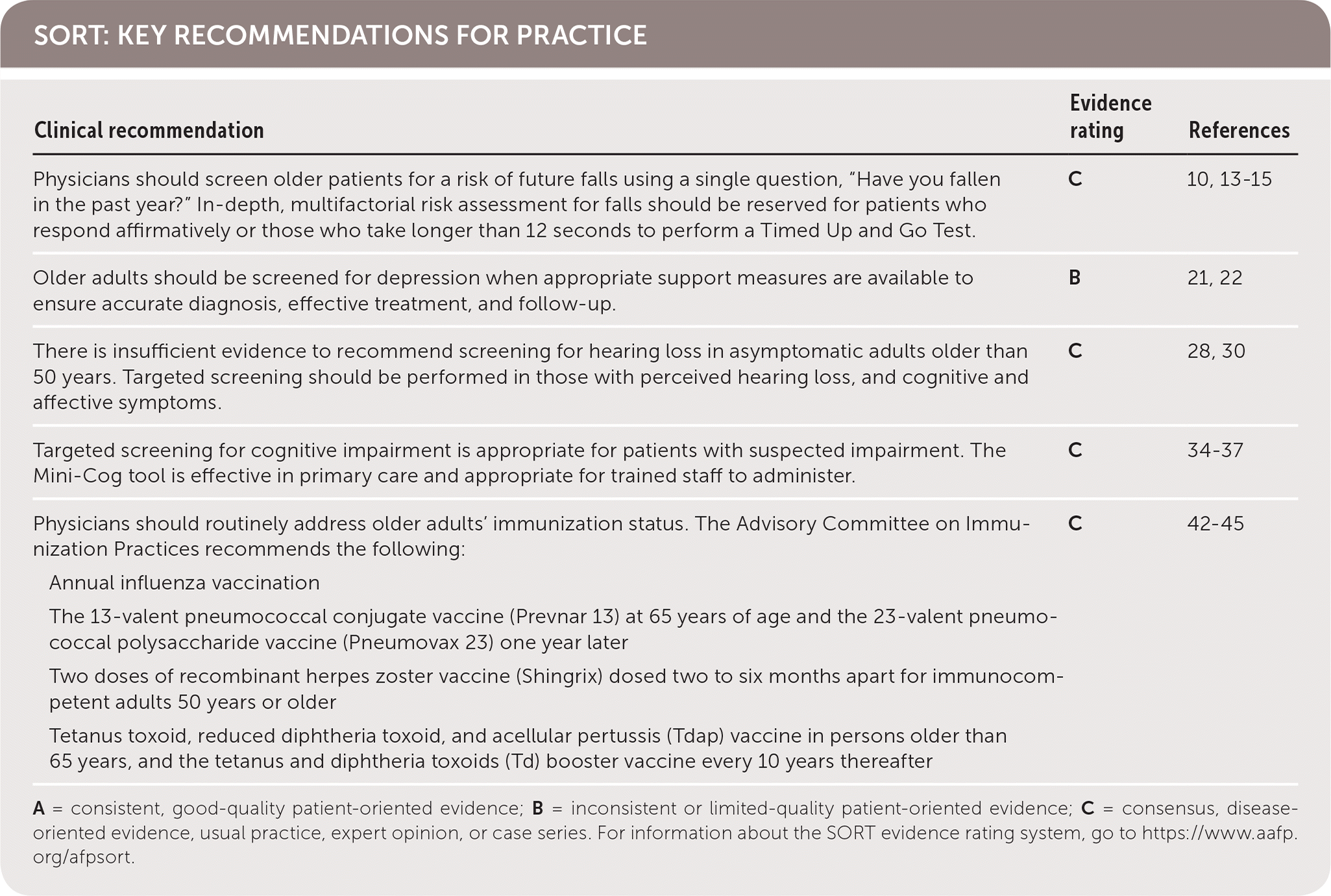
| Physicians should screen older patients for a risk of future falls using a single question, “Have you fallen in the past year?” In-depth, multifactorial risk assessment for falls should be reserved for patients who respond affirmatively or those who take longer than 12 seconds to perform a Timed Up and Go Test. | C | 10, 13–15 |
| Older adults should be screened for depression when appropriate support measures are available to ensure accurate diagnosis, effective treatment, and follow-up. | B | 21, 22 |
| There is insufficient evidence to recommend screening for hearing loss in asymptomatic adults older than 50 years. Targeted screening should be performed in those with perceived hearing loss, and cognitive and affective symptoms. | C | 28, 30 |
| Targeted screening for cognitive impairment is appropriate for patients with suspected impairment. The Mini-Cog tool is effective in primary care and appropriate for trained staff to administer. | C | 34–37 |
Physicians should routinely address older adults' immunization status. The Advisory Committee on Immunization Practices recommends the following:
|
C | 42–45 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN GERIATRIC MEDICINE
| Recommendations from the Choosing Wisely Campaign | |
|---|---|
| Recommendation | Sponsoring organization |
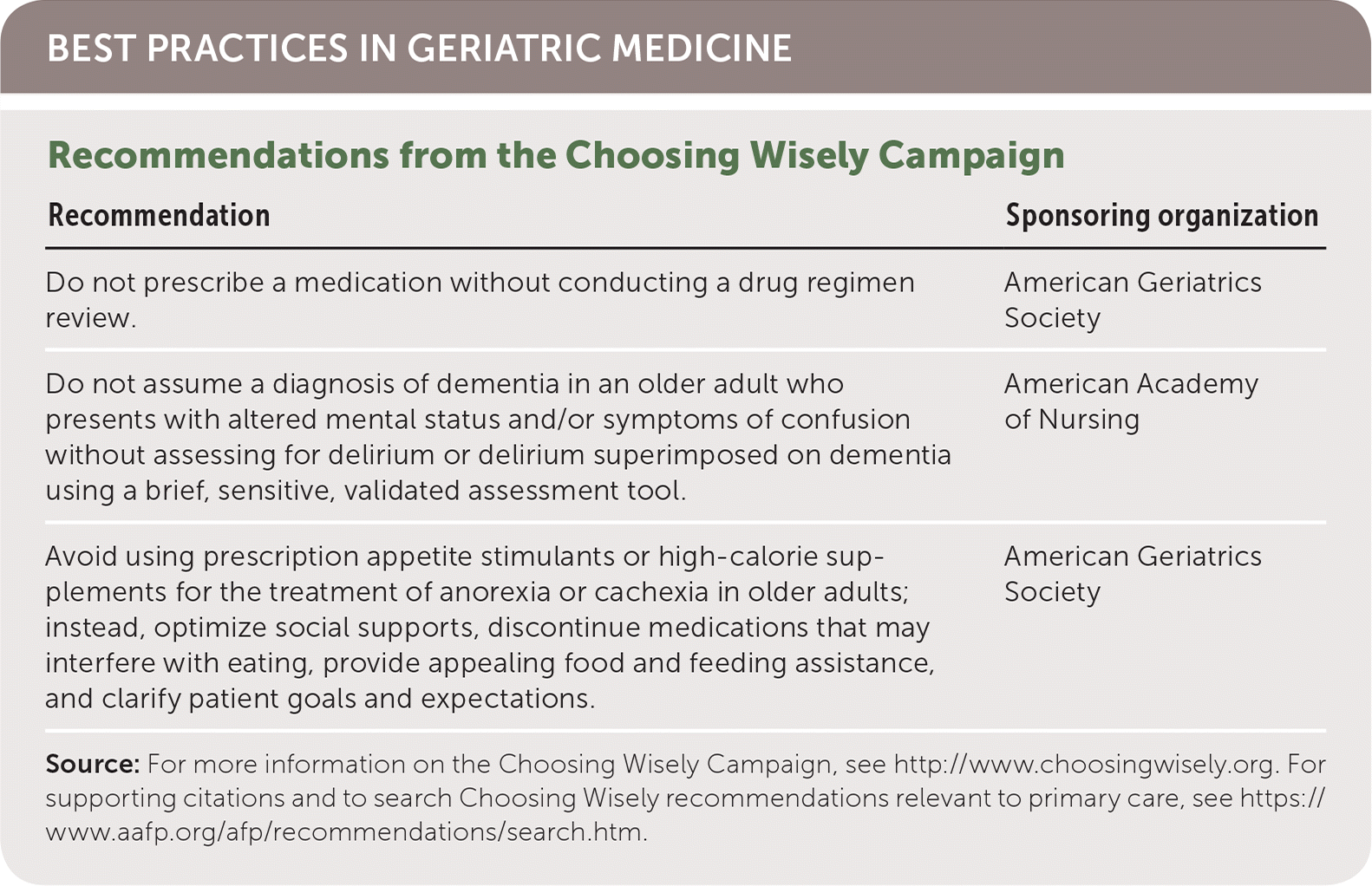
| Do not prescribe a medication without conducting a drug regimen review. | American Geriatrics Society |
| Do not assume a diagnosis of dementia in an older adult who presents with altered mental status and/or symptoms of confusion without assessing for delirium or delirium superimposed on dementia using a brief, sensitive, validated assessment tool. | American Academy of Nursing |
| Avoid using prescription appetite stimulants or high-calorie supplements for the treatment of anorexia or cachexia in older adults; instead, optimize social supports, discontinue medications that may interfere with eating, provide appealing food and feeding assistance, and clarify patient goals and expectations. | American Geriatrics Society |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
The comprehensive geriatric assessment model has been studied in hospital, home care, and clinic settings. Virtually all trials of this model improved detection and documentation of problems in this population, but the impact on patient-oriented outcomes varied.4 A meta-analysis of 29 trials showed that hospitalized older adults treated by a comprehensive geriatric assessment team were more likely to be alive and in their own homes 12 months after hospitalization.5 In a survey of primary care physicians in a preferred provider organization who had referred patients for geriatric assessment, 69% of respondents agreed that outpatient comprehensive geriatric assessment more fully assessed the physical, mental, and social needs of patients than other consultative clinics.6
Geriatric Assessment in the Family Physician's Office
Although formal comprehensive geriatric assessment includes a large team of clinicians, individual family physicians must use the interprofessional resources available. Geriatric assessment by an individual clinician expands the focus from a traditional disease-oriented visit to assess for common underreported conditions affecting quality of life and functional status.
