Child maltreatment is a devastating type of adverse childhood experience that encompasses neglect and emotional, physical, and sexual abuse (including sex trafficking). Adverse childhood experiences are exposures to maltreatment or household dysfunction during crucial developmental periods that disrupt neurodevelopment and can result in lifelong physical and psychological harm, altering the child's behavior and disease risk into adulthood. Maltreatment can affect patients of any gender identity and from all racial and ethnic backgrounds, socioeconomic statuses, and community settings. Use of the validated five-item Pediatric Hurt-Insult-Threaten-Scream-Sex screening tool to identify victims of child abuse is recommended. All suspected cases of child abuse must be reported to Child Protective Services. A trauma-informed approach to care requires that team members be mindful of the potential for traumatic stress, recognize and appropriately respond to the symptoms and signs of trauma, and prevent retraumatization. Prevention through education and anticipatory guidance provided during routine well-child visits and community partnerships can foster awareness and resiliency in children. Although caring for victims of child maltreatment may be among the most challenging professional situations encountered by physicians, advocating for these endangered patients can save lives and help prevent revictimization and chronic sequelae associated with adverse childhood experiences.
The U.S. Department of Health and Human Services defines child maltreatment as “any recent act or failure to act on the part of a parent or caretaker which results in death, serious physical or emotional harm, sexual abuse or exploitation; or an act or failure to act, which presents an imminent risk of serious harm.”1 Child maltreatment is a type of adverse childhood experience. These involve exposures to maltreatment or household dysfunction during crucial developmental periods that can have profound impacts on physical, neurologic, and intellectual development (Table 1).2–4 These impacts may then result in negative and enduring effects on health and behavior in a compounding manner.5 Risk factors and protective elements for victimization and perpetration of child maltreatment can be framed in terms of the child, the caregiver or abuser, and the environment (Table 2).1,6
SORT: KEY RECOMMENDATIONS FOR PRACTICE
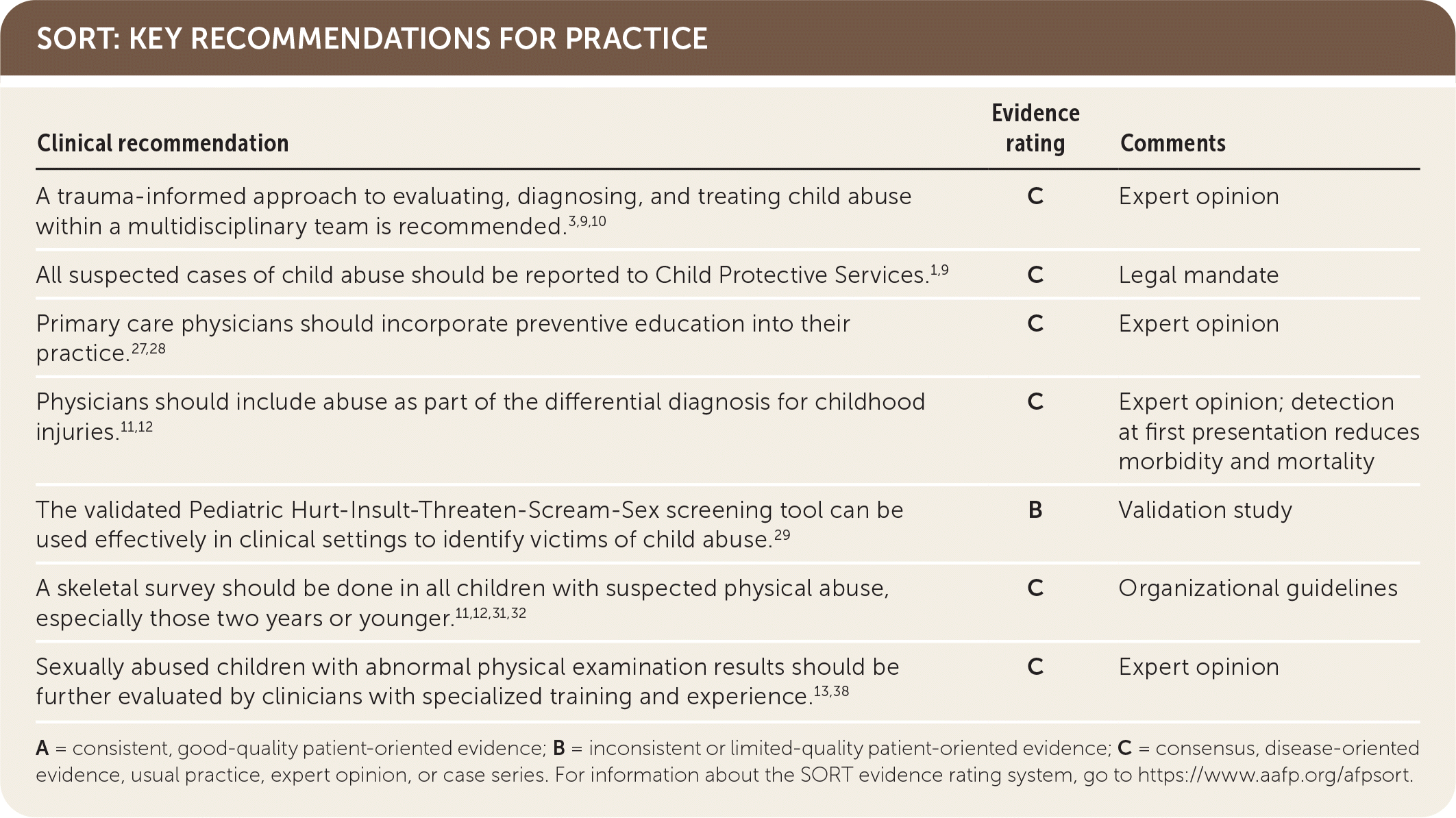
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
TABLE 1. Potential Sequelae of Adverse Childhood Experiences Due to Child Maltreatment

| Effects | Examples* |
|---|---|
| Health-risk behaviors | High-risk sexual behaviors, revictimization, sexually transmitted infections, substance abuse, suicidal ideations or attempts, unplanned pregnancies |
| Medical conditions | Fibromyalgia, irritable bowel syndrome, obesity |
| Psychological conditions | Anxiety, depression, posttraumatic stress disorder |
*—The compilation of these conditions may result in early death.
TABLE 2. Risk Factors for Child Maltreatment and Protective Factors for Recovery

| Source | Risk factors | Protective factors |
|---|---|---|
| Child | Chronic illness Emotional or behavioral difficulties Physical disabilities Preterm birth Unplanned or unwanted pregnancy | Above average cognitive ability Belief in one's ability to control own destiny External attribution of blame High degree of impulse control and modulation High self-esteem or sense of self-worth Presence of spirituality |
| Caregiver(s) | Alcohol or other substance abuse Criminal history Depression or other mental illness Development of unrealistic expectations for the child History of abuse Low educational attainment Low self-esteem Negative perception of normal childhood behavior Poor impulse control Poor knowledge of the child Young parental age | Caregiver resilience Caregiver social support network |
| Home environment | Family or intimate partner violence Non–biologically related adult living in the home Single-parent home | Presence of caring and supportive adult |
