This article summarizes the top 20 research studies of 2021 identified as POEMs (patient-oriented evidence that matters) that did not address the COVID-19 pandemic. Sodium-glucose cotransporter-2 inhibitors and glucagon-like peptide-1 receptor agonists prevent adverse cardiovascular and renal outcomes in patients with type 2 diabetes mellitus and also reduce all-cause and cardiovascular mortality. Most older adults (mean age, 75 years) with prediabetes do not progress to diabetes. Among patients in this age group with type 2 diabetes treated with medication, an A1C level of less than 7% is associated with increased risk of hospitalization for hypoglycemia, especially when using a sulfonylurea or insulin. For patients with chronic low back pain, exercise, nonsteroidal anti-inflammatory drugs, duloxetine, and opioids were shown to be more effective than control in achieving a 30% reduction in pain, but self-discontinuation of duloxetine and opioids was common. There is no clinically important difference between muscle relaxants and placebo in the treatment of nonspecific low back pain. In patients with chronic pain, low- to moderate-quality evidence supports exercise, yoga, massage, and mindfulness-based stress reduction. For acute musculoskeletal pain, acetaminophen, 1,000 mg, plus ibuprofen, 400 mg, without an opioid is a good option. Regarding screening for colorectal cancer, trial evidence supports performing fecal immunochemical testing every other year. For chronic constipation, evidence supports polyethylene glycol, senna, fiber supplements, magnesium-based products, and fruit-based products. The following abdominal symptoms carry a greater than 3% risk of cancer or inflammatory bowel disease: dysphagia or change in bowel habits in men; rectal bleeding in women; and abdominal pain, change in bowel habits, or dyspepsia in men and women older than 60 years. For secondary prevention in those with established arteriosclerotic cardiovascular disease, 81 mg of aspirin daily appears to be effective. The Framingham Risk Score and the Pooled Cohort Equations both overestimate the risk of cardiovascular events. Over 12 years, no association between egg consumption and cardiovascular events was demonstrated. Gabapentin, pregabalin, duloxetine, and venlafaxine provide clinically meaningful improvements in chronic neuropathic pain. In patients with moderate to severe depression, initial titration above the minimum starting dose of antidepressants in the first eight weeks of treatment is not more likely to increase response. In adults with iron deficiency anemia, adding vitamin C to oral iron has no effect. In children with pharyngitis, rhinosinusitis, acute bronchitis, or acute otitis media, providing education combined with a take-and-hold antibiotic prescription results in 1 in 4 of those children eventually taking an antibiotic.
Annually for 23 years, a team of clinicians has systematically reviewed English-language medical journals to identify the research most likely to change and improve primary care. The team includes experts in family medicine, pharmacology, hospital medicine, and women’s health.1,2
The goal of this process is to identify POEMs (patient-oriented evidence that matters). A POEM must report at least one patient-oriented outcome, such as improvement in symptoms, morbidity, or mortality. It should also be free of important methodologic bias, making the results valid and trustworthy. Finally, if the results were applied in practice, some physicians would change what they do by adopting a new practice or discontinuing an old one shown to be ineffective or harmful. Adopting POEMs in clinical practice should improve patient outcomes. Of more than 20,000 research studies published in 2021 in the journals reviewed by the POEMs team, only 260 met criteria for validity, relevance, and practice change. These POEMs are emailed daily to subscribers of Essential Evidence Plus (Wiley-Blackwell, Inc.).
The Canadian Medical Association purchases a POEMs subscription for its members, many of whom receive the daily POEM. As these physicians read each POEM, they can rate it using a validated questionnaire. This process is called the Information Assessment Method (https://www.mcgill.ca/iam). POEM ratings address the domains of clinical relevance, cognitive impact, use in practice, and expected health benefits if that POEM is applied to a specific patient.2,3 In 2021, each of the 260 daily POEMs were rated by an average of 1,189 physicians.
In this article, the 11th installment of our annual series (https://www.aafp.org/pubs/afp/content/top-poems.html), we present the 20 most clinically relevant POEMs of 2021 as determined by Canadian Medical Association members. Looking beyond COVID-19, our patients continue to face the usual (and unusual) health problems of everyday life. Thus, we summarize the clinical questions and bottom-line answers for research studies about a variety of topics that were identified as top 20 POEMs, followed by a brief discussion. This set of 20 POEMs includes the most relevant practice guidelines of the year. The full POEMs are available online at https://www.aafp.org/pubs/afp/content/top-poems/2021.html.
