Purpose: To review the evidence and provide clinical recommendations for appropriate blood pressure treatment targets for adults with hypertension.
Methods: This guideline is based on a systematic review of randomized controlled trials (RCTs) from database inception to May 2019. The target audience for the guideline includes all primary care clinicians, including family physicians, and the target patient population includes adults who have hypertension with or without cardiovascular disease (CVD). The panel defined patients as having hypertension when their blood pressures routinely measured higher than 140/90 mm Hg. This guideline was developed using a modified version of the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) system, a transparent approach to evaluating the certainty of the evidence and determining the strength of recommendations.
Recommendation 1: The American Academy of Family Physicians (AAFP) strongly recommends clinicians treat adults who have hypertension to a standard blood pressure target (less than 140/90 mm Hg) to reduce the risk of all cause and cardiovascular mortality (strong recommendation; high-quality evidence). Treating to a lower blood pressure target (less than 135/85 mm Hg) did not provide additional benefit at preventing mortality; however, a lower blood pressure target could be considered based on clinical assessment and patient preferences and values.
Recommendation 2: The AAFP recommends clinicians consider treating adults who have hypertension to a lower blood pressure target (less than 135/85 mm Hg) to reduce risk of myocardial infarction (weak recommendation; moderate-quality evidence). Although treatment to a standard blood pressure target (less than 140/90 mm Hg) reduced the risk of myocardial infarction, there was a small additional benefit observed with a lower blood pressure target. There was no observed additional benefit in preventing stroke with the lower blood pressure target.
Guideline Scope and Purpose
The purpose of this guideline is to provide recommendations relevant to primary care for blood pressure treatment targets. This guideline will not discuss specific pharmacologic or other hypertension treatments. The target audience includes family physicians and other primary care clinicians. The target patient population is adults with hypertension, with or without CVD.
Introduction
Hypertension is a highly prevalent condition that results in significant morbidity and mortality. Defined as systolic blood pressure 140 mm Hg and higher or diastolic blood pressure 90 mm Hg and higher, hypertension affects approximately 32% of adults in the United States1 and is a leading cause of death worldwide.2 In the United States, hypertension annually costs between $131 billion and $198 billion, including costs of medications, health care services, and loss of productivity from premature death.3
Risk factors for hypertension include having obesity or overweight,4 alcohol use,5 increasing age,6 a family history of hypertension,7 exposure to systemic racism,8 diabetes mellitus,6 and physical inactivity.6 Uncontrolled hypertension is associated with CVD, renal disease, cerebrovascular disease, and death.9 Typical interventions for aiding patients in reducing blood pressure include lifestyle modifications (i.e., weight loss, dietary changes, and increased physical activity) and antihypertensive medications. The most common pharmacologic treatments for reducing blood pressure include angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, thiazide diuretics, calcium channel blockers, and beta blockers. Selection of medications should include cost, ease of use, adverse effect profile, and comorbid conditions.
Accurate measurement of blood pressure is essential to the diagnosis and management of hypertension. Ambulatory and home blood pressure measurements can be useful in diagnosis and monitoring. Although the optimal method for blood pressure measurement remains unclear and under investigation, diagnosis requires two or more blood pressure readings on two or more occasions that meet the criteria for hypertension.
The goal of treatment is to reduce morbidity and mortality while minimizing risk of harms from medical intervention. Significant debate exists as to the ideal blood pressure targets for treatment of hypertension, and clinicians and patients are faced with conflicting recommendations from different organizations. The AAFP endorsed the Eighth Joint National Committee (JNC 8) guidelines for the management of hypertension in 2014 and reaffirmed it in 2019 as part of its five-year review process.10 Additionally, the AAFP developed a joint guideline with the American College of Physicians in 2017 that provided evidence-based recommendations for blood pressure treatment targets in adults older than 60 years.11 However, both guidelines are now considered out of date, and, given the availability of new evidence, updated guidance from the AAFP was identified as a need. Multiple other guidelines have been published with differing recommendations.12–16 Due to differences in methodologic rigor, insufficient consideration of harms, and the management of conflicts of interest, the AAFP has not endorsed these guidelines, leaving uncertainty for family physicians and other primary care clinicians when managing hypertension.17 Identifying evidence-based blood pressure treatment targets using shared decision-making that incorporates patient risks and values will improve patient-oriented outcomes while minimizing harms.
Methods
SYSTEMATIC REVIEW
In 2020, the Cochrane Database of Systematic Reviews published an updated systematic review on blood pressure targets in adults with hypertension (Arguedas, et al.).18 The report included studies evaluating the effectiveness of standard and lower blood pressure treatment targets in adults. The review included adults with or without preexisting CVD; however, most patients (76%) included in the studies did not have preexisting CVD and were receiving hypertension treatment for primary prevention. The average age of participants was 63.1 years, and the mean weighted blood pressure was 155/91 mm Hg. The review used the following definitions: Lower targets were defined as blood pressure levels less than or equal to 135/85 mm Hg, and standard targets were defined as blood pressure levels less than or equal to 140/90 mm Hg.18 It is important to note that all the included trials used a blood pressure target of less than 130 mm Hg, with most using a target of less 120 mm Hg for the lower blood pressure targets.
The main objective of the review was to determine whether lower blood pressure targets were associated with lower morbidity and mortality compared with standard blood pressure targets. The review also assessed differences in study withdrawals as a marker of tolerability, average number of medications by patients in each group, and mean blood pressure achieved in studies using a lower blood pressure target.18 Serious adverse events were defined according to U.S. Food and Drug Administration criteria, including death, life-threatening event, requiring or prolonging hospitalization, congenital anomaly, or requiring intervention to prevent permanent impairment or damage.