| Community environment | Poverty Social isolation or lack of social support | Access to good health, education, and social welfare services Caring adult in school or extracurricular activities Involvement with extracurricular activities or hobbies Involvement with religious community Structured school environment |
Maltreatment can affect patients of any gender identity and from all racial and ethnic backgrounds, socioeconomic statuses, and community settings. The actual number of maltreated children is challenging to track because of a lack of consistent reporting and difficulty confirming suspicions. The prevalence of maltreatment varies by type, gender, and geographic location.7 Approximately 4.4 million children are reported to Child Protective Services (CPS) each year, and about nine out of 1,000 children in the United States have evidence of maltreatment after investigation.8
Being vigilant for possible child maltreatment, knowing how to assess for and report it, and remaining adept at providing a trauma-informed approach to care9,10 (Table 33,11–13 ) within a multidisciplinary team can help optimize patient care. The principles of trauma-informed care require the health care team to realize the widespread impact of trauma, recognize and appropriately respond to signs and symptoms of trauma, and actively prevent retraumatization in their patients.14
TABLE 3. Elements of Trauma-Informed Care to Incorporate While Interviewing and Examining Patients for Suspected Child Abuse

| General |
| Preview chart, if available, for documentation regarding trauma to prevent revictimization by asking the patient to completely repeat this history |
| Remain seated to prevent the perception of a patient-physician power differential |
| Discuss the importance of confidentiality, trust, safety, and holistic care and expectations for the encounter (i.e., history with detailed note taking, comprehensive physical examination, and procedures, laboratory testing, imaging, and referrals as clinically indicated) |
| Ask open-ended questions in a nonjudgmental manner and explain medical rationale for asking sensitive questions (e.g., sexual and substance use histories) |
| If using an interpreter, inquire about cultural and gender preferences |
| Key history components |
| Developmental, medical, surgical, social, and family histories (especially with relation to genetic, metabolic, hematologic, and bone disorders) |
| Familial disciplinary methods, the child's baseline temperament and demeanor, and biopsychosocial stressors affecting the family |
| History of child, sibling, and parental/caregiver trauma |
| History of parental/caregiver substance abuse, incarcerations, arrests, intimate partner violence, behavioral health conditions, and previous or current Child Protective Services or law enforcement involvement with the patient's family |
| Maternal pregnancy and behavioral health histories |
| Physical examination |
| Consider referral to a medical forensic professional or child abuse team before performing an examination |
| Ensure presence of a chaperone |
| Ask the child if they are anxious about any components of the examination, and if there is anything that you can do to improve their comfort |
| Discuss that they can dictate the pace of the examination |
| Provide children with gowns and drapes for the examination |
| Judiciously expose and cover bodily areas (ask the patient to do so, if able, to promote personal empowerment) during examination to maximize privacy |
| Use age-appropriate language and ask permission to proceed with increasingly sensitive portions of the examination |
| Offer suggestions about how to potentially improve patient comfort while the examination is being performed (e.g., it may be helpful to take a deep breath during this portion of the examination) |
| Verbalize what is intended to be visualized and why |
| Discuss any invasive procedures (e.g., speculum examinations) in detail, obtain consent, and describe to the patient what they might experience (e.g., hearing a click with speculum opening) |
| Avoid performing repetitive anogenital examinations as able to prevent retraumatization |
Types of Abuse