Geriatric assessment is labor- and time-intensive, and, therefore, should target patients who can most benefit. Possible triggers for an assessment include multimorbidity, cognitive changes, functional status changes, frailty, risk of falling, medication nonadherence, polypharmacy, transitions in care setting, unexplained weight loss, and family concerns for safety. Geriatric assessment is generally not as useful in patients with terminal illness, advanced dementia, or complete functional dependence. To overcome the time-intensity barriers, which are a challenge for patients and clinicians, family physicians can adapt the comprehensive geriatric assessment into their clinics in a variety of ways. Portions of the geriatric assessment can be performed over several regularly scheduled visits. Targeting at least one domain for screening during each office visit can be integrated into staff workflow with the use of structured templates to guide evaluation of problems such as falls, dementia, or urinary incontinence.
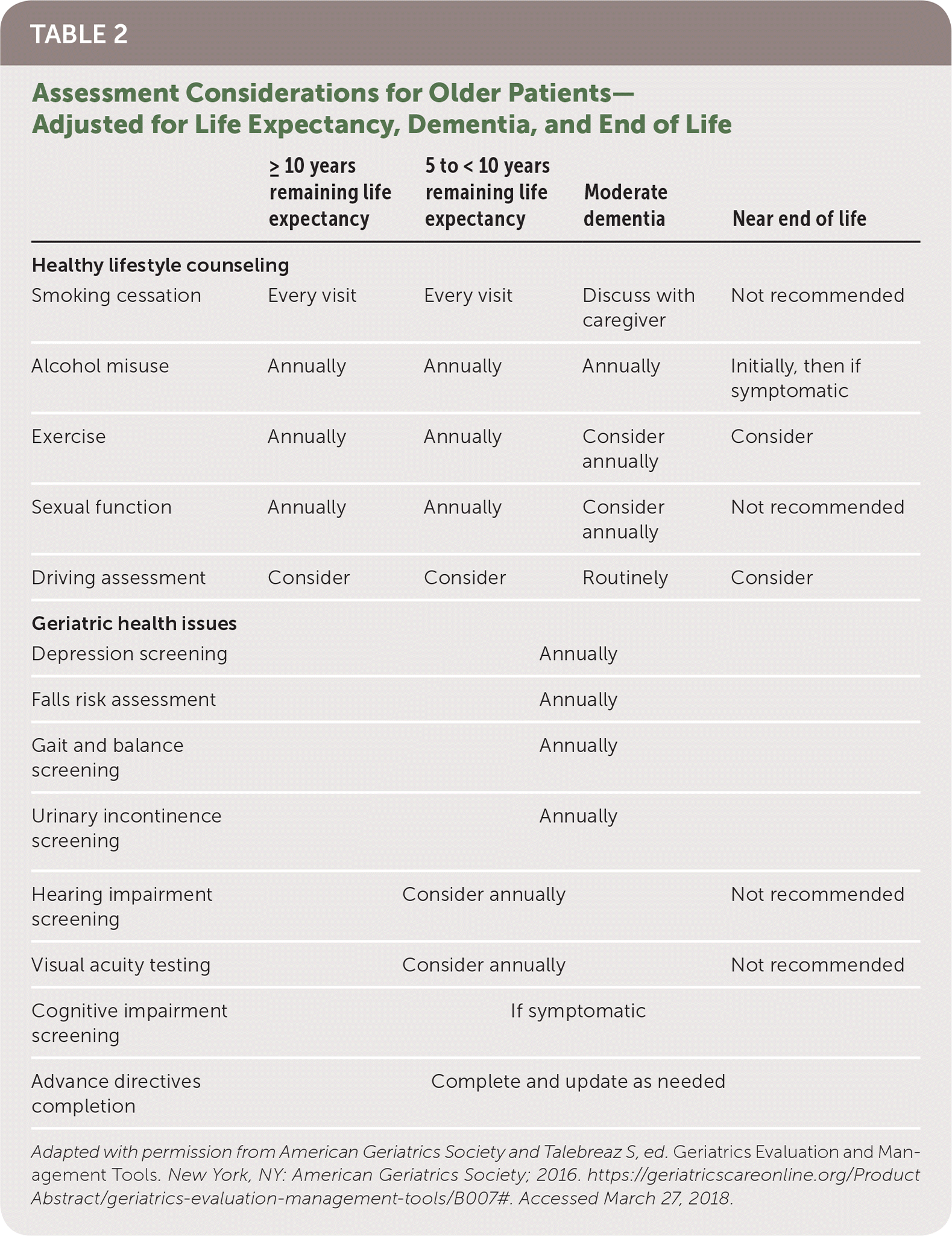
Medicare's Annual Wellness Visit is an opportunity to incorporate geriatric assessment into a single office visit. The elements of the Annual Wellness Visit are listed in Table 1, with suggested tools for assessment in addition to several new billing codes.7 Screening and counseling should be adjusted based on prognosis and life expectancy (Table 2).8
TABLE 1. Geriatric Assessment Components in the Medicare Annual Wellness Visit

| Action | Elements and interventions |
|---|---|
| Data collected before the physician enters the examination room (completed by the patient or family member in 20 minutes or less) | |
| Identify all current clinicians and medical suppliers | — |
| Perform health risk assessment | Self-assessment of health status: excellent, good, fair, poor |
| Psychosocial risks | |
| Behavioral risks (e.g., alcohol, drug, and tobacco use; new sex partners) | |
| Activities of daily living (e.g., dressing, toileting, bathing, walking, feeding) | |
| Instrumental activities of daily living (e.g., shopping, housekeeping, managing medications, handling finances) | |
| Review and update medical/family history and comprehensive pharmaceutical review | Update recent medical events |
| Obtain family history targeted to history of longevity, cognitive impairment, and parents' and siblings' end-of-life experiences | |
Perform medication review for potentially inappropriate medications
| |
| Review medication list for vitamins and supplements, and potential medication interactions | |
| Screen for depression | Patient Health Questionnaire-2, Patient Health Questionnaire-9, five- or 15-item Geriatric Depression Scale |
| Screen for functional status and safety | Do you need help with dressing, toileting, bathing, walking, or feeding? |
| In the past year, have you fallen? | |
| Do you feel you have hearing loss? | |
| Home Safety Self-Assessment Tool | |
| Screen for urinary incontinence | In the past year, have you ever lost your urine and gotten wet? |
| If so, have you lost your urine on at least six separate days? | |
| Screen for weight loss or malnutrition | Have you lost weight in the previous six months? |
