Key Points for Practice
• Screening tools can identify unhealthy alcohol use, which can be treated effectively with brief interventions.
• Benzodiazepines are the primary therapy for alcohol withdrawal; gabapentin, carbamazepine, and valproic acid appear to be effective for less severe withdrawal symptoms.
• Naltrexone and topiramate are effective for preventing relapse in alcohol use disorder.
• Psychological therapies are a primary treatment for cannabis and stimulant use disorders and are effective for alcohol use disorder, but they are not beneficial in opioid use disorder.
From the AFP Editors
More than 20 million people in the United States meet the criteria for substance use disorder, leading to $600 billion in health care expenditures annually. Despite this growing problem, only one in eight people with substance use disorder receives targeted care. The U.S. Department of Veterans Affairs and the U.S. Department of Defense (VA/DoD) published updated clinical practice guidelines for managing substance use disorders, based on a systematic review.
Screening for Unhealthy Substance Use
ALCOHOL USE
Many people have risky drinking habits without meeting criteria for alcohol use disorder. Screening for unhealthy alcohol use is recommended based on evidence for patients who do not have alcohol use disorder. Brief interventions for these patients help reduce alcohol consumption and improve health outcomes.
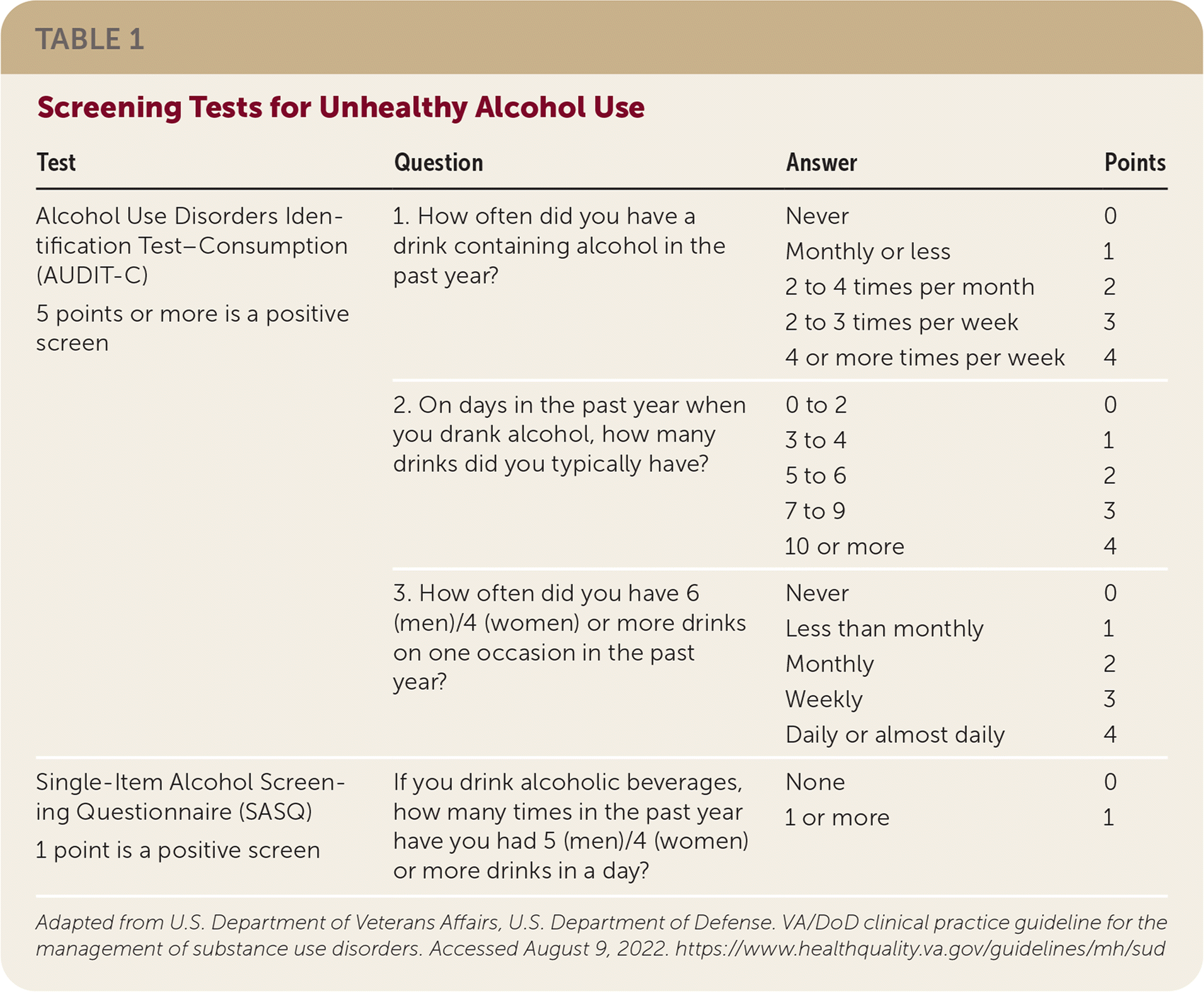
The Alcohol Use Disorders Identification Test–Consumption (AUDIT-C) and the Single-Item Alcohol Screening Questionnaire (SASQ) are the recommended tools for assessing unhealthy alcohol use in primary care (Table 1). The AUDIT-C provides more information on normal and heavy drinking, yet requires more time to administer and score. The SASQ is a single question and easy to use within a patient encounter.