All suspected cases of child abuse must be reported to CPS.1,9,10 Major categories of abuse include neglect, and emotional, physical, and sexual abuse.
NEGLECT
Neglect consists of parental omissions in care that result in actual or potential harm to a child.1,15 It is the most common form of child maltreatment, occurring as the only offense in 61% of all cases of confirmed maltreatment and in combination with abuse in 15% of cases.16 Additionally, it accounts for 73% of child fatalities caused by maltreatment.16
Neglect occurs when a child's basic physical, emotional, educational, or medical needs are not adequately met in a consistent pattern.1,15 Physical neglect involves exposure to environmental hazards that could lead to injuries or harmful ingestions, or a failure to provide adequate hygiene, nutrition, clothing, or shelter.1,15,17 Inadequate supervision is a subtype of physical neglect that includes abandonment and expulsion.1,15,17 Medical neglect results from refusing or delaying necessary health care.1,9,15,17 Emotional neglect involves inadequate nurturing or affection, an exposure to intimate partner violence, permitted drug or alcohol abuse, or refusing or delaying necessary psychological care.1,15,17 Educational neglect includes a failure to enroll a child in school, truancy, or inattention to special education needs.15,17
Manifestations of the subtypes of neglect overlap and can include malnourishment or failure to thrive, advanced medical or dental disease, developmental delays, attention-deficit/hyperactivity disorder, and alcohol or drug abuse, all of which can cause long-term intellectual, social, and psychological deficits.15,17,18 Assessment of suspected neglect involves taking a detailed medical and psychosocial history (i.e., growth, immunization status, previous hospitalizations, family stressors, and past contact with CPS) and performing a thorough physical examination.15 Additional guidance is provided in Table 33,11–13 and Table 4.11,19 Evaluations should also include screening for contributing factors (e.g., poverty, food insecurity, lack of transportation, lack of health care access, language barriers, low health literacy). Screening tools are listed in eTable A. Referral to appropriate community resources is warranted when concerns are identified.9,15,18 Home visitation programs have been shown to reduce the incidence of maltreatment in high-risk families.20–22 CPS referrals are indicated when assistance has been offered and refused, and the child's needs have been left unmet.15
TABLE 4. Differential Diagnoses of Physical Abuse

| Injury | Differential diagnoses |
|---|---|
| Bite marks | |
| Abrasions, lacerations, or ecchymoses in an ovoid or elliptical pattern May require co-evaluation by dentist or forensic odontologist | Accidental or nonaccidental bite mark from animal or another human |
| Bruises* | |
| Age cannot be accurately determined forensically External sign of potentially severe internal injury Inflicted bruises may occur in atypical locations (e.g., behind ears, inside lips, along hard palate of mouth) Noninflicted bruises are usually notable on shins, knees, and forehead | Accidental or nonaccidental trauma, dermatologic disorders, congenital dermal melanocytosis, Henoch-Schönlein purpura, genetic disorders (e.g., Ehlers-Danlos syndrome), vascular or hematologic disorders |
| Burns | |
| Object contact burns Scalding immersion burns | Accidental or nonaccidental burn, dermatitis, skin infection, Stevens-Johnson syndrome, toxic epidermal necrolysis |
| Fractures | |
| Commonly identified on skeletal radiographs Improved detection with repeated imaging | Accidental or nonaccidental fracture, birth trauma, congenital syphilis, leukemia, osteogenesis imperfecta, osteomyelitis, physiologic changes, vitamin deficiencies |
| Head trauma | |
| Associated with abuse-related fatalities Recommend co-assessment by ophthalmologist | Accidental or nonaccidental trauma, birth trauma, hemorrhagic disease, infection, intracranial vascular anomalies, metabolic disease |
*—TEN-4 mnemonic (Torso, Ears, Neck; and any infant younger than four months or child younger than four years) helps identify bruises likely associated with abuse.