The five most highly rated POEMs in 2021, and eight of the top 15, were about the COVID-19 vaccines and their effectiveness in different populations. Because of the emergence of variants and widespread endorsement of the vaccine by family physicians, these POEMs are not as likely to lead to practice changes as they were when originally published. One additional COVID-19 POEM reported the incidence of myocarditis following vaccination with the Pfizer BioNTech and Moderna mRNA vaccines in U.S. military personnel. The incidence of approximately 4 more cases than expected per 100,000 patients is significantly lower than the more than 300 per 100,000 patients seen among those with SARS-CoV-2 infection.4 The rest of this article includes POEMs not related to the COVID-19 pandemic.
Type 2 Diabetes Mellitus
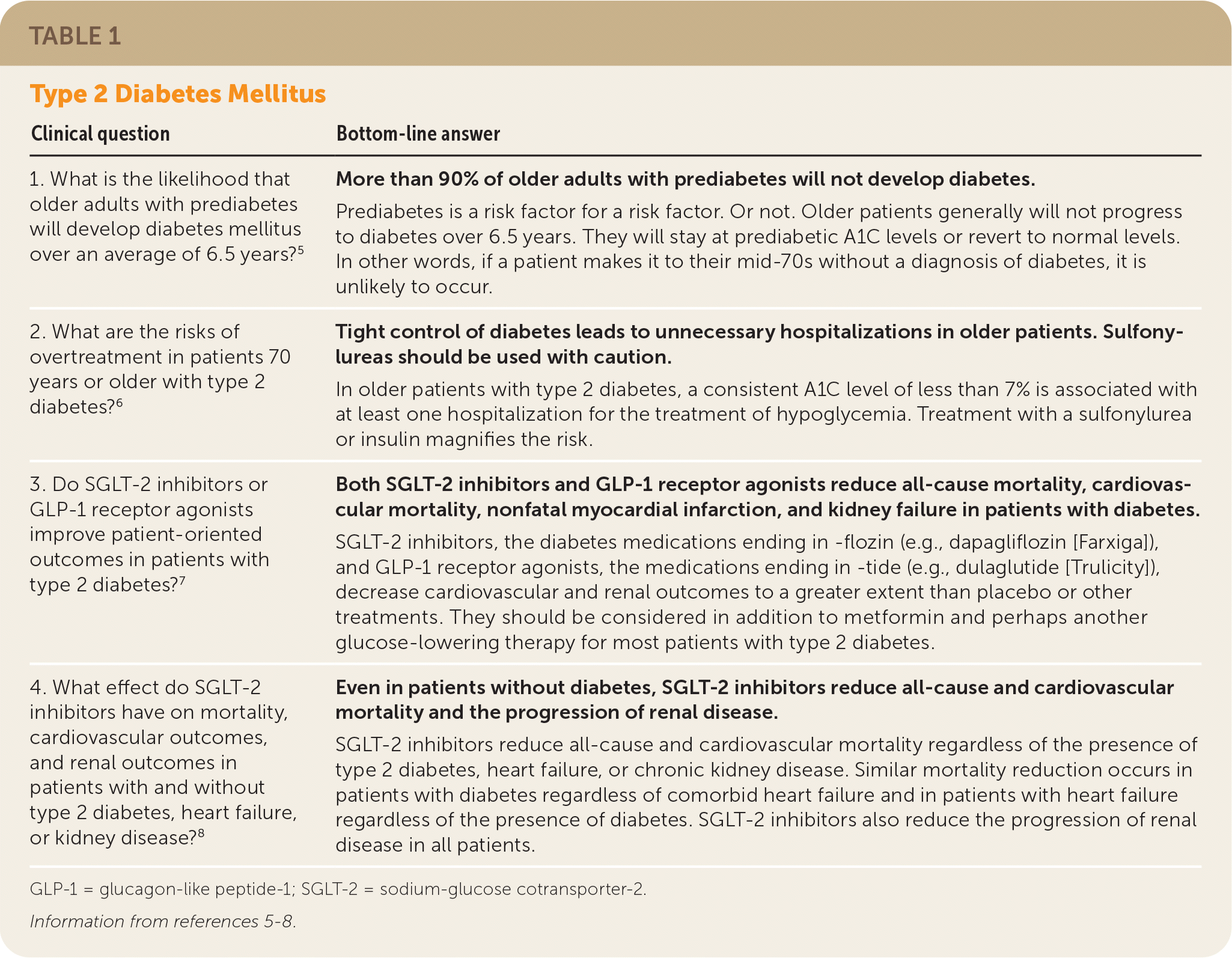
The first three POEMs in this category are about the management of type 2 diabetes (Table 1).5–8 The first study identified 2,482 adults with a mean age of 75 years who had prediabetes (defined as an A1C level between 5.7% and 6.4%, a fasting glucose level between 100 and 125 mg per dL [5.55 and 6.94 mmol per L], or both).5 Over an average of 6.5 years, only 8% to 9% of patients progressed to diabetes, many regressed to normoglycemia, and the remainder stayed at prediabetic levels. These results will help reassure physicians and avoid overtreatment of older patients with prediabetes. Of note, the U.S. Preventive Services Task Force does not recommend screening for prediabetes or type 2 diabetes beyond 70 years of age.9
TABLE 1. Type 2 Diabetes Mellitus
| Clinical question | Bottom-line answer |
|---|---|
| 1. What is the likelihood that older adults with prediabetes will develop diabetes mellitus over an average of 6.5 years?5 | More than 90% of older adults with prediabetes will not develop diabetes. Prediabetes is a risk factor for a risk factor. Or not. Older patients generally will not progress to diabetes over 6.5 years. They will stay at prediabetic A1C levels or revert to normal levels. In other words, if a patient makes it to their mid-70s without a diagnosis of diabetes, it is unlikely to occur. |
| 2. What are the risks of overtreatment in patients 70 years or older with type 2 diabetes?6 | Tight control of diabetes leads to unnecessary hospitalizations in older patients. Sulfonylureas should be used with caution. In older patients with type 2 diabetes, a consistent A1C level of less than 7% is associated with at least one hospitalization for the treatment of hypoglycemia. Treatment with a sulfonylurea or insulin magnifies the risk. |
