Genital ulcers may be located on the vagina, penis, and anorectal or perineal areas and may be infectious or noninfectious. Herpes simplex virus is the most common cause of genital ulcers in the United States. A diagnosis of genital herpes simplex virus infection is made through physical examination and observation of genital lesions. The 2015 Centers for Disease Control and Prevention sexually transmitted disease guidelines provide strategies for the management of patients with genital ulcer disease. Specific testing includes a polymerase chain reaction test for herpes simplex virus; syphilis serology and darkfield microscopy or a direct fluorescent antibody test for Treponema pallidum; and/or culture for Haemophilus ducreyi in settings where chancroid is highly prevalent. Rarely, cases of Epstein-Barr virus may present with genital ulcers. Syphilis and chancroid cause genital ulcers and are mandatory reportable diseases to the local health department. In some cases, no pathogen is identified. It is important to consider noninfectious etiologies such as sexual trauma, psoriasis, Behçet syndrome, and fixed drug eruptions. Genital ulcers are symptomatic by definition, and the U.S. Preventive Services Task Force recommends screening for syphilis infection for those at risk, early screening for syphilis infection in all pregnant women, and against routine serologic screening for genital herpes simplex virus infection in asymptomatic adolescents and adults, including those who are pregnant.
Genital ulcers may be located on the vagina, penis, and anorectal or perineal areas and may be infectious (sexually transmitted infections [STIs], secondary bacterial, or fungal) or noninfectious (Table 1).1–3 The most common causes of STIs characterized by genital ulcers in the United States are genital herpes simplex virus types 1 and 2 (HSV-1, HSV-2).1 Less common infectious causes include syphilis (Treponema pallidum) and rarely chancroid (Haemophilus ducreyi), granuloma inguinale (donovanosis [Klebsiella granulomatis], formerly known as Calymmatobacterium granulomatis), and lymphogranuloma venereum (Chlamydia trachomatis serovars L1, L2, and L3).1 Genital ulcer disease commonly refers to ulcerations associated with STIs, but the ulcerations have also been reported as rare sequelae of mononucleosis (Epstein-Barr virus)4 and can be caused by noninfectious etiologies such as psoriasis, sexual trauma, Behçet syndrome, or fixed drug eruptions.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
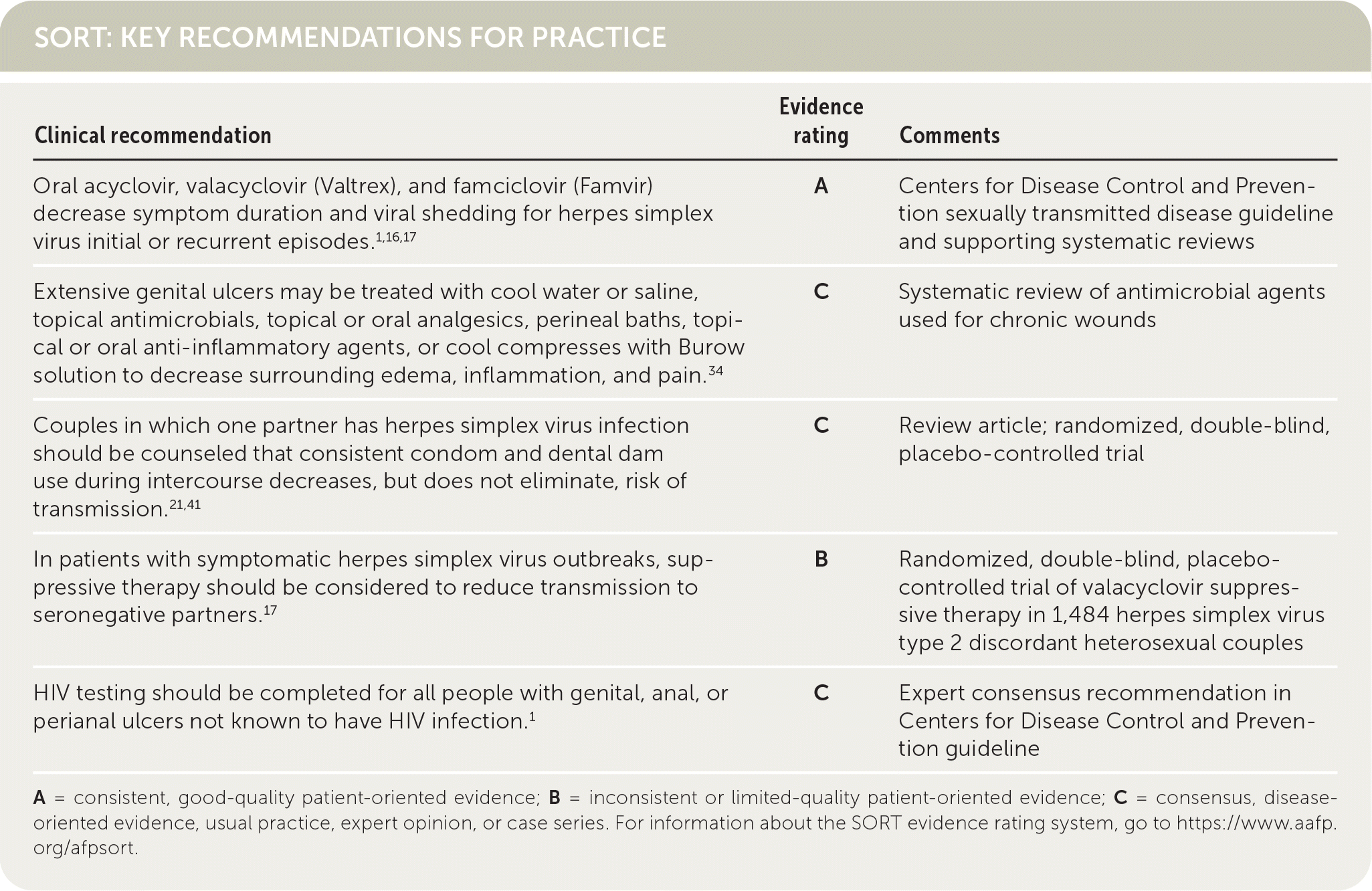
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN INFECTIOUS DISEASE

| Recommendation | Sponsoring organization |
|---|---|
| Do not screen for genital herpes simplex virus infection in asymptomatic adults, including pregnant women. | American Academy of Family Physicians |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
TABLE 1. Differential Diagnosis of Genital Ulcers

| Infectious (most common)* | |
| Genital herpes simplex virus | |
| Syphilis | |
| Chancroid | |
| Lymphogranuloma venereum | |