Databases were searched for English-language studies published from database inception to May 29, 2019, and included Embase, MEDLINE and Epub Ahead of Print, In-Process & Other Non-Indexed Citations, Cochrane Central Registrar of Controlled Trials, Ovid Cochrane Database of Systematic Reviews, U.S. National Institutes of Health Ongoing Trials Register (clinicaltrials.gov), and World Health Organization International Clinical Trials Registry Platform (https://apps.who.int/trialsearch).18
Titles and abstracts were reviewed using prespecified inclusion and exclusion criteria.18 The authors then assessed all included studies for quality using the Cochrane Risk of Bias Tool. The review included 11 RCTs (36,688 patients with a mean follow-up of 3.7 years).18
UPDATED LITERATURE REVIEW
A targeted, updated literature search to identify new RCTs was completed by AAFP staff using similar search terms as the original review with focus on systematic reviews, RCTs, and meta-analyses that were available in English. The updated search resulted in 11 articles spanning the time of the completion of the systematic review in 2020 through December 1, 2021. Three original reports were relevant to the scope of the guideline; however, they were not included in the evidence table because of differences in outcome measurements and methodologic concerns.19–21 Where appropriate, these studies are acknowledged in the supporting text. Additionally, the guideline development group considered another Cochrane systematic review published in 2020 (Saiz, et al.), which addressed blood pressure targets in adults who have hypertension and CVD.22 The Arguedas, et al., and Saiz, et al., reviews analyzed many of the same studies; however, the Saiz, et al., review evaluated composite outcomes and used slightly different blood pressure targets and, as a result, was not included as part of the evidence tables.18,22 Because the Saiz, et al., review showed similar results supportive of the recommendations, it is discussed in the supporting text below.
Constructing the Guideline
The AAFP’s Commission on Health of the Public and Science appointed a guideline development group to develop the guideline. Members of the group included physicians with expertise in guideline development and family medicine. A patient panel was convened to provide key perspectives on the evidence-to-decision frameworks, recommendations, and the draft guideline. The guideline development group followed the development process that can be found in the AAFP Clinical Practice Guideline Manual.23 The group reviewed the evidence from the systematic review and used a modified version23 of the GRADE24 system to rate the quality of the evidence for each outcome and the overall strength of each recommendation. The strength of recommendation reflects the extent to which one can be confident that the desirable effects of an intervention outweigh the undesirable effects and reflect the degree to which there is evidence of improved patient-oriented health outcomes (Table 1).
TABLE 1. AAFP Grading System
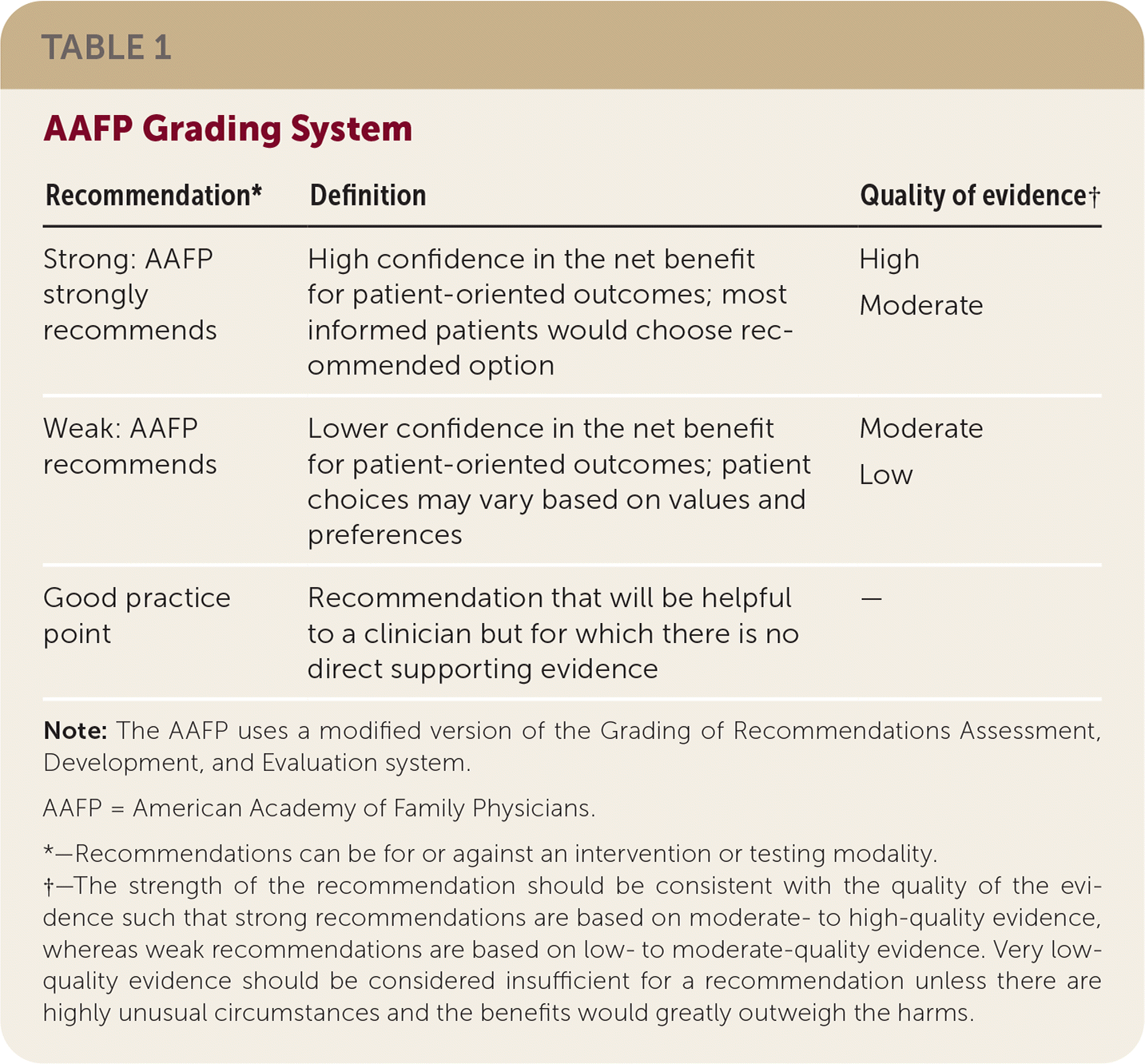
| Recommendation* | Definition | Quality of evidence† |
|---|---|---|
| Strong: AAFP strongly recommends | High confidence in the net benefit for patient-oriented outcomes; most informed patients would choose recommended option | High Moderate |
| Weak: AAFP recommends | Lower confidence in the net benefit for patient-oriented outcomes; patient choices may vary based on values and preferences | Moderate Low |
| Good practice point | Recommendation that will be helpful to a clinician but for which there is no direct supporting evidence | — |
Note: The AAFP uses a modified version of the Grading of Recommendations Assessment, Development, and Evaluation system.
AAFP = American Academy of Family Physicians.
