Key Points for Practice
• Most states permit expedited partner therapy, including provision of packaged medications or prescriptions without evaluation, to limit the spread of STIs.
• For chlamydial infections affecting the urethra, rectum, or pharynx, doxycycline, 100 mg orally twice daily for seven days, is most effective.
• For gonorrheal infection, ceftriaxone, 500 mg intra-muscularly as a single dose, is recommended for most people, with azithromycin cotreatment no longer recommended.
• For pelvic inflammatory disease, metronidazole is added to ceftriaxone and doxycycline treatment to eradicate anaerobic organisms.
From the AFP Editors
Evidence-based prevention and treatment of sexually transmitted infections (STIs) continue to evolve. The Centers for Disease Control and Prevention (CDC) released updated recommendations for STI management. These recommendations are summarized in a point-of-care application available at https://www.cdc.gov/std/treatment-guidelines, and recommendations for providing quality STI clinical services are summarized at https://www.cdc.gov/std/qcs.
STI Prevention
Prevention efforts include preexposure vaccination for hepatitis A, hepatitis B, and human papillomavirus; provision of HIV pre- and postexposure prophylaxis; and partner services. Prevention also continues to include discussions about condom use, decreasing the number of sex partners, abstinence from intercourse during STI treatment, and emergency contraceptives.
HIV PREEXPOSURE PROPHYLAXIS
HIV preexposure prophylaxis with a daily combination of emtricitabine with tenofovir disoproxil fumarate (Truvada) is safe and effective for men who have sex with men (MSM), mixed-status heterosexual couples, and heterosexually active people at high risk due to a high number of sex partners or inconsistent or no condom use. An alternative combination of emtricitabine and tenofovir alafenamide (Descovy) has demonstrated effectiveness for MSM.
PARTNER SERVICES
Expedited partner therapy allows clinicians to treat sex partners of their patients, without seeing the partners directly, with patient-facilitated delivery of prepackaged medication or prescription. Expedited partner therapy is legal in most states, with state-specific information at https://www.cdc.gov/std/ept. Expedited partner therapy with doxycycline is appropriate for people with chlamydial infection who are uncertain whether sex partners will seek care. Although it is an alternative regimen, expedited partner therapy with single-dose cefixime (Suprax), 800 mg orally, can be used to treat sex partners of those with gonorrheal infection. The CDC recommends people diagnosed with an STI notify sex partners except in situations of intimate partner violence.
Screening Recommendations
The CDC recommends obtaining sexual histories with a nonjudgmental attitude and respectful language. STI- and HIV-focused prevention counseling is most important for adults with a recent STI diagnosis or multiple partners, as well as all sexually active adolescents. Syphilis, gonorrhea, chlamydia, chancroid, and HIV are reportable infections in every state.
SPECIAL POPULATIONS
Sexually active adolescents and young adults are at particular risk of chlamydia and gonorrhea infection and other STIs, especially those in vulnerable groups, including young MSM, transgender youth, and those with mental health conditions, multiple sex partners, early sexual experiences, or engagement in exchange sex (e.g., for money). Screening for chlamydia and gonorrhea is recommended for all females younger than 25 years, and HIV screening should be offered to all adolescents. Multiple medical societies recommend that clinicians privately assess patients' sexual behaviors and have awareness of challenges in protecting confidentiality. All states explicitly allow minors to consent for their own STI care.
Although MSM are at high risk for STIs, including HIV, some are at higher risk. Disparities research suggests that approximately one in two Black/African American and one in four Latino/Hispanic MSM acquire HIV during their lifetime. Counseling should be tailored based on assessed risk. HIV testing is recommended for patients with unknown HIV status and HIV-negative patients who have had more than one sex partner since their previous test. Routine testing for gonococcal and chlamydial infections is recommended at least annually and as frequently as every three months. Urethral testing by urine, as well as rectal and pharyngeal sampling by patient- or clinician-collected swabs, is recommended depending on sex practices. Approximately 70% of infections are missed by urogenital-only testing strategies. Hepatitis B and C testing is recommended at least once for all adults except in those at extremely low risk. Routine stool culture for enteric pathogens should be considered in MSM with diarrhea due to elevated risk.
Women who have sex exclusively with women have lower STI risk than women who have sex with women and men or exclusively with men.
Recommendations for transgender and gender-diverse people are guided by current anatomy and sexual behaviors.
During pregnancy, universal screening for HIV, syphilis, and hepatitis B is recommended, with risk-based screening for chlamydia, gonorrhea, and hepatitis C.
Given patient risk profiles, opt-out recommendations for STI screening for persons in correctional facilities and other high-risk settings are generally recommended.
