Clinical Question
Is it possible to predict the likelihood of bacterial meningitis in children with clinically suspected meningitis?
Evidence Summary
Meningitis is a potentially life-threatening condition characterized by infection or inflammation of the central nervous system. It is classified as bacterial, viral, or aseptic. Delayed or untreated bacterial meningitis is associated with high morbidity and mortality. The incidence of bacterial meningitis in U.S. children ranges from 0.2 to 3.7 cases per 100,000. There is a strong predominance in infants younger than two months,1 likely because of the initiation of Haemophilus influenzae type B and pneumococcal vaccines at two months of age. Because an estimated 11% to 28% of meningitis cases are bacterial,2,3 it is important to accurately distinguish between bacterial and nonbacterial meningitis. Most physicians will perform a lumbar puncture and consider antibiotics for all infants and children with suspected meningitis. Having a clinical prediction rule to determine the need for lumbar puncture and which patients need antibiotics could reduce morbidity and the cost associated with unnecessary procedures and treatment.
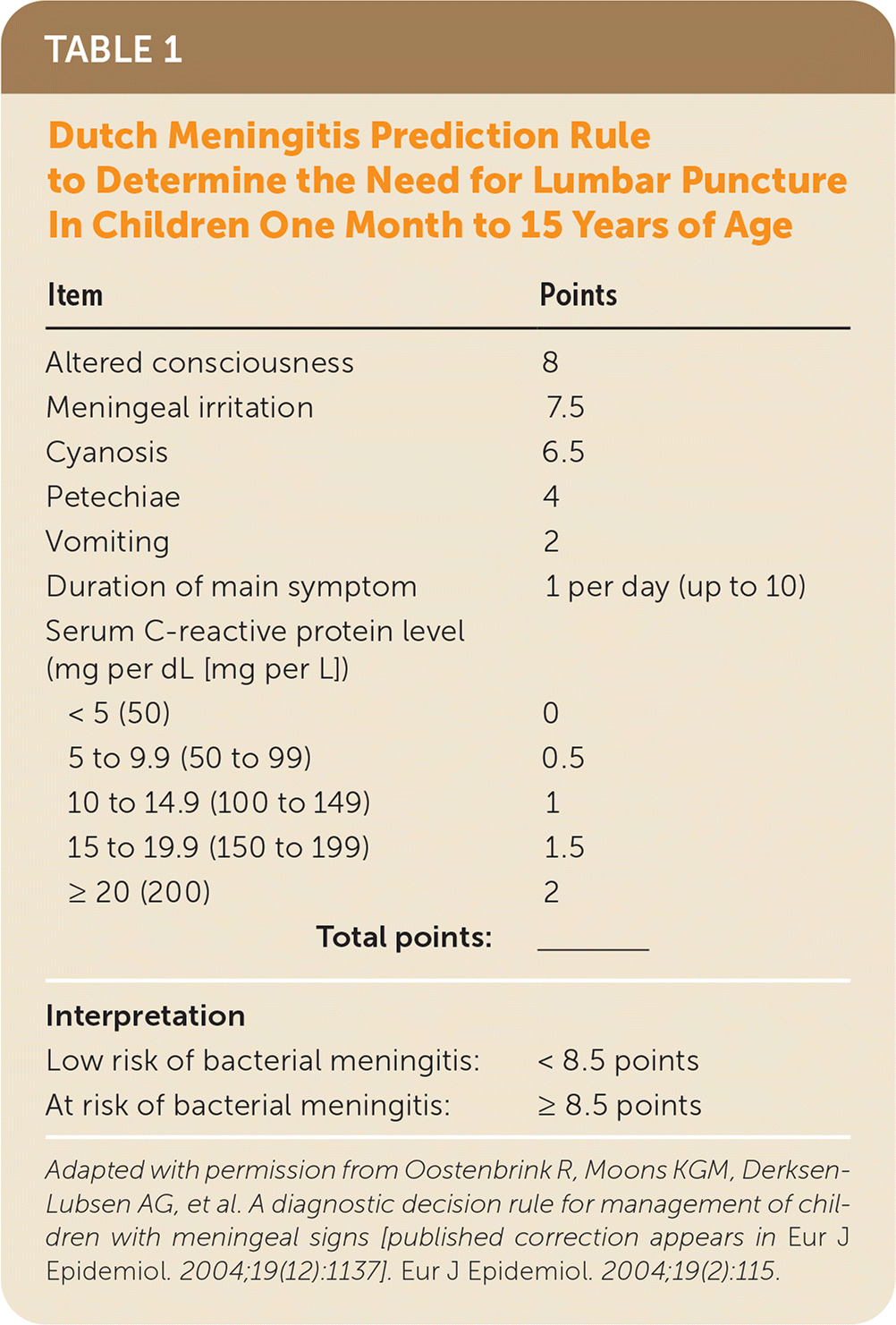
Several clinical prediction rules to determine the risk of bacterial meningitis have been proposed. One clinical prediction rule, derived and validated from cohorts seen in pediatric hospitals in the Netherlands, found that altered consciousness, meningeal irritation, cyanosis, petechiae, vomiting, duration of main symptom, and an elevated C-reactive protein level were independent predictors of bacterial meningitis (Table 1).2 Patients below a predefined threshold on a risk score incorporating these elements could be safely considered as not having bacterial meningitis (observed cases of bacterial meningitis = 0; 95% CI, 0 to 2), rendering a lumbar puncture unnecessary.2
TABLE 1. Dutch Meningitis Prediction Rule to Determine the Need for Lumbar Puncture In Children One Month to 15 Years of Age
| Item | Points |
|---|---|
| Altered consciousness | 8 |
| Meningeal irritation | 7.5 |
| Cyanosis | 6.5 |
| Petechiae | 4 |
| Vomiting | 2 |
| Duration of main symptom | 1 per day (up to 10) |
| Serum C-reactive protein level (mg per dL [mg per L]) | |
| < 5 (50) | 0 |
| 5 to 9.9 (50 to 99) | 0.5 |
| 10 to 14.9 (100 to 149) | 1 |
| 15 to 19.9 (150 to 199) | 1.5 |
| ≥ 20 (200) | 2 |
| Total points: | ________ |
| Interpretation | |
| Low risk of bacterial meningitis: | < 8.5 points |
| At risk of bacterial meningitis: | ≥ 8.5 points |
Adapted with permission from Oostenbrink R, Moons KGM, Derksen-Lubsen AG, et al. A diagnostic decision rule for management of children with meningeal signs [published correction appears in Eur J Epidemiol. 2004;19(12):1137]. Eur J Epidemiol. 2004;19(2):115.