*—Recommendations can be for or against an intervention or testing modality.
†—The strength of the recommendation should be consistent with the quality of the evidence such that strong recommendations are based on moderate- to high-quality evidence, whereas weak recommendations are based on low- to moderate-quality evidence. Very low-quality evidence should be considered insufficient for a recommendation unless there are highly unusual circumstances and the benefits would greatly outweigh the harms.
The quality of evidence is based on the certainty of the evidence where high-quality evidence means the authors have high certainty in the estimate of effect and additional studies will most likely not change the outcome.25,26 Low-quality evidence means the authors have lower certainty in the estimate of effect and that additional studies may likely change the result.
The AAFP also issues guideline recommendations without a rating when appropriate (e.g., those that will be helpful to a clinician but for which there is no direct evidence to support the recommendation), which the AAFP labels good practice points.26,27 No good practice points were considered for this guideline.
The guideline development group prioritized patient-oriented clinical outcomes, which included total mortality, cardiovascular-related mortality, cardiovascular events (e.g., stroke, myocardial infarction), and adverse events. A GRADE evidence table was constructed for these outcomes based on the Arguedas, et al., review (Table 2).18 The wording of the recommendations reflects the strength and direction of the recommendation, and the quality of the evidence was listed parenthetically. Recommendations were finalized based on consensus of the guideline development group after completion of GRADE evidence-to-decision framework, which enabled consideration of the strength of the evidence in addition to issues of feasibility, acceptability, equity, and patient preferences and values (Table 3).
TABLE 2. GRADE Evidence Table: Patient-oriented Clinical Outcomes
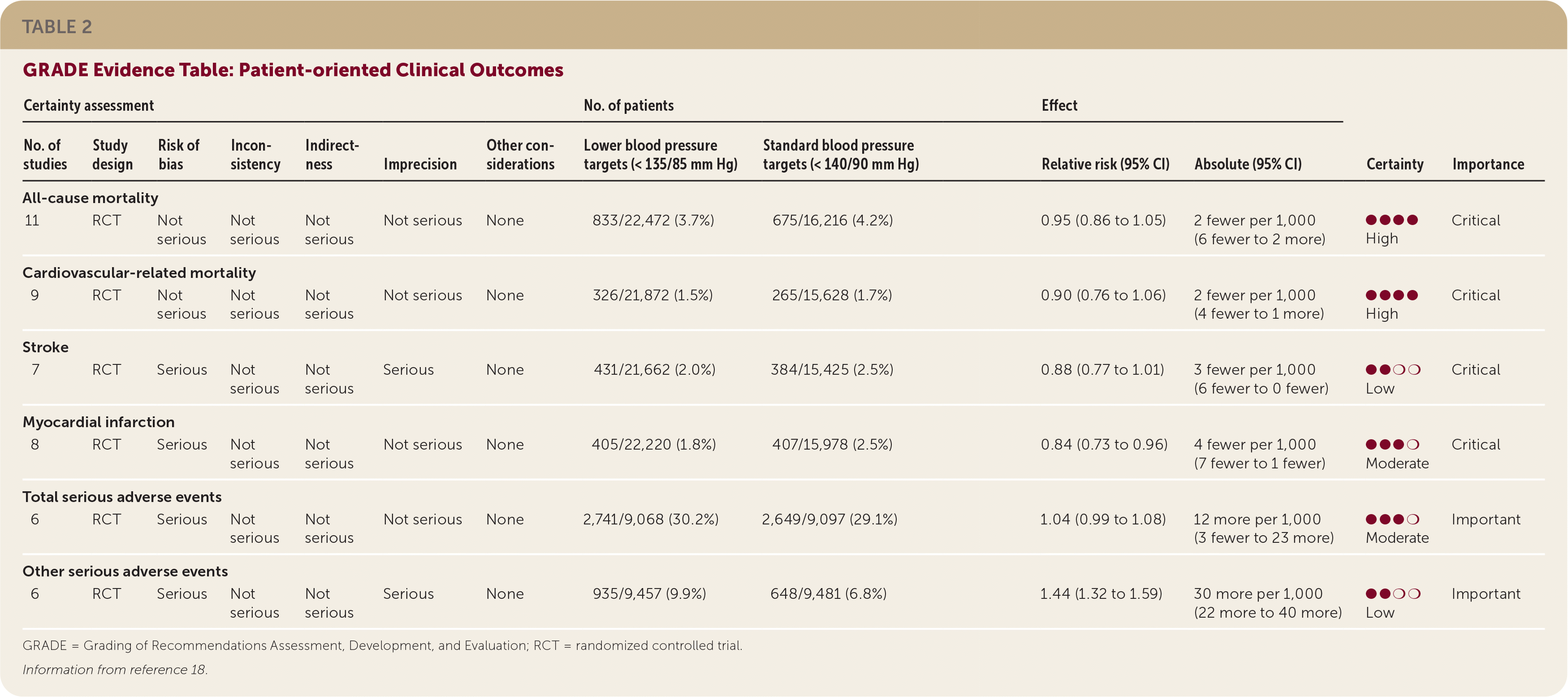
| Certainty assessment | No. of patients | Effect | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No. of studies | Study design | Risk of bias | Inconsistency | Indirectness | Imprecision | Other considerations | Lower blood pressure targets (< 135/85 mm Hg) | Standard blood pressure targets (< 140/90 mm Hg) | Relative risk (95% CI) | Absolute (95% CI) | Certainty | Importance |
| All-cause mortality | ||||||||||||
| 11 | RCT | Not serious | Not serious | Not serious | Not serious | None | 833/22,472 (3.7%) | 675/16,216 (4.2%) | 0.95 (0.86 to 1.05) | 2 fewer per 1,000 (6 fewer to 2 more) | ●●●● High | Critical |
| Cardiovascular-related mortality | ||||||||||||
| 9 | RCT | Not serious | Not serious | Not serious | Not serious | None | 326/21,872 (1.5%) | 265/15,628 (1.7%) | 0.90 (0.76 to 1.06) | 2 fewer per 1,000 (4 fewer to 1 more) | ●●●● High | Critical |
| Stroke | ||||||||||||
| 7 | RCT | Serious | Not serious | Not serious | Serious | None | 431/21,662 (2.0%) | 384/15,425 (2.5%) | 0.88 (0.77 to 1.01) | 3 fewer per 1,000 (6 fewer to 0 fewer) | ●●❍❍ Low | Critical |
| Myocardial infarction | ||||||||||||
| 8 | RCT | Serious | Not serious | Not serious | Not serious | None | 405/22,220 (1.8%) | 407/15,978 (2.5%) | 0.84 (0.73 to 0.96) | 4 fewer per 1,000 (7 fewer to 1 fewer) | ●●●❍ Moderate | Critical |
| Total serious adverse events | ||||||||||||
| 6 | RCT | Serious | Not serious | Not serious | Not serious | None | 2,741/9,068 (30.2%) | 2,649/9,097 (29.1%) | 1.04 (0.99 to 1.08) | 12 more per 1,000 (3 fewer to 23 more) | ●●●❍ Moderate | Important |
| Other serious adverse events | ||||||||||||
| 6 | RCT | Serious | Not serious | Not serious | Serious | None | 935/9,457 (9.9%) | 648/9,481 (6.8%) | 1.44 (1.32 to 1.59) | 30 more per 1,000 (22 more to 40 more) | ●●❍❍ Low | Important |
GRADE = Grading of Recommendations Assessment, Development, and Evaluation; RCT = randomized controlled trial.