| For targeted screening, consider the Mini Nutritional Assessment | |
| Data collected by physician | |
| Assessment | Perform required elements from the Centers for Medicare and Medicaid Services:
|
Suggested other assessments:
| |
| Counseling | Review age-appropriate prevention measures covered by Medicare (Table 2) |
| Review recommendations from the U.S. Preventive Services Task Force and the Advisory Committee on Immunization Practices | |
Give targeted health advice and make appropriate referrals:
| |
| Billing codes | |
| G0438 | Annual Wellness Visit; includes a personalized prevention plan of service, initial visit |
| G0439 | Annual Wellness Visit; includes a personalized prevention plan of service, subsequent visit |
| 99497 | Advance care planning including the explanation and discussion of advance directives such as standard forms (with completion of such forms, when performed) by the physician or other qualified health care professional; first 30 minutes, face-to-face with the patient, family member(s), and/or surrogate |
| 99498 | Advance care planning including the explanation and discussion of advance directives such as standard forms (with completion of such forms, when performed) by the physician or other qualified health care professional; each additional 30 minutes (list separately in addition to code for primary procedure) |
Note: See the FPM Toolbox for additional resources for the Medicare Annual Wellness visit: https://www.aafp.org/fpm/toolBox/viewToolType.htm?toolTypeId=20.
START = screening tool to alert doctors to right treatment; STOPP = screening tool of older persons' prescriptions.
Information from reference 7.
TABLE 2. Assessment Considerations for Older Patients—Adjusted for Life Expectancy, Dementia, and End of Life
| ≥ 10 years remaining life expectancy | 5 to < 10 years remaining life expectancy | Moderate dementia | Near end of life | |
|---|---|---|---|---|
| Healthy lifestyle counseling | ||||
| Smoking cessation | Every visit | Every visit | Discuss with caregiver | Not recommended |
| Alcohol misuse | Annually | Annually | Annually | Initially, then if symptomatic |
| Exercise | Annually | Annually | Consider annually | Consider |
| Sexual function | Annually | Annually | Consider annually | Not recommended |
| Driving assessment | Consider | Consider | Routinely | Consider |
| Geriatric health issues | ||||
| Depression screening | Annually | |||
| Falls risk assessment | Annually | |||
| Gait and balance screening | Annually | |||
| Urinary incontinence screening | Annually | |||
| Hearing impairment screening | Consider annually | Not recommended | ||
| Visual acuity testing | Consider annually | Not recommended | ||
| Cognitive impairment screening | If symptomatic | |||
| Advance directives completion | Complete and update as needed | |||
Adapted with permission from American Geriatrics Society and Talebreaz S, ed. Geriatrics Evaluation and Management Tools. New York, NY: American Geriatrics Society; 2016. https://geriatricscareonline.org/ProductAbstract/geriatrics-evaluation-management-tools/B007#. Accessed March 27, 2018.
