Childhood sleep disorders can disrupt family dynamics and cause cognitive and behavior problems. Early recognition and management can prevent these complications. Behavior subtypes of childhood insomnias affect 10% to 30% of children and result from inconsistent parental limit-setting and improper sleep-onset association. Behavior insomnias are treated using extinction techniques and parent education. Hypnotic medications are not recommended. Obstructive sleep apnea affects 1% to 5% of children. Polysomnography is required to diagnose obstructive sleep apnea; history and physical examination alone are not adequate. Adenotonsillectomy is the first-line treatment for obstructive sleep apnea. Nasal continuous positive airway pressure is the second-line treatment for children who do not respond to surgery or if adenotonsillectomy is contraindicated. Restless legs syndrome can be difficult to recognize and has an association with attention-deficit/hyper-activity disorder. Management of restless legs syndrome includes treatment of iron deficiency, if identified, and removal of triggering factors. Parasomnias affect up to 50% of children and usually resolve spontaneously by adolescence. Management of parasomnias involves parental education, reassurance, safety precautions, and treating comorbid conditions. Delayed sleep phase syndrome is found during adolescence, manifesting as a night owl preference. Treatment of delayed sleep phase syndrome includes sleep hygiene, nighttime melatonin, and morning bright light exposure. Sleep deprivation is of increasing concern, affecting 68% of people in high school.
Sleep is essential for good health and is an important part of child and family life. Sleep supports homeostatic, cognitive, immune, and cardiovascular functions and is fundamental for a child's growth and development. Sleep disruptions can lead to cognitive and emotional challenges and affect family dynamics.1,2 Early recognition and management can prevent these complications. This article provides an overview of common sleep disorders in children.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
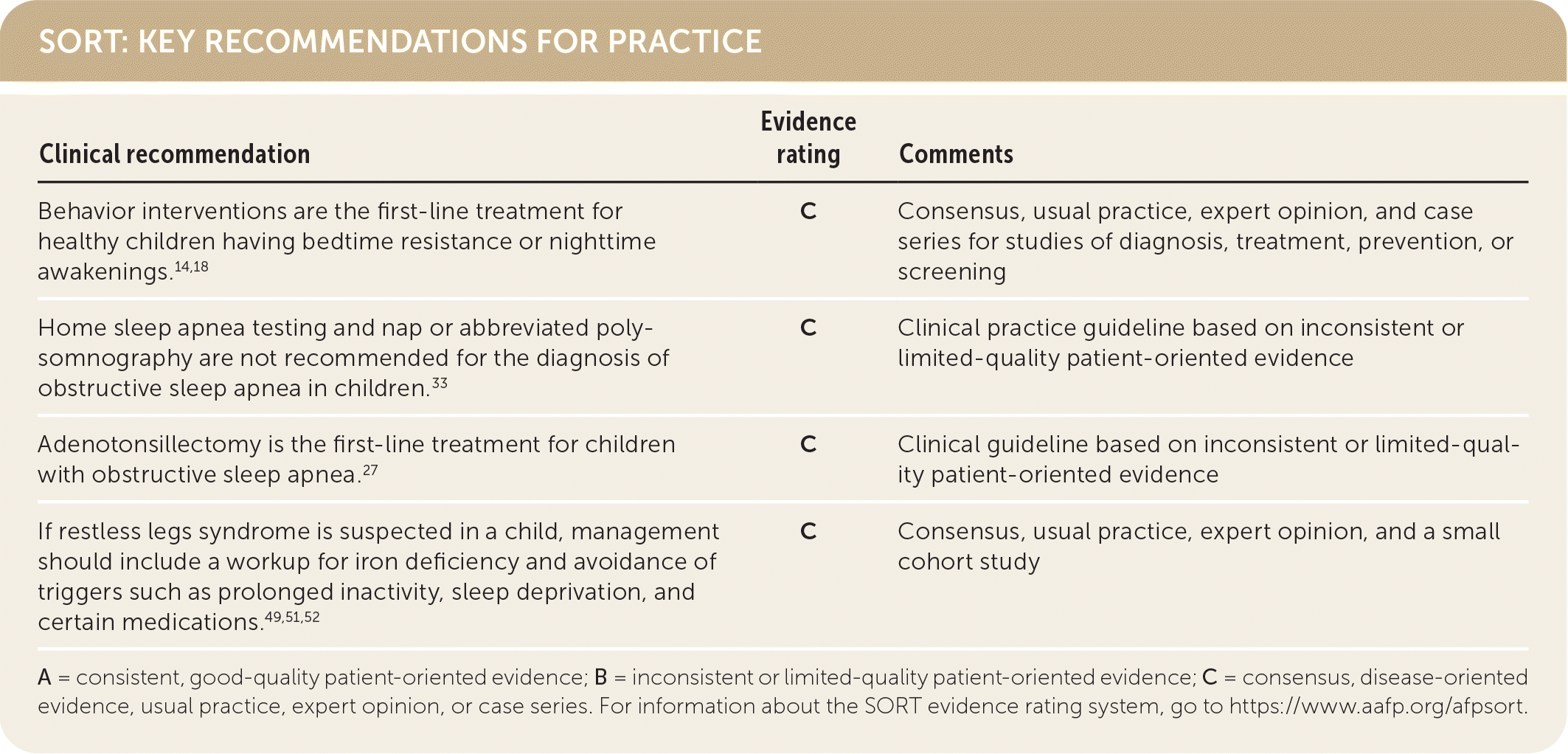
