Migraines impose significant health and financial burdens. Approximately 38% of patients with episodic migraines would benefit from preventive therapy, but less than 13% take prophylactic medications. Preventive medication therapy reduces migraine frequency, severity, and headache-related distress. Preventive therapy may also improve quality of life and prevent the progression to chronic migraines. Some indications for preventive therapy include four or more headaches a month, eight or more headache days a month, debilitating headaches, and medication-overuse headaches. Identifying and managing environmental, dietary, and behavioral triggers are useful strategies for preventing migraines. First-line medications established as effective based on clinical evidence include divalproex, topiramate, metoprolol, propranolol, and timolol. Medications such as amitriptyline, venlafaxine, atenolol, and nadolol are probably effective but should be second-line therapy. There is limited evidence for nebivolol, bisoprolol, pindolol, carbamazepine, gabapentin, fluoxetine, nicardipine, verapamil, nimodipine, nifedipine, lisinopril, and candesartan. Acebutolol, oxcarbazepine, lamotrigine, and telmisartan are ineffective. Newer agents target calcitonin gene-related peptide pain transmission in the migraine pain pathway and have recently received approval from the U.S. Food and Drug Administration; however, more studies of long-term effectiveness and adverse effects are needed. The complementary treatments petasites, feverfew, magnesium, and riboflavin are probably effective. Nonpharmacologic therapies such as relaxation training, thermal biofeedback combined with relaxation training, electromyographic feedback, and cognitive behavior therapy also have good evidence to support their use in migraine prevention.
The disabling nature of migraine headaches causes frequent visits to outpatient clinic and emergency department settings, imposing significant health and financial burdens. Headaches rank among the top five reasons for emergency department visits and top 20 reasons for outpatient visits.1 The prevalence of migraines is an estimated 16%; they are more common in women, with a peak sex prevalence ratio of 3:1.1 Approximately 38% of persons who have episodic migraines would benefit from prophylactic therapy, but only 3% to 13% obtain it.2
SORT: KEY CLINICAL RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Preventive therapy should be considered in patients having four or more headaches a month or at least eight headache days a month, significantly debilitating attacks despite appropriate acute management, difficulty tolerating or having a contraindication to acute therapy, medication overuse headache, patient preference, or the presence of certain migraine subtypes (i.e., hemiplegic migraine; migraine with brainstem aura; migrainous infarction; or frequent, persistent, or uncomfortable aura symptoms). | C | 8 |
| Divalproex (Depakote), topiramate (Topamax), metoprolol, propranolol, and timolol are effective for migraine prevention and should be offered as first-line treatment. | A | 7–9, 11–18 |
| Petasites has been established as effective and can be considered for migraine prevention. | B | 29, 30 |
| Behavioral treatments, such as relaxation training, thermal biofeedback combined with relaxation training, electromyographic biofeedback, and cognitive behavior therapy, are effective options for migraine prevention. | B | 11, 32 |
| Adding acupuncture to symptomatic treatment decreases the frequency of migraine headaches. | A | 33 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Migraines are distinguished from other headache types by the following attributes: lasting four to 72 hours; unilateral location; pulsating quality; moderate to severe intensity; aggravated by physical activity; and associations with nausea, vomiting, phonophobia, or photophobia. Migraine headaches may be preceded by aura symptoms.3 Episodic and chronic migraines are part of a spectrum of migraine disorders but are distinct clinical entities4 (Table 13,4 ). Chronic migraines are less common (1% to 5% of patients with migraines) and are defined as having headaches at least 15 times a month for at least three months.3 Limited data guide treatment for chronic migraines, which are associated with a poor quality of life.4 Preventive therapy for episodic migraines may decrease headache frequency, severity, and prevent progression to chronic migraines.
TABLE 1. International Classification of Headache Disorders, 3rd Edition

| Classification | Determinants |
|---|---|
| Migraine without aura |
|
| Migraine with aura |
|
| Episodic migraine* | Characterized by those with migraine who have zero to 14 headache days per month4 |
| Chronic migraine |
|
| Medication- overuse headache |
|
*—Episodic migraine is not recognized in the International Classification of Headache Disorders, 3rd ed., but its definition in the literature is recognized as zero to 14 headache days per month.