Information from reference 18.
TABLE 3. Should Lower (< 135/85 mm Hg) vs. Standard (< 140/90 mm Hg) Blood Pressure Targets Be Used for Adults With Hypertension?
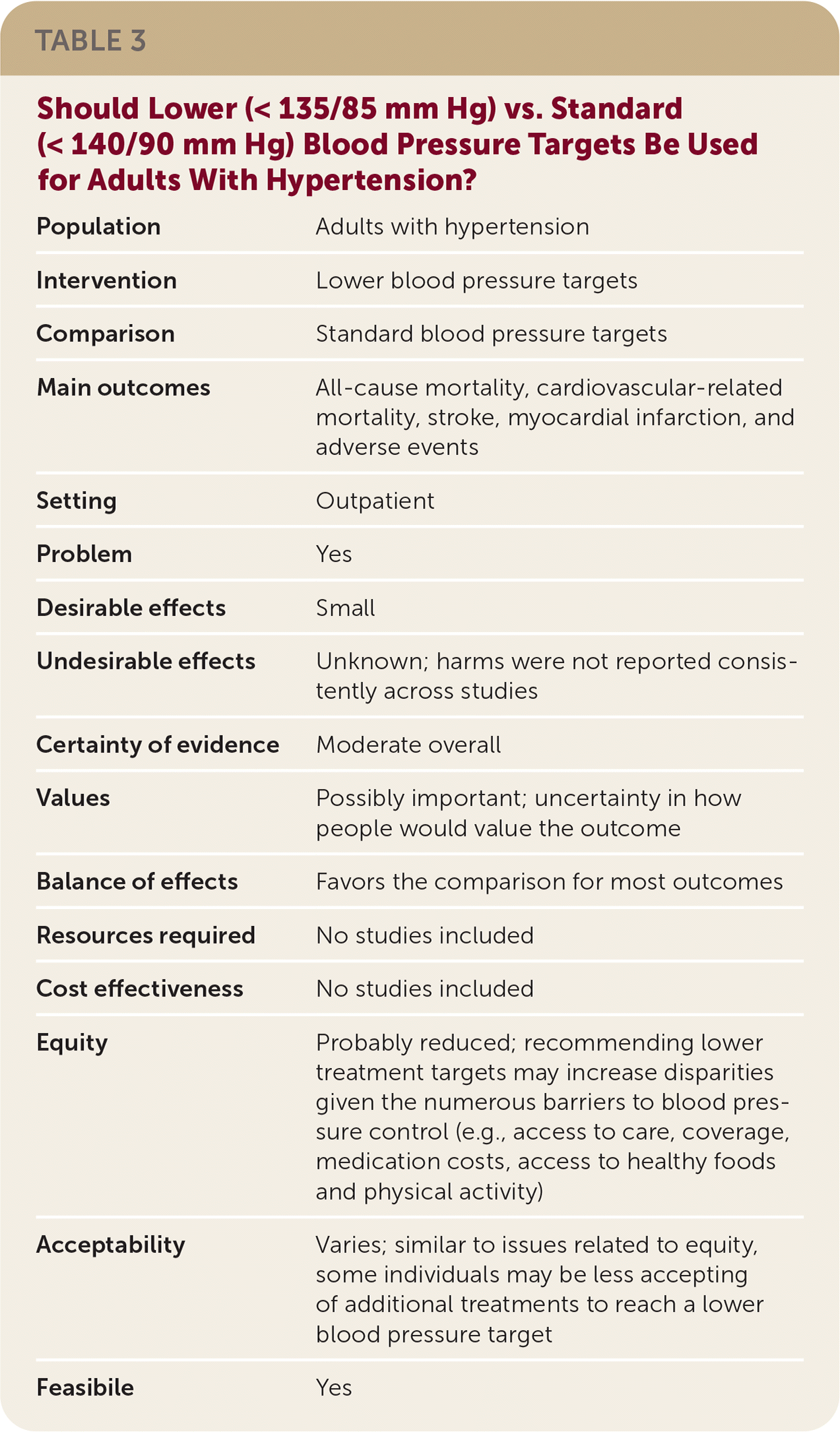
| Population | Adults with hypertension |
| Intervention | Lower blood pressure targets |
| Comparison | Standard blood pressure targets |
| Main outcomes | All-cause mortality, cardiovascular-related mortality, stroke, myocardial infarction, and adverse events |
| Setting | Outpatient |
| Problem | Yes |
| Desirable effects | Small |
| Undesirable effects | Unknown; harms were not reported consistently across studies |
| Certainty of evidence | Moderate overall |
| Values | Possibly important; uncertainty in how people would value the outcome |
| Balance of effects | Favors the comparison for most outcomes |
| Resources required | No studies included |
| Cost effectiveness | No studies included |
| Equity | Probably reduced; recommending lower treatment targets may increase disparities given the numerous barriers to blood pressure control (e.g., access to care, coverage, medication costs, access to healthy foods and physical activity) |
| Acceptability | Varies; similar to issues related to equity, some individuals may be less accepting of additional treatments to reach a lower blood pressure target |
| Feasibile | Yes |
Patient/Consumer Perspective
Patient preferences and perspective were sought during all stages of guideline development. A panel of three patient representatives was convened to provide input on the prioritization of outcomes, evidence-to-decision framework, the draft recommendations, and peer review comments on the guideline. Additional input was obtained from disease advocacy organizations during the external peer review process.