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN SLEEP MEDICINE

| Recommendation | Sponsoring organization |
|---|---|
| Do not prescribe medication to treat behavioral childhood insomnia, which usually develops from parent-child interactions and responds to behavior interventions. | American Academy of Sleep Medicine |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Inadequate sleep and sleep disorders can present differently in children. Adults present with fatigue and daytime sleepiness; however, children may present with behavior problems, including irritability, hyperactivity, and poor school performance. Teenagers may experience increased motor vehicle crashes caused by drowsy driving.3 Although 50% of children may experience sleep problems, only 4% are diagnosed with a formal sleep disorder.4 Children with sleep disorders have at least two more clinic visits for illnesses per year than those without sleep issues.5
Normal Sleep Development
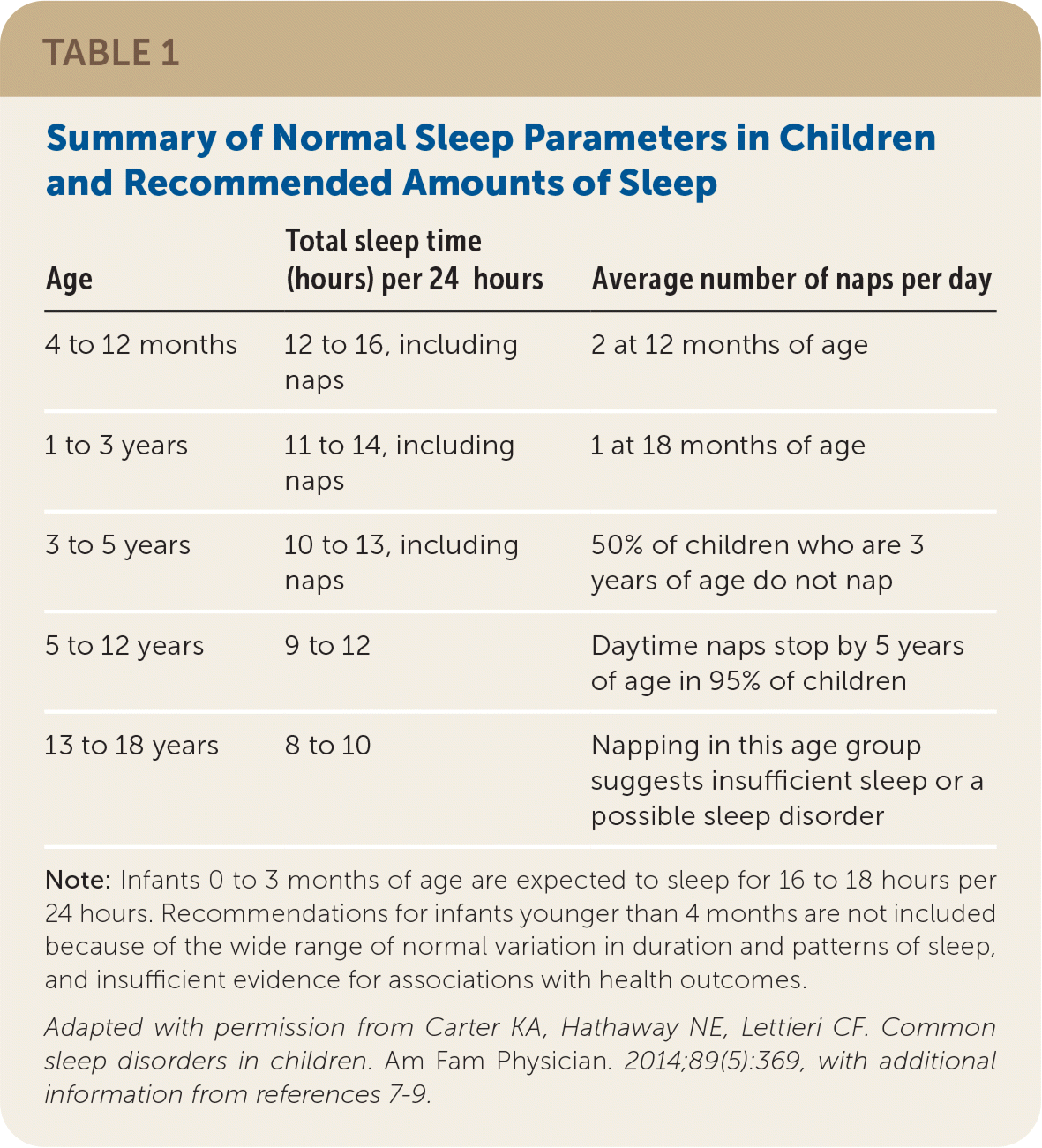
Sleep architecture and patterns change from infancy through adolescence. Understanding normal sleep patterns and progression helps clinicians and caretakers differentiate normal sleep behavior from sleep disorders (Table 16–9 ).
TABLE 1. Summary of Normal Sleep Parameters in Children and Recommended Amounts of Sleep
| Age | Total sleep time (hours) per 24 hours | Average number of naps per day |
|---|---|---|
| 4 to 12 months | 12 to 16, including naps | 2 at 12 months of age |
| 1 to 3 years | 11 to 14, including naps | 1 at 18 months of age |
| 3 to 5 years | 10 to 13, including naps | 50% of children who are 3 years of age do not nap |
| 5 to 12 years | 9 to 12 | Daytime naps stop by 5 years of age in 95% of children |
| 13 to 18 years | 8 to 10 | Napping in this age group suggests insufficient sleep or a possible sleep disorder |
Note: Infants 0 to 3 months of age are expected to sleep for 16 to 18 hours per 24 hours. Recommendations for infants younger than 4 months are not included because of the wide range of normal variation in duration and patterns of sleep, and insufficient evidence for associations with health outcomes.