†—Regular intake of ergotamine, triptan, or opioid medications for a total of at least 10 days per month or nonopioid medications (e.g., acetaminophen, nonsteroidal anti-inflammatory drugs) for at least 15 days per month.
Identifying and Managing Triggers
Migraine triggers are specific to individuals. A headache diary is a helpful tool to aid patients in identifying particular triggers, monitoring the number of headache days, and documenting therapeutic response. Common triggers include delayed or missed meals, menstruation, stress, weather changes, alcohol, and certain odors. Common dietary triggers include chocolate, soft cheeses, red wine, and artificial sweeteners and additives such as monosodium glutamate.5,6 Caffeine can be helpful in relieving headache pain, but acute withdrawal from daily consumption can be a trigger (Table 25,6 ). After triggers are identified, a physician can recommend ways to manage these triggers, such as avoiding certain foods, establishing regular mealtimes, managing stress, and evaluating and treating underlying sleep disorders or psychiatric conditions.
TABLE 2. Common Migraine Triggers

|
Initiating Preventive Therapy
Considerations for starting prophylactic treatment include the following: having four or more headaches a month or at least eight headache days a month, debilitating attacks despite appropriate acute management, difficulty tolerating or having a contraindication to acute therapy, medication-overuse headache (Table 13,4 ), patient preference, or the presence of certain migraine subtypes (i.e., hemiplegic migraine; migraine with brainstem aura; migrainous infarction; or frequent, persistent, or uncomfortable aura symptoms) (Figure 17 ).8
FIGURE 1.

Algorithm for initiating pharmacologic migraine prophylaxis.
Adapted with permission from Modi S, Lowder DM. Medications for migraine prophylaxis [published correction appears in Am Fam Physician. 2006;74(10):1685]. Am Fam Physician. 2006;73(1):73.
Once the need for prophylactic treatment is established, adhering to the following consensus-based principles of care may improve the success of preventive therapy.8
- Start therapy with medications that have the highest level of evidence-based effectiveness (Table 39 and eTable A).
- Consider comorbid conditions when selecting a medication; choose medications that also treat these conditions. Avoid agents that are contraindicated or that may exacerbate coexisting conditions (Table 48,10 and Table 58 ).
- Start with the lowest effective dose and titrate every two to four weeks until therapeutic effect or until patient develops adverse effects (Table 48,10 and Table 58 ).
- Set realistic goals. Successful treatment is defined as a 50% reduction in the number of headache attacks or days, a significant decrease in the duration of attacks, or an improvement in response to acute therapy.
- Allow an adequate trial for each treatment. The patient may see improvement in six to eight weeks, but it may take up to six months for full effect.5
- Reevaluate therapy. Patient may have partial response and require dose titration. Consider changing therapy if no response occurs after two months.
- Discontinue therapy. If headaches are controlled for at least six to 12 months, consider slowly tapering and discontinuing therapy.
TABLE 3. Recommended Medications for Episodic Migraine Prevention

| First-line agents (established efficacy based on evidence) | Second-line agents (probably effective based on evidence) |
|---|---|
| Divalproex (Depakote) | Amitriptyline |
| Frovatriptan (Frova)* | Atenolol |
| Metoprolol | Nadolol (Corgard) |
| Propranolol | Naratriptan (Amerge)* |
| Timolol | Venlafaxine |
| Topiramate (Topamax) | Zolmitriptan (Zomig)* |
*—For menstrual-associated migraines.