| Granuloma inguinale (donovanosis) | |
| Fungal infection (e.g., Candida) | |
| Secondary bacterial infection | |
| Noninfectious (less common) | |
| Behçet syndrome | |
| Fixed drug eruption | |
| Psoriasis | |
| Sexual trauma | |
| Wegener granulomatosis |
*—Listed in order of frequency.
Epidemiology
According to the Centers for Disease Control and Prevention (CDC) National Center for Health Statistics 2015–2016 National Health and Nutrition Examination Survey interviews followed by standardized physical examinations, including serologic HSV-1 and -2 evaluations, 11.9% of U.S. people 14 to 49 years of age have genital HSV-2 infection, whereas 47.8% have HSV-1.2 HSV-1 and -2 occur more commonly in women (50.9%) than men (45.2%).2,3 Transmission from male to female partners is more likely than from female to male.3 The age-adjusted prevalence of HSV-1 is highest among Mexican Americans (71.7%), whereas HSV-2 prevalence is highest among non-Hispanic blacks (34.6%).2–4
In 2017, most cases of primary and secondary syphilis (57.9%) occurred among men who have sex with men, but the overall rate is increasing for all groups—men who have sex with men, heterosexual men, and women.3 Syphilis is more common in urban areas and among adults 20 to 35 years of age. Syphilis in an untreated pregnant woman, even if infected up to four years before delivery, can result in an 80% rate of fetal infection and could lead to up to 40% stillbirths or miscarriage. Secondary, tertiary, or congenital syphilis cases are less common in the United States. Syphilis and chancroid are typically mandatory reportable diseases to local health departments.1 Chancroid usually occurs in discrete outbreaks but may be endemic in some regions. The incidence of chancroid has been declining in the United States, with only seven cases reported in 2017.3 Approximately 10% of people with chancroid acquired in the United States are coinfected with syphilis or HSV-1 or -2, with an even greater proportion of coinfection if chancroid is acquired outside the United States.5
Based on reported cases, lymphogranuloma venereum primarily occurs in men who have sex with men,6 but the prevalence is unknown, likely because widely available testing does not distinguish between lymphogranuloma venereum and nonlymphogranuloma venereum–related C. trachomatis.7 Behçet syndrome is most common in the Middle East, Asia, and Japan—affecting more men than women in Middle Eastern and Asian countries—but it is more common among women in the rare occurrences reported in the United States.8
The probability of HIV transmission increases in the presence of genital ulcer disease.9,10 Maternal HSV-2 coinfection is associated with increased mother-to-child perinatal HIV transmission.11
Diagnostic Evaluation
The diagnosis of genital ulcer disease can be made with one or more mucocutaneous ulcers involving the genitalia, perineum, or anus.4 Diagnosing the specific cause of genital ulcer disease is based on history, physical examination, and, in some cases, laboratory findings.
