Family physicians are in a unique position to care for transgender athletes, including providing preventive and gender-affirming care and addressing acute athletic injuries and chronic health concerns.1,2 Clinical considerations while caring for transgender patients become even more relevant in athletes because of the additional social and physical challenges that occur in sports. Transgender athletes may have poor access to inclusive competitive environments, and hormonal and surgical gender-affirming treatments affect biologic health and clearance to compete.3 There are no valid statistics on the percentage of athletes who identify as transgender; however, approximately 0.6% of adults in the United States (1 to 1.4 million) identify as transgender,4,5 and 2% of surveyed high schoolers identified as transgender (150,000 to 300,000).6
The most recent edition of the PPE: Preparticipation Physical Evaluation Monograph, which was released in 2019, highlights clinical considerations and participation guidelines for transgender athletes, such as emphasizing the psychosocial evaluation.7 A key stressor is the degree of acceptance of the athlete's preferred gender identity by athletic organizations, school administrators, coaches, and teammates. When obtaining a medical history during the preparticipation physical evaluation (PPE), physicians should allow athletes to self-identify using the two-step method of gender identity: inquiring about gender identity and sex assigned at birth.8 Additionally, athletes should be asked their preferred name and pronouns to create an inclusive environment integral to the physician-patient relationship. It is also important to address transition plans that may impact the current competitive season, including past surgeries, future surgical plans, and the stability of gender-affirming hormone therapy. Gender-affirming hormone therapy may include the use of testosterone as a masculinizing hormone or estrogen as a feminizing hormone.
Routine management of gender-affirming therapy is not part of the PPE,7 but it is an important opportunity for the family physician to consider the effects of hormones on the athlete's health. For example, testosterone therapy in a transgender male athlete can impact bone and muscle mass.9 Spironolactone, a potassium-sparing diuretic, may be used in a transgender female athlete to block testosterone synthesis, but it could create electrolyte imbalances and increase the risk of hyperkalemia.9 Those undergoing gonadotropin-releasing hormone blockade may be at increased risk of temperature instability. More importantly, gonadotropin-releasing hormone blockade may affect bone mineral density, which can make athletes more susceptible to skeletal stress injuries.3,8,10 However, there are currently few studies on the clinical impact of gender-affirming hormone therapy on bone mass.9
The illicit use of supplemental testosterone as a performance-enhancing drug has led to the regulation of hyperandrogenism in competitive cisgender and transgender female athletes. The International Olympic Committee and various other organizations at the state and national levels have implemented regulations on what hormone levels are acceptable for transgender female athletes to be eligible to compete.11 These regulations are not uniform, and at the high school level, they vary by state. The International Olympic Committee states that for a transgender female athlete to compete as a female in an Olympic competition, the total testosterone level must be below 288.18 ng per dL (10 nmol per L) for at least 12 months.11,12 The International Association of Athletics Federations requires transgender female athletes to maintain a total testosterone level below 144.09 ng per dL (5 nmol per L) for at least six months before and during international competition.12,13
The International Olympic Committee does not regulate testosterone levels for transgender males and competing as a male, but it requires a therapeutic use exemption for use of testosterone in any form. For transgender female athletes, a therapeutic use exemption is necessary for the use of spironolactone. More specific guidance about therapeutic use exemptions in transgender athletes is provided by the World Anti-Doping Agency (https://www.wada-ama.org/sites/default/files/resources/files/tue_physician_guidelines_transgender_version1.1.pdf).
Transgender athletes may also undergo surgery as part of their transition, which may affect their ability to compete. As part of preoperative counseling, physicians and athletes should discuss expectations about return-to-sport participation. Physicians should also be aware of potential complications of body-modifying garments. Before mastectomy with chest wall reconstruction, transgender male athletes may bind their chests, using tight garments to create a flatter contour. Binding can lead to skin infections, musculoskeletal pain, neurologic changes, overheating, rib fractures, and local discomfort.3,14 It can also restrict the chest wall, impeding respiratory function, which may impact performance.3,8 Before surgery, transgender female athletes may tuck their penis and or testicles. Tucking can lead to complications such as inguinal hernias, urinary reflux, prostatitis, cystitis, or epididymo-orchitis.