eTABLE A Helpful Resources Regarding Child Maltreatment

EMOTIONAL ABUSE
The Child Abuse Prevention and Treatment Act defines psychological maltreatment as repeated patterns of caregiver behavior or extreme incidents that convey to children that they are worthless, flawed, unloved, unwanted, endangered, or only of value in meeting another's needs.4,23 Also known as emotional abuse, this subtype may be widely prevalent but is difficult to detect because of a lack of physical findings and difficulty discerning when suboptimal parenting becomes maltreatment.24 Even though emotional abuse is generally present when other forms of abuse are identified, only 8% of victims substantiated by CPS are confirmed to have experienced emotional abuse in isolation.1 Harmful parental behaviors are varied and include spurning, terrorizing, rejecting, isolating, exploiting, corrupting, denying emotional responsiveness, demonstrating unreliability or inconsistency, verbally assaulting, overpressuring, and neglecting emotional needs.4,23,24
Indicators that may warrant an evaluation include attention problems, violent or oppositional behaviors, difficulty with attachment or impaired social skills, developmental or educational delays, depression, anxiety, or physical manifestations (e.g., psychosocial short stature or failure to thrive).1,4,24,25 During the assessment, it is important to include specific quotes from both parent and child to document observations and substantiate claims.4,24 Reports from a child's school, childcare workers, or other professionals involved with the family can help guide management.4
The response to emotional abuse depends on both intent and harm, and options include parental education, counseling, CPS referral, and potentially removing the child from their home.23 Trauma-specific psychotherapy with an emphasis on cognitive behavior therapy or other behavioral therapies can provide benefit; psychopharmacologic intervention as a temporary adjunct may be useful to modulate specific symptoms such as difficulty sleeping, nightmares, and anxiety.1,25,26 Although the U.S. Preventive Services Task Force found insufficient evidence to balance the benefits and harms of primary care interventions, the American Academy of Family Physicians still endorses the provision of developmentally appropriate anticipatory guidance and preventive education, and instructions on healthy parenting approaches during well-child visits.27,28 Participation in parenting training programs (e.g., Triple-P: Positive Parenting Program) and educational home visitation programs (e.g., Nurse-Family Partnership) may be indicated when risk factors are present (Table 2).1,6
PHYSICAL ABUSE
Physical abuse encompasses any nonaccidental physical injury (e.g., biting, striking, burning, kicking) or action that results in the physical impairment of a minor.1 The most common types of injuries include bruises, burns, bite marks, fractures, and head trauma1; further details are available in Table 411,19 and eTable A. When a child presents with an injury, the potential for nonaccidental trauma should always remain in the differential diagnosis, because earlier detection of nonaccidental trauma can reduce morbidity and mortality.12 Using the validated five-item Pediatric Hurt-Insult-Threaten-Scream-Sex screening tool to identify victims of child abuse and taking a trauma-informed approach to care are recommended.3,29,30 The Pediatric Hurt-Insult-Threaten-Scream-Sex questionnaire assesses on a scale from 0 to 5 how often an immediate family member was estimated to have physically hurt, insulted, threatened, screamed or cursed at, or forced sexual acts on a child 12 years or younger within the past year; higher scores indicate an increased exposure to abuse.29