HISTORY AND PHYSICAL EXAMINATION
Risk factors for sexually transmitted genital ulcers are similar to those for other STIs transmitted through infected lesions, mucosal surfaces, or genital or oral secretions, including unprotected sexual contact, multiple sex partners, alcohol or illicit drug use, men who have sex with men, and lack of male circumcision. According to the U.S. Preventive Services Task Force (USPSTF), populations at increased risk for STIs also include sexually active adolescents; adults with current STIs or those who have had an STI in the past year; people living in low-income urban settings; current or former inmates; military recruits; sex workers or people who exchange sex for drugs; people with a history of mental illness, disability, or sexual abuse; current or former injection drug users; and patients treated at public STI clinics.12 Poverty, homelessness, and unstable housing may be particularly important risk factors for women.12,13
Based on the prevalence of primary and secondary syphilis, physicians should routinely ask men who have sex with men about common STI symptoms (e.g., urethral discharge, dysuria, genital and perianal ulcers, regional lymphadenopathy, proctitis) and proceed with diagnostic testing when indicated.1 Risk factors for noninfectious causes of genital ulcers include a history of inflammatory disease (e.g., psoriasis) and exposure to sexual trauma or medications with ulcerative adverse effects or drug eruptions such as nonsteroidal anti-inflammatory drugs, antimalarials, angiotensin-converting enzyme inhibitors, beta blockers, lithium, salicylates, or corticosteroids. Initiation of antiretroviral therapy in patients coinfected with HIV/HSV-2 is associated with a transient increased risk of genital ulcer outbreaks.14
Genital HSV infection is most reliably diagnosed through observation of characteristic genital lesions (Figure 1,15 Table 21,16,17 ) and, when considered necessary, confirmatory testing for HSV DNA. Internal lesions may be difficult to observe, and absent observable lesions and despite HSV DNA testing, no pathogen may be identified.18 HSV lesions are commonly painful, are preceded by prodromal symptoms (tingling before vesicular eruptions), and may be found inside the foreskin, labia, vagina, or rectum. The chancre lesion of primary syphilis (Figure 2) is a single, painless, indurated ulcer with a clean base and is caused by active infection with T. pallidum.