Adapted with permission from Carter KA, Hathaway NE, Lettieri CF. Common sleep disorders in children. Am Fam Physician. 2014;89(5):369, with additional information from references 7–9.
Newborns typically sleep one to four hours at a time and frequently wake for feeding. Circadian rhythm is endogenously generated and cycles over 24 hours. Defined sleep and wake periods are generally seen after two months of age.10 Infants start to develop the ability to sleep through the night by five to six months of age. Infants should be placed on their backs to sleep in a supine position until they reach one year of age to decrease the risk of sudden infant death syndrome. Sleeping in a side position is not safe and is not recommended.11 Prevalence of common childhood sleep disorders differs by age group (Table 26 ).
TABLE 2. Common Sleep Disorders in Children

| Sleep disorder (prevalence) | Clinical features | Diagnostic criteria | Treatment options |
|---|---|---|---|
| Childhood insomnias (behavior subtypes; 10% to 30%) | Sleep-onset association: children have trouble falling asleep without relying on a person or activity such as rocking or other environmental cue, which results in a significant delay or absence of sleep onset without caregiver involvement Limit-setting: parent or caregiver does not establish sleep routines, or limits are not consistently followed Mixed: problems with associations and limit-setting | Diagnosis is clinical Sleep-wake disturbances characterized by difficulties in initiating or maintaining sleep occurring at least 3 times per week for at least 3 months | Behavior interventions (Table 3) Hypnotic medications are not recommended |
| Obstructive sleep apnea (1% to 5%, peaks between 2 and 8 years) | Recurrent episodes of partial or complete upper airway obstruction associated with arousals, awakenings, or oxygen desaturations (Table 5) Obesity and tobacco smoke exposure are risk factors | Polysomnography Home sleep apnea testing is not recommended | Adenotonsillectomy Nasal continuous positive airway pressure for second-line treatment |
| Restless legs syndrome (2% to 4%; more common in adolescents) | Unpleasant sensations in the legs that cause difficulty in initiating and maintaining sleep; daytime symptoms can happen with extended periods of inactivity or sitting About one-fourth of patients with restless legs syndrome have attention-deficit/hyperactivity disorder symptoms, and up to one-third with attention-deficit/hyperactivity disorder have restless legs syndrome | Diagnosis is clinical and requires the following: (1) urge to move legs because of unpleasant or uncomfortable sensations, (2) sensations begin or worsen with rest or inactivity, lying down, or sitting, (3) temporary partial or complete relief with movement such as stretching or walking, (4) occurs mostly in the evening or night, (5) symptoms cause sleep disturbance or impairment of daytime functioning, and (6) symptoms need to be described in the child's words | Iron therapy of 3 mg per kg per day if ferritin levels < 50 ng per mL (50 mcg per L) Screen for and address triggers if identified as cause or contributing factor (e.g., prolonged inactivity, sleep deprivation, diphenhydramine [Benadryl], selective serotonin reuptake inhibitors, metoclopramide [Reglan], caffeine, nicotine, alcohol) |
| Parasomnias (up to 50%) | During sleep-wake transitions, activities appear purposeful or automatic, but the child has no meaningful interaction with the environment; child is difficult to arouse, appears confused, may quickly go back to sleep, and may have amnesia about the episode Repetitive stereotypic behaviors and posturing indicate need for investigation for nocturnal seizures | Diagnosis is clinical Polysomnography is indicated if: (1) the description is not typical or there has been an injury, (2) there is concern about nocturnal seizures or rapid eye movement sleep behavior disorder, or (3) there is concern for precipitating factors such as obstructive sleep apnea or periodic limb movement disorder (clustered neurologically mediated leg movements that disturb sleep) | Self-limiting; most resolve spontaneously by adolescence Education and reassurance; address sleep hygiene and stress; treat comorbid conditions such as gastroesophageal reflux, obstructive sleep apnea, and restless legs syndrome; take safety precautions Refer for violent behavior or injury, or when there is no response to conservative treatment |
| Delayed sleep phase syndrome (7% to 16%) | Sleep-onset and wake-up times are delayed | Diagnosis is clinical with a sleep diary for 7 to 14 days showing sleep period delayed by more than 2 hours for at least 3 months | Sleep-wake schedules with patient's input Avoid exposure to bright and blue light (e.g., electronic devices) before bedtime Melatonin (0.3 to 5 mg) given about 1.5 to 6.5 hours before bedtime Bright-light therapy in the first 1 to 2 hours after awakening |
Information from reference 6.
Childhood Insomnia
Insomnias of childhood are sleep or wake disturbances characterized by difficulties in initiating or maintaining sleep, ultimately leading to chronic sleeplessness. Diagnostic criteria specify that disturbances occur at least three times per week for at least three months.12
Bedtime problems are common in young children, with an estimated prevalence of 10% to 30%.13 Parental concerns involve the child's and their own sleeplessness. Behavior insomnias are no longer considered distinct from chronic insomnia but continue being used for diagnosis and treatment because they develop from improper sleep training by parents or caregivers.12
Sleep-onset association insomnia occurs when the child is unable to fall asleep without certain conditions or actions by the parent or caregiver.12 For example, when a child is first put to bed, a parent or caregiver must sing to the child or rock the child for sleep onset. The same action must be repeated every time the child wakes up during the night for them to return to sleep. This approach is not to be confused with bedtime preparatory routines. In limit-setting insomnia, the child stalls or resists going to bed at the designated bedtime.12 For example, the child may demand to spend time watching television past their bedtime, usually because of a parent or caregiver's inadequate implementation of a bedtime schedule. When making a diagnosis of limit-setting insomnia, other causes of bedtime resistance such as underlying fears (e.g., nightmares, being in the dark, sleeping alone) and anxiety need to be considered. Most children with behavior insomnias have features of the sleep-onset association and limit-setting types (i.e., a mixed type). The diagnosis of insomnia is clinical. Polysomnography is not needed unless other sleep disorders are suspected.