TABLE 1. Screening Tests for Unhealthy Alcohol Use
| Test | Question | Answer | Points |
|---|---|---|---|
| Alcohol Use Disorders Iden tification Test–Consumption (AUDIT-C) 5 points or more is a positive screen | 1. How often did you have a drink containing alcohol in the past year? | Never | 0 |
| Monthly or less | 1 | ||
| 2 to 4 times per month | 2 | ||
| 2 to 3 times per week | 3 | ||
| 4 or more times per week | 4 | ||
| 2. On days in the past year when you drank alcohol, how many drinks did you typically have? | 0 to 2 | 0 | |
| 3 to 4 | 1 | ||
| 5 to 6 | 2 | ||
| 7 to 9 | 3 | ||
| 10 or more | 4 | ||
| 3. How often did you have 6 (men)/4 (women) or more drinks on one occasion in the past year? | Never | 0 | |
| Less than monthly | 1 | ||
| Monthly | 2 | ||
| Weekly | 3 | ||
| Daily or almost daily | 4 | ||
| Single-Item Alcohol Screening Questionnaire (SASQ) 1 point is a positive screen | If you drink alcoholic beverages, how many times in the past year have you had 5 (men)/4 (women) or more drinks in a day? | None | 0 |
| 1 or more | 1 |
Adapted from U.S. Department of Veterans Affairs, U.S. Department of Defense. VA/DoD clinical practice guideline for the management of substance use disorders. Accessed August 9, 2022. https://www.healthquality.va.gov/guidelines/mh/sud
For positive screening results in patients who do not meet criteria for alcohol use disorder based on the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., a brief intervention about alcohol-related risks and advice on abstaining or reducing consumption to daily or weekly recommendations should be considered. Short behavioral interventions decrease the mean number of drinks per week and heavy drinking episodes, while increasing the percentage of patients whose alcohol consumption is within recommended limits. Benefits are similar after interventions lasting five to 20 minutes, given by physicians or psychologists and provided in the clinic, emergency department, or inpatient ward.
When substance use disorders, including alcohol, are diagnosed, there are no evidence-based criteria to guide treatment location. The American Society of Addiction Medicine has proposed assessing six dimensions of substance abuse, but the criteria have not been verified.
DRUG USE
The U.S. Preventive Services Task Force recommends screening for unhealthy drug use in adults if resources for diagnosis and treatment are available, although reductions in drug use occur primarily in patients who seek care. Drug use disorder screening does not appear to increase treatment program enrollment. Brief interventions for unhealthy drug use do not appear to reduce drug use.
Alcohol Use Disorder
Alcohol use disorder affects 14.5 million people in the United States, and annually more than 95,000 deaths are related to alcohol use.
TREATING ALCOHOL WITHDRAWAL
Alcohol withdrawal is a risk after cessation of consistent alcohol use. Withdrawal symptoms are often graded by the Clinical Institute Withdrawal Assessment for Alcohol-revised version (CIWA-Ar). Because withdrawal delirium has a mortality rate of up to 4% among hospitalized patients, inpatient treatment should be considered for people with CIWA-Ar scores of 20 or more, a history of delirium tremens or withdrawal seizures, complicating medical conditions, comorbid substance use, lack of success with outpatient care, inability to complete an outpatient program, active psychosis, or cognitive impairment. Benzodiazepines are the preferred therapy for patients with CIWA-Ar scores of 10 or more because they reduce the risk of withdrawal seizures by 84% compared with placebo (risk ratio = 0.16; 95% CI, 0.04 to 0.69).