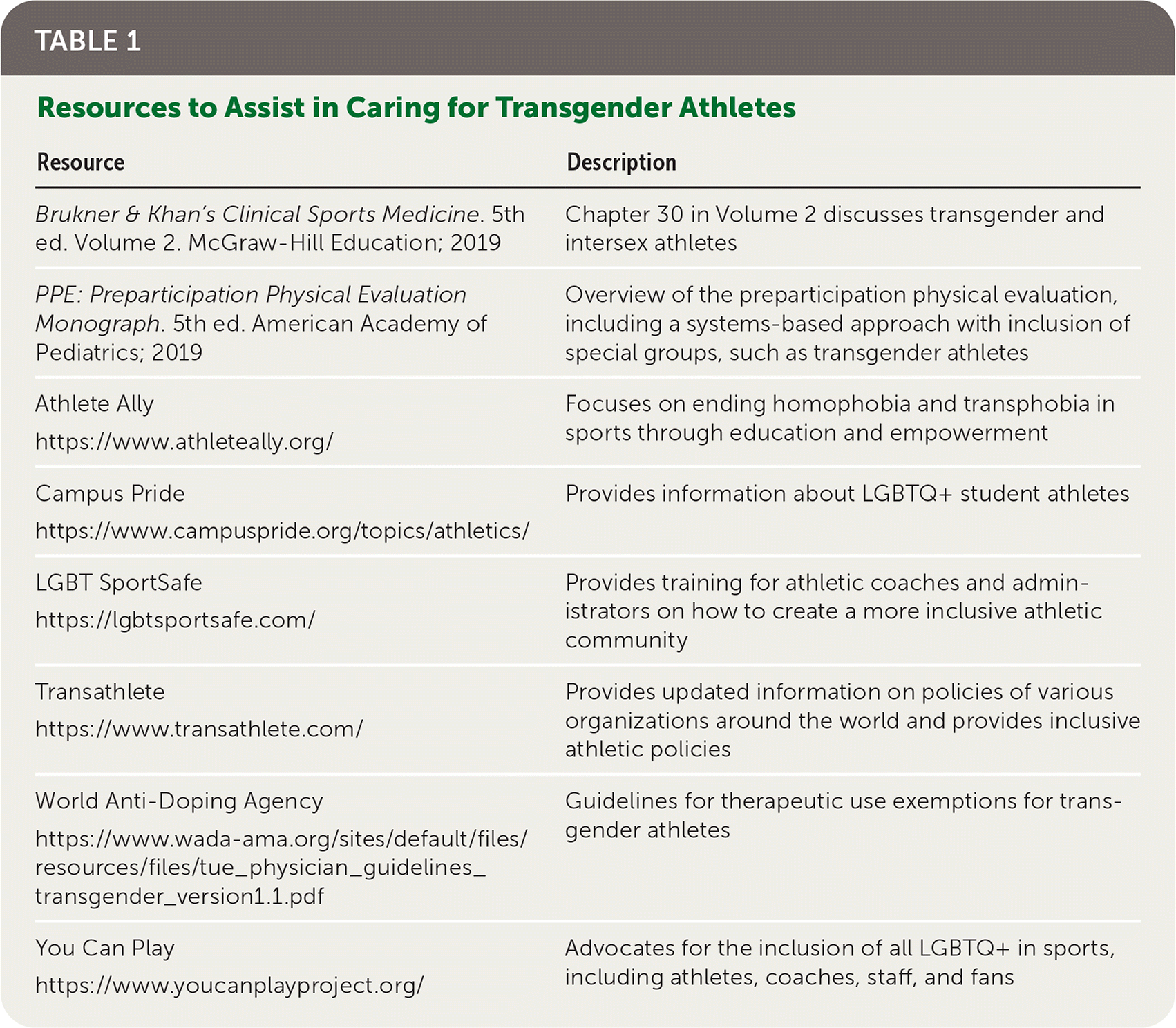
The resources in Table 1 can further assist family physicians in providing comprehensive care to transgender athletes. Roles of the family physician may include working with athletes on their transition plan, performing a psychosocial evaluation, and coordinating care with specialists and athletic teams as needed to provide guidance on competition and return-to-sport participation.
TABLE 1. Resources to Assist in Caring for Transgender Athletes
| Resource | Description |
|---|---|
| Brukner & Khan's Clinical Sports Medicine. 5th ed. Volume 2. McGraw-Hill Education; 2019 | Chapter 30 in Volume 2 discusses transgender and intersex athletes |
| PPE: Preparticipation Physical Evaluation Monograph. 5th ed. American Academy of Pediatrics; 2019 | Overview of the preparticipation physical evaluation, including a systems-based approach with inclusion of special groups, such as transgender athletes |
| Athlete Ally https://www.athleteally.org/ | Focuses on ending homophobia and transphobia in sports through education and empowerment |
| Campus Pride https://www.campuspride.org/topics/athletics/ | Provides information about LGBTQ+ student athletes |
| LGBT SportSafe https://lgbtsportsafe.com/ | Provides training for athletic coaches and administrators on how to create a more inclusive athletic community |
| Transathlete https://www.transathlete.com/ | Provides updated information on policies of various organizations around the world and provides inclusive athletic policies |
| World Anti-Doping Agency https://www.wada-ama.org/sites/default/files/resources/files/tue_physician_guidelines_transgender_version1.1.pdf | Guidelines for therapeutic use exemptions for transgender athletes |
| You Can Play https://www.youcanplayproject.org/ | Advocates for the inclusion of all LGBTQ+ in sports, including athletes, coaches, staff, and fans |
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the U.S. government.
Drs. Marra and Conlon are military service members. This work was prepared as part of their official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. 101 defines a United States Government work as a work prepared by a military service member or employee of the United States Government as part of that person's official duties.

