
Am Fam Physician. 2019;100(4):211-212
Author disclosure: No relevant financial affiliations.
We estimate that 217,208 primary care physicians provided direct patient care in the United States in 2018. This represents an even lower percentage (30%) of the total U.S. physician cohort than the 2010 Council on Graduate Medical Education's (COGME's) recommendation to increase primary care to 40% of the overall physician workforce.
In 2010, the congressional advisory group COGME declared in its 20th report that “policies supporting physicians providing primary care should be implemented that raise the percentage of primary care physicians (general internists, general pediatricians, and family physicians) among all physicians to at least 40 percent from the current level of 32 percent, a percentage that is actively declining at the present time.”1 We used data from the 2018 American Medical Association Masterfile and the same methods of calculation as COGME to assess progress toward the recommendation, using an established method to account for hospitalists—physicians with primary care specialty training working primarily in hospitals (more than 90% of claims;2 Table 1 and Table 2). We adjusted for retired physicians using methods developed by Petterson, et al., 2016.3
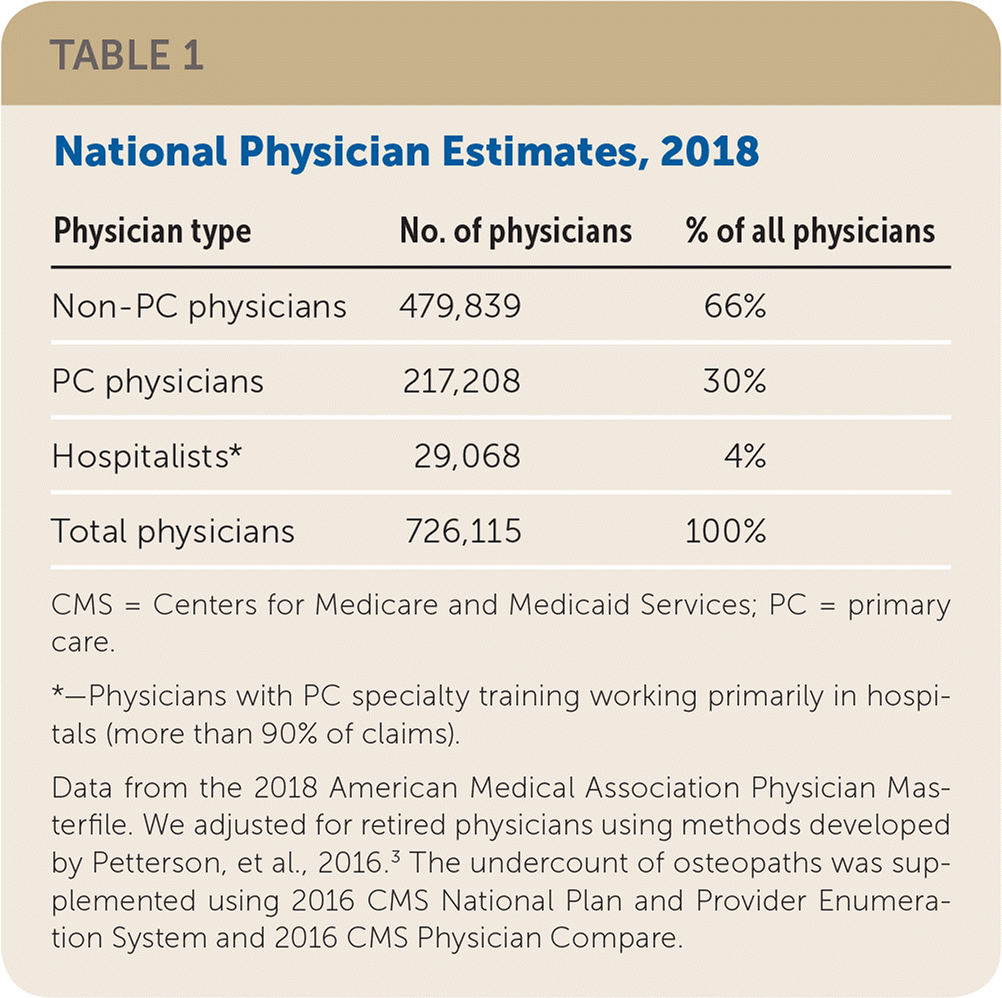
| Physician type | No. of physicians | % of all physicians |
|---|---|---|
| Non-PC physicians | 479,839 | 66% |
| PC physicians | 217,208 | 30% |
| Hospitalists* | 29,068 | 4% |
| Total physicians | 726,115 | 100% |
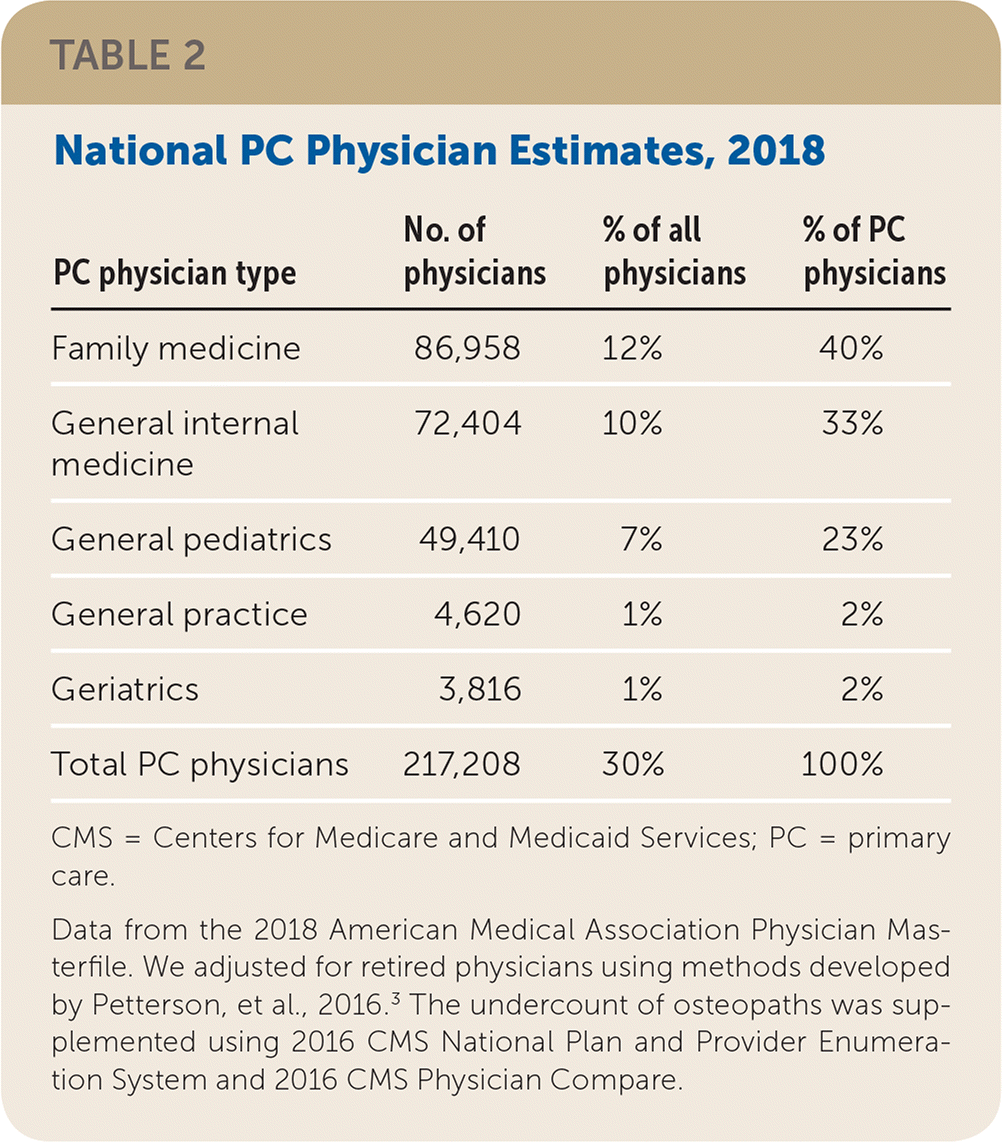