| 3. Do SGLT-2 inhibitors or GLP-1 receptor agonists improve patient-oriented outcomes in patients with type 2 diabetes?7 | Both SGLT-2 inhibitors and GLP-1 receptor agonists reduce all-cause mortality, cardiovascular mortality, nonfatal myocardial infarction, and kidney failure in patients with diabetes. SGLT-2 inhibitors, the diabetes medications ending inflozin (e.g., dapagliflozin [Farxiga]), and GLP-1 receptor agonists, the medications ending intide (e.g., dulaglutide [Trulicity]), decrease cardiovascular and renal outcomes to a greater extent than placebo or other treatments. They should be considered in addition to metformin and perhaps another glucose-lowering therapy for most patients with type 2 diabetes. |
| 4. What effect do SGLT-2 inhibitors have on mortality, cardiovascular outcomes, and renal outcomes in patients with and without type 2 diabetes, heart failure, or kidney disease?8 | Even in patients without diabetes, SGLT-2 inhibitors reduce all-cause and cardiovascular mortality and the progression of renal disease. SGLT-2 inhibitors reduce all-cause and cardiovascular mortality regardless of the presence of type 2 diabetes, heart failure, or chronic kidney disease. Similar mortality reduction occurs in patients with diabetes regardless of comorbid heart failure and in patients with heart failure regardless of the presence of diabetes. SGLT-2 inhibitors also reduce the progression of renal disease in all patients. |
GLP-1 = glucagon-like peptide-1; SGLT-2 = sodium-glucose cotransporter-2.
A study in the United Kingdom identified 6,288 people 70 years and older with type 2 diabetes and three consecutive A1C measurements of less than 7%.6 Approximately 90% were taking a sulfonylurea. Compared with a similar group of people with type 2 diabetes who did not have A1C levels of less than 7% and were not taking a sulfonylurea, those with tight control were 2.5 times more likely to be hospitalized for severe hypoglycemia, with a 1 in 7 risk of hospitalization over 10 years. Use of a sulfonylurea or insulin was associated with severe hypoglycemia and death. A more relaxed A1C target of 7.0% to 8.0% is more appropriate, especially for older patients, and sulfonylureas should be used with caution.
A systematic review assessed the effectiveness of sodium-glucose cotransporter-2 (SGLT-2) inhibitors and glucagon-like peptide-1 (GLP-1) receptor agonists in patients with type 2 diabetes.7 The authors did not receive pharmaceutical funding. Both classes of drugs reduced all-cause mortality, cardiovascular mortality, nonfatal myocardial infarction, and kidney failure. SGLT-2 inhibitors were more effective at reducing hospital admission, whereas GLP-1 receptor agonists were more likely to reduce nonfatal stroke. The absolute benefit of treatment increased with a patient’s cardiac risk. For example, over five years, there were 2 to 5 fewer deaths per 1,000 patients at low cardiac risk compared with 24 to 48 fewer deaths per 1,000 patients at the highest risk. A useful calculator that allows estimates of benefit at various risk levels is available at https://magicevidence.org/match-it/200820dist.