Team-Based Data Collection from Patients and Caregivers
To maximize efficiency, physicians may delegate data-gathering to leave more time for addressing problems. Validated screening instruments completed by trained office staff, as well as patient- and caregiver-completed tools, can be used to collect information on history, prevention measures, and functional status (eTable A).
eTABLE A Pre–Physician Visit Geriatric Assessment Forms
| Completion | ||
|---|---|---|
| Patient/family | Trained staff | |
| Functional status | ||
| Home Safety Self-Assessment Tool | x | |
| Katz Index of Independence in Activities of Daily Living | x | |
| Lawton Instrumental Activities of Daily Living Scale | x | |
Timed Up and Go Test
|
x | |
Tinetti Balance Assessment Tool
|
x | |
| Nutrition | ||
| Mini Nutritional Assessment | x | |
| Advance care planning | ||
| Conversation Project (family discussion guides) | x | |
| Prepare for Your Care (self-completed goal assessment tool) | x | |
| Stanford Letter Project (allows patients to write a letter to their physician or a life review letter to a family member) | x | |
| Cognition* | ||
| Mini-Cog examination | x | |
| Montreal Cognitive Assessment | x | |
| Depression | ||
| Geriatric Depression Scale | x | |
| Patient Health Questionnaire-2 | x | |
Patient Health Questionnaire-9
|
x | |
*—Additional resources from the AAFP's Cognitive Care Kit are available at https://www.aafp.org/patient-care/public-health/cognitive-care.html.
Geriatric Conditions
FUNCTIONAL STATUS AND FALLS
Precompleted basic and instrumental activities of daily living scales may identify declines in functional status. For highly functional patients, a simple open-ended question asking how a typical day is spent provides a good review of daily function.
Falls are common and often unreported. One-third of community-dwelling individuals older than 65 years fall every year.9 A single screening question, “Have you fallen in the past year?” is highly effective. A positive response is associated with a 2.8-times higher likelihood of falling in the next year.10 The American Academy of Family Physicians (AAFP) does not recommend an automatic comprehensive fall assessment, but it should be considered in the context of individual patient needs.11
Physician assessment of gait can begin with direct observation as the patient enters the examination room. Reduced gait speed has been associated with reduced survival in pooled analysis of nine cohort studies, and patients with slow gait are more likely to fall.12 The Get Up and Go Test measures a patient's ability to rise from a chair, walk 3 m (10 ft), turn, walk back, and sit down again. Evaluation by the family physician may be a simple qualitative assessment of normal or impaired, but if staff are assessing, then a timed score with the Timed Up and Go Test may be preferable (Table 3).13,14 A patient who takes longer than 12 seconds on the Timed Up and Go Test or a physician assessment that gait is mildly abnormal or worse should be evaluated further. Patients at high risk of falling need a multifactorial assessment including orthostatic vital signs, visual acuity testing and cataract screening, gait and balance testing, medication review, and investigation of environmental hazards in the home.15
TABLE 3. Rapid Gait Assessment and Scoring

| Instructions | |
| Sit comfortably in a straight-backed chair | |
| Use your typical walking aid | |
When I say “go,” I want you to:
| |
| Scoring | |
| Qualitative scoring (when a physician administers the test): Get Up and Go Test | |
| Observe the patient's movements for any deviation from a confident, normal performance | |
Intermediate grades reflect the presence of any of the following as indicators of the possibility of falling: undue slowness, hesitancy, abnormal movements of the trunk or upper limbs, staggering, or stumbling
| |
| Quantitative scoring (when trained staff administer the test): Timed Up and Go Test | |
| On the word “go,” begin timing | |
| Stop timing after the patient sits back down, and record total time | |
| Any adult who takes longer than 12 seconds to complete is at high risk of falling | |
Early identification of functional decline and fall risk can lead to interventions that maximize independence and safety. Effective multifactorial interventions such as regular exercise and balance training, minimizing polypharmacy, treating visual impairment, managing hypotension, and using proper footwear can reduce the frequency of falling and may help maintain functional status.10 The U.S. Preventive Services Task Force (USPSTF) recommends exercise to prevent falls (grade B) and that clinicians selectively offer multifactorial interventions to prevent falls to community-dwelling adults 65 years or older who are at increased risk of falls. The USPSTF also cautions that patients and clinicians should consider the balance of benefits and harms based on the circumstances of prior falls, presence of comorbid medical conditions, and the patient's values and preferences.16
POLYPHARMACY
Increased use of prescription and over-the-counter medications puts older adults at risk of adverse drug reactions, impaired cognition, falls, and functional decline.17 A thorough medication review can identify medications that are underprescribed and necessary, those that are not being used correctly, and those that are inappropriate and should be discontinued. The Beers, STOPP (screening tool of older persons' prescriptions), and START (screening tool to alert doctors to right treatment) criteria are helpful resources for reviewing the appropriateness of medications in older adults.18,19 The Beers criteria list potentially inappropriate medications for most older adults, medications to avoid with specific conditions, combinations that may lead to harmful interactions, and medications that should be dosed differently for persons with poor kidney function.18 STOPP and START comprise clinically significant criteria for potentially inappropriate prescribing in older persons and potential prescribing omissions.19 When reviewing medications for older adults, it is important to take into account the patient's ability to adhere to the medication regimen, the patient's goals of treatment, and the time to achieve benefit from the medication in relation to the patient's life expectancy. Strategies to improve adherence include using pillboxes, easy-open lids on bottles, daily organized medications in blister packs, once-daily medications instead of more frequent administration, and direct patient education with a pharmacist.