FIGURE 1
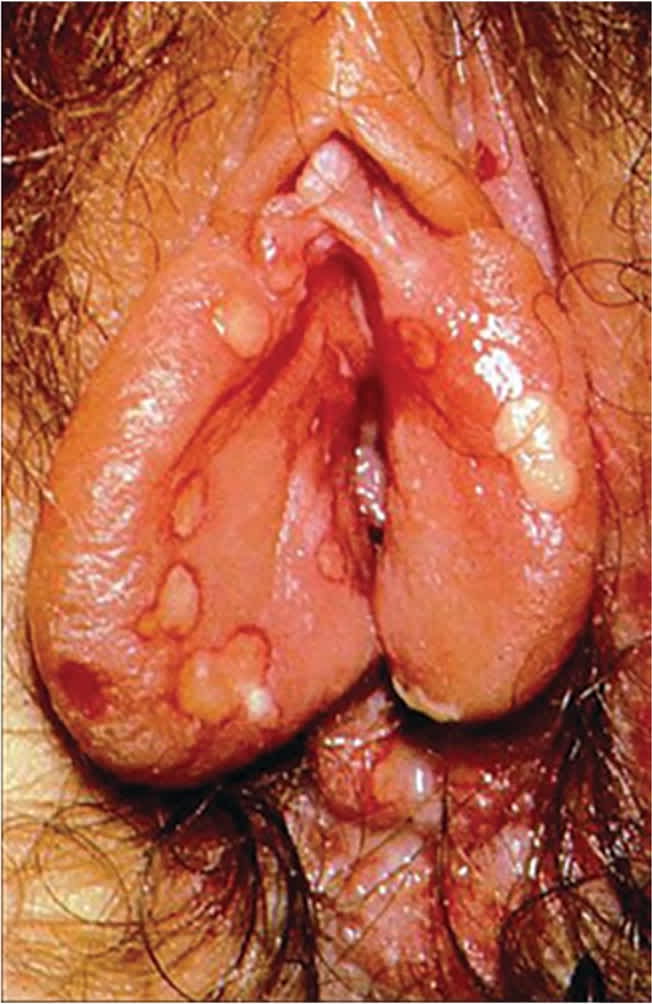
Genital herpes simplex virus. Painful, shallow ulcers may manifest from ruptured vesicular lesions.
Reprinted with permission from Kohn M. Herpes simplex in emergency medicine. Updated July 16, 2019. Accessed September 13, 2011. http://emedicine.medscape.com/article/783113-overview
TABLE 2. Summary of the Diagnosis and Treatment for Herpes Simplex Virus and Syphilis

| Significant history and physical examination findings | Laboratory findings | Treatments |
|---|---|---|
| Herpes simplex virus | ||
| Initial lesions are usually multiple vesicles; lesions may spontaneously rupture before clinical presentation, leaving a shallow, painful ulcer First-time infections may cause constitutional symptoms and lymphadenopathy | Definitive: Detection of herpes simplex virus DNA by nonculture methods (polymerase chain reaction) from ulcer scraping or aspiration of vesicle fluid Presumptive: Typical lesions plus any of the following: Previously known outbreak Exclusion of other causes of ulcers | First episode (may extend treatment if not healed after 10 days): Acyclovir, 400 mg 3 times daily for 7 to 10 days, or Acyclovir, 200 mg 5 times daily for 7 to 10 days, or Valacyclovir (Valtrex), 1 g twice daily for 7 to 10 days, or Famciclovir (Famvir), 250 mg 3 times daily for 7 to 10 days Recurrent episode: Acyclovir, 400 mg 3 times daily for 5 days, or Acyclovir, 800 mg twice daily for 5 days, or Acyclovir, 800 mg 3 times daily for 2 days, or Acyclovir, 200 mg 5 times daily for 5 days, or Valacyclovir, 500 mg twice daily for 3 days, or Valacyclovir, 1 g daily for 5 days, or Famciclovir, 125 mg twice daily for 5 days, or Famciclovir, 1 g twice daily for 1 day, or Famciclovir, 500 mg once, then 250 mg twice daily for 2 days Suppressive therapy: Acyclovir, 400 mg twice daily, or Acyclovir, 200 mg 3 to 5 times daily, or Valacyclovir, 500 mg daily, or Valacyclovir, 1 g daily, or Famciclovir, 250 mg twice daily Severe acute disease: Admit the patient, begin intravenous acyclovir, 5 to 10 mg per kg every 8 hours for 10 days; intravenous therapy for 2 to 7 days until improvement, then switch to oral therapy to complete 10 days of treatment |
| Syphilis | ||