The final study is a meta-analysis that examined the effect of SGLT-2 inhibitors in patients with and without type 2 diabetes or heart failure.8 These drugs similarly reduced all-cause and cardiovascular mortality in patients with or without type 2 diabetes and with or without heart failure (overall hazard ratio for all-cause mortality = 0.84 [95% CI, 0.78 to 0.91]). SGLT-2 inhibitors reduced the progression of renal disease in all patients.
Musculoskeletal Conditions
The next, and largest, category of POEMs addresses musculoskeletal conditions (Table 2).10–14 The first three present research on low back pain, one of the most challenging conditions in primary care. The first POEM is a systematic review of a broad range of therapies for chronic low back pain.10 The review included 63 randomized controlled trials (RCTs) reporting a clinical response, generally a reduction in pain of at least 30%, to any one of 15 interventions. Exercise was effective at reducing pain (number needed to treat [NNT] = 7) and had a sustained benefit. Although other medical therapies such as oral nonsteroidal anti-inflammatory drugs (NNT = 6), duloxetine (Cymbalta; NNT = 10), and opioids (NNT = 16) also reduced pain, they did not have sustained benefits and were associated with adverse effects. Lower-quality data suggest that manipulation and topical capsaicin are also effective.
TABLE 2. Musculoskeletal Conditions

| Clinical question | Bottom-line answer |
|---|---|
| 5. What interventions are effective in managing chronic low back pain?10 | Exercise is the main intervention that produces sustained improvement in chronic low back pain. The interventions that are more effective than control in achieving at least a 30% reduction in pain are exercise, oral nonsteroidal anti-inflammatory drugs, duloxetine (Cymbalta), and opioids, but discontinuation of duloxetine and opioids was common in the study. Exercise is the only intervention resulting in sustained relief. Lower-quality data suggest that manipulation and topical capsaicin are also effective. It is possible the inclusion criteria for this systematic review missed important studies. |
| 6. Do muscle relaxants provide relief for nonspecific lower back pain?11 | Muscle relaxants are not reliably effective for treating low back pain. Despite benzodiazepine or nonbenzodiazepine muscle relaxants being used for almost 50 years to treat low back pain, the evidence supporting their use is of low certainty. None of the treatments produce a clinically important difference over placebo treatment. Nonsteroidal anti-inflammatory drugs should be used for the treatment of low back pain. |
| 7. Are patients reassured by negative MRI findings for low back pain?12 | Patients with low back pain do better when told that their MRI results are unremarkable, compared with seeing the actual report without context. Information given to patients without context can be harmful. Patients with low back pain who were given the results of their MRI without interpretation by a clinician had greater pain, less self-efficacy, and lower function, even after six weeks of conservative treatment, than patients who were reassured that their MRI results were normal with age-related findings. |
| 8. For acute muscle pain, which oral analgesic provides the best immediate relief?13 | For acute muscle pain, oral acetaminophen plus ibuprofen is safer than combinations that include opioids, with equal effectiveness. A single dose of an opioid analgesic provides acute pain relief similar to a single dose of an acetaminophen and ibuprofen combination in patients with acute musculoskeletal pain in the emergency department. Opioids increase the likelihood of nausea or vomiting. There is no added benefit from 800 mg of ibuprofen compared with 400 mg. These results are similar to those of previous studies of opioids and varying doses of ibuprofen. |
| 9. Which nondrug therapies are effective for chronic pain?14 | Multiple nondrug therapies are effective for chronic musculoskeletal pain. There is low-quality and, in some cases, moderate-quality evidence for a range of noninvasive, nondrug therapies for chronic pain. Exercise, yoga, massage, and mindfulness-based stress reduction have health benefits, are relatively inexpensive, and do not require interaction with the health system. |
MRI = magnetic resonance imaging.
Another systematic review, this time looking at muscle relaxants for nonspecific low back pain, found small reductions in pain intensity that were not clinically important and not seen when only the highest-quality studies were included.11 We have said it before—it is inappropriate to routinely prescribe muscle relaxants for low back pain.