After ensuring that the child is hemodynamically stable, the clinician should obtain a comprehensive history from the patient (if able, based on language capabilities) and caregivers, preferably separately, using a nonaccusatory and sensitive manner with a focus on open-ended questions to create a safe environment and develop a trusting rapport. It is important to note details about the timing and mechanism of injury, symptom onset and progression, the child's behavior at baseline, any changes in behavior during and after the injury, and the child's demeanor both with and without the caregiver present. Vague and inconsistent explanations, denials of injury, and excessive delays in obtaining medical care may indicate abuse.11,12 Additional useful information to obtain during this trauma-informed assessment is included in Table 3.3,11–13
In all children presenting with injuries, physical examination findings should be evaluated carefully in the context of their developmental levels, mechanisms of injury, histories, and laboratory and imaging findings. Isolated injuries are rarely pathognomonic for child abuse. Resources that can help clinicians identify suspicious injuries are included in eTable A. Injuries should be distinguished as either noninflicted/unintentional or inflicted/intentional. Inflicted injuries can be further classified as sentinel injuries (i.e., minor injuries that are detected before the recognition of child abuse) and defensive injuries (i.e., those sustained in self-defense, such as on the forearms). Signs of potential abuse include injuries that are unexplained, patterned, involving more than one organ system, in various stages of healing, in an atypical location (e.g., on the ears, neck, and face), or involving a preambulatory infant.11,12
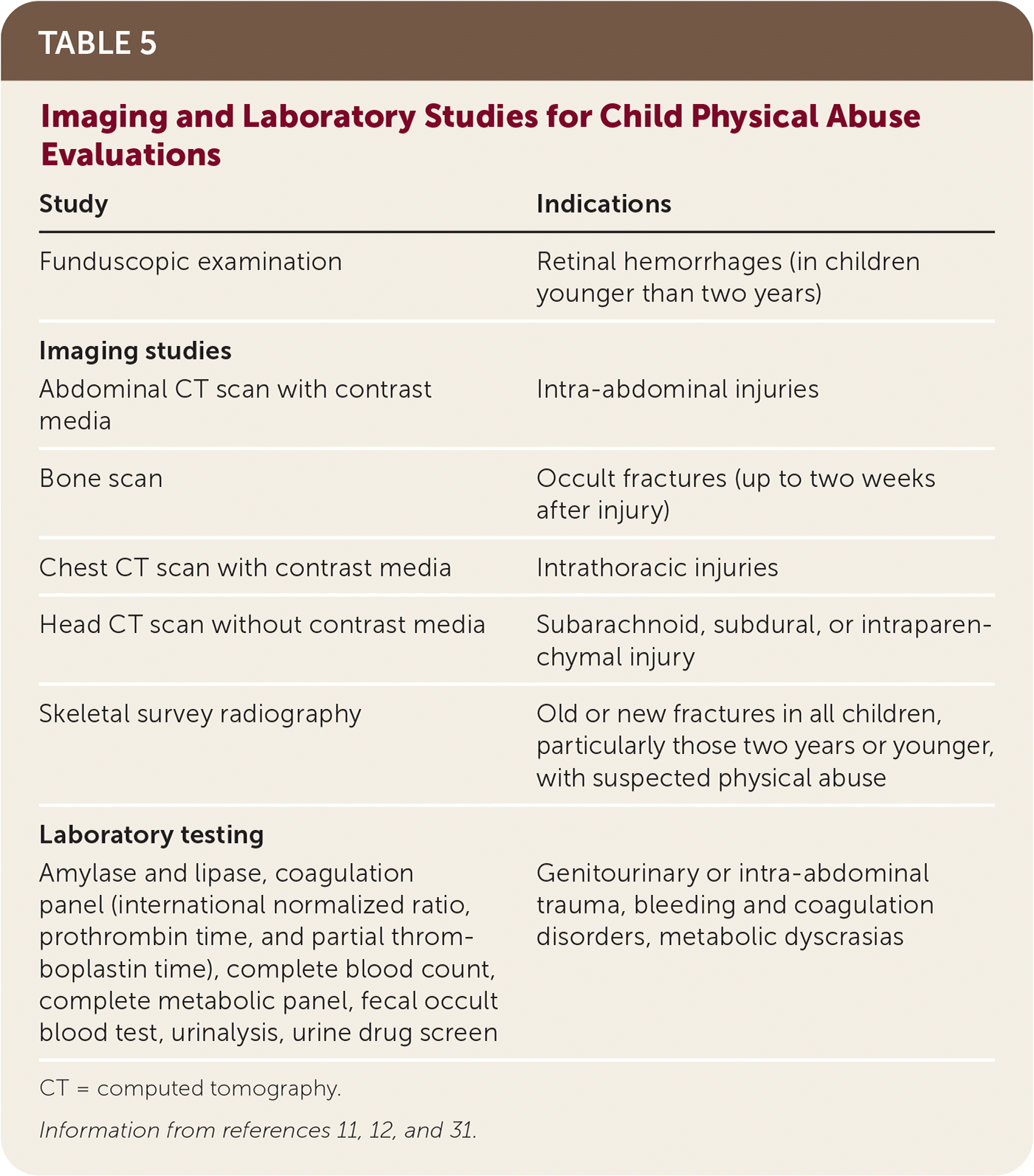
Imaging and laboratory studies are typically indicated to further investigate physical examination findings (Table 511,12,31 ). Per guidelines from the American Academy of Pediatrics and American College of Radiology, a skeletal survey should be performed in all children with suspected physical abuse, especially those two years or younger.11,12,31,32 Comprehensive and detailed documentation is essential, and the inclusion of body diagrams and confidential forensic photographs may be useful to supplement the medical record, especially if requested to provide a court testimony or if records undergo a peer review13 (eTable A). Additionally, it is important to maintain a chain of custody with law enforcement or CPS that chronologically records the movement of medical documentation and other evidence from the assessment. Elements that have potential evidentiary value include sterile swabs and items of clothing containing biologic materials (e.g., saliva, blood, semen).
TABLE 5. Imaging and Laboratory Studies for Child Physical Abuse Evaluations
| Study | Indications |
|---|---|
| Funduscopic examination | Retinal hemorrhages (in children younger than two years) |
| Imaging studies | |
| Abdominal CT scan with contrast media | Intra-abdominal injuries |
| Bone scan | Occult fractures (up to two weeks after injury) |
| Chest CT scan with contrast media | Intrathoracic injuries |