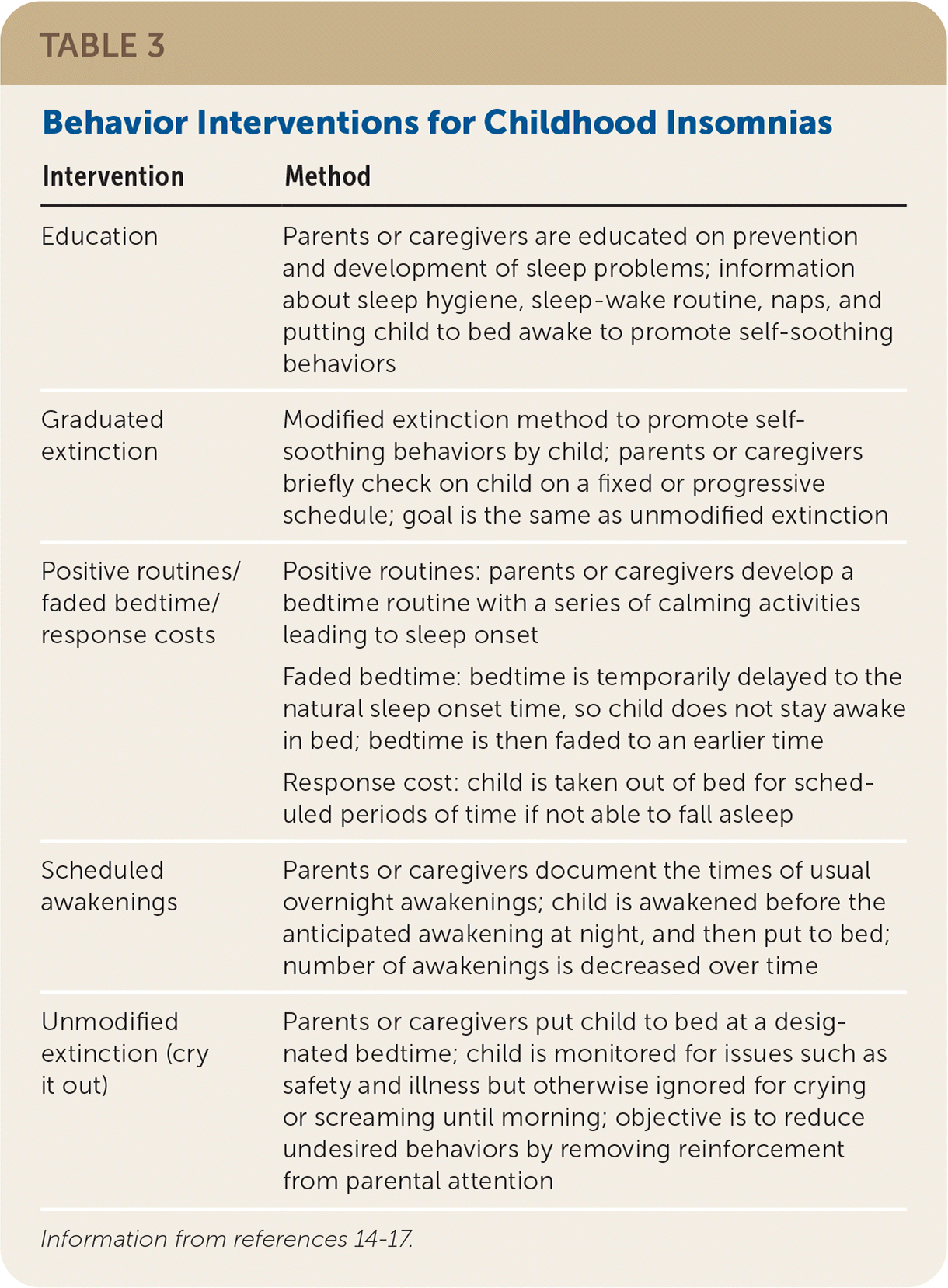
Behavior interventions are the first-line treatment for bedtime problems and nighttime awakenings caused by behavior insomnias in healthy infants and children14–18 (Table 314–17 ). Extinction techniques are designed to promote self-soothing behaviors to fall asleep. Infants learn to self-soothe when placed awake in the crib.19 Parental education about age-appropriate sleep times and healthy sleep habits (i.e., sleep hygiene) is important (Table 418,20 ). Following a consistent bedtime routine of calming transition activities such as taking a bath, changing into pajamas, and reading is effective.21 Television and electronic media are best avoided. 22,23 Hypnotic medications are not recommended for the treatment of behavior insomnias.16 Children who do not respond to simple behavior interventions or have complex problems (e.g., medical, psychiatric, developmental) should be referred to a sleep specialist.16,18
TABLE 3. Behavior Interventions for Childhood Insomnias
| Intervention | Method |
|---|---|
| Education | Parents or caregivers are educated on prevention and development of sleep problems; information about sleep hygiene, sleep-wake routine, naps, and putting child to bed awake to promote self-soothing behaviors |
| Graduated extinction | Modified extinction method to promote self-soothing behaviors by child; parents or caregivers briefly check on child on a fixed or progressive schedule; goal is the same as unmodified extinction |
| Positive routines/faded bedtime/response costs | Positive routines: parents or caregivers develop a bedtime routine with a series of calming activities leading to sleep onset Faded bedtime: bedtime is temporarily delayed to the natural sleep onset time, so child does not stay awake in bed; bedtime is then faded to an earlier time Response cost: child is taken out of bed for scheduled periods of time if not able to fall asleep |
| Scheduled awakenings | Parents or caregivers document the times of usual overnight awakenings; child is awakened before the anticipated awakening at night, and then put to bed; number of awakenings is decreased over time |
| Unmodified extinction (cry it out) | Parents or caregivers put child to bed at a designated bedtime; child is monitored for issues such as safety and illness but otherwise ignored for crying or screaming until morning; objective is to reduce undesired behaviors by removing reinforcement from parental attention |
TABLE 4. Sleep Hygiene Recommendations

| Bedtime routines and wake-up time should be as consistent as possible |
| Bedroom should be quiet and dark; temperatures should be comfortably cool; external noise should be minimized |
| Child may have a snack before bedtime if hungry; excessive fluids should be avoided; caffeinated beverages and foods should be avoided for several hours before bedtime |
| Child should learn to fall asleep alone |
| Vigorous activity should be avoided before bedtime |
Obstructive Sleep Apnea