The next study showed the power of language on health outcomes.12 Patients with low back pain and no red flags on magnetic resonance imaging (MRI) or indications for surgery were randomized to receive their MRI results in one of two ways: by stating that all findings were normal and incidental or age-related or by stating that all findings were normal and incidental or age-related but also including words such as degeneration, tears, ruptures, and neural compression. Patients receiving the easily misinterpreted version of the report that used alarming words had more pain, lower self-efficacy, and less function over six weeks of follow-up compared with patients who were essentially told their findings were normal. Physicians should develop their own script for sharing results that avoids catastrophizing language.
The next POEM studied several types of musculoskeletal pain other than back pain.13 Patients presenting in the emergency department with acute musculoskeletal pain were randomized to one of five single-dose pain regimens: (1) acetaminophen, 1,000 mg, with ibuprofen, 400 mg; (2) acetaminophen, 1,000 mg, with ibuprofen, 800 mg; (3) acetaminophen, 300 mg, with codeine, 30 mg; (4) acetaminophen, 300 mg, with hydrocodone, 5 mg; or (5) acetaminophen, 325 mg, with oxycodone, 5 mg. Pain scores decreased by about 3 points on a 10-point scale in all five groups at one hour and by about 4.5 points at two hours, with no significant difference between groups. About 1 out of 4 patients in each group required rescue pain medication, again with no difference. Nausea and vomiting were more common in patients receiving an opioid. Thus, a good choice is acetaminophen, 1,000 mg, plus ibuprofen, 400 mg, or even acetaminophen alone, without an opioid.15
A large systematic review asked the question: Which nondrug therapies are effective for chronic musculoskeletal pain?14 For chronic low back pain, exercise, massage, yoga, cognitive behavior therapy, mindfulness-based stress reduction, acupuncture, spinal manipulation, low-level laser therapy, and rehabilitation all reduced pain and/or improved function. There was evidence for the use of exercise, massage, low-level laser therapy, acupuncture, and Pilates in the treatment of chronic neck pain. Only exercise and cognitive behavior therapy were helpful for knee osteoarthritis. There is evidence only for the use of exercise and manual therapies for the treatment of hip osteoarthritis. Patients with fibromyalgia benefited from cognitive behavior therapy, myofascial release massage, tai chi, qi gong, acupuncture, rehabilitation, and exercise.
Gastrointestinal
The next set of POEMs addresses colorectal cancer screening, constipation treatment, and vague abdominal symptoms (Table 3).16–18 Most countries screen for colorectal cancer using fecal immunochemical testing (FIT) as the initial method. Canada includes flexible sigmoidoscopy as an option, and the United States most commonly uses colonoscopy. The first POEM on gastrointestinal conditions is a Norwegian RCT that invited previously unscreened adults 50 to 74 years of age to undergo flexible sigmoidoscopy (52% had the procedure) or FIT every two years (68% had at least one test).16 Although flexible sigmoidoscopy initially identified more cancers and advanced adenomas, FIT surpassed it over time, with a cancer detection rate of 0.49% after three rounds of FIT testing vs. 0.27% with flexible sigmoidoscopy. This is a very important point—screening programs must be compared over time, not just after a single round, using different tests. RCTs comparing FIT with colonoscopy over time are underway.
TABLE 3. Gastrointestinal Conditions

| Clinical question | Bottom-line answer |
|---|---|
| 10. Is FIT an effective method of screening for colorectal cancer?16 | Regular FIT is an effective screening method for colorectal cancer. Screening with FIT every other year for at least six years identified fewer cancers or advanced adenomas initially but surpassed a single sigmoidoscopy after three rounds of testing. The increased detection might be in part due to greater participation in FIT than sigmoidoscopy. |
| 11. Which over-the-counter products are effective in treating chronic constipation?17 | Polyethylene glycol (Miralax) and senna are the best initial treatments for chronic constipation. In this limited systematic review without formal data synthesis, the authors concluded there is good evidence to recommend polyethylene glycol or senna as first-line therapy and moderate evidence to support fiber supplements, other stimulant laxatives, magnesium-based products, and fruit-based products. |
| 12. Which patients with vague abdominal symptoms should be referred for further workup?18 | Dysphagia, changes in bowel habits, and rectal bleeding are the most worrisome abdominal symptoms for cancer or IBD. Using a cutoff of 3% risk (from the National Institute for Health and Care Excellence), dysphagia or changes in bowel habits in men and rectal bleeding in women should prompt referral for further workup to exclude cancer or IBD. In addition, abdominal pain, changes in bowel habits, or dyspepsia in patients older than 60 years should be investigated because they predict cancer or IBD in more than 3% of men and women. |
FIT = fecal immunochemical testing; IBD = inflammatory bowel disease.