Information from reference 9.
eTABLE A Other Medications (Less Evidence Based) for Episodic Migraine Prevention

| Possibly effective |
| Candesartan (Atacand) |
| Carbamazepine (Tegretol) |
| Lisinopril |
| Nebivolol (Bystolic) |
| Nicardipine (Cardene) |
| Conflicting or inadequate data to support or refute use |
| Bisoprolol (Zebeta) |
| Fluoxetine (Prozac) |
| Gabapentin (Neurontin) |
| Nifedipine |
| Nimodipine (Nimotop) |
| Pindolol |
| Protriptyline |
| Verapamil |
| Ineffective |
| Acebutolol (Sectral) |
| Lamotrigine (Lamictal) |
| Oxcarbazepine (Trileptal) |
| Telmisartan (Micardis) |
Information from Silberstein SD, Holland S, Freitag F, Dodick DW, Argoff C, Ashman E. Evidence-based guideline update: pharmacologic treatment for episodic migraine prevention in adults: Report on the Quality Standards Subcommittee of the American Academy of Neurology and the American Headache Society [published correction appears in Neurology. 2013;80(9)871]. Neurology. 2012;78(17):1337–1345.
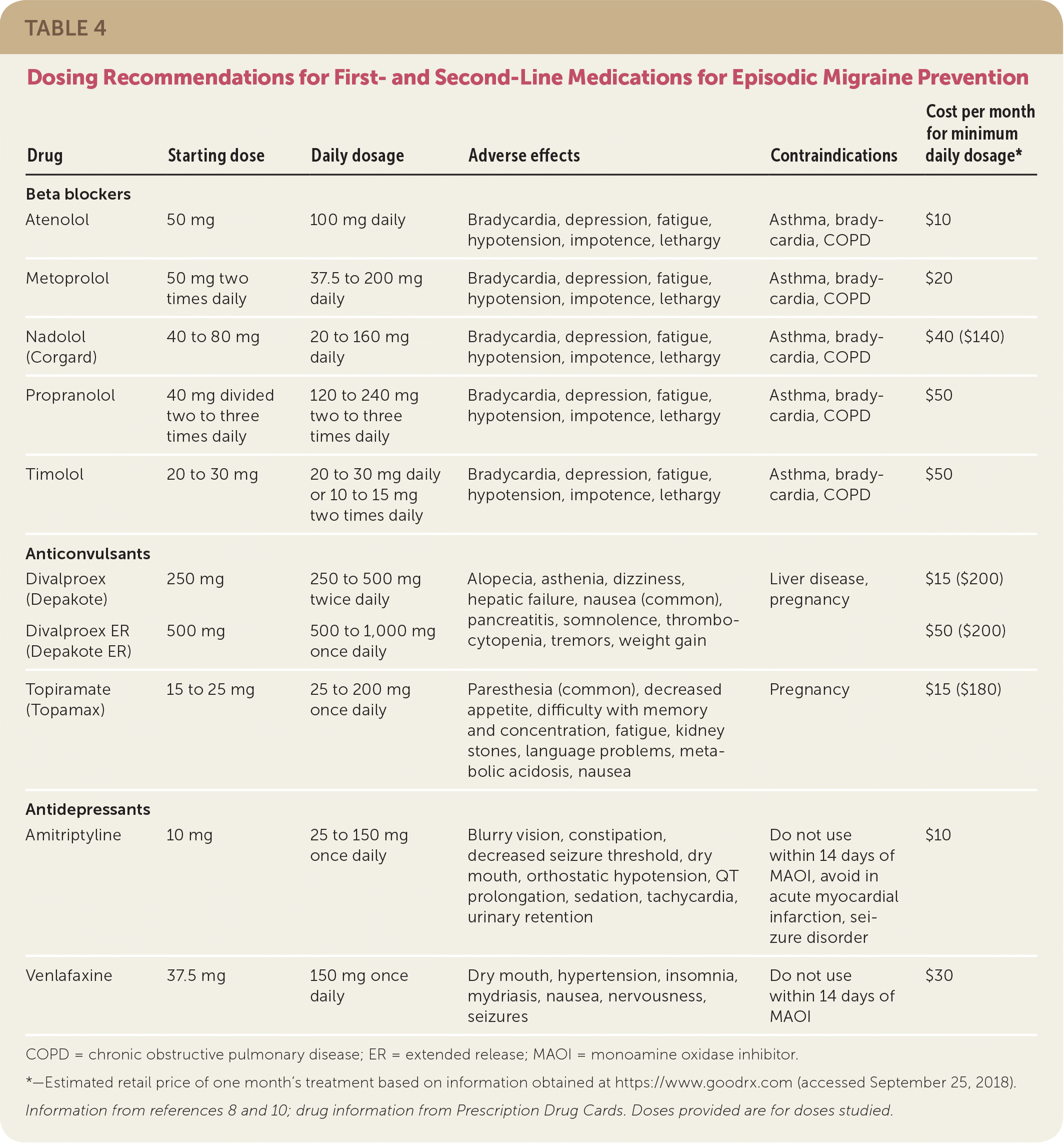
TABLE 4. Dosing Recommendations for First- and Second-Line Medications for Episodic Migraine Prevention
| Drug | Starting dose | Daily dosage | Adverse effects | Contraindications | Cost per month for minimum daily dosage* |
|---|---|---|---|---|---|
| Beta blockers | |||||
| Atenolol | 50 mg | 100 mg daily | Bradycardia, depression, fatigue, hypotension, impotence, lethargy | Asthma, brady-cardia, COPD | $10 |
| Metoprolol | 50 mg two times daily | 37.5 to 200 mg daily | Bradycardia, depression, fatigue, hypotension, impotence, lethargy | Asthma, brady-cardia, COPD | $20 |
| Nadolol (Corgard) | 40 to 80 mg | 20 to 160 mg daily | Bradycardia, depression, fatigue, hypotension, impotence, lethargy | Asthma, brady-cardia, COPD | $40 ($140) |