Peer Review
The guideline was peer reviewed by relevant internal and external stakeholders, including representatives from family medicine, cardiology, internal medicine, and patients. All comments and any modifications based on those comments were documented. The AAFP Commission on Health of the Public and Science and Board of Directors reviewed and approved the final version of the guideline.
Conflict of Interest
The AAFP considers financial and intellectual conflicts of interest (COI), which were solicited in writing at the beginning of the guideline process and updated verbally at each subsequent call. No panel member disclosed any COI. Policies for disclosures and management of COI are outlined in the AAFP Clinical Practice Guideline Manual.23
Guideline Updating
All AAFP guidelines are scheduled for review five years after completion. Guidelines are reviewed at a shorter interval of time if new evidence becomes available. This process is managed through the Commission on Health of the Public and Science. Following review, the AAFP determines whether the guideline should be reaffirmed, updated, or deleted from the website. All current guidelines developed by the AAFP are available to the public at https://www.aafp.org/family-physician/patient-care/clinical-recommendations.html.
Recommendations
RECOMMENDATION 1
The AAFP strongly recommends clinicians treat adults who have hypertension to a standard blood pressure target (less than 140/90 mm Hg) to reduce the risk of all-cause and cardiovascular mortality (strong recommendation; high-quality evidence). Treating to a lower blood pressure target (less than 135/85 mm Hg) does not provide additional benefit at preventing mortality; however, a lower blood pressure target could be considered based on patient preferences and values.
High-quality evidence showed that treatment of blood pressure to a target of less than 140/90 mm Hg reduced the risk of total and cardiovascular mortality (Table 2).18 Treating to a lower blood pressure target (less than 135/85 mm Hg) does not provide any additional mortality benefit. The Cochrane review conducted by Arguedas, et al., evaluated the effect on total mortality between treatment to standard (less than 140/90 mm Hg) and lower blood pressure targets (less than 135/80 mm Hg).18 It included 11 RCTs with 38,688 patients and a mean follow-up of 3.7 years.18 Most trials included patients with an additional cardiovascular risk factor and approximately 23.7% of participants had existing CVD. In trials examining systolic blood pressure targets, 120 mm Hg was the lower target in four trials,28–31 and 130 mm Hg was the lower target in three trials.32–34 Four trials examined diastolic blood pressure, and lower targets were defined from 65 to 80 mm Hg.35–38 The pooled effect size showed no significant difference in total mortality between the groups (relative risk [RR] = 0.95; 95% CI, 0.86 to 1.05).18 No significant difference in mortality was noted when examining systolic or diastolic blood pressure targets independently. The systematic review included seven studies evaluating systolic blood pressure with 19,013 patients and found no improvement in total mortality to a lower target (RR = 0.91; 95% CI, 0.80 to 1.04).28–34 The review included four studies evaluating diastolic blood pressure targets and found no improvement when treating to a lower target (RR = 1.02; 95% CI, 0.86 to 1.20).35–38 Nine studies with 37,500 participants evaluated cardiovascular mortality and found no improvement when treating to a lower target (RR = 0.90; 95% CI, 0.76 to 1.06).18 As with total mortality, there continued to be no significant difference in subgroup analysis of lower systolic blood pressure (RR = 0.81; 95% CI, 0.65 to 1.02) or diastolic blood pressure targets (RR = 1.01; 95% CI, 0.80 to 1.29).18
The systematic review found no significant difference (Table 2) in total serious adverse events between the lower and standard target groups (RR = 1.04; 95% CI, 0.99 to 1.08).18 The review defined serious adverse events as death, life-threatening event, required hospitalizations or prolonged existing hospitalization, resulting in persistent and significant disability, or required intervention to prevent permanent impairment or damage. Of note, only six studies included serious adverse events as an outcome, and there was inconsistent reporting of harms across the included studies.28,29,31,32,34,36 There was a significant increase in all other adverse events (e.g., syncope, hypotension) when treating to a lower systolic target (RR = 1.44; 95% CI, 1.32 to 1.59). This subgroup analysis included six trials with 18,938 participants and was rated as low-quality evidence. The lower target group had an absolute risk increase of 3% of all other serious adverse events compared with the standard target group (9.8% vs. 6.8%). This is a number needed to harm of 33 over 3.7 years. Additional use of medication is also a potential harm. In Arguedas, et al., individuals in the lower target group required an average of one additional medication.18 Increased medication burden can increase cost, medication adverse effects, and drug-drug interactions. These results are consistent with data from the two largest trials, ACCORD and SPRINT.28,29 The ACCORD trial found that treating to a systolic blood pressure of less than 120 mm Hg increased adverse events attributed to blood pressure medications (RR = 2.58; 95% CI, 1.70 to 3.91), resulting in a number needed to harm of 50 over 4.7 years.28 The SPRINT trial also demonstrated increased adverse events in the lower blood pressure target groups (RR = 1.87; 95% CI, 1.50 to 2.33) and a number needed to harm of 46 every 3.3 years.29 This included a 1.2% absolute increase in acute kidney injury caused by medication.29
Similar results were observed in another 2020 Cochrane systematic review by Saiz, et al., looking at patients with hypertension and CVD.22 Whereas the Arguedas, et al., review focuses more on adults in the general population, the Saiz, et al., review was specific for adults with hypertension and CVD. The trials in this review included individuals who had a history of myocardial infarction, stroke (not including transient ischemic attack), chronic peripheral vascular occlusive disease, or angina pectoris. This review also included adults who had diabetes and impaired kidney function. In this review, six trials with 9,484 participants evaluated total mortality and found moderate-quality evidence that there is no benefit to lower blood pressure target (less than 135/85 mm Hg) compared with the standard target (less than 140/90 mm Hg) (RR = 1.06; 95% CI, 0.91 to 1.23). There was also no difference in cardiovascular specific mortality (RR = 1.03; 95% CI, 0.82 to 1.29). Subgroup analysis equally found no improvement in total or cardiovascular mortality for lower blood pressure targets for individuals with diabetes. Saiz, et al., also found no difference in serious adverse events but noted more withdrawals due to adverse events in the lower target group (RR = 8.16; 95% CI, 2.06 to 32.28).22
One multicenter RCT from China (STEP trial) with 8,511 participants was published following the included Cochrane review that randomized patients 60 to 80 years of age with hypertension to a systolic blood pressure target of 110 to 130 mm Hg or a target of 130 to 150 mm Hg.20 This study also found no difference in death from any cause (RR = 1.11; 95% CI, 0.78 to 1.56) or death from cardiovascular causes (RR = 0.72; 95% CI, 0.39 to 1.32).20
RECOMMENDATION 2
The AAFP recommends clinicians consider treating adults who have hypertension to a lower blood pressure target (less than 135/85 mm Hg) to reduce risk of myocardial infarction (weak recommendation; moderate-quality evidence). Although treatment to a standard blood pressure target (less than 140/90 mm Hg) reduced the risk of myocardial infarction, there was a small additional benefit observed with a lower blood pressure target. There was no observed additional benefit in preventing stroke with the lower blood pressure target.