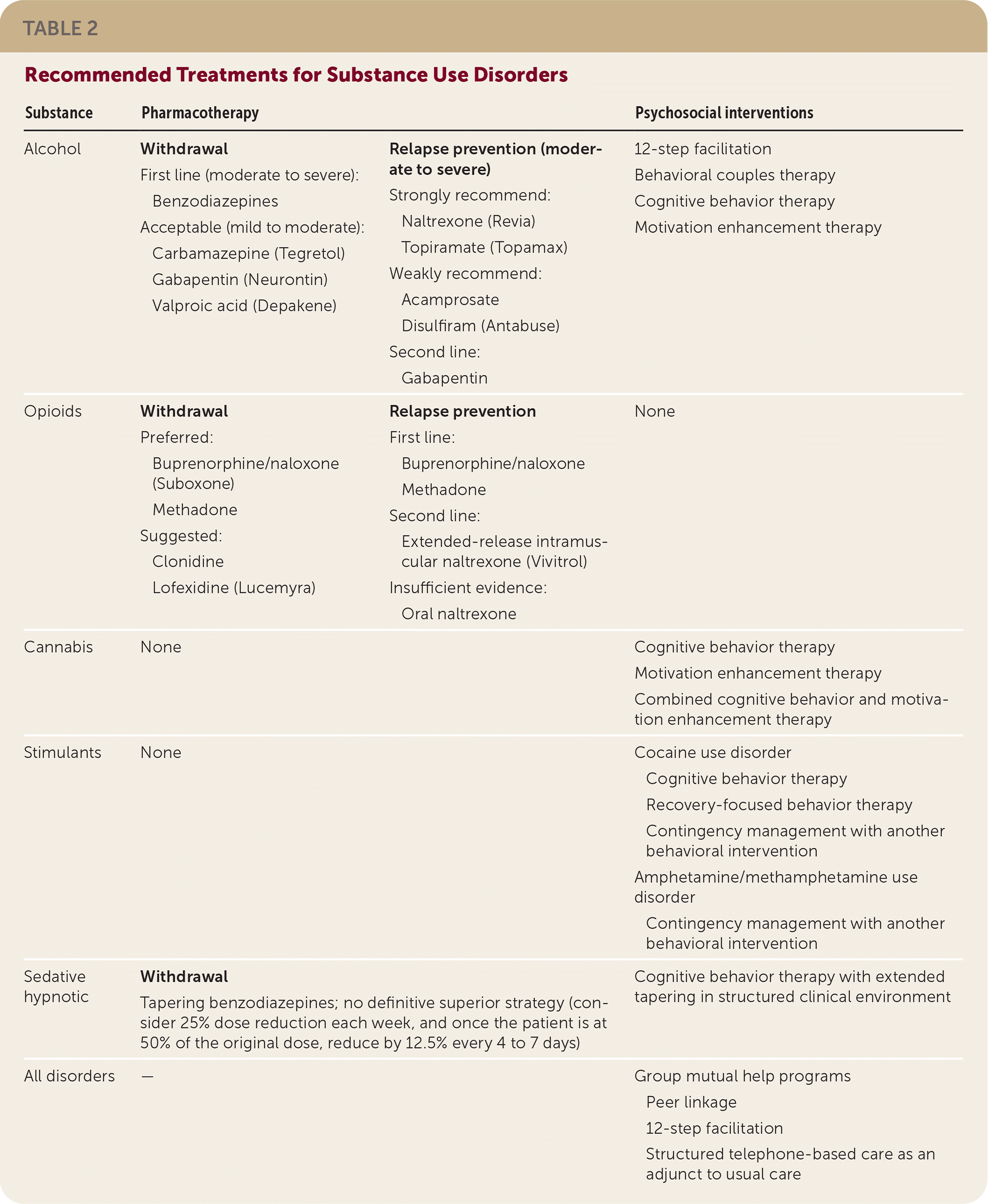
If withdrawal symptoms are less severe, treatment options (Table 2) include gabapentin (Neurontin), carbamazepine (Tegretol), and valproic acid (Depakene). All appear to have similar effectiveness compared with benzodiazepines. These medications may be useful if there are concerns about inadequate monitoring, a history of sedative abuse, or adverse reactions to benzodiazepines.
TABLE 2. Recommended Treatments for Substance Use Disorders
| Substance | Pharmacotherapy | Psychosocial interventions | |
|---|---|---|---|
| Alcohol | Withdrawal First line (moderate to severe): Benzodiazepines Acceptable (mild to moderate): Carbamazepine (Tegretol) Gabapentin (Neurontin) Valproic acid (Depakene) | Relapse prevention (moderate to severe) Strongly recommend: Naltrexone (Revia) Topiramate (Topamax) Weakly recommend: Acamprosate Disulfiram (Antabuse) Second line: Gabapentin | 12-step facilitation Behavioral couples therapy Cognitive behavior therapy Motivation enhancement therapy |
| Opioids | Withdrawal Preferred: Buprenorphine/naloxone (Suboxone) Methadone Suggested: Clonidine Lofexidine (Lucemyra) | Relapse prevention First line: Buprenorphine/naloxone Methadone Second line: Extended-release intramuscular naltrexone (Vivitrol) Insufficient evidence: Oral naltrexone | None |
| Cannabis | None | Cognitive behavior therapy Motivation enhancement therapy Combined cognitive behavior and motivation enhancement therapy | |
| Stimulants | None | Cocaine use disorder Cognitive behavior therapy Recovery-focused behavior therapy Contingency management with another behavioral intervention Amphetamine/methamphetamine use disorder Contingency management with another behavioral intervention | |
| Sedative hypnotic | Withdrawal Tapering benzodiazepines; no definitive superior strategy (consider 25% dose reduction each week, and once the patient is at 50% of the original dose, reduce by 12.5% every 4 to 7 days) | Cognitive behavior therapy with extended tapering in structured clinical environment | |
| All disorders | — | Group mutual help programs Peer linkage 12-step facilitation Structured telephone-based care as an adjunct to usual care | |
MAINTAINING ABSTINENCE
For maintenance pharmacotherapy in alcohol use disorder, naltrexone (Revia, Vivitrol) and topiramate (Topamax) have the best evidence. Naltrexone, delivered daily as an oral dose or monthly as an intramuscular injection, reduces drinking days, heavy drinking, and return to heavy drinking. Topiramate improves abstinence and reduces heavy drinking. In addition to being off label for alcohol use disorder, topiramate often requires more titration. For patients with comorbid posttraumatic stress disorder, topiramate can reduce symptom severity and alcohol use.