| Propranolol | 40 mg divided two to three times daily | 120 to 240 mg two to three times daily | Bradycardia, depression, fatigue, hypotension, impotence, lethargy | Asthma, brady-cardia, COPD | $50 |
| Timolol | 20 to 30 mg | 20 to 30 mg daily or 10 to 15 mg two times daily | Bradycardia, depression, fatigue, hypotension, impotence, lethargy | Asthma, brady-cardia, COPD | $50 |
| Anticonvulsants | |||||
| Divalproex (Depakote) | 250 mg | 250 to 500 mg twice daily | Alopecia, asthenia, dizziness, hepatic failure, nausea (common), pancreatitis, somnolence, thrombocytopenia, tremors, weight gain | Liver disease, pregnancy | $15 ($200) |
| Divalproex ER (Depakote ER) | 500 mg | 500 to 1,000 mg once daily | $50 ($200) | ||
| Topiramate (Topamax) | 15 to 25 mg | 25 to 200 mg once daily | Paresthesia (common), decreased appetite, difficulty with memory and concentration, fatigue, kidney stones, language problems, metabolic acidosis, nausea | Pregnancy | $15 ($180) |
| Antidepressants | |||||
| Amitriptyline | 10 mg | 25 to 150 mg once daily | Blurry vision, constipation, decreased seizure threshold, dry mouth, orthostatic hypotension, QT prolongation, sedation, tachycardia, urinary retention | Do not use within 14 days of MAOI, avoid in acute myocardial infarction, seizure disorder | $10 |
| Venlafaxine | 37.5 mg | 150 mg once daily | Dry mouth, hypertension, insomnia, mydriasis, nausea, nervousness, seizures | Do not use within 14 days of MAOI | $30 |
COPD = chronic obstructive pulmonary disease; ER = extended release; MAOI = monoamine oxidase inhibitor.
*—Estimated retail price of one month's treatment based on information obtained at https://www.goodrx.com (accessed September 25, 2018).
Information from references 8 and 10; drug information from Prescription Drug Cards. Doses provided are for doses studied.