| Head CT scan without contrast media | Subarachnoid, subdural, or intraparenchymal injury |
| Skeletal survey radiography | Old or new fractures in all children, particularly those two years or younger, with suspected physical abuse |
| Laboratory testing | |
| Amylase and lipase, coagulation panel (international normalized ratio, prothrombin time, and partial thromboplastin time), complete blood count, complete metabolic panel, fecal occult blood test, urinalysis, urine drug screen | Genitourinary or intra-abdominal trauma, bleeding and coagulation disorders, metabolic dyscrasias |
CT = computed tomography.
SEXUAL ABUSE
Sexual abuse represents a significantly underreported public health crisis that is associated with an array of potentially lifelong biopsychosocial manifestations. According to the Centers for Disease Control and Prevention, an estimated one in four girls and one in 13 boys are sexually abused during childhood, and the perpetrators are known by the child or the child's family in about 90% of cases.33 Additionally, sex trafficking of minors is an underestimated form of child sexual abuse that can involve the recruitment, provision, transportation, harboring, and solicitation of persons younger than 18 years in exchange for commercial sex acts. Victims may be children of all ages, races and ethnicities, gender identities, and socioeconomic backgrounds within rural, suburban, and urban communities in the United States and abroad.34 Table 6 lists psychosocial warning signs and physical features to look for in victims or their traffickers during an office visit.35,36
TABLE 6. Identifying Features of Child Sex Trafficking

| Psychosocial warning signs | Physical warning signs |
|---|---|
| Claim that the patient is “just visiting the area” Display of emotional distress (e.g., depression, anxiety, low self-esteem) Dominating or controlling adult in room with patient Family dysfunction, abuse in the home, neglect or absence of a caregiver Involvement with several sex partners Lack of identification (e.g., driver's license) Multiple foster home or group home placements Prior record of arrest for prostitution Relationship with an older adult Repeated attempts to run away from home Restricted or controlled communication Sex industry association Use of slang relating to street work Victim in crisis, but downplaying health problems or risks Victim resisting help because of fear | Atypical behavior (e.g., caused by traumatic brain injury) Branding (e.g., tattoos with a name or initials) Discrepancy between apparent and reported age (e.g., clues in behavior and appearance) Inappropriate dress Injuries around the head or mouth Multiple visits for sexually transmitted infections Presence of unexplained scars, scar tissue, or bruises Signs of drug use, substance abuse, or intoxication Signs of having intercourse while masking menses (e.g., retained cotton balls, tampons, and makeup sponges in the vaginal canal) Signs of malnourishment Signs of self-inflicted injuries or suicide attempts Signs of sexual trauma Vaginal wall thinning or tearing |
