Clinical Question
Can the neonatal early-onset sepsis calculator safely and accurately evaluate the risk of early-onset sepsis in neonates?
Evidence Summary
Although early-onset sepsis is a potentially fatal condition in neonates, the incidence in the United States has significantly decreased over the past two decades with the implementation of intrapartum antibiotic prophylaxis for group B Streptococcus (GBS).1 Many neonates are unnecessarily exposed to empiric antibiotic therapy because physicians are using the Centers for Disease Control and Prevention (CDC) guidelines for management of early-onset sepsis. For every episode of culture-proven sepsis, up to 118 high-risk infants and up to 1,400 well-appearing infants born to mothers with chorioamnionitis will receive antibiotic therapy.2 Exposure to empiric antibiotics can result in sequelae, including separation of mother and infant, increased neonatal intensive care unit (NICU) admissions, difficulty breastfeeding, and increased health care costs.1,2
The Kaiser Permanente neonatal early-onset sepsis calculator (https://neonatalsepsiscalculator.kaiserpermanente.org) is a tool designed to improve the selection of neonates with suspected early-onset sepsis to receive empiric antibiotic therapy. The tool was created after analyzing a cohort of 608,014 newborns born at 34 weeks' gestation or later at 14 hospitals in the United States.3 This multivariate risk-assessment tool uses the estimated incidence of early-onset sepsis in a specific health care setting, gestational age, highest maternal antepartum temperature, length of rupture of membranes, maternal GBS status, and type of intrapartum antibiotics to calculate the risk of early-onset sepsis at birth. This risk is adjusted based on the clinical status of the infant by defining neonates as well-appearing, equivocal, or with clinical illness based on objective findings from a clinical examination. Based on the overall risk of early-onset sepsis, clinical monitoring, laboratory evaluation, or antibiotic administration is recommended. The creators of the risk assessment tool estimate that use of the calculator could result in 80,000 to 240,000 fewer newborns in the United States receiving antibiotic treatment.3
A meta-analysis of six high-quality non-randomized controlled trials and 172,385 neonates evaluated the sepsis calculator vs. the standard approach recommended by CDC guidelines for management of early-onset sepsis.1 All studies were published in 2017 or later and reported a statistically significant reduction in antibiotic use in neonates who were treated using the sepsis calculator compared with the standard approach (3.3% vs. 6%; odds ratio [OR] = 0.22; 95% CI, 0.14 to 0.36; P < .00001). The number needed to treat (NNT) was 37 to prevent the use of antibiotics in one neonate. An additional meta-analysis using many of the same studies confirmed the findings related to antibiotic use.2 Five of the studies reported data on laboratory testing for early-onset sepsis and included 168,432 neonates. All five studies reported a reduction in the number of laboratory tests in neonates who were treated using the sepsis calculator (2.5% vs. 15.5%; OR = 0.14; 95% CI, 0.08 to 0.27; P < .00001), with an NNT of 8 to prevent the use of laboratory testing in one neonate.1