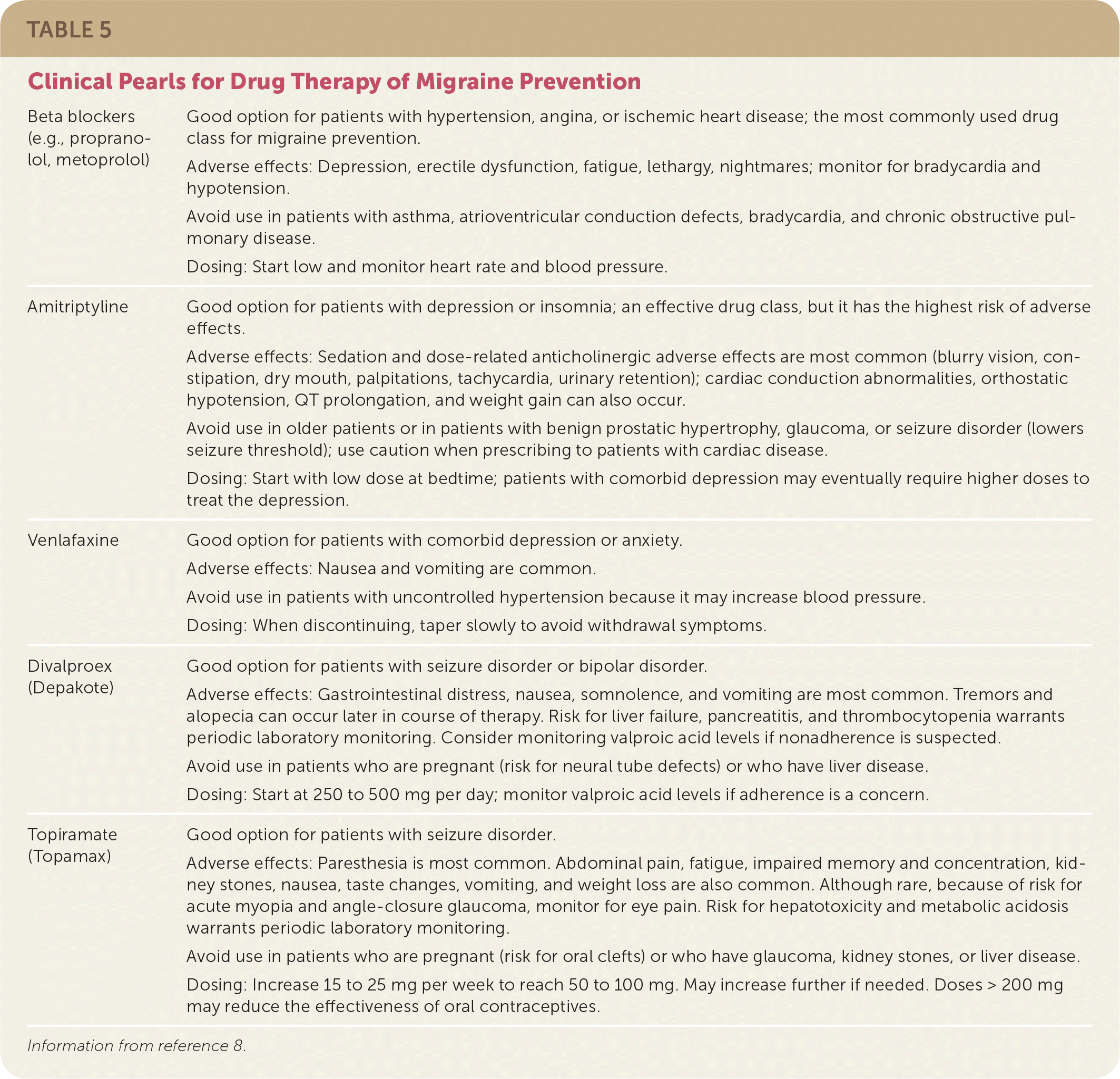
TABLE 5. Clinical Pearls for Drug Therapy of Migraine Prevention
| Beta blockers (e.g., propranolol, metoprolol) | Good option for patients with hypertension, angina, or ischemic heart disease; the most commonly used drug class for migraine prevention. Adverse effects: Depression, erectile dysfunction, fatigue, lethargy, nightmares; monitor for bradycardia and hypotension. Avoid use in patients with asthma, atrioventricular conduction defects, bradycardia, and chronic obstructive pulmonary disease. Dosing: Start low and monitor heart rate and blood pressure. |
| Amitriptyline | Good option for patients with depression or insomnia; an effective drug class, but it has the highest risk of adverse effects. Adverse effects: Sedation and dose-related anticholinergic adverse effects are most common (blurry vision, constipation, dry mouth, palpitations, tachycardia, urinary retention); cardiac conduction abnormalities, orthostatic hypotension, QT prolongation, and weight gain can also occur. Avoid use in older patients or in patients with benign prostatic hypertrophy, glaucoma, or seizure disorder (lowers seizure threshold); use caution when prescribing to patients with cardiac disease. Dosing: Start with low dose at bedtime; patients with comorbid depression may eventually require higher doses to treat the depression. |
| Venlafaxine | Good option for patients with comorbid depression or anxiety. Adverse effects: Nausea and vomiting are common. Avoid use in patients with uncontrolled hypertension because it may increase blood pressure. Dosing: When discontinuing, taper slowly to avoid withdrawal symptoms. |
| Divalproex (Depakote) | Good option for patients with seizure disorder or bipolar disorder. Adverse effects: Gastrointestinal distress, nausea, somnolence, and vomiting are most common. Tremors and alopecia can occur later in course of therapy. Risk for liver failure, pancreatitis, and thrombocytopenia warrants periodic laboratory monitoring. Consider monitoring valproic acid levels if nonadherence is suspected. Avoid use in patients who are pregnant (risk for neural tube defects) or who have liver disease. Dosing: Start at 250 to 500 mg per day; monitor valproic acid levels if adherence is a concern. |
| Topiramate (Topamax) | Good option for patients with seizure disorder. Adverse effects: Paresthesia is most common. Abdominal pain, fatigue, impaired memory and concentration, kidney stones, nausea, taste changes, vomiting, and weight loss are also common. Although rare, because of risk for acute myopia and angle-closure glaucoma, monitor for eye pain. Risk for hepatotoxicity and metabolic acidosis warrants periodic laboratory monitoring. Avoid use in patients who are pregnant (risk for oral clefts) or who have glaucoma, kidney stones, or liver disease. Dosing: Increase 15 to 25 mg per week to reach 50 to 100 mg. May increase further if needed. Doses > 200 mg may reduce the effectiveness of oral contraceptives. |
Information from reference 8.
Preventive Medication
Several medications have been studied for the prevention of episodic migraines. Based on guidelines from the American Headache Society and the American Academy of Neurology, agents with the most quality evidence to support their use should generally be considered first for migraine prevention9,11 (Table 39 ).