Once the potential for child sexual abuse or sex trafficking is suspected, a physician's priorities comprise the following: (1) a safety assessment of the child's home environment (i.e., inquiring if the child is safe to return home, at risk of sustaining additional maltreatment in response to disclosing abuse, or at risk of being reexposed to a suspect at home), (2) the physician's professional duty to report suspected cases of abuse to appropriate government agencies, (3) a comprehensive evaluation of the child's mental and physical health, and (4) the possible need for a medical forensic examination (especially if patients present within 72 hours of an act of sexual abuse to obtain biologic specimens that could potentially have evidentiary value via rape/sexual assault kits) by referral to trained medical forensic professionals or transfer to a higher level of care (e.g., an emergency department, a child advocacy center, an abuse assessment clinic).11,13
When assessing children who may have been sexually abused, it is important to differentiate between normal and abnormal sexual behaviors. eTable A provides examples of ways to distinguish these behaviors in children up to 12 years of age. Many sexual behaviors that are considered normal increase in frequency and variety up until five years of age and wane afterwards.37 Notably, children with developmental delays may have different expectations of normal and abnormal sexual behaviors.
The aforementioned principles of assessing victims of physical abuse in a trauma-informed manner also apply to victims of sexual abuse. For female victims of sexual assault, a speculum examination is recommended in pubertal and postpubertal girls, but it is usually contraindicated in prepubertal children. For male and female victims, digital rectal and anoscopic examinations usually are not indicated. Sexually abused children with abnormal physical examination results should be further evaluated by clinicians with specialized training and experience.13,38 Medical examinations and records from all victims of sexual trauma should, ideally, be further reviewed by an experienced physician with medical forensic–related training.13,19,38
Of note, many victims of sexual abuse have anogenital examinations that appear normal, and a negative examination cannot disprove the occurrence of sexual trauma. These patients should be screened for sexually transmitted infections (i.e., HIV, syphilis, gonorrhea, chlamydia, and trichomoniasis). They can also be tested for bacterial vaginosis and vaginal candidiasis. Patients should receive treatment for any detected sexually transmitted infections and be offered emergency contraception and HIV postexposure prophylaxis.13,38
Once the occurrence of childhood sexual trauma is divulged, it can trigger distressing and emotionally charged responses throughout the child's support system. Physicians should remain vigilant for these responses and provide caregivers with anticipatory guidance, education, and resources for behavioral health services (especially those that specialize in childhood trauma) and child advocacy facilities. Parents are encouraged to support and believe their children, respond in a protective and calm manner, reassure their children that they are not at fault, and ensure close follow-up with their children's medical and behavioral health professionals.11,13
Although the various types of child maltreatment may have nuances in their presentations, there are similarities in many aspects of diagnosis and treatment. Physicians should use a trauma-informed approach and employ their duty to report all suspected cases of maltreatment, and the patient's medical care team should stay actively involved by facilitating access to behavioral health services and community resources.1,9,39 Strategies for preventing and managing all types of abuse and neglect, as well as helpful resources, can be found in eTable A and eTable B.