| A single, painless, well-demarcated ulcer with a clean base and indurated borders (chancre) Mild or minimally tender inguinal lymphadenopathy Secondary syphilis is typically a nonulcerative phase (patients presenting with condyloma lata lesions) Tertiary syphilis is typically a nonulcerative phase (aortitis, gumma, and iritis) Early latent syphilis is typically a nonulcerative phase (the presence of infection less than 1 year, but time unknown) Late latent syphilis (the likely duration of infection is more than 1 year) includes other stages of syphilis but does not present during the ulcerative phase of the disease to allow for diagnosis | Identification of Treponema pallidum from a chancre or lymph node aspirate on darkfield microscopy or by direct fluorescent antibody | Primary, secondary, or latent < 1 year: Intramuscular penicillin G benzathine (600,000 units per mL), 2.4 million units in a single dose; may repeat dose after 1 week if pregnant Latent > 1 year or unknown duration or tertiary syphilis with normal cerebral spinal fluid examination: Intramuscular penicillin G benzathine, 2.4 million units once per week for 3 weeks Any patient allergic to penicillin should undergo desensitization and then treatment with penicillin Sex partners exposed within 90 days before diagnosis should undergo treatment |
FIGURE 2
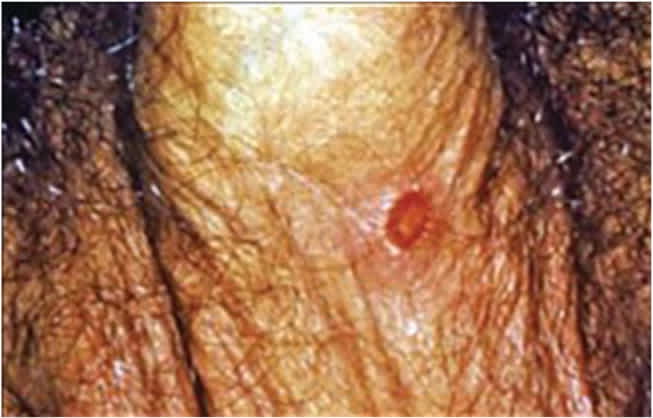
Primary syphilis begins as a single, well-demarcated ulcer (chancre) with a clean base and indurated border.
Photo courtesy of N.J. Fiumara, Gavin Hart; Centers for Disease Control and Prevention
Chancroid ulcerations are usually nonindurated, painful lesions (Figure 3, Table 21,16,17 ). They are characterized by a serpiginous border surrounding a friable base covered with a necrotic and often purulent exudate. A painful, unilateral inguinal adenitis is present in one-half of cases,19 and these can develop into buboes, an inflammatory swelling of lymphatic glands in the groin area.19 Behçet syndrome is most commonly characterized by minor aphthous ulcers (round and less than 10 mm in diameter).20
FIGURE 3
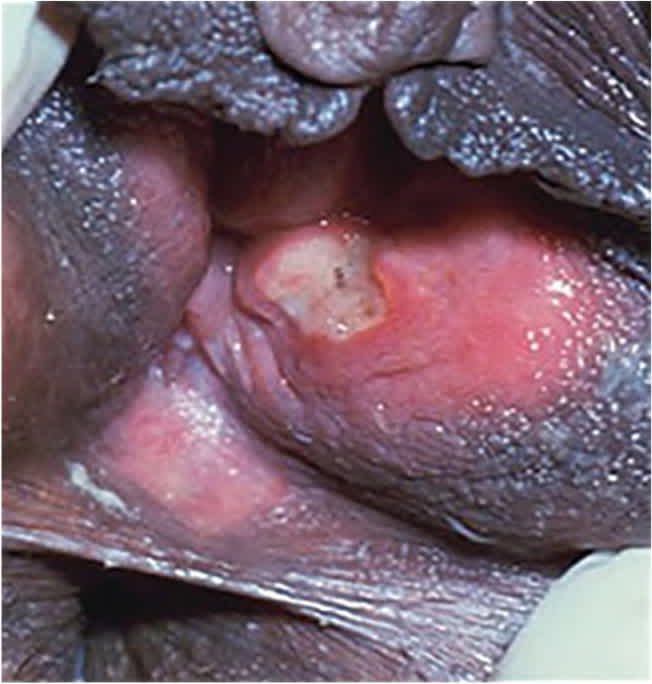
Chancroid ulcers are usually nonindurated with serpiginous borders and friable base, often covered with purulent exudate.