STI Treatment Recommendations
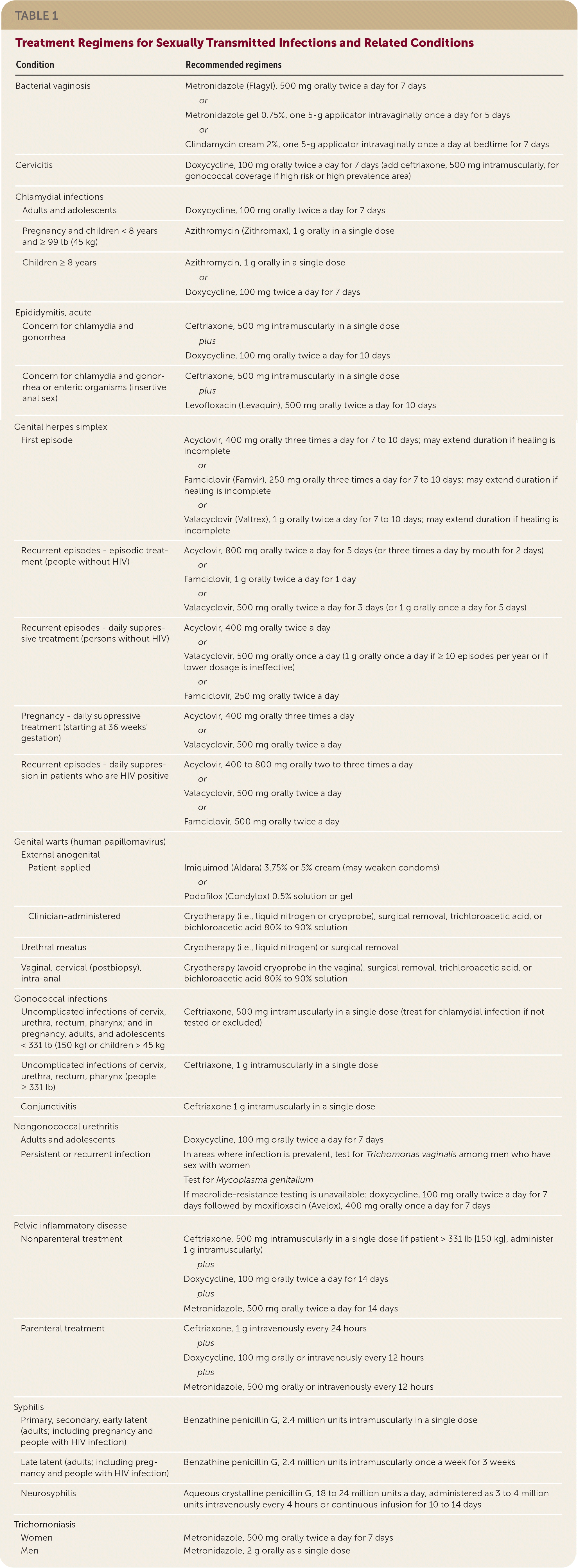
Based on recent evidence, the primary antimicrobial or dose has changed for many STIs. Table 1 lists recommended treatments.
TABLE 1. Treatment Regimens for Sexually Transmitted Infections and Related Conditions
| Condition | Recommended regimens |
|---|---|
| Bacterial vaginosis | Metronidazole (Flagyl), 500 mg orally twice a day for 7 days or Metronidazole gel 0.75%, one 5-g applicator intravaginally once a day for 5 days or Clindamycin cream 2%, one 5-g applicator intravaginally once a day at bedtime for 7 days |
| Cervicitis | Doxycycline, 100 mg orally twice a day for 7 days (add ceftriaxone, 500 mg intramuscularly, for gonococcal coverage if high risk or high prevalence area) |
| Chlamydial infections | |
| Adults and adolescents | Doxycycline, 100 mg orally twice a day for 7 days |
| Pregnancy and children < 8 years and ≥ 99 lb (45 kg) | Azithromycin (Zithromax), 1 g orally in a single dose |
| Children ≥ 8 years | Azithromycin, 1 g orally in a single dose or Doxycycline, 100 mg twice a day for 7 days |
| Epididymitis, acute | |
| Concern for chlamydia and gonorrhea | Ceftriaxone, 500 mg intramuscularly in a single dose plus Doxycycline, 100 mg orally twice a day for 10 days |
| Concern for chlamydia and gonorrhea or enteric organisms (insertive anal sex) | Ceftriaxone, 500 mg intramuscularly in a single dose plus Levofloxacin (Levaquin), 500 mg orally twice a day for 10 days |
| Genital herpes simplex | |
| First episode | Acyclovir, 400 mg orally three times a day for 7 to 10 days; may extend duration if healing is incomplete or Famciclovir (Famvir), 250 mg orally three times a day for 7 to 10 days; may extend duration if healing is incomplete or Valacyclovir (Valtrex), 1 g orally twice a day for 7 to 10 days; may extend duration if healing is incomplete |
| Recurrent episodes - episodic treatment (people without HIV) | Acyclovir, 800 mg orally twice a day for 5 days (or three times a day by mouth for 2 days) or Famciclovir, 1 g orally twice a day for 1 day or Valacyclovir, 500 mg orally twice a day for 3 days (or 1 g orally once a day for 5 days) |
| Recurrent episodes - daily suppressive treatment (persons without HIV) | Acyclovir, 400 mg orally twice a day or Valacyclovir, 500 mg orally once a day (1 g orally once a day if ≥ 10 episodes per year or if lower dosage is ineffective) or Famciclovir, 250 mg orally twice a day |
| Pregnancy - daily suppressive treatment (starting at 36 weeks' gestation) | Acyclovir, 400 mg orally three times a day or Valacyclovir, 500 mg orally twice a day |
| Recurrent episodes - daily suppression in patients who are HIV positive | Acyclovir, 400 to 800 mg orally two to three times a day or Valacyclovir, 500 mg orally twice a day or Famciclovir, 500 mg orally twice a day |
| Genital warts (human papillomavirus) | |
| External anogenital | |
| Patient-applied | Imiquimod (Aldara) 3.75% or 5% cream (may weaken condoms) or Podofilox (Condylox) 0.5% solution or gel |