DEPRESSION
Depression in older adults often presents in an atypical manner, such as apathy, weight loss, or cognitive impairment (e.g., responding to questions with “I don't know”), especially when there is comorbid cognitive impairment. Depression can lead to significant weight loss, decline in functional status, increased risk of suicide, and overall increased mortality and increased use of health care services.20
The USPSTF and the AAFP recommend screening adults for depression only when staff-assisted depression care supports are available for accurate diagnosis, effective treatment, and follow-up.21,22 Screening for depression can be performed with a brief two-item screen, the Patient Health Questionnaire-2 (PHQ-2).23 A positive result (score of 3 or greater) on the simple screen should be followed by the Patient Health Questionnaire-9, which has been validated as a reliable measure of depression severity in older adults.24
WEIGHT LOSS AND MALNUTRITION
Undernutrition is associated with increased need for health care services and mortality. Among older adults receiving home health care, 12% were malnourished and 51% were at risk of malnourishment.25 Medicare defines normal body mass index (BMI) in older adults as 23 to 30 kg per m2; BMI less than 23 kg per m2 is associated with increased mortality.26 Screening for nutritional impairment in older adults can be accomplished by asking a single question (e.g., “Have you lost weight in the past six months?”), monitoring weight, or asking patients or caregivers to complete the Mini Nutritional Assessment (eTable A). Older adults who unintentionally lose 5% or more of their body weight in six months or have a low BMI require further evaluation for poor nutrition. Through the Choosing Wisely Campaign, the American Geriatrics Society recommends against the use of appetite stimulants or high-calorie supplements because of the lack of proven effectiveness in long-term survival or improvement in quality of life. Instead, it recommends discontinuing medications that contribute to weight loss and diminish appetite, providing appealing foods, ensuring social support, and offering feeding assistance.27
HEARING AND VISION
Hearing loss is often unrecognized by patients, and affects more than 80% of adults older than 80 years. Only 10% to 20% of older adults with hearing loss have used hearing aids.28 Moderate to severe hearing loss is associated with a three- to fourfold higher incidence of dementia.29 The USPSTF and the AAFP concluded that there was insufficient evidence to recommend screening for hearing loss in asymptomatic adults older than 50 years.28,30 Physicians should assess for objective hearing impairment when the patient or a family member raises a concern, or if there are cognitive or mood symptoms that could be influenced by hearing loss, and refer for hearing aids when appropriate. Although audiometry is the screening standard, a whispered voice test at 2 ft or a single question (e.g., “Do you feel you have hearing loss?”) is an effective alternative.30
Vision loss is common among older adults in the United States, affecting 12% of those 65 to 74 years of age and 15% of those 75 years and older.31 Common causes of visual impairment include macular degeneration, cataracts, glaucoma, refractive errors, and diabetic retinopathy. Decreased visual acuity increases the risk of falls, fractures, social isolation, and depression. In 2016, the USPSTF and AAFP concluded that the current evidence was insufficient to assess the balance of benefits and harms of screening for impaired visual acuity in older adults.32,33 Despite lack of evidence of benefit, vision testing offers little harm and can be accomplished by office staff using a Snellen chart.
COGNITION
Cognitive impairment rates increase with age. In primary care, impaired cognition may go unrecognized in up to 81% of affected patients.34 The USPSTF and AAFP concluded that there is insufficient evidence for screening for cognitive impairment, but the USPSTF advises clinicians to assess cognition when there is suspicion of impairment.35,36 The Medicare Annual Wellness Visit requires assessment of cognitive function by direct observation, self-report, and concerns raised by family members, care-givers, or others.7 A brief, structured cognitive assessment using the Mini-Cog tool improves primary care physicians' spontaneous detection of mild cognitive impairment or dementia from 59% to 83%.37 The Mini-Cog test combines three-item recall and clock drawing, and has been validated against the Mini-Mental State Examination.38 Medical staff can administer the Mini-Cog in five minutes or less.34 The Mini-Mental State Examination, although well known and well studied, has fallen out of favor because of copyright fees.
Positive results on a cognitive screening test do not diagnose dementia, but should lead to more comprehensive evaluation of memory, language, visual-spatial, and executive function, as well as how identified deficits interfere with daily activities. The Montreal Cognitive Assessment is one tool that assesses these domains in depth. AAFP's Cognitive Care Kit includes several other validated, evidence-based instruments for cognitive evaluation (eTable A).
Although no pharmacologic agents are indicated for patients identified with mild cognitive impairment but not dementia, an exercise prescription is an appropriate intervention. A meta-analysis of 11 studies showed that exercise improved global cognition, and an aerobic component to the exercise appears to be important.39
URINARY INCONTINENCE
Urinary incontinence is a common condition impacting 70% of long-term nursing home residents, and 24% of community-dwelling older adults experience incontinence that is rated as moderate to very severe.40 Although the incidence increases with age, urinary incontinence is abnormal at any age and significantly affects quality of life.