Obstructive sleep apnea (OSA) is defined as recurrent episodes of partial or complete upper airway obstruction associated with arousals, awakenings, or oxygen desaturations despite the respiratory effort.24 OSA disrupts normal sleep patterns and ventilation and is a cause of morbidity in children, with a prevalence of 1% to 5%.25 Habitual snoring, defined as loud snoring at least three nights per week without evidence of hypoxia, hypercarbia, or arousability, is more common with a prevalence of 10% to 27% but warrants further diagnostic consideration because of its strong association with OSA.26 According to the 2012 American Academy of Pediatrics guideline, all children should be screened for snoring at well-child visits.27 OSA peaks between two and eight years of age, coinciding with adenotonsillar hypertrophy, which is the primary cause of upper airway obstruction in children.28 OSA occurs equally in prepubertal males and females. Postpuberty, males have a higher prevalence of OSA. Obesity and tobacco smoke exposure are considered risk factors for OSA.29,30 Children with craniofacial abnormalities, Down syndrome, and neuromuscular disorders have a higher prevalence of OSA.30–32
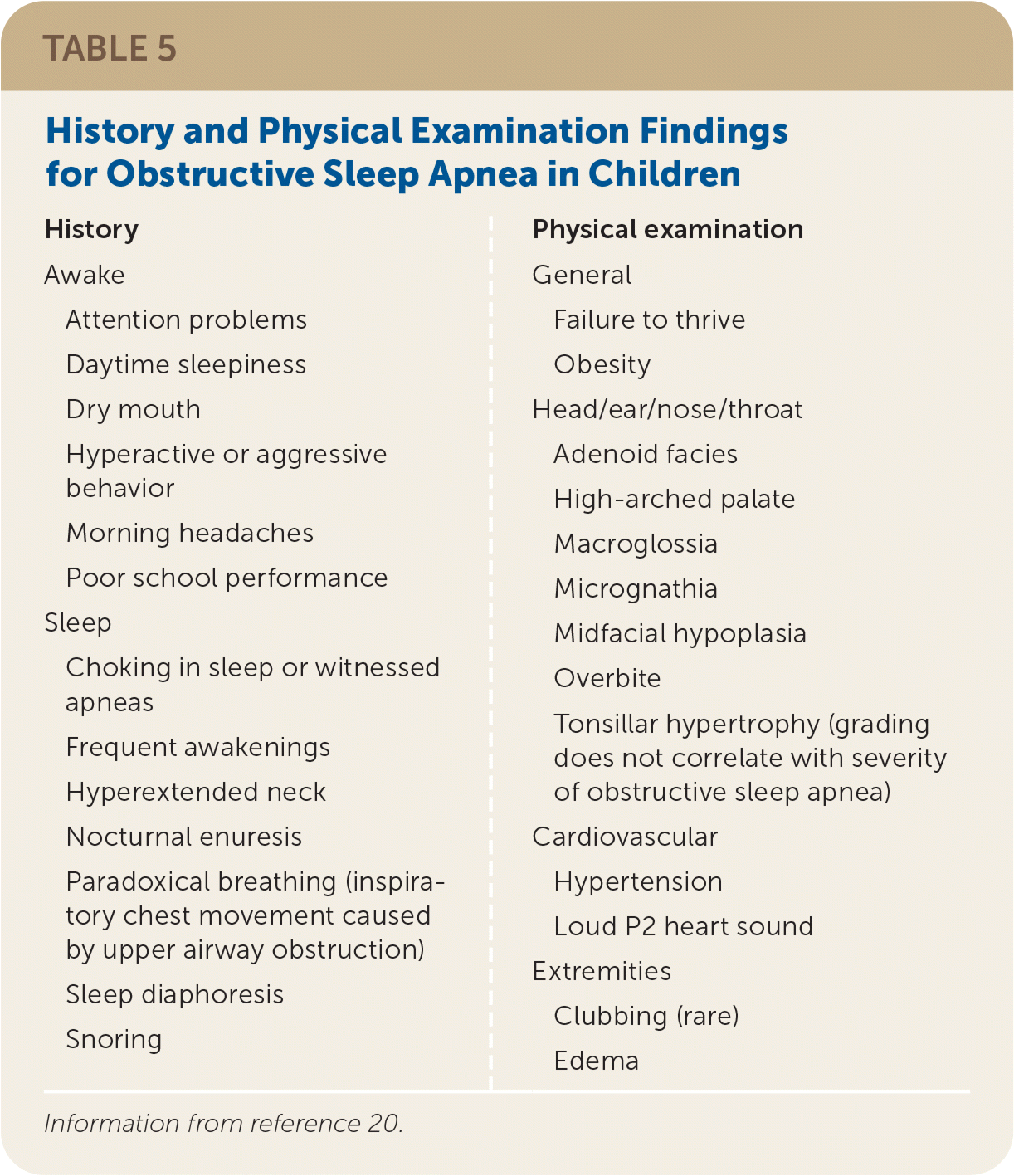
Polysomnography is required to make the diagnosis of OSA. History and physical examination are helpful but do not quantify ventilatory and other disturbances caused by OSA (Table 520 ). Home sleep apnea testing and nap or abbreviated polysomnography are not recommended for evaluation of children with suspected OSA.33
If left untreated, OSA is associated with impaired growth, nocturnal enuresis, problems with attention and emotions, and pulmonary and systemic hypertension34–37 (eTable A). The first-line treatment of OSA in children is adenotonsillectomy.27,38,39 Following adenotonsillectomy, resolution of OSA occurs in 70% of children at a normal body weight but in less than 30% of children who are obese.27
TABLE 5. History and Physical Examination Findings for Obstructive Sleep Apnea in Children
| History Awake Attention problems Daytime sleepiness Dry mouth Hyperactive or aggressive behavior Morning headaches Poor school performance Sleep Choking in sleep or witnessed apneas Frequent awakenings Hyperextended neck Nocturnal enuresis Paradoxical breathing (inspiratory chest movement caused by upper airway obstruction) Sleep diaphoresis Snoring | Physical examination General Failure to thrive Obesity Head/ear/nose/throat Adenoid facies High-arched palate Macroglossia Micrognathia Midfacial hypoplasia Overbite Tonsillar hypertrophy (grading does not correlate with severity of obstructive sleep apnea) Cardiovascular Hypertension Loud P2 heart sound Extremities Clubbing (rare) Edema |
Information from reference 20.
eTABLE A Consequences of Untreated Obstructive Sleep Apnea

| Complication | Mechanism |
|---|---|
| Cardiovascular issues such as hypertension and increased heart rate | Increased adrenaline Nocturnal hypoxemia Renin-angiotensin activation |
| Failure to thrive | Abnormal insulin-like growth factor caused by decreased non–rapid eye movement (Delta) sleep Difficulty swallowing, reduced appetite Increased work of breathing |
| Neurobehavior consequences and oppositional defiant disorder | Nocturnal hypoxemia Sleep fragmentation |
| Nocturnal enuresis | Impaired arousal response Impaired urodynamics Insufficient vasopressin Sleep fragmentation |
Information from:
Hinkle J, Connolly HV, Adams HR, et al. Severe obstructive sleep apnea in children with elevated blood pressure. J Am Soc Hypertens. 2018;12(3):204–210.