Low-quality evidence showed no significant reduction in incidence of stroke between the lower and standard blood pressure groups (Table 2).18 The Arguedas, et al., systematic review included seven trials and 37,087 participants evaluating this outcome and found a slight reduction in stroke when looking only at the systolic blood pressure subgroup analysis (RR = 0.80; 95% CI, 0.67 to 0.94).18 When diastolic blood pressure studies were included in the pooled analysis, there was no significant difference between the groups (RR = 0.88; 95% CI, 0.77 to 1.01). This is low-quality evidence due to the high degree of heterogeneity between the subgroups and serious risk of bias of the included studies. Additional post-intervention data from the SPRINT trial were published after completion of the Arguedas, et al., review. Although additional events in the composite outcome were observed, there were no differences in mortality, stroke, or myocardial infarction between the treatment groups.39 The STEP trial also found a reduction in stroke when treating to a lower systolic blood pressure target of 110 to 130 mm Hg (RR = 0.67; 95% CI, 0.47 to 0.97).20 However, the study was discontinued early, which may exaggerate the beneficial effect. The Saiz, et al., review did not evaluate stroke as an independent variable but included a composite of fatal and nonfatal cardiovascular events (including myocardial infarction, stroke, sudden death, hospitalization or death from congestive heart failure, or other significant vascular events).22 There was no difference between the lower and standard target groups for this composite outcome (RR = 0.89; 95% CI, 0.80 to 1.00).22
Moderate-quality evidence showed treating adults who have hypertension to a lower blood pressure target (less than 135/85 mm Hg) further reduced the risk of myocardial infarction. In the included systematic review, eight RCTs (n = 38,198) evaluated the incidence of myocardial infarction in patients treated with a lower target compared with those with a standard target.18 Compared with standard targets, lower targets decreased the risk of myocardial infarction (2.55% vs. 1.82%; RR = 0.84; 95% CI, 0.73 to 0.96) with a number needed to treat of 137 over 3.7 years. Per 1,000 patients, lower targets resulted in four fewer myocardial infarction events compared with standard targets.
Similar to stroke, myocardial infarction was not evaluated as a separate outcome in the Saiz, et al., review for patients with CVD.22 The STEP trial also used a composite primary outcome (including stroke, acute coronary syndrome [myocardial infarction and hospitalization for unstable angina], acute decompensated heart failure, coronary revascularization, atrial fibrillation, or death from a cardiovascular cause).20 In this trial, most patients had elevated cardiovascular risk, as determined by the Framingham Risk Score. This study found a reduction in the primary outcome for lower blood pressure target group (RR = 0.74; 95% CI, 0.60 to 0.92) as well as reduction in stroke (RR = 0.67; 95% CI, 0.47 to 0.97) and acute coronary syndrome (RR = 0.67; 95% CI, 0.47 to 0.94).20 As mentioned previously, there was no reduction in mortality, and this trial was stopped early, which may exaggerate the benefits and minimize the harms.
Clinicians should employ shared decision-making and consider patient values, goals, and preferences when considering blood pressure targets to reduce the risk of myocardial infarction. Although the potential for a small decrease in myocardial infarction risk at lower blood pressure targets occurs, there is also the potential for increased harms, as described previously. Shared decision-making conversations should consider additional clinical risk factors of myocardial infarction, alternative measures to reduce risk (such as smoking cessation and lifestyle modification), harms of medication regimens, costs, and impact of treatment options on the lives of patients and their families. Because of the small additional clinical benefit, patient values, preferences, and goals are critical and may significantly alter each individual’s decision-making.
Implementation of Recommendations
BARRIERS TO IMPLEMENTATION
There may be several barriers to effective implementation of these recommendations at the patient-clinician, practice, and community levels. At the patient level, there could be a barrier of costs for office visits and additional medications. Insurance coverage of home blood pressure monitoring systems may vary, and individuals without insurance may find necessary equipment cost prohibitive. Patients may need instructions on home monitoring, calibration of home machines, and parameters for when to call their clinician.
At the practice or community level, recommendations of blood pressure goals may differ between specialties, creating confusion for patients and the care team. Addressing racial, socioeconomic, and geographic disparities should be considered when implementing any guideline recommendations. Lack of access to health care services, in addition to other social determinants of health that affect patients, could be a significant impediment to implementation of these recommendations.
TECHNIQUES FOR IMPLEMENTATION
Vital signs are standard at most clinic visits, so assessing blood pressure is routine for most clinicians and patients. Workflows should be established to allow for accurate blood pressure measurements. This could include allowing patients to sit for several minutes in the room to acclimate, purchasing and using appropriately sized blood pressure cuffs, and taking blood pressure measurements at multiple time points during the visit.
Because patients may receive different recommendations from specialists and health care systems regarding blood pressure targets, family physicians and specialists should collaborate and coordinate care. Large health groups may benefit from multispecialty discussions to create consistent messaging for patients.
Additionally, clinicians should discuss patient preferences and access to services when recommending treatment options. Insights from the patient panel demonstrated that there are important differences in how individuals value the potential benefits and harms. Treatment plans should involve shared decision-making that considers individual goals for blood pressure control and potential harms and adverse effects of medications. The potential impacts on work, home, and family are important considerations when deciding on a treatment plan. A patient’s occupation, support structures, or comorbid conditions may alter the patient’s risk tolerance or ability and willingness to accept treatment adverse effects. Patient risk for CVD should be incorporated into shared decision-making, and treatment options should include risk-reduction measures. Multiple cardiovascular risk assessment tools are available to assist in patient-centered treatment discussions, but many are limited by their use of race as a risk factor. Patients should be actively engaged in decision-making when determining blood pressure targets, and these targets should be frequently reassessed to ensure that changes in patient values and preferences are incorporated into treatment planning.