In a systematic review of over-the-counter treatments for chronic constipation, polyethylene glycol (Miralax) and senna were the most effective initial options.17 Fiber supplements, other stimulant laxatives, magnesium-based products, and fruit-based products were also effective.
The final POEM evaluated the predictive value of common abdominal symptoms for cancer or inflammatory bowel disease.18 Combinations of symptoms, such as change in bowel habits with rectal bleeding, were more predictive but varied by age and sex. Dysphagia or changes in bowel habits in men and rectal bleeding in women should prompt referral for further workup to exclude cancer or inflammatory bowel disease. Dyspepsia was largely unhelpful, except in patients older than 60 years. The severity and duration of gastrointestinal symptoms and whether they appear to be progressive were not part of this study but are important additional factors.
Cardiovascular Disease
Four POEMs about cardiovascular disease made the top 20 list (Table 4).19–22 The first two addressed prevention. One was a large pragmatic trial that randomized 15,076 patients with established arteriosclerotic cardiovascular disease to 81 mg or 325 mg of aspirin daily and evaluated the likelihood of death, nonfatal myocardial infarction, or nonfatal stroke after a median of two years.19 There was no difference between groups for these outcomes (7.3% for 81 mg and 7.5% for 325 mg) and no difference in hospitalization for major bleeding. The trial was a bit messy, with 7% in the 81-mg group switching to 325 mg and 42% in the 325-mg group switching to the lower dose. It is not clear why so many switched to the lower dose, but, for whatever reason, there is no advantage with the higher dose.
TABLE 4. Cardiovascular Diseases

| Clinical question | Bottom-line answer |
|---|---|
| 13. What dose of aspirin is best for secondary prevention in people with established ASCVD?19 | The best daily dosage of aspirin to use for secondary prevention of ASCVD is 81 mg. There is no advantage to using a 325-mg dose of aspirin for patients with established ASCVD, and people taking the higher dose often switch to the lower dose (although the reason is unclear). |
| 14. How well do the Framingham Risk Score and Pooled Cohort Equations estimate the risk of cardiovascular events in the general population?20 | These two commonly used cardiovascular risk scores overestimate the risk of cardiovascular events by about double. The Framingham Risk Score and Pooled Cohort Equations both significantly overpredicted the five-year risk of a composite cardiovascular event outcome. This is consistent with other research and should give us pause as we use these risk scores to guide therapeutic decision-making. For example, a person with a 10-year risk of 10% probably has a true risk closer to 5%, leading to very different guideline recommendations for a statin. |
| 15. How do routine clinical measurements of systolic blood pressure compare with ideal blood pressure measurement?21 | Office measurements tend to overestimate “true” blood pressure. Compared with blood pressure measurements that follow the strict protocols used in research, measurement in typical physician offices will be an average of 4.6 to 7.3 mm Hg higher for systolic readings. This study also found wide variations in clinical blood pressure readings compared with the reference standard. SPRINT demonstrated that reducing a systolic blood pressure to less than 120 mm Hg is associated with decreased mortality. However, most guidelines suggest higher goals, given that the SPRINT method of blood pressure measurement was more accurate than the method used in usual clinical practice, which overestimates true blood pressure. |
| 16. Is the consumption of eggs associated with an increased risk of cardiovascular disease?22 | Eggs do not increase the risk of cardiovascular disease. Over an average of 12 years, egg consumption is not associated with increased cardiovascular events. This meta-analysis showed that eating more than one egg per day, on average, was associated with an approximately 11% decreased likelihood of coronary artery disease. However, this decrease may be due to a healthy user bias (i.e., eating eggs might be associated with healthier habits). |
ASCVD = arteriosclerotic cardiovascular disease; SPRINT = Systolic Blood Pressure Intervention Trial.
U.S. guidelines for cardiovascular prevention all begin with an assessment of cardiovascular risk using the Pooled Cohort Equations. The second cardiovascular POEM warns us that this score significantly overestimates risk. The Canadian researchers identified more than 80,000 people 40 to 79 years of age and estimated their risk using the Framingham Risk Score and the Pooled Cohort Equations.20 Cardiovascular risk estimates from both tools were about twice as high as the real-world risk. The overestimates occurred in all groups regardless of age and sex but tended to be larger in younger patients. This is important for shared decision-making. For example, an estimated risk of 10% based on the Pooled Cohort Equations might lead to prescribing a statin, but the true cardiovascular risk may be significantly lower.