Nieminen P, Löppönen T, Tolonen U, et al. Growth and biochemical markers of growth in children with snoring and obstructive sleep apnea. Pediatrics. 2002;109(4):e55.
Su MS, Xu L, Pan WF, et al. Current perspectives on the correlation of nocturnal enuresis with obstructive sleep apnea in children. World J Pediatr. 2019;15(2):109–116.
Patients at high risk (e.g., younger than three years, neuromuscular disorders, chromosomal abnormalities, history of loud snoring with apnea before surgery) should have surgery in a hospital setting with overnight monitoring due to an increased risk of respiratory compromise after adenotonsillectomy.40 Referral to a sleep medicine specialist should be considered for patients at high risk, and these patients need postoperative polysomnography at six to eight weeks to assess for resolution of OSA.
Nasal continuous positive airway pressure is a second-line treatment for children who do not respond to the surgery or for whom adenotonsillectomy is contraindicated (e.g., severe bleeding tendency, craniofacial abnormality, neuromuscular disease, absence of adenotonsillar hypertrophy).27,41,42 Other treatment options such as weight loss, oral appliances, orthodontic treatments, myofascial stimulation,43 topical nasal corticosteroids, or montelukast (Singulair) may be considered for select cases.44
Restless Legs Syndrome
Restless legs syndrome (RLS) is a sensorimotor condition with an estimated prevalence of 2% to 4% in children. It is more common in adolescents than in young children.45 Male and female adolescents are equally affected. Children with chronic kidney disease and those who have first-degree relatives with the condition are more likely to develop RLS.46 About one-fourth of individuals with RLS have attention-deficit/hyperactivity disorder symptoms, and conversely, about 12% to 35% of those with attention-deficit/hyperactivity disorder have RLS.47
Children with RLS report unpleasant sensations in their legs that cause difficulty in initiating and maintaining sleep.45 Children may use phrases such as ‘want to kick' when describing their urge to move. They may describe feeling ants or spiders, tingly, wiggly, and funny in their legs. Some may report daytime symptoms with extended periods of inactivity or sitting in school. RLS is often misdiagnosed as growing pains. The child's mood, energy, and schoolwork may be negatively affected.47,48 Pathophysiology is thought to be caused by a brain iron deficiency, disturbances of dopamine regulation in the central nervous system, and genetic factors.49
Diagnosis is clinical and requires the six following features: urge to move legs because of unpleasant or uncomfortable sensations; sensations begin or worsen with rest or inactivity, lying down, or sitting; temporary partial or complete relief with movement such as stretching or walking; occurs mostly in the evening or night; symptoms cause sleep disturbance or impairment of daytime functioning; and symptoms need to be described in the child's words.50 Polysomnography is not required to make a diagnosis. The differential diagnoses for RLS include leg cramps, positional discomfort, myalgia, venous stasis, leg edema, arthritis, and habitual foot tapping.