When planning implementation strategies, clinicians and health policy makers should be conscious of how social determinants of health can affect patient care. The U.S. Preventive Services Task Force recommends that patients with cardiovascular risk factors, such as elevated blood pressure, be referred for or given counseling on healthy diet and physical activity.40 The AAFP supported this recommendation. Access to healthy foods, safe environments for exercise, spaces to cook and store healthy foods, and budgetary considerations varies from patient to patient and may make implementation of lifestyle changes challenging. To help patients achieve the desired blood pressure target, individualized strategies must be used. Educational material about hypertension, medications, and lifestyle interventions should be at appropriate literacy levels and available in multiple languages. Practices should consider screening for social determinants of health and help address those issues by connecting patients to community resources. Screening tools and resource databases are available from the AAFP’s EveryOne Project (www.aafp.org/everyone).
Home monitoring may facilitate telemedicine follow-up, increasing opportunities for patients to seek care in multiple modalities. Home blood pressure monitoring may also help distinguish those patients with white coat hypertension from those with hypertension after an elevated office blood pressure reading and for those with masked hypertension with normal office blood pressure levels and elevated blood pressures at home.16 It is important for electronic blood pressure devices to be compared with an office blood pressure reading on an annual basis to ensure accuracy. Expert opinion based on American Heart Association guidelines recommends the use of an appropriately sized upper-arm cuff on a bare arm.41 While measuring blood pressure, a patient’s feet should be flat on the floor and the arm supported with the cuff at the level of the heart. It is recommended that a patient’s bladder be empty, that caffeinated beverages be avoided for 30 minutes prior, and that the patient rest for five minutes before measuring blood pressure. Multiple readings in the morning and evenings, taken at least one minute apart, can be averaged (https://www.cdc.gov/bloodpressure/measure.htm). Patients should check with their insurance plans to see whether a home blood pressure monitor is a covered benefit.
Until recently, clinicians have been taught that certain blood pressure medications should be used preferentially in certain racial groups. Because it is well documented that race is a social construct, the AAFP encourages family physicians to be aware of the inappropriate use of race as a proxy for biology or genetics in clinical decision-making42,43 (https://www.aafp.org/about/policies/all/racebased-medicine.html).
Limitations of the Guideline
The guideline development group acknowledges that there were several limitations in evidence used to inform the guideline recommendations, including the following:
- Heterogeneity in participants’ risk of cardiovascular events across trials
- Different blood pressure targets in the groups assigned to lower targets
- No analysis of benefits and harms of specific antihypertensive drug classes
- Lack of consistent reporting of harms across trials
Conclusions and Future Research
The purpose of this guideline is to provide clinical recommendations for primary care physicians on blood pressure goals for adult patients with and without existing CVD. The AAFP recommends primary care clinicians treat adults with hypertension to a standard blood pressure target (less than 140/90 mm Hg) because there was no additional benefit to reduce risk of all-cause or cardiovascular mortality or stroke compared with a lower blood pressure target (less than 135/85 mm Hg). The AAFP also recommends primary care clinicians consider treating adults with hypertension to a lower blood pressure target (less than 135/85 mm Hg) to reduce risk of myocardial infarction. Treatment decisions should be based on clinical judgment, as well as patient preferences and values, and involve shared decision-making by the patient and clinician. Variation exists across specialty society guidelines, with some recommending lower blood pressure targets regardless of age. However, it should be noted that lower blood pressure targets are not recommended across all guidelines, and the recommendations outlined here are consistent with recommended blood pressure targets from others (Table 410,11,13–16,44 ). The AAFP acknowledges that this variation presents a challenge to clinicians and patients. The care team, including the patient, should develop a treatment plan to lower blood pressure to an achievable target that provides benefit while minimizing harms in accordance with patient goals and preferences. A recent study from the United Kingdom suggested that a decrease of 5 mm Hg resulted in decreased risk of cardiovascular events, which supports a role for minor reductions in blood pressure providing benefit even if targets are not met.19