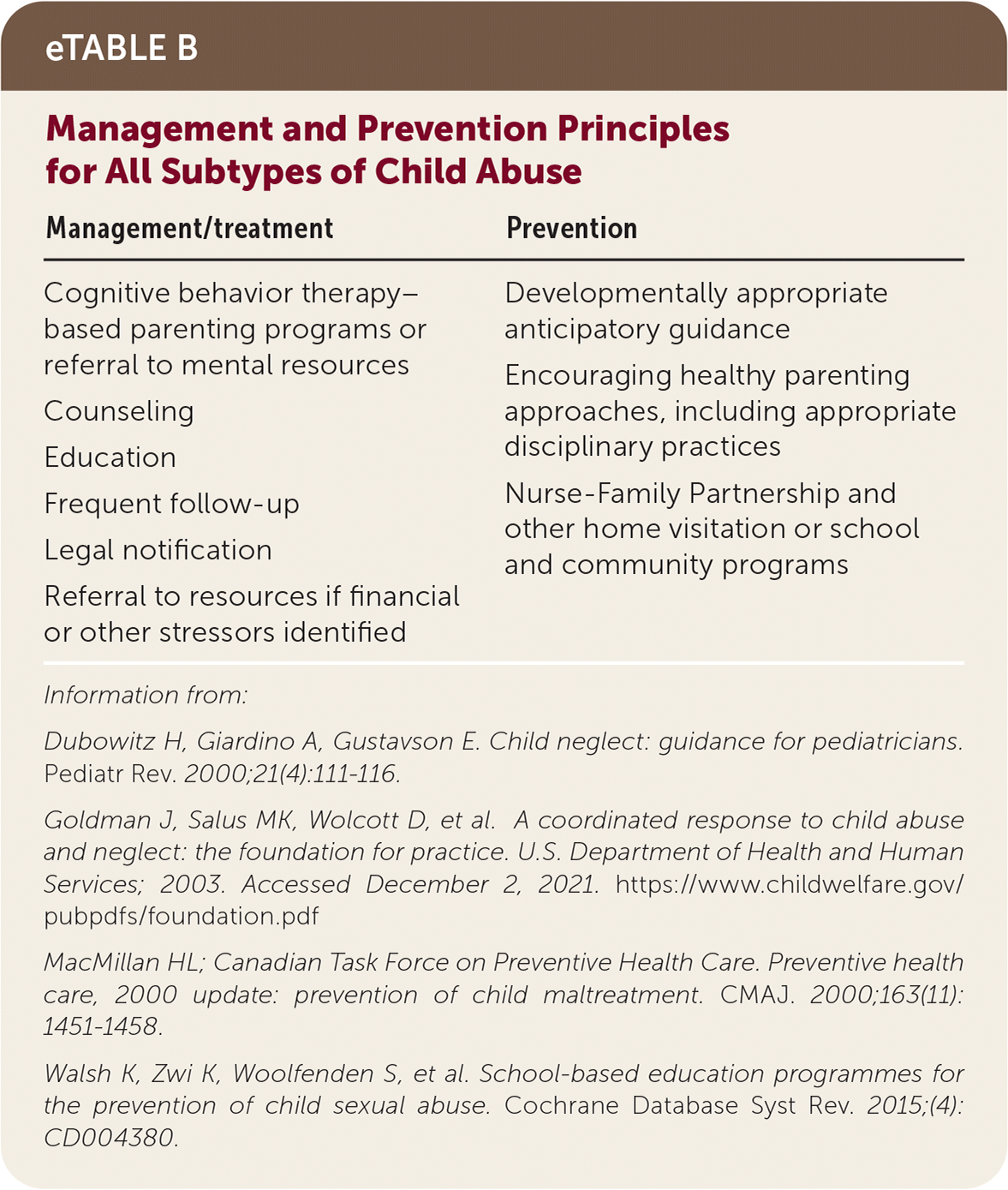
eTABLE B Management and Prevention Principles for All Subtypes of Child Abuse
| Management/treatment | Prevention |
|---|---|
| Cognitive behavior therapy–based parenting programs or referral to mental resources Counseling Education Frequent follow-up Legal notification Referral to resources if financial or other stressors identified | Developmentally appropriate anticipatory guidance Encouraging healthy parenting approaches, including appropriate disciplinary practices Nurse-Family Partnership and other home visitation or school and community programs |
Information from:
Dubowitz H, Giardino A, Gustavson E. Child neglect: guidance for pediatricians. Pediatr Rev. 2000;21(4):111–116.
Goldman J, Salus MK, Wolcott D, et al. A coordinated response to child abuse and neglect: the foundation for practice. U.S. Department of Health and Human Services; 2003. Accessed December 2, 2021. https://www.childwelfare.gov/pubpdfs/foundation.pdf
MacMillan HL; Canadian Task Force on Preventive Health Care. Preventive health care, 2000 update: prevention of child maltreatment. CMAJ. 2000;163(11):1451–1458.
Walsh K, Zwi K, Woolfenden S, et al. School-based education programmes for the prevention of child sexual abuse. Cochrane Database Syst Rev. 2015;(4):CD004380.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms “child abuse,” “physical abuse,” “physical trauma,” “sexual abuse,” “sexual trauma,” and “sex trafficking.” Search dates: February 20 and March 23, 2021. Essential Evidence Plus was also used with the search terms “child abuse” and “neglect.” Search dates: March 22, 2021, and January 7, 2022.