Photo courtesy of Connie Celum, Walter Stamm; Seattle STD/HIV Prevention Training Center, University of Washington
LABORATORY EVALUATION
The CDC recommends that physicians routinely ask men who have sex with men about common STI symptoms (e.g., urethral discharge, dysuria, genital and perianal ulcers, regional lymphadenopathy, skin rash) and perform appropriate diagnostic testing when indicated.1 An initial genital ulcer eruption may be diagnosed by observation of characteristic lesions, but if indicated, may be evaluated with laboratory testing (Table 21,16,17 ), including polymerase chain reaction testing for HSV DNA and HSV type-specific serology. Serologic testing for syphilis should be performed. Culture for H. ducreyi should be included only in settings with a high chancroid prevalence.19 HSV polymerase chain reaction sensitivity is 96% to 100%, 1.5 to four times greater than viral culture, and specificity is 97% to 98%.3,21–23 HSV serologic testing may be appropriate in women when definitive diagnosis by observation of lesions is not possible, when HSV DNA testing or viral isolation from active lesions is unavailable, or with a higher pretest probability such as persistent, unexplained genitourinary symptoms.18 HSV-2 serology and point-of-care tests from serum or capillary blood are available, with 80% to 98% sensitivity, but more frequent false-negative results occur at the early stage of infection.24 However, HSV-2 serologic testing has low specificity and produces many false-positive results.25 Immunoglobulin M testing for HSV-1 or -2 is not indicated because the virus might be positive during recurrent episodes.25
Syphilis infections are detected by serologic testing.1 Darkfield microscopy and direct fluorescent antibody tests of exudate or tissue are definitive for diagnosing early syphilis.1,20 A presumptive diagnosis can be made with the use of two types of serologic tests: nontreponemal tests (e.g., VDRL, rapid plasma reagin) and treponemal tests (e.g., fluorescent treponemal antibody absorbed, T. pallidum particle agglutination, enzyme immunoassays, rapid treponemal assays, immunoblots, chemiluminescence immunoassays).1 Treponemal tests may be reactive for a lifetime.
A positive rapid plasma reagin is considered indicative of an active infection.19 However, a reactive nontreponemal test (e.g., rapid plasma reagin) should always be followed by a confirmatory treponemal test to confirm the diagnosis of syphilis. Using only one type of serologic test is inadequate for diagnosis because false-positive nontreponemal test results are sometimes associated with other conditions unrelated to syphilis such as systemic lupus erythematosus and viral hepatitis.26 Nontreponemal tests typically become nonreactive with time after treatment, but in some patients, low titer antibodies may persist for extended periods (i.e., serofast reaction). Titers for nontreponemal antibodies are generally used to follow response, which is considered successful if a fourfold decrease is observed. If a second treponemal test is positive and the patient has a history of previous treatment, then repeated treatment is indicated only if sexual history suggests reexposure. Repeat testing in two to four weeks is recommended to evaluate for early infection. For neurosyphilis, the VDRL–cerebrospinal fluid test is highly specific, but it is not highly sensitive.