Four studies involving 16,628 neonates included data on admissions to the NICU, three of which demonstrated a significant reduction in admissions. Meta-analysis confirmed similar findings (5.4% vs. 19%; OR = 0.24; 95% CI, 0.11 to 0.51; P < .0001), with an NNT of 7 to prevent one admission to the NICU.1 Data regarding readmissions to the NICU were available from three studies and included 156,394 neonates. All studies reported no difference in readmission rates, and meta-analysis confirmed these findings (OR = 0.87; 95% CI, 0.57 to 1.33; P = .53).1 Meta-analysis of all six studies, including 172,385 neonates, reported no difference in culture-positive sepsis between neonates treated using the sepsis calculator and those treated with the standard approach (OR = 0.94; 95% CI, 0.51 to 1.74; P = .85).1 Table 1 summarizes the NNTs of the sepsis calculator compared with standard care.1,2
TABLE 1. Results of Meta-Analysis Comparing Use of Kaiser Permanente Neonatal Early-Onset Sepsis Calculator with Standard Care
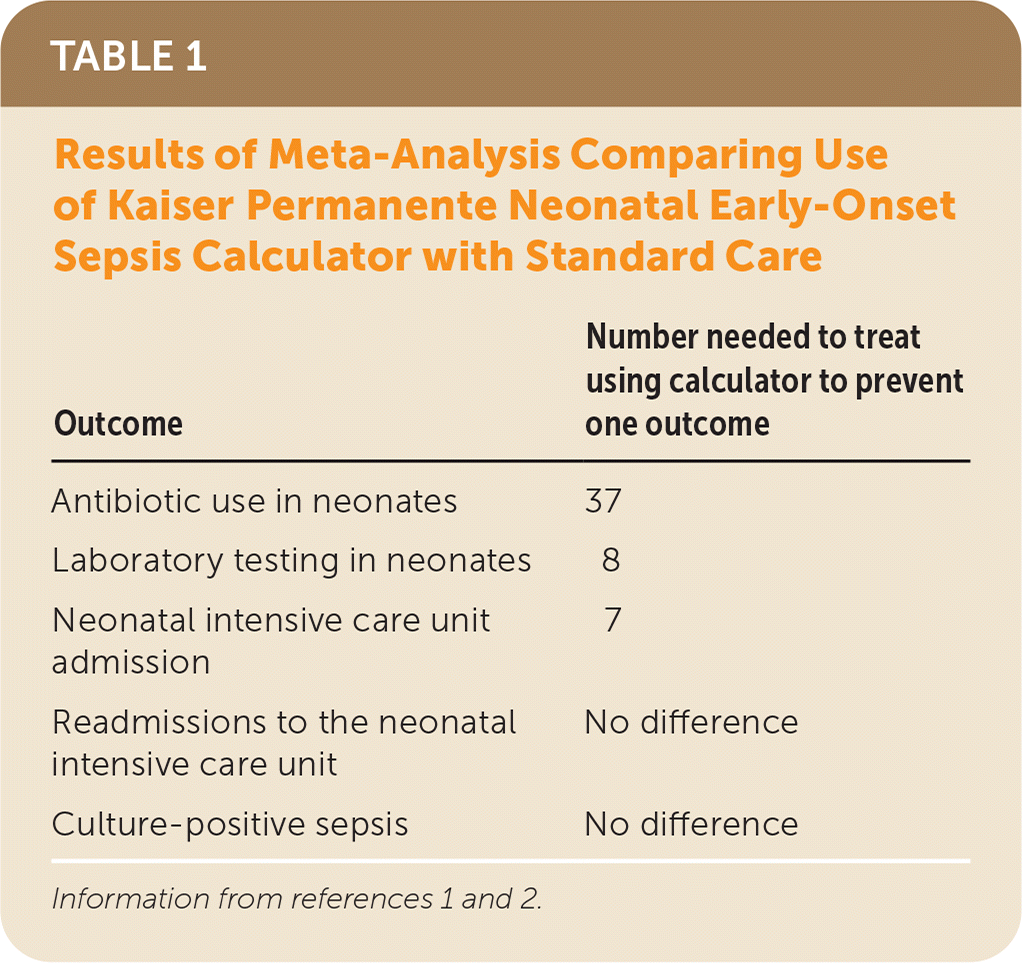
| Outcome | Number needed to treat using calculator to prevent one outcome |
|---|---|
| Antibiotic use in neonates | 37 |
| Laboratory testing in neonates | 8 |
| Neonatal intensive care unit admission | 7 |
| Readmissions to the neonatal intensive care unit | No difference |
| Culture-positive sepsis | No difference |
Evidence on safety was limited.2 Mortality was reported in only one study. Two deaths were reported, one in the sepsis calculator group and one in the standard therapy group. Deaths were attributed to hypoxic-ischemic encephalopathy and pulmonary hypertension, respectively, and both neonates received prompt antibiotic therapy. No increase was found in the incidence of early-onset sepsis or mortality with the use of the calculator across all studies. There was no increase in missed cases of early-onset sepsis; five of 18 (28%) were missed with the sepsis calculator and eight of 28 (29%) were missed with standard therapy. Newborns with missed early-onset sepsis were started on antibiotics.2
There is moderate-quality evidence that the implementation of the sepsis calculator is associated with reduced antibiotic administration and laboratory testing. Available data indicate no difference in rates of mortality, readmission to the NICU, or culture-positive sepsis between neonates treated using the sepsis calculator and those treated using the standard approach. Although there is the potential for missing culture-positive sepsis or delaying antibiotic administration with the CDC guideline and the sepsis calculator, there is an opportunity to significantly reduce exposure to empiric antibiotics and related sequelae using the latter.
Applying the Evidence
An infant was born at 37 weeks' gestation to a mother with chorioamnionitis that was diagnosed after she had a fever of 102.2°F (39.0°C) during labor. Rupture of membranes occurred 12 hours before delivery. Maternal GBS status was unknown, and the mother received broad-spectrum antibiotics three hours before birth. Using the CDC national incidence of early-onset sepsis of 0.5 per 1,000 live births, the calculator estimates this infant's early-onset sepsis risk to be 2.12 per 1,000 births. After determining that the infant is well-appearing on clinical examination, the risk is adjusted to 0.87 per 1,000 births. No blood cultures are obtained, and antibiotics are not initiated. Vital signs are checked every four hours for 24 hours, and the infant continues to have normal measurements and clinically appears well. The infant is discharged home with the mother at 48 hours.
Editor's Note: Dr. Brown is a contributing editor for AFP.