| Clinician-administered | Cryotherapy (i.e., liquid nitrogen or cryoprobe), surgical removal, trichloroacetic acid, or bichloroacetic acid 80% to 90% solution |
| Urethral meatus | Cryotherapy (i.e., liquid nitrogen) or surgical removal |
| Vaginal, cervical (postbiopsy), intra-anal | Cryotherapy (avoid cryoprobe in the vagina), surgical removal, trichloroacetic acid, or bichloroacetic acid 80% to 90% solution |
| Gonococcal infections | |
| Uncomplicated infections of cervix, urethra, rectum, pharynx; and in pregnancy, adults, and adolescents < 331 lb (150 kg) or children > 45 kg | Ceftriaxone, 500 mg intramuscularly in a single dose (treat for chlamydial infection if not tested or excluded) |
| Uncomplicated infections of cervix, urethra, rectum, pharynx (people ≥ 331 lb) | Ceftriaxone, 1 g intramuscularly in a single dose |
| Conjunctivitis | Ceftriaxone 1 g intramuscularly in a single dose |
| Nongonococcal urethritis | |
| Adults and adolescents | Doxycycline, 100 mg orally twice a day for 7 days |
| Persistent or recurrent infection | In areas where infection is prevalent, test for Trichomonas vaginalis among men who have sex with women |
| Test for Mycoplasma genitalium | |
| If macrolide-resistance testing is unavailable: doxycycline, 100 mg orally twice a day for 7 days followed by moxifloxacin (Avelox), 400 mg orally once a day for 7 days | |
| Pelvic inflammatory disease | |
| Nonparenteral treatment | Ceftriaxone, 500 mg intramuscularly in a single dose (if patient > 331 lb [150 kg], administer 1 g intramuscularly) plus Doxycycline, 100 mg orally twice a day for 14 days plus Metronidazole, 500 mg orally twice a day for 14 days |
| Parenteral treatment | Ceftriaxone, 1 g intravenously every 24 hours plus Doxycycline, 100 mg orally or intravenously every 12 hours plus Metronidazole, 500 mg orally or intravenously every 12 hours |
| Syphilis | |
| Primary, secondary, early latent (adults; including pregnancy and people with HIV infection) | Benzathine penicillin G, 2.4 million units intramuscularly in a single dose |
| Late latent (adults; including pregnancy and people with HIV infection) | Benzathine penicillin G, 2.4 million units intramuscularly once a week for 3 weeks |
| Neurosyphilis | Aqueous crystalline penicillin G, 18 to 24 million units a day, administered as 3 to 4 million units intravenously every 4 hours or continuous infusion for 10 to 14 days |
| Trichomoniasis | |
| Women | Metronidazole, 500 mg orally twice a day for 7 days |
| Men | Metronidazole, 2 g orally as a single dose |
Chlamydia
Doxycycline continues to be the first-line treatment for chlamydial infections because of consistent effectiveness at urethral, rectal, and pharyngeal sites. Single-dose azithromycin (Zithromax) is now a second-line treatment because of dramatically increased treatment failure rates, especially with infection in the rectum. Rectal disease is detected in at least one of three women with urogenital infection and no anorectal sexual activity, suggesting migration of infection and highlighting the importance of prioritizing doxycycline over azithromycin for treatment.