A definitive diagnosis of chancroid requires the identification of H. ducreyi on special culture media not readily available from commercial sources, with sensitivity less than 80%. There is no polymerase chain reaction test for H. ducreyi approved by the U.S. Food and Drug Administration available in the United States.1
Differential Diagnosis
In the United States, most sexually active patients who present with genital ulcers have HSV or syphilis3 (Table 11–3 ). HSV-2 predominates as the pathogen in adolescents, with an increasing incidence of HSV-1-positive genital cultures, especially in women.27 In adolescent men who have sex with men, syphilis predominates. From 2007 to 2010, 87.4% of HSV-2 seropositive people 14 to 49 years of age reported that they were unaware of any personal history or discussion with a health care professional about having genital herpes.4 Syphilis and chancroid are more common in adults than adolescents. Other infectious causes of vulvar ulcers include granuloma inguinale (K. granulomatis), lymphogranuloma venereum (C. trachomatis L1-L3), and rare cases of mononucleosis (Epstein-Barr virus).1,28 Lymphogranuloma venereum and granuloma inguinale are rare infections in the United States; outbreaks of lymphogranuloma venereum typically occur in men who have sex with men, with proctitis or proctocolitis as the typical finding and genital ulcerations with inflamed inguinal lymph nodes (buboes) being less common.16
Treatment
The 2015 CDC sexually transmitted disease guidelines provide strategies for the management of patients with STI-related genital ulcer disease1 (Table 21,16,17 ). Early treatment of HSV without serologic testing or waiting for results decreases transmission and duration of symptoms.1 Acyclovir and valacyclovir (Valtrex) are effective for preventing HSV transmission, viral shedding, reducing healing time, and relieving pain in immunocompromised patients.29 All patients should abstain from sexual activity in the presence of lesions, including abstinence during the herpes prodrome.1 For maternal HSV, suppressive therapy reduces the risk of active lesions during labor,30 reducing the risk of recurrence by 75% and reducing the rate of cesarean delivery secondary to HSV by 40%.31 Daily oral suppressive medication is effective for preventing recurrence of HSV ulcers. Pericoital application of tenofovir gel may reduce the likelihood of HSV-2 transmission to women but is not currently recommended for suppressive therapy.32 Although viral shedding is reduced by 90% while patients are taking oral suppressants, some risk of transmission still exists.17
Asymptomatic patients with genital HSV-2 still exhibit genital viral shedding up to 10.2% of the time, compared with 20.1% for symptomatic patients.33 In those with symptomatic HSV outbreaks, suppressive therapy should be considered to reduce transmission to seronegative partners.17 Recurrent HSV-1 infection may be slower to heal and more painful for patients who are immunocompromised, such as during cancer treatment.29 Based on the high prevalence of primary and secondary syphilis for men who have sex with men, if the patient presents with a genital ulcer, the CDC recommends presumptive treatment for syphilis after serologic testing has been performed.1
Noninfectious ulcers may be treated with topical treatments such as pastes, gels, sprays, injections, laser, and locally dissolving tablets, many of which are available as over-the-counter therapies, but limited evidence exists for topical prescriptions.34 Extensive genital ulcers may be treated with cool water or saline, topical antimicrobials, topical or oral analgesics, perineal baths, topical or oral anti-inflammatory agents, or cool compresses with over-the-counter Burow solution to decrease surrounding edema, inflammation, and pain.34 In the patient with a persistent ulcer after treatment, consider biopsy of the ulcer to help identify other causes.1
Prevention and Screening
The USPSTF recommends screening for syphilis infection for those at risk,35 early screening for syphilis infection in all pregnant women,36 and against routine serologic screening for genital HSV infection in asymptomatic adolescents and adults, including those who are pregnant.37 The CDC recommends that physicians offer evidence-based counseling on safer sex using interventions known to decrease STI incidence.1 The USPSTF recommends screening for HIV in adolescents and adults who are at increased risk.38 HIV screening should be completed for all people with genital, anal, or perianal ulcers with unknown HIV status.1 The USPSTF also recommends preexposure prophylaxis for patients at risk for HIV, which includes those previously diagnosed with syphilis.39 STI risk-reduction counseling is the primary method of health education related to genital ulcer disease, but in some circumstances it may be less effective. For instance, individualized patient-centered risk-reduction counseling at the time of rapid HIV testing among adults 18 years and older does not significantly reduce the risk of subsequent STIs.40
Risk-reduction counseling should include limiting the number of sex partners, encouraging male or female condom use with each sexual encounter, and recommending regular STI screening. Condom use reduces but does not eliminate risk of transmission because mucocutaneous ulcers may transmit infection by contact with skin not covered by a condom.21,41 The three most common pathogens implicated in genital ulcer disease (HSV-2, HSV-1, and T. pallidum) can be efficiently transmitted by oral sex.
This article updates a previous article on this topic by Roett, et al.21
Data Sources: The literature search strategy included using PubMed, Cochrane, Essential Evidence Plus, and U.S. Preventive Services Task Force searching key words diagnosis, treatment, and management of genital ulcers; herpes simplex virus; and sexually transmitted infection/disease treatment guidelines from September 1, 2018, to October 1, 2019. This article is an update of a prior publication; therefore, the prior AFP publications on genital ulcers were reviewed.

