Key Points for Practice
• Adding POCUS to a standard diagnostic workup for dyspnea does not improve clinical outcomes, although it increases the probability of a correct diagnosis and appropriate treatment at four hours.
• Adding POCUS to a standard diagnostic workup for dyspnea improves diagnostic accuracy for pneumonia, congestive heart failure, pulmonary embolism, and pleural effusion.
• POCUS is less helpful when used instead of a standard diagnostic pathway or when the workup does not suggest a diagnosis.
From the AFP Editors
Respiratory issues, including dyspnea, led more than 1 million people to the emergency department before the COVID-19 pandemic. The standard clinical workup for patients with undifferentiated dyspnea often includes electrocardiography, chest radiography, and laboratory measurements. Point-of-care ultrasonography (POCUS) can aid in diagnosing numerous etiologies for dyspnea, including decompensated heart failure, pleural effusion, pneumothorax, pulmonary embolism, and exacerbations of chronic obstructive pulmonary disease using limited echocardiography, lung, inferior vena cava, and deep vein assessments.
The American College of Physicians (ACP) released clinical guidelines for POCUS use in patients with acute dyspnea based on a systematic review of 49 studies that included five randomized controlled trials.
Impact of Adding POCUS to a Workup of Dyspnea
Adding POCUS to a standard diagnostic workup does not appear to improve clinical outcomes in patients with dyspnea based on five randomized controlled trials that included about 1,500 patients. In these studies, adding POCUS to the workup did not improve mortality, length of hospitalization, or readmission within 30 days. No studies reported harms from POCUS, such as from incidental findings or false-positive or false-negative results.
Diagnostic accuracy and the time to correct diagnosis are improved when POCUS examinations are added to the standard diagnostic workup in patients with dyspnea. In one trial, adding POCUS to the workup increased the correct diagnosis at four hours by 24% and the appropriate treatment at four hours by 21%. In one small study, POCUS shortened the time to finding a diagnosis for a patient with dyspnea.
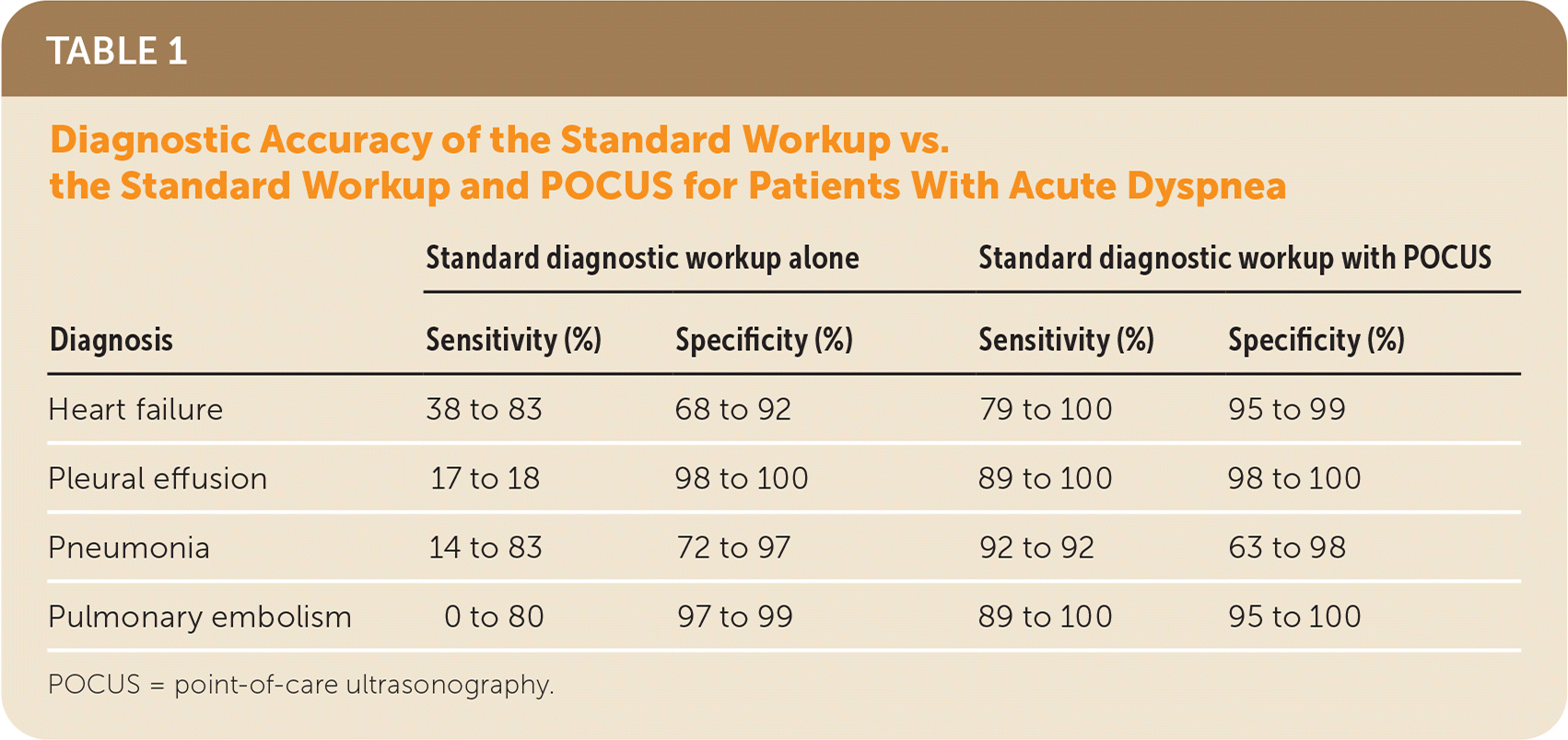