Management of RLS requires screening for triggers such as lack of sleep and activity, and medications that can aggravate RLS (Table 26 ). Treatment involves removal of any identified causes or contributing factors and addressing iron deficiency if found. Iron therapy with 3 mg per kg per day of elemental iron should be started if serum ferritin levels are less than 50 ng per mL (50 mcg per L). Periodic measurement of ferritin is recommended.51,52 Other pharmacologic treatments with dopaminergic medications, alpha-2 ligands (e.g., gabapentin [Neurontin]), benzodiazepines, and clonidine have not been adequately investigated in children.53
Parasomnias
Parasomnias are undesirable physical events or experiences during sleep onset, within sleep, or during arousal from sleep.54 They affect up to 50% of children.55 Most parasomnias resolve spontaneously by adolescence; however, up to 4% of individuals may have persistence into adulthood.
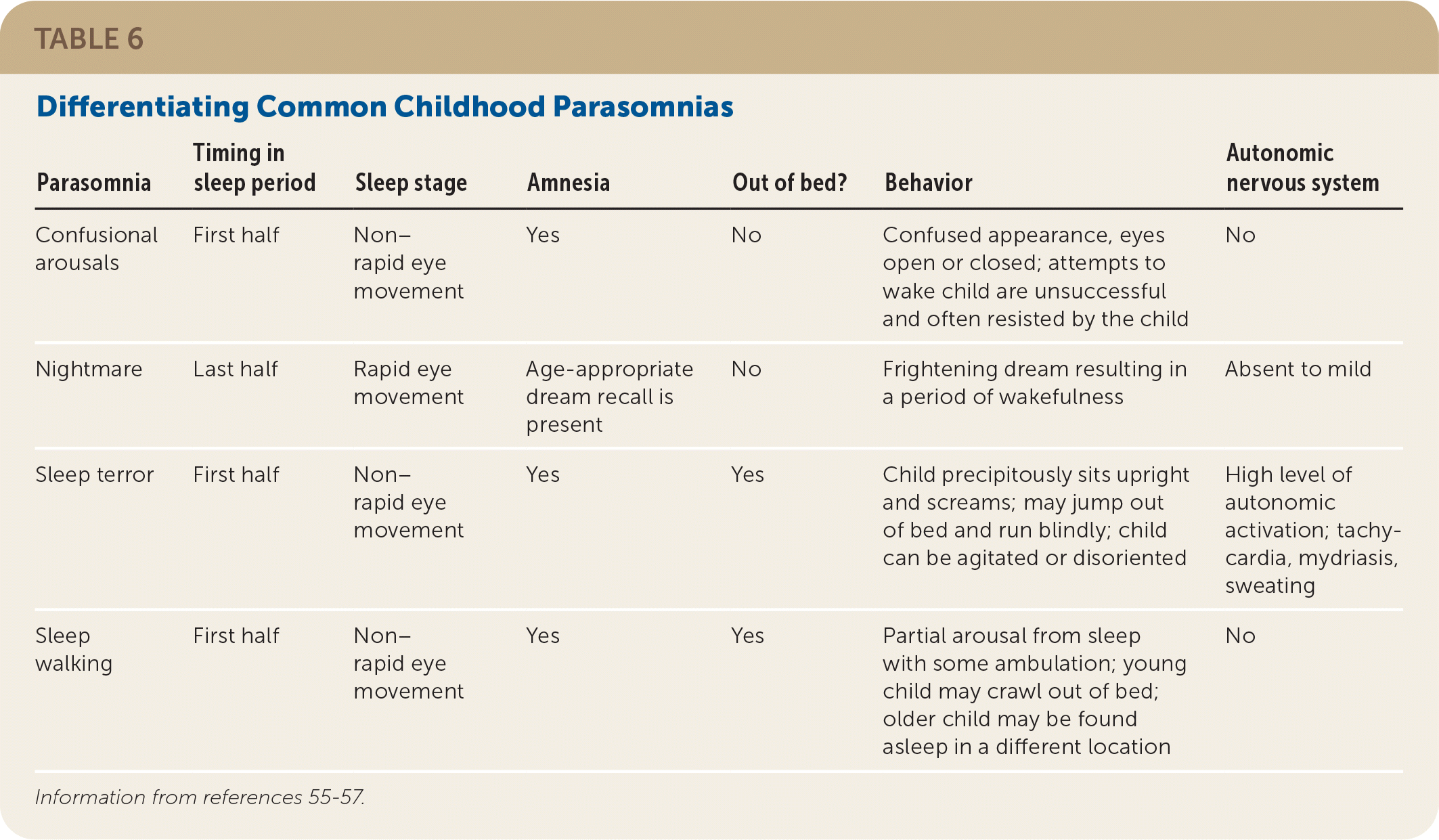
During sleep-wake transitions, parasomnias manifest as complex, sometimes dramatic activities that appear purposeful or automatic but do not represent meaningful interactions with the environment. The child can be difficult to arouse, appear confused, may quickly return to sleep, and may have amnesia about the episode. Parasomnias occur in the setting of genetic predisposition primed with sleep deprivation in the presence of precipitating factors (e.g., OSA, RLS, gastroesophageal reflux disease, pain, stress, external stimuli). Table 6 lists the differentiating features of common parasomnias.55–57 Children with repetitive stereotypical behaviors and posturing should be investigated for nocturnal seizures. Confusional arousals, sleep terrors, and sleepwalking are parasomnias of non–rapid eye movement sleep and occur in the first half of the sleep period. The child may sit up in bed, appear confused, scream precipitously, or leave the bed, and usually have amnesia of the event. Nightmares occur during rapid eye movement sleep, predominantly in the second half of the sleep period, with age- appropriate dream recall when awake. The diagnosis is made based on history. Polysomnography is indicated for reasons shown in Table 2.6
TABLE 6. Differentiating Common Childhood Parasomnias
| Parasomnia | Timing in sleep period | Sleep stage | Amnesia | Out of bed? | Behavior | Autonomic nervous system |
|---|---|---|---|---|---|---|
| Confusional arousals | First half | Non–rapid eye movement | Yes | No | Confused appearance, eyes open or closed; attempts to wake child are unsuccessful and often resisted by the child | No |
| Nightmare | Last half | Rapid eye movement | Age-appropriate dream recall is present | No | Frightening dream resulting in a period of wakefulness | Absent to mild |
| Sleep terror | First half | Non–rapid eye movement | Yes | Yes | Child precipitously sits upright and screams; may jump out of bed and run blindly; child can be agitated or disoriented | High level of autonomic activation; tachycardia, mydriasis, sweating |
| Sleep walking | First half | Non–rapid eye movement | Yes | Yes | Partial arousal from sleep with some ambulation; young child may crawl out of bed; older child may be found asleep in a different location | No |
Although dramatic from the parent's or caregiver's perspective, parasomnias are often self-limiting. Treatment is based on education, reassurance, and management of precipitating factors56,57 (Table 26 ). Because parasomnias may involve leaving the bed and even running, safety precautions should be taken. These include locking doors and windows, using motion alarms, removing firearms and sharp objects, clearing the floor of toys, and placing the mattress on the floor. Referral to a sleep medicine specialist is needed for children with violent behavior or injury or no response to conservative treatment.