A group based in the United States created the Bacterial Meningitis Score to determine which children with cerebrospinal fluid (CSF) pleocytosis diagnosed by lumbar puncture require antibiotic treatment. This score relies on CSF Gram stain; presence of seizure; and elevations in CSF absolute neutrophil count, C-reactive protein level, and peripheral blood absolute neutrophil count. In a meta-analysis of validation studies, the rule was found to have a sensitivity of 99.3%, specificity of 62%, negative predictive value of 99.7%, and negative likelihood ratio of 0.01 in a symptomatic population with an overall risk of bacterial meningitis of 23%.3
With the advent of additional biomarkers for serious infection, a group in Spain created an updated clinical prediction rule for children two months to 14 years of age using retrospectively collected data from a derivation population of 819 patients seen in pediatric emergency departments. Patients were excluded if they were critically ill, had purpura, or had been treated with antibiotics in the 72 hours before lumbar puncture.
The Meningitis Score for Emergencies incorporates procalcitonin, C-reactive protein, CSF absolute neutrophil count, and CSF protein (Table 2).4 Admission and antibiotics are recommended for all children with CSF pleocytosis who have any of these findings. Alternatively, well-appearing, previously healthy children with a score less than 2 may be candidates for discharge without antibiotics if close outpatient follow-up can be arranged. Using prospectively collected data from a validation population of 190 patients, the group found the tool had a sensitivity of 100% (95% CI, 89% to 100%), specificity of 77.4% (95% CI, 70% to 83%), and negative predictive value of 100% (95% CI, 97% to 100%) with no missed cases. Two patients with bacterial meningitis were missed by the Bacterial Meningitis Score but were correctly found to have bacterial meningitis by the validated Meningitis Score for Emergencies.4 Potential limitations for this rule include an all-Spanish cohort and the relatively small validation cohort.
TABLE 2. Meningitis Score for Emergencies for Children Two Months to 14 Years of Age

| Predictor | Points | |
|---|---|---|
| Present | Absent | |
| Serum procalcitonin > 1.20 ng/mL | 3 | 0 |
| Serum CRP > 40 mg/L | 1 | 0 |
| CSF ANC > 1000/μL | 1 | 0 |
| CSF protein > 80 mg/dL | 2 | 0 |
ANC = absolute neutrophil count; CRP = C-reactive protein; CSF = cerebrospinal fluid.
Reprinted with permission from Mintegi S, García S, Martín MJ, et al.; Meningitis Group of the Spanish Society of Pediatric Emergencies. Clinical prediction rule for distinguishing bacterial from aseptic meningitis. Pediatrics. 2020;146(3):e20201126.
Applying the Evidence
A previously healthy four-year-old child in the emergency department has been running a fever and has had neck pain and vomiting for one day. On examination, the child is normotensive and has no focal neurologic deficits or purpura, but does have meningismus (Dutch prediction rule score of 8.5, indicating the need for lumbar puncture). You perform serology studies and perform a lumbar puncture. The child’s serum procalcitonin level is less than 0.1 ng per mL, C-reactive protein level is 0.40 mg per dL (4 mg per L), CSF absolute neutrophil count is 200 per μL, and CSF protein level is 40 mg per dL. You calculate the Meningitis Score for Emergencies as 0. You provide the parent with precautions and send the patient home without antibiotics and schedule follow-up for the following day in the clinic.
Editor’s Note: Dr. Saguil is a contributing editor for AFP.
The views expressed are those of the authors and do not reflect the official policy or position of the Uniformed Services University of the Health Sciences, the Department of the Army, the Department of Defense, or the U.S. government.