Adding POCUS to a standard diagnostic workup increases the sensitivity and specificity of diagnosing congestive heart failure, pneumonia, pulmonary embolism, and pleural effusion (Table 1). Data could be combined only for congestive heart failure, where adding POCUS to the workup resulted in a sensitivity of 76% (95% CI, 48% to 91%) and specificity of 96% (95% CI, 90% to 98%). No study looked at the accuracy of POCUS for diagnosing pneumothorax. POCUS is less helpful when used instead of a standard diagnostic workup, or if the workup does not suggest a diagnosis.
TABLE 1. Diagnostic Accuracy of the Standard Workup vs. the Standard Workup and POCUS for Patients With Acute Dyspnea
| Diagnosis | Standard diagnostic workup alone | Standard diagnostic workup with POCUS | ||
|---|---|---|---|---|
| Sensitivity (%) | Specificity (%) | Sensitivity (%) | Specificity (%) | |
| Heart failure | 38 to 83 | 68 to 92 | 79 to 100 | 95 to 99 |
| Pleural effusion | 17 to 18 | 98 to 100 | 89 to 100 | 98 to 100 |
| Pneumonia | 14 to 83 | 72 to 97 | 92 to 92 | 63 to 98 |
| Pulmonary embolism | 0 to 80 | 97 to 99 | 89 to 100 | 95 to 100 |
POCUS = point-of-care ultrasonography.
Limitations
No studies were identified that analyzed replacing the standard diagnostic workup with POCUS. In the studies examined for this guideline, the patients and their pretest probabilities differed significantly, with the prevalence of pneumonia at 21% in one study and 91% in another. Most studies included patients with multiple chronic conditions. The reference for the true diagnosis varied from independent chart review to diagnosis at discharge to imaging results. More than one-half of the studies were judged to be at high risk of bias. Few studies reported indeterminate POCUS results, suggesting these results were likely not included in the analysis.
The views expressed are those of the author and do not necessarily reflect the official policy or position of the U.S. Department of the Army, Uniformed Services University of the Health Sciences, U.S. Department of Defense, or the U.S. government.
Editor's Note: Although there are other systematic reviews looking at the benefit of POCUS, this is the first with enough data to support clinical guidelines. For patients with dyspnea, adding POCUS to a clinical evaluation improves the probability of an accurate, timely diagnosis.—Michael J. Arnold, MD, Contributing Editor
Guideline source: American College of Physicians
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? Yes
Recommendations based on patient-oriented outcomes? Yes
Published source: Ann Intern Med. July 2021;174(7):985–993 (published correction appears in Ann Intern Med. 2022;175(3):458–459)
Available at: https://www.acpjournals.org/doi/10.7326/m20-5504