Delayed Sleep Phase Syndrome
Delayed sleep phase syndrome is a circadian rhythm disorder in which the major sleep period is delayed by more than two hours for at least three months.58 Sleep-onset and wake-up times are both delayed, with individuals demonstrating night owl tendencies. The sleep-wake schedule is not aligned with socially acceptable schedules with this syndrome.
Delayed sleep phase syndrome is more common among adolescents, with a prevalence of 7% to 16%. Genetic factors (e.g., polymorphism in period circadian regulator 3 gene), environmental factors, including decreased morning light exposure and increased evening light exposure, exacerbate the delayed circadian phase. A family history of delayed sleep phase syndrome is reported in about 40% of cases.59
Light is the most powerful entrainer of the master circadian clock located in the suprachiasmatic nucleus.58 Light exposure before the desired bedtime (e.g., screen exposure while using social media) decreases melatonin secretion, thereby delaying the onset of sleep.60 Cues involving activities of daily living such as meals, physical activity, and bathing can help reset the circadian clock.
The diagnosis is clinical. The child and family should be encouraged to maintain a sleep diary for seven to 14 days, including weekends. Polysomnography is not required for diagnosis.
Management strategies are used to align the sleep-wake schedule to the desired pattern. Bedtime routines and wake-up times need to be practiced consistently with good sleep hygiene. Treatment rationale should be explained to establish expectations for ideal and realistic sleep-onset and offset times. Treatment options are shown in Table 2.6 Timed melatonin of 0.3 to 5 mg administered 1.5 to 6.5 hours before bedtime is recommended.61 Bright-light therapy provided in the first one to two hours after waking combined with behavior treatments may be beneficial. Sunlight exposure or a bright indoor light-emitting box with a 2,500 lux intensity for at least 30 minutes can be used. Bright light is most effective when combined with active play or exercise.62
Sleep Deprivation
Sleep deprivation is a health concern with serious consequences. Most U.S. high school students (68%) sleep seven hours or less on school nights and do not get the recommended amount of sleep.63 Children and adolescents who do not get enough sleep have a higher risk of obesity, diabetes mellitus, injuries, poor mental health, and problems with attention and behavior.9,64 Recommended sleep times are described in Table 1.6–9
This article updates a previous article on this topic by Carter, et al.6
Data Sources: A search of PubMed, the Cochrane database, Essential Evidence Plus, and the U.S. Preventive Services Task Force was conducted using key terms such as childhood/pediatric sleep-wake disorders, insomnia, parasomnia, obstructive sleep apnea, circadian rhythm/delayed sleep phase, insufficient sleep, enuresis, normal sleep, social media, and key words identifying specific conditions. Filters were used to identify literature for children from birth to 18 years. The references from the previous American Family Physician article on this topic were reviewed and included. Search dates: February 2021, March 2021, April 2021, and October 2021.