Incontinence is often unidentified because of embarrassment. A two-question screening tool is effective in identifying urinary incontinence: (1) In the past year, have you ever lost your urine and gotten wet? and (2) If so, have you lost your urine on at least six separate days? 41 Positive responses to both questions should lead to a more in-depth assessment of transient and established factors that are contributing to the incontinence.
IMMUNIZATIONS
Geriatric assessment is an opportunity to identify older adults who have not received recommended vaccinations. Patients older than 60 years account for 60% of tetanus cases and more than 90% of influenza deaths, and the morbidity of pneumonia and zoster greatly increases after 65 years of age. The Advisory Committee on Immunization Practices (ACIP) recommends annual influenza vaccination.42 It also recommends that clinicians not miss the opportunity to vaccinate persons older than 65 years with the tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) vaccine and the tetanus and diphtheria toxoids (Td) booster vaccine every 10 years thereafter.43 For pneumonia vaccination, the ACIP recommends the 13-valent pneumococcal conjugate vaccine (Prevnar 13) at 65 years of age and the 23-valent pneumococcal polysaccharide vaccine (Pneumovax 23) one year later.44 The ACIP recommends two doses of recombinant herpes zoster vaccine (Shingrix) administered two to six months apart for immunocompetent adults 50 years or older.45
ADVANCE CARE PLANNING
Geriatric assessment provides opportunity to review preferences for medical care, such as prolonging life, maintaining independence, preventing illness, relieving suffering, and maximizing time with family and friends. Understanding these goals should inform specific treatment plans, including preferences for preventive care and decisions regarding life-sustaining treatments. Completion of advance directives should document patient goals and preferences for future medical care, and identify the patient's chosen surrogate decision maker. This is a particular priority when dementia is diagnosed and some partial decision making is preserved.
There are several evidence-based tools to engage older adults in shared decision making.46,47 Resources such as the Prepare for Your Care48 (https://www.prepareforyourcare.org/) and the Stanford Letter Project (https://med.stanford.edu/letter.html) websites can help persons prioritize goals and facilitate advance care planning before the office visit.
Post-Assessment
Once assessment is complete, the problem list should be updated with newly identified geriatric syndromes, and care plans should be modified based on patient goals. eTable B provides a compendium of practice recommendations from American Family Physician for subsequent management of geriatric conditions.
eTABLE B Selected Key Post-Assessment Recommendations for Geriatric Evaluation and Management from American Family Physician
| Topic and article | Key recommendations |
|---|---|
| Falls | |
| Preventing Falls in Older Persons* | Community-dwelling older persons at high risk of falls should receive a multifactorial risk assessment and intervention tailored to their needs. |
| Older persons at risk of falls who are hospitalized in an acute setting or for an extended time in a subacute setting should receive a multifactorial risk assessment and intervention tailored to their needs. | |
| Nursing home residents at risk of falls should receive a multifactorial risk assessment and intervention tailored to their needs and administered by a multidisciplinary team. | |
Components to include in multifactorial interventions for falls in older persons:
| |
| Dual chamber cardiac pacing should be considered in patients with carotid sinus hypersensitivity who experience unexplained recurrent falls. | |
| Geriatric Assistive Devices | Assistive devices can be prescribed to improve balance, reduce pain, and increase mobility and confidence. |
| Because most patients obtain their assistive device without recommendations or instructions from a medical professional, assistive devices should be evaluated routinely for proper fit and use. | |
| When only one upper extremity is needed for balance or weight bearing, a cane is preferable. If both upper extremities are needed, crutches or a walker is more appropriate. | |
| The correct height of cane or walker is at level of the patient's wrist crease. Measure with patient standing upright with arms relaxed at sides. When holding the device at this height, patient's elbow is naturally flexed at 15- to 30-degree angle. | |
| Gait and Balance Disorders in Older Adults | Gait and balance disorders are usually multifactorial in origin and require a comprehensive assessment to determine contributing factors and targeted interventions. |
| Older adults should be asked at least annually about falls, and older adults who report a fall should be observed for any gait or balance disturbances. | |
| Exercise and physical therapy can help improve gait and balance disorders in older adults. | |
| Declining functional status | |
| Functional Decline in Older Adults | Evaluate new or progressive disability in older adults with careful assessment for underlying health conditions, impairments, and contextual factors. |
| Treatment of disability: use strategies to increase the patient's capacity to respond to environmental challenges, and to reduce task demand. | |
| Exercise Prescriptions in Older Adults | For older adults, any physical activity is better than being sedentary. Reducing sedentary time has cardiovascular, metabolic, and functional benefits. |
| Resistance training preserves muscle strength and physical functioning in older adults. | |
| Aim for at least 150 minutes of moderate-intensity aerobic activity and two or more days of resistance training per week. | |
| Flexibility exercises improve and maintain joint range of movement in older adults. | |
| Balance exercises (e.g., tai chi, yoga) can improve/maintain physical function, and reduce falls in older adults at risk of falling. | |