BETA BLOCKERS
Close to 60 trials confirm the effectiveness of propranolol.7,9 Based on nine randomized placebo-controlled trials, the overall relative risk of response to propranolol was 1.94 (95% confidence interval [CI], 1.61 to 2.35).12 Metoprolol is also effective. In four studies evaluating the use of metoprolol compared with placebo, the pooled mean difference in headaches per month was –0.94 (95% CI, –1.4 to –0.46).13 Timolol has demonstrated effectiveness compared with placebo in three studies.7,9,11 Atenolol and nadolol (Corgard) have adequate evidence to support their effectiveness.9
Less Evidence-Based Options. Nebivolol (Bystolic) has one randomized controlled trial to support its use and is considered possibly effective. This study found that nebivolol and metoprolol were equally effective in reducing migraine attacks in the final four weeks of a 14-week trial.14 There are not enough studies to determine the effectiveness of bisoprolol (Zebeta) and pindolol. Acebutolol (Sectral) is not considered effective for migraine prevention.9
ANTICONVULSANTS AND ANTIEPILEPTICS
Ten clinical studies have consistently demonstrated that valproic acid in the form of valproate (not available in the United States) or divalproex (Depakote) is effective. In four trials evaluating divalproex and placebo, the risk ratio for responders was 2.18 (95% CI, 1.78 to 3.72).15 A more recent study evaluated the use of extended-release divalproex compared with placebo in 239 patients. The divalproex group had a statistically greater mean reduction in four-week migraine headache rates from baseline when compared with placebo, 1.2 vs. 0.6 fewer headaches, respectively.16
Topiramate (Topamax) is an antiepileptic supported by substantial data. Based on a Cochrane review including 17 trials, topiramate reduces the frequency of headaches and is two times more likely to reduce headache frequency by 50% or more when compared with placebo.17 In head-to-head clinical studies, topiramate was as effective as amitriptyline and propranolol.17,18 In one study, there was no significant difference in the reduction of mean monthly migraine episodes from baseline between topiramate and amitriptyline.18 Based on pooled data from two trials comparing topiramate and propranolol, no significant difference in headache frequency occurred.17
Less Evidence-Based Options. Carbamazepine (Tegretol) is an antiepileptic that has been studied for use in migraine prevention and is considered possibly effective. Gabapentin (Neurontin) has been compared with placebo in six randomized controlled trials with mixed results. Four studies found no differences in headache frequency or percent responders, whereas two found small, but statistically significant, differences in headache frequency or percent responders.19 Because of these mixed results, guidelines do not support or discourage the use of gabapentin. Based on available studies, oxcarbazepine (Trileptal) is categorized as possibly ineffective, and lamotrigine (Lamictal) is considered ineffective.9
ANTIDEPRESSANTS