The U.S. Preventive Services Task Force draft guidelines recommend prescribing a statin for adults 40 to 75 years of age with at least one cardiovascular risk factor (dyslipidemia, diabetes, hypertension, or smoking) and an estimated 10-year cardiovascular risk of 10% or greater. Statins should be selectively offered to those with a risk factor and a risk between 7.5% and 10% because the benefits are smaller than those at higher risk.23
Another calibration issue was addressed by the third POEM. The researchers compared the blood pressure measurements used by researchers in SPRINT (Systolic Blood Pressure Intervention Trial) with those recorded by the patients’ regular primary care physicians.21 The physician-recorded systolic blood pressure measurements were about 5 to 7 mm Hg higher; therefore, the SPRINT recommendations to lower systolic blood pressure to less than 120 mm Hg need to be interpreted accordingly—in the real world, achieving a level of 130 mm Hg is probably similar to 120 mm Hg in the trial setting.
The next POEM made our day, as egg lovers. This systematic review included 23 observational studies with nearly 1.4 million patients.22 Eating more eggs was not shown to increase the risk of cardiovascular events. In fact, compared with eating one or no eggs per day, those eating more than one egg per day had a decreased risk of coronary disease (hazard ratio = 0.89; 95% CI, 0.86 to 0.93).
Miscellaneous
Four top POEMs do not fall easily into a single category (Table 5).24–27 A systematic review addressed treatment of chronic pain caused by diabetic neuropathy or postherpetic neuralgia.24 It included only studies reporting an outcome of clinically meaningful response, defined as a 30% improvement on a pain or function score. Moderate-quality evidence supported the use of the anticonvulsants gabapentin (Neurontin) and pregabalin (Lyrica) and the serotonin-norepinephrine reuptake inhibitors duloxetine and venlafaxine, and low-quality evidence supported the use of rubefacients (usually salicylates). The NNT was 7 or 8 for all the identified therapies. Opioid studies were of low quality and also showed more harms (number needed to harm = 12). Only a few trials with low-certainty evidence studied acupuncture and tricyclic antidepressants.
TABLE 5. Miscellaneous

| Clinical question | Bottom-line answer |
|---|---|
| 17. Which treatments for chronic neuropathic pain can provide clinically meaningful improvement?24 | The anticonvulsants gabapentin (Neurontin) and pregabalin (Lyrica) and the SNRIs duloxetine (Cymbalta) and venlafaxine improve chronic neuropathic pain. Given the balance of benefits and harms, there is moderate-quality evidence for anticonvulsants (gabapentin and pregabalin were similarly effective and well tolerated) and SNRIs (duloxetine and venlafaxine were similarly effective and well tolerated). Rubefacients (usually salicylates) appear to be effective but are not as well studied and have low-quality evidence. Acupuncture, opioids, and tricyclic antidepressants cannot be recommended based on current evidence. |
| 18. Does increasing anti-depressants to above the minimum dose improve outcomes?25 | Low doses of selected antidepressants work just as well as higher doses. For new-generation antidepressants, including selective serotonin reuptake inhibitors, venlafaxine, and mirtazapine (Remeron), initial titration over the first eight weeks of treatment provides no benefit over starting with the minimum dose in patients with moderate to severe depression. Unfortunately, this means waiting six to eight weeks to judge the response to treatment before moving to another medication. |
| 19. What is the effect of a delayed prescription approach for children with respiratory tract infection?26 | “Take-and-hold” prescriptions for upper respiratory tract infections reduce antibiotic use and adverse effects. A strategy of providing education about the natural history of respiratory symptoms in children combined with giving a take-and-hold prescription (to be filled only if symptoms persist) resulted in only 1 in 4 children eventually taking an antibiotic. However, it increased the number of children who used other medications to control symptoms, which indicates the parents’ need to do something. Symptom severity and time to resolution, complications, and follow-up visits were similar whether children received immediate, delayed, or no antibiotic treatment. Immediate treatment resulted in more gastrointestinal symptoms. Similar results have been shown in adults. |
| 20. Is supplemental oral vitamin C plus iron replacement more effective than oral iron replacement alone in adults with iron deficiency anemia?27 | Vitamin C should not be added to iron replacement therapy. This study found no difference in hemoglobin or serum ferritin level after three months in adults with iron deficiency anemia who were treated with oral iron plus vitamin C vs. oral iron alone. |
SNRI = serotonin-norepinephrine reuptake inhibitor.