| Polypharmacy | |
| Reducing the Risk of Adverse Drug Events in Older Adults | Limit the use of antipsychotics, antidepressants, benzodiazepines, and sedative/hypnotics in older adults to reduce the risk of falls. |
| Limit the number of medications used by older adults; each new medication adds more than one adverse drug event each year, and taking six or more medications increases the risk fourfold. | |
| Ideally, the primary care physician should prescribe all medications, because each additional prescriber increases the risk of adverse drug events in older adults by 30%. | |
| Patients with several chronic health conditions should be asked often about adverse drug events; the odds of an event double for four or five conditions and triple for six or more. | |
| Depression | |
| Depression in Later Life: A Diagnostic and Therapeutic Challenge | Depression in older persons is widespread, often undiagnosed, and usually untreated. |
| Because there is no reliable diagnostic test, a careful clinical evaluation is essential. | |
| Depressive illness in later life should be treated with antidepressants that are appropriate for use in older patients. | |
| A comprehensive, multidisciplinary approach, including consideration of electroconvulsive treatment in some cases, is important. | |
| Weight loss and malnutrition | |
| Unintentional Weight Loss in Older Adults | Unintentional weight loss of more than 5% within six to 12 months is associated with increased morbidity and mortality in older adults and should prompt evaluation. |
| Conduct a baseline evaluation for unexplained, unintentional weight loss in older adults: history, physical examination, laboratory tests, chest radiography, fecal occult blood testing, and possibly abdominal ultrasonography. | |
| If baseline test results are negative, close observation for three to six months is justified. | |
| Appetite stimulants have not been shown to reduce mortality in those with unintentional weight loss. | |
| Hearing loss | |
| Caring for Older Patients Who Have Significant Hearing Loss [Curbside Consultation] | To address communication barriers, face the patient, make eye contact, and talk clearly at a normal pace. |
| Incorporate visual aids. | |
| Ensure hearing amplification is used by the patient, if it is an option. | |
| Hearing Loss in Older Adults | Older patients who report hearing loss can be referred directly for audiometry. |
| Magnetic resonance imaging with gadolinium contrast media is recommended for patients presenting with idiopathic sudden sensorineural hearing loss to identify serious underlying pathologic conditions. | |
| Provide appropriate counseling to patients with hearing loss; patient perceptions and expectations are the most important factors in the acquisition and use of hearing aids. | |
| Referral for assessment for assistive listening devices should be considered in patients with hearing loss who are unable to use hearing aids. | |
| Visual impairment | |
| Vision Loss in Older Adults | Daily AREDS or AREDS2 vitamin supplementation delays vision loss in patients with age-related macular degeneration. |
| Intravitreal injection of a vascular endothelial growth factor inhibitor, such as bevacizumab (Avastin), ranibizumab (Lucentis), or aflibercept (Eylea), can stabilize vision in patients with neovascular age-related macular degeneration or diabetic macular edema. | |
| Fenofibrate (Tricor) may slow the progression of diabetic retinopathy. | |
| Medical testing before cataract surgery does not improve outcomes and is not recommended. | |
| Counsel older adults who smoke to quit; smoking increases the risk of vision loss associated with age-related macular degeneration and cataracts. | |
| Cognitive impairment | |
| Evaluation of Suspected Dementia | Perform formal cognitive testing in patients with abnormal results on initial dementia screening. |
| Perform routine blood work (i.e., complete blood count; complete metabolic panel; and measurement of thyroid-stimulating hormone, vitamin B12, folate, and calcium levels) in patients with suspected dementia. | |
| Consider additional testing (e.g., neuroimaging, cerebrospinal fluid analysis, human immunodeficiency virus testing, Lyme titer, rapid plasma reagin test) in patients with suspected dementia and specific risk factors or symptoms. | |
| Incontinence | |
| Diagnosis of Urinary Incontinence | Consider using a three-day voiding diary in the initial assessment for urinary incontinence symptoms. |
| A positive cough stress test result is the most reliable clinical assessment for confirming stress incontinence. | |
| Perform postvoid residual urine measurement in select high-risk patients (e.g., persons with overflow incontinence). | |
AREDS = Age-Related Eye Disease Study.
*—AFP content published within the past 12 months is accessible to AAFP members and paid subscribers only.
This article updates a previous article on this topic by Elsawy and Higgins.49
Data Sources: A Medline search was completed in OVID. The following grouped concepts were searched as subject headings and/or textwords with truncation: (geriatric assessment or geriatric or elderly or gerontolo$) and (depress$ or cognition disorders or cognitive dysfunction or hearing loss or vision or vision disorders or accidental falls or fall or falling or falls or cancer or neoplasm$) and screen$. The search results included meta-analyses, systematic reviews, and general review articles. Additional sources searched include the Cochrane database, DynaMed, MEDLINE In-Process, and U.S. Preventive Services Task Force website. Search dates: February 7, 2017, and February 27, 2018.
The authors thank Susan Meadows and Susan Elliott for assistance in the literature review and reference formatting, and Diane Herigon for assistance with manuscript review and table preparation.
This material is the result of work supported with resources and the use of facilities at South Texas Veterans Health Care System, San Antonio, Tex., and the George E. Wahlen Department of Veterans Affairs Medical Center, Salt Lake City, Utah.