Tricyclic antidepressants, including amitriptyline, doxepin, nortriptyline (Pamelor), and protriptyline, are used in migraine prevention, but only amitriptyline has substantial data from about 12 randomized trials that support its effectiveness.20 However, because of a high incidence of adverse effects, it is classified as only probably effective.8,9 Venlafaxine is considered probably effective based on two studies. One study was a randomized double-blind crossover study comparing venlafa xine and amitriptyline. Venlafa xine produced a significant decrease in the number of migraine attacks per month as well as a decrease in the duration and severity of attacks. There was no significant difference in effectiveness between venlafaxine and amitriptyline.21
Less Evidence-Based Options. Studies of fluoxetine (Prozac) have demonstrated inconsistent results. Two placebo-controlled studies showed a significant reduction in headache and pain scores.9,22 However, in another study, fluoxetine was not effective in reducing headache frequency or pain scores.23 Because of the conflicting data, its use is not supported or discouraged by guidelines.9
CALCIUM CHANNEL BLOCKERS
The quality of evidence for calcium channel blockers in migraine prevention is weak. Nicardipine (Cardene) is classified as possibly effective. In past guidelines, verapamil and nimodipine (Nimotop) were originally considered effective for migraine prophylaxis. However, on reevaluation of previous studies, supporting data for verapamil and nimodipine are now considered insufficient. Likewise, data regarding nifedipine are inadequate or conflicting.9
ANGIOTENSIN-CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS
Three studies have been conducted with angiotensin-converting enzyme inhibitors and angiotensin receptor blockers for migraine prevention. One study demonstrated that patients taking lisinopril reported fewer days with migraines compared with those taking a placebo (14.5 days vs. 18.5 days [95% CI, 9 to 34 days]).24 Studies for angiotensin receptor blockers have been conflicting. Candesartan (Atacand) was associated with reduced migraine days and hours as secondary end points in one study, whereas telmisartan (Micardis) failed to show a significant reduction in migraine days compared with placebo in another study.25,26 Lisinopril and candesartan are possibly effective, and telmisartan is possibly ineffective for migraine prevention.9
ONABOTULINUMTOXINA
OnabotulinumtoxinA (Botox) is ineffective and should not be offered for preventing episodic migraine. However, there is evidence supporting the use of onabotulinumtoxinA in the prevention of chronic migraines.27
CALCITONIN GENE-RELATED PEPTIDE THERAPY
Erenumab (Aimovig) was approved by the U.S. Food and Drug Administration in May 2018 for migraine prevention. Erenumab was the first approved monoclonal antibody; it binds to the calcitonin gene-related peptide receptor, which mediates migraine pain transmission. In a six-month study, subcutaneous erenumab, 70 mg and 140 mg given monthly, reduced the baseline mean migraine days per month of 8.3 by 3.2 and 3.7 days, respectively, compared with 1.8 days in the placebo group (P < .001). Injection site pain and constipation were more common in the groups taking erenumab, but no statistically significant differences in adverse effects vs. placebo occurred. More studies are needed to determine its long-term effectiveness and adverse effects.28 Two additional monoclonal antibodies against calcitonin gene-related peptide (fremanezumab-vfrm [Ajovy] and galcanezumab-glnm [Emgality]) are approved for migraine prevention.