| PC physician type | No. of physicians | % of all physicians | % of PC physicians |
|---|---|---|---|
| Family medicine | 86,958 | 12% | 40% |
| General internal medicine | 72,404 | 10% | 33% |
| General pediatrics | 49,410 | 7% | 23% |
| General practice | 4,620 | 1% | 2% |
| Geriatrics | 3,816 | 1% | 2% |
| Total PC physicians | 217,208 | 30% | 100% |
Family physicians are the largest contributor to the primary care physician workforce, making up 40% of all primary care physicians, followed by general internists and general pediatricians. With 40% of U.S. family physicians being older than 55 years,4 and substantial proportions of primary care residents choosing to subspecialize or become hospitalists, primary care access is likely to worsen. The shrinking proportion of primary care physicians does not reflect the growing demands of an aging U.S. population. Primary care physicians are more likely to provide care in rural areas and safety net settings relative to other subspecialties.5
Among noteworthy advocacy responses to these trends, major U.S. family medicine organizations have collectively declared a “25 by 30” goal, hoping to see 25% of all U.S. medical school graduates selecting the primary care discipline by 2030.6 Still, the need for policy attention to these developments is even greater and more acute today than in 2010. Evidence-based reforms are needed to enhance educational exposures, graduate medical education financing, and downstream payment for learners interested in primary care, while also reducing burnout.