Although a test of cure following treatment is rarely recommended because of common false-positive results, screening for reinfection three months after treatment is recommended. Repeat testing is recommended four weeks after treatment for pregnant patients; if nonadherence is suspected, if azithromycin is used for rectal infection, if symptoms persist, or if reinfection is suspected.
Gonorrhea
Ceftriaxone remains the primary treatment for gonorrheal infection, but it now warrants a single 500-mg intramuscular dose or a 1-g intramuscular dose for patients weighing 331 lb (150 kg) or more. Combination treatment with azithromycin is no longer recommended. Cotreatment for chlamydia is required if chlamydial infection is not excluded.
Even with emerging antibiotic resistance, reinfection with gonorrhea is much more likely than treatment failure, so screening for reinfection is recommended at three months. Patients with pharyngeal gonorrhea should receive a test of cure at seven to 14 days, although early testing increases false-positive results. For pharyngeal symptoms that persist three to five days after treatment, patients should be evaluated with culture to determine antibiotic susceptibility unless they have had new sexual contact and require retreatment.
Urethritis, Epididymitis, and Cervicitis
Empiric treatment of urethritis and cervicitis comprises regimens effective against gonorrhea and chlamydia. Trichomoniasis may also cause persistent infection in women or heterosexual men. If trichomonas is confirmed, treatment should include metronidazole (Flagyl), 2 g as a single dose in men or 500 mg twice daily for seven days in women. Treatment for acute epididymitis targets gonorrhea and chlamydia, unless risk factors such as insertive anal sex suggest enteric organisms.
Patients should be advised to abstain from intercourse until they and their partners complete treatment and are asymptomatic. For single-dose treatments, seven days of abstinence is recommended. Clinicians may leave an intrauterine device in place during cervicitis treatment but should delay new placement.
Patients with chlamydia, gonorrhea, or trichomonas infection should be screened for HIV and syphilis and retested in three months.
Pelvic Inflammatory Disease
Because of new short-term outcome data suggesting benefit of anaerobic organism treatment, combination treatment with metronidazole, ceftriaxone, and doxycycline is recommended for pelvic inflammatory disease. Hospitalization should be considered with pregnancy, oral medication intolerance, possible appendicitis, or tubo-ovarian abscess.
Human Papillomavirus
For those at high risk of anal cancer, the CDC recommends digital rectal examination to detect early anal cancer; data are insufficient to recommend routine anal cytology.
The quadrivalent and nonavalent vaccines protect against genital warts and cancers caused by human papillomavirus and are recommended for all people 11 through 26 years of age. Shared decision-making guides vaccination through 45 years of age. Human papillomavirus appears to be spread sexually between women who have sex with women, and vaccination reduces this risk.
Herpes Simplex Virus and Syphilis
Herpes simplex virus (HSV) and syphilis are the most common causes of genital or perianal STIs. Evaluation includes HIV testing, syphilis serology testing, and HSV nucleic acid amplification testing or culture. Syphilis testing starts with nontreponemal testing because these tests resolve after previous infection, with treponemal testing to confirm infection. HSV nucleic acid amplification testing is more sensitive and faster than culture.
Type-specific serologic testing for HSV is useful for symptoms with negative HSV nucleic acid amplification testing or culture, clinically diagnosed HSV without confirmation, or if the patient has a partner with genital herpes. Serologic testing can be falsely negative in primary HSV infection and should be repeated in 12 weeks.
The views expressed in this publication are those of the authors and do not reflect the official policy or position of the Departments of the Air Force, the Department of Defense, or the U.S. government.
Editor's Note: This is the first comprehensive update on STI recommendations from the CDC since 2015. Changes, including the clear preference of doxycycline over azithromycin for chlamydial infection and the recommendation to add metronidazole to ceftriaxone and doxycycline for pelvic inflammatory disease, differ from the most recent review of urethritis (https://www.aafp.org/afp/2021/0501/p553.html). All states allow minors to receive diagnosis and treatment of STIs without parental notification or consent and some states allow other services as well (https://www.cdc.gov/hiv/policies/law/states/minors.html). Preexposure prophylaxis recommendations for HIV are frequently refined, and the most recent include a recommendation to inform all sexually active people about preexposure prophylaxis and discuss the new option for monthly injection of cabotegravir/rilpivirine (Cabenuva) (https://www.cdc.gov/hiv/pdf/risk/prep/cdc-hiv-prep-guidelines-2021.pdf).—Michael J. Arnold, MD, Contributing Editor
Guideline source: Centers for Disease Control and Prevention
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Recommendations based on patient-oriented outcomes? Yes
Published source: MMWR Morb Mortal Wkly Rep. July 23, 2021;70(4):1–192