Complementary Therapy
Petasites, an extract of the butterbur plant, is effective for the prophylactic treatment of migraines in dosages of 50 to 75 mg twice a day.29 The most common adverse effects are gastrointestinal upset and belching; less often, hepatotoxicity may occur. Although the American Academy of Neurology retired their 2012 guidelines on complementary therapy secondary to serious safety concerns regarding butterbur,30 the Canadian Headache Society still strongly recommends its use. The Canadian Headache Society cautions that only commercially prepared products that have passed federal health inspection should be used.29 Other treatments that are probably effective are riboflavin (400 mg daily) and feverfew (Tanacetum parthenium). Coenzyme Q10, 100 mg three times a day, and magnesium dicitrate, 600 mg daily, are possibly effective.29,31
Nonpharmacologic Therapy
A U.S. Headache Consortium meta-analysis concluded that relaxation training, thermal biofeedback combined with relaxation training, electromyographic biofeedback, and cognitive behavior therapy may be considered as treatment options for the prevention of migraine. Additionally, behavioral therapy (i.e., relaxation, biofeedback) may be combined with preventive drug therapy (i.e., propranolol, amitriptyline) for patients to achieve additional clinical improvement for migraine relief.11,32 A 2016 Cochrane review suggests that adding acupuncture to symptomatic treatment decreases the frequency of headaches and was at least as effective as prophylactic medication.33
Special Considerations
MENSTRUAL-ASSOCIATED MIGRAINE
For menstrual migraines, starting preventive therapy before the time of expected migraine onset can help prevent disability and reduce severity.34 Frovatriptan (Frova), naratriptan (Amerge), and zolmitriptan (Zomig) all demonstrated effectiveness. Frovatriptan has the strongest evidence and is supported by two clinical studies. In one study, frovatriptan groups had a lower incidence of menstrual headaches during a six-day period vs. placebo (52% with frovatriptan, 2.5 mg daily, vs. 41% with frovatriptan, 2.5 mg two times a day, vs. 67% with placebo; P < .0001). Naratriptan and zolmitriptan have been found beneficial in one study.9,34
CHILDREN
Only flunarizine has sufficient evidence to be considered probably effective for migraine prevention in children, but it is not available in the United States. Agents commonly prescribed for children, such as propranolol and topiramate, have conflicting results in studies. Other agents, including cyproheptadine, amitriptyline, valproic acid (Depakene), and levetiracetam (Keppra), have insufficient data in children. More quality randomized controlled trials are needed in this population.35
PREGNANCY
Guidelines on preventing migraines in pregnancy suggest considering nonpharmacologic options before drug therapy. If drug therapy is needed, an agent with the lowest risk of harm to the fetus can be considered at the lowest effective dose.11 Although there have been reports of intrauterine growth retardation, beta blockers such as propranolol are generally considered safe in pregnancy.36,37 Valproic acid should be avoided in pregnancy because of teratogenic risk. Topiramate and angiotensin-converting enzyme inhibitors should be avoided because of potential fetal harm.
This article updates a previous article on this topic by Modi and Lowder.7
Data Sources: The National Guideline Clearinghouse was used and searched for the key words migraine prevention, migraine prophylaxis, and botulinum and migraines. The search included all relevant guidelines. A PubMed search was completed in Clinical Queries using the key words migraine prevention and migraine prophylaxis. A PubMed search was also completed using the key words author name/publication year for relevant trials noted in various guidelines. The aforementioned searches included randomized controlled trials, clinical trials, guidelines, and reviews. There were also searches using Essential Evidence Plus, the Agency for Healthcare Research and Quality evidence reports, Cochrane database, National Center for Complementary and Integrative Health, and UpToDate. Search dates: July 29, 2017; August 8–9, 2017; September 13–16, 2017; October 20–26, 2017; and October 10, 2018.