Acamprosate and disulfiram (Antabuse) have less evidence for improving outcomes. Acamprosate reduces return to drinking after abstinence but has limited adherence because of large tablet size and three times daily dosing. Disulfiram is only more effective than placebo in open-label trials, especially those with witnessed medication ingestion. Disulfiram rarely causes hepatotoxicity, which is worsened with alcohol use. The benefit of gabapentin for maintenance in alcohol use disorder is uncertain.
Several psychosocial interventions are effective for patients with alcohol use disorder. Twelve-step programs appear to be more effective than cognitive behavior therapy and motivation enhancement therapy, which are both superior to minimal control interventions. Behavioral couples therapy and community reinforcement approaches reduce alcohol use, and couples therapy improves marital satisfaction.
Opioid Use Disorder
In 2018, more than 46,800 people in the United States died from opioid overdose. Slightly less than 48,300 people died by suicide. Synthetic opioids such as fentanyl are the primary cause of opioid overdose deaths, which affect twice as many men as women.
TREATING OPIOID WITHDRAWAL
Because of high rates of relapse and overdose, opioid withdrawal management is only recommended as part of long-term treatment (Table 2). When starting long-term treatment for opioid use disorder, opioid agonist treatment with buprenorphine/naloxone (Suboxone) or methadone is recommended. Methadone can only be prescribed in accredited opioid treatment programs. Buprenorphine/naloxone may be more effective than methadone. When methadone and buprenorphine/naloxone are contraindicated, unacceptable, or unavailable, prescribing clonidine or lofexidine (Lucemyra) should be considered.
MAINTAINING ABSTINENCE
Buprenorphine/naloxone and methadone are the primary treatments for maintaining abstinence, and they are more effective than psychological treatment for opioid use disorder. Oral buprenorphine/naloxone is recommended to reduce harm from injection of crushed pills. Methadone is limited to accredited opioid treatment programs because of significant risks.
Naltrexone appears less effective than buprenorphine/naloxone for maintaining abstinence. Intramuscular naltrexone can be given monthly after at least seven days of opioid abstinence. Buprenorphine/naloxone is more effective than intramuscular naltrexone at preventing relapse at 24 weeks, with a number needed to treat of 13. Oral naltrexone has little evidence but appears less effective than buprenorphine and intravenous naltrexone.
Adding psychological therapy to medication-assisted treatment does not appear to improve outcomes in opioid use disorder.
Benzodiazepine Use Disorder
The primary treatment for benzodiazepine use disorder is slow benzodiazepine dose tapering. Although there is little evidence, tapering is usually more rapid early because early withdrawal is more tolerable. A common strategy is to reduce the dose by 25% each week to 50% of the original dose, then reduce the dose by 12.5% every four to seven days. Slow tapering is successful in two-thirds of patients. No additional interventions appear to be beneficial.
Cannabis Use Disorder
No medication, including cannabinoids, leads to increased abstinence in cannabis use disorder. Cognitive behavior therapy and motivation enhancement therapy do increase abstinence.
Stimulant Use Disorder
No medication, including topiramate, appears to increase abstinence in stimulant use disorder. Cognitive behavior therapy, recovery-focused behavior therapy, and contingency management increase abstinence in cocaine use disorder. Contingency management is effective for amphetamine use disorder.
The views expressed are those of the authors and do not necessarily reflect the official policy or position of the U.S. Department of the Navy, Uniformed Services University of the Health Sciences, or the U.S. government.
Guideline source: U.S. Department of Veterans Affairs and U.S. Department of Defense
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? Yes
Recommendations based on patient-oriented outcomes? Yes
Available at: https://www.healthquality.va.gov/guidelines/mh/sud