A systematic review identified RCTs that compared treatment of moderate to severe depression using the minimum licensed dose of a selective serotonin reuptake inhibitor, venlafaxine, or mirtazapine (Remeron) with a dosing regimen that allowed titration to higher doses.25 There was no improvement in the balance of effectiveness and harms between taking the minimum dose and titrating to higher doses, although patients taking venlafaxine may respond to a higher dose if they show no response to the minimum dose.
The next POEM identified 436 children with pharyngitis, rhinosinusitis, acute bronchitis, or acute otitis media whose treating physician had reasonable doubts about the need for an antibiotic.26 Patients were randomized to no antibiotics; an immediate antibiotic; or an antibiotic prescription to be filled only if the child had fever, felt much worse after 24 hours, or was not improving after a longer period (varied by type of infection). Only 25% of children in the delayed antibiotic group and 12% in the no antibiotic group ultimately filled a prescription, and there was no difference between these groups and the immediate antibiotic group in the duration of symptoms (eight days) or complications. Gastrointestinal symptoms and cost were higher in those receiving an antibiotic.
Finally, clinicians have long recommended that people taking iron supplements also take vitamin C because it theoretically improves absorption. A study tested the theory by randomizing 440 adults with iron deficiency anemia to ferrous succinate, 100 mg, plus vitamin C, 200 mg, or to ferrous succinate alone, each given every eight hours. There was no difference in hemoglobin or serum ferritin levels at three months.27
Practice Guidelines
POEMs sometimes summarize high-impact clinical practice guidelines. Key messages from the three highest-rated guidelines, which address antibiotics for common infections, non–low back musculoskeletal injuries, and tobacco screening and cessation, are summarized in Table 6.28–30
TABLE 6. Practice Guidelines

| Clinical question | Bottom-line answer |
|---|---|
| 21. Are short antibiotic courses as effective as longer courses for common infections?28 | Short antibiotic courses should be used for community-acquired pneumonia, COPD exacerbation, uncomplicated pyelonephritis, and nonpurulent cellulitis. American College of Physicians guidelines recommend five days of antibiotics for community-acquired pneumonia, five days for COPD exacerbation, five to seven days for uncomplicated pyelonephritis if using a quinolone, and five to six days for nonpurulent cellulitis. Longer courses may be necessary if there is no clinical improvement. Guideline summary: https://www.aafp.org/afp/2022/0200/p205.html |
| 22. What therapies are recommended for acute pain from non–low back musculoskeletal injuries?29 | Topical NSAIDs are first-line therapy for non–low back musculoskeletal injuries. Oral NSAIDs, acetaminophen, acupressure, or TENS may also be used. The American College of Physicians and American Academy of Family Physicians collaborated to create guidelines on the management of non–low back musculoskeletal injuries. Based on a large systematic review and network meta-analysis, they give a strong recommendation for topical diclofenac as first-line therapy and a conditional recommendation for oral NSAIDs, acetaminophen, acupressure, or TENS. Opioids are not recommended because of greater adverse effects and risk of prolonged use. Guideline summary: https://www.aafp.org/afp/2020/1201/p697.html |
| 23. What is the optimal approach to screening for tobacco use in adults?30 | Physicians should screen for tobacco use in all adults and provide behavioral interventions and pharmacotherapy to aid in smoking cessation. The U.S. Preventive Services Task Force found sufficient evidence to support the use of nicotine replacement therapy, bupropion, varenicline (Chantix), or behavioral interventions, with the combination of pharmacotherapy and behavioral interventions more effective than either alone. Effective behavioral interventions include advice from a physician or nurse, individual counseling, group behavioral interventions, telephone counseling, mobile phone–based interventions (including texting), health education, feedback, financial incentives, and social support. In pregnancy, only behavioral interventions are recommended given the lack of evidence around pharmacotherapy in pregnancy. Guideline summary: https://www.aafp.org/afp/2021/0615/od1.html |
COPD = chronic obstructive pulmonary disease; NSAID = nonsteroidal anti-inflammatory drug; TENS = transcutaneous electrical nerve stimulation.
Editor's Note: This article was cowritten by Dr. Mark Ebell, deputy editor for evidence-based medicine for AFP and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell’s dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP’s medical editors. In addition, the article underwent peer review and editing by four of AFP’s medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia for their work as peer reviewers; Canadian Medical Association Joule for supporting the POEMs CME program in Canada; Pierre Pluye, PhD, for codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs.