TABLE 4. Comparison of Recommended Blood Pressure Targets in Recent Guidelines
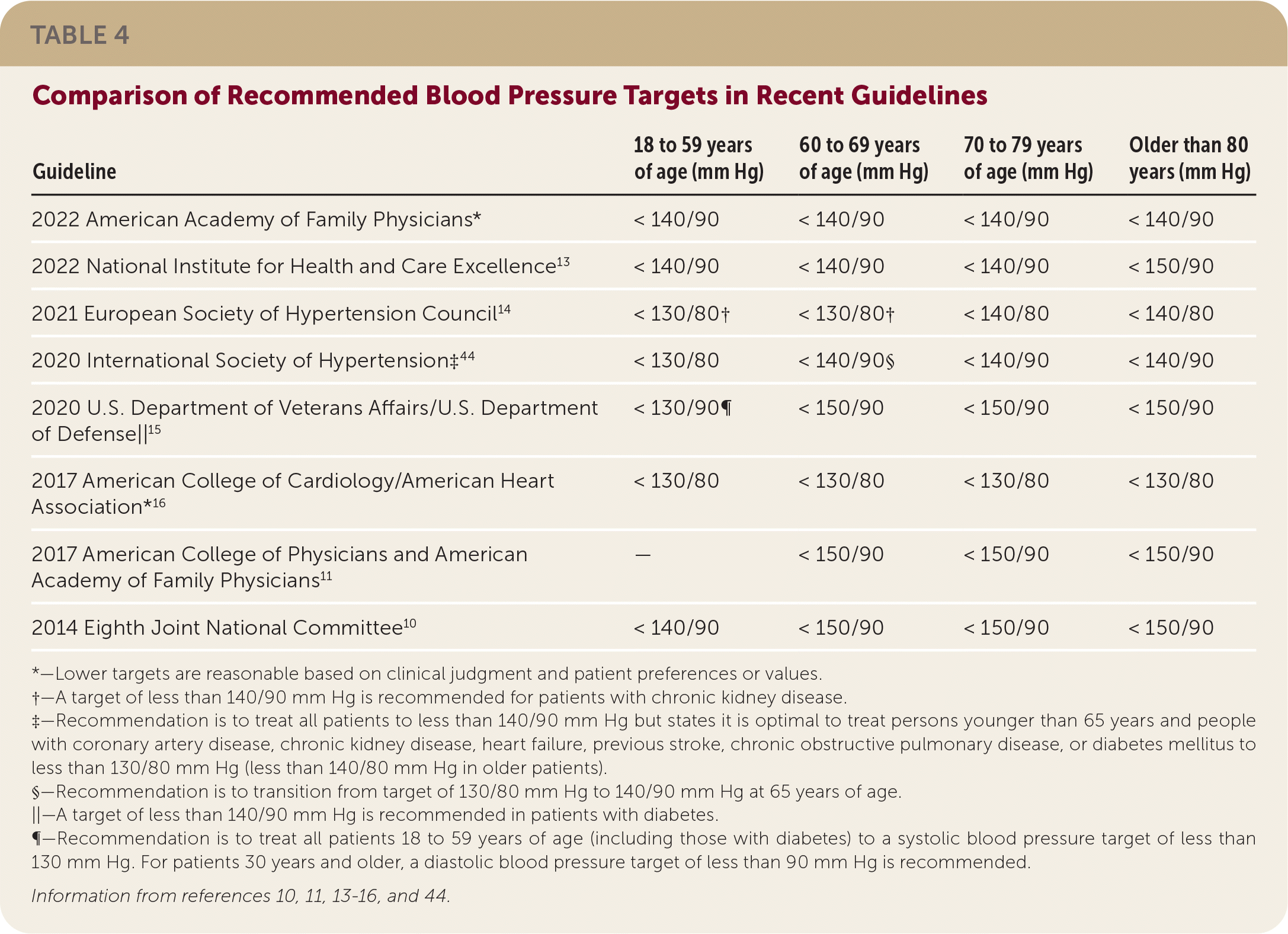
| Guideline | 18 to 59 years of age (mm Hg) | 60 to 69 years of age (mm Hg) | 70 to 79 years of age (mm Hg) | Older than 80 years (mm Hg) |
|---|---|---|---|---|
| 2022 American Academy of Family Physicians* | < 140/90 | < 140/90 | < 140/90 | < 140/90 |
| 2022 National Institute for Health and Care Excellence13 | < 140/90 | < 140/90 | < 140/90 | < 150/90 |
| 2021 European Society of Hypertension Council14 | < 130/80† | < 130/80† | < 140/80 | < 140/80 |
| 2020 International Society of Hypertension‡44 | < 130/80 | < 140/90§ | < 140/90 | < 140/90 |
| 2020 U.S. Department of Veterans Affairs/U.S. Department of Defense||15 | < 130/90¶ | < 150/90 | < 150/90 | < 150/90 |
| 2017 American College of Cardiology/American Heart Association*16 | < 130/80 | < 130/80 | < 130/80 | < 130/80 |
| 2017 American College of Physicians and American Academy of Family Physicians11 | — | < 150/90 | < 150/90 | < 150/90 |
| 2014 Eighth Joint National Committee10 | < 140/90 | < 150/90 | < 150/90 | < 150/90 |
*—Lower targets are reasonable based on clinical judgment and patient preferences or values.
†—A target of less than 140/90 mm Hg is recommended for patients with chronic kidney disease.
‡—Recommendation is to treat all patients to less than 140/90 mm Hg but states it is optimal to treat persons younger than 65 years and people with coronary artery disease, chronic kidney disease, heart failure, previous stroke, chronic obstructive pulmonary disease, or diabetes mellitus to less than 130/80 mm Hg (less than 140/80 mm Hg in older patients).
§—Recommendation is to transition from target of 130/80 mm Hg to 140/90 mm Hg at 65 years of age.
||—A target of less than 140/90 mm Hg is recommended in patients with diabetes.
¶—Recommendation is to treat all patients 18 to 59 years of age (including those with diabetes) to a systolic blood pressure target of less than 130 mm Hg. For patients 30 years and older, a diastolic blood pressure target of less than 90 mm Hg is recommended.
This guideline was developed using available evidence; however, significant gaps were identified in the systematic review and by members of the guideline development group. New research into these areas may affect the recommendations, at which time the guideline will be updated accordingly. Research that would provide important information for the clinical questions discussed here includes the following:
- Studies evaluating longer-term outcomes of treating to a standard or lower blood pressure target.
The mean follow-up period was less than four years in the included RCTs in this guideline; it is unclear whether longer follow-up would modify these outcomes. This is particularly important for evaluating harms of long-term intensive blood pressure treatment.
- Studies examining certain subgroups in the population that may benefit from lower blood pressure targets.
Targeting to lower blood pressure goals in the general population did not appear to improve outcomes in this review; however, it is not clear whether certain subgroups in the population would benefit from lower targets.
- Studies examining harms to subgroups of patients treated to a lower blood pressure target.
This review identified a higher incidence of serious adverse events in patients treated to a lower systolic blood pressure target compared with standard systolic targets in the general population. However, inconsistent reporting of adverse events across trials occurred, and several large trials (e.g., SPRINT) were stopped early for benefit limiting the assessment of harms for intensive blood pressure treatment.
- Studies evaluating blood pressure targets in younger individuals at low risk.
The average age of the participants in the trials included in this guideline was 63 years with moderate to high cardiovascular risk. Data on younger patients are currently lacking.
- Studies evaluating the comparative benefits and harms of specific antihypertensive drug classes used to achieve blood pressure targets.
- Studies evaluating the use of ambulatory blood pressure monitoring to assess the accuracy of blood pressure readings and the relationship with blood pressure targets and outcomes using this method of measurement.
- Studies examining the social determinants of health, including systemic racism, that contribute to health care disparities and blood pressure goals and management to reduce adverse cardiovascular outcomes.
- Studies into the development of risk assessment calculators, algorithms, and tools that do not rely on race as a proxy for biology or genetics.
Editor's Note: Dr. Lin is deputy editor for AFP.
The authors thank Ms. Karen Campbell, Dr. Kam Hunter, and Dr. Gary Bird for serving on the patient/consumer panel for this guideline.
All costs associated with the development of this guideline came exclusively from the operating budget of the AAFP.
APPROVED BY THE AAFP BOARD OF DIRECTORS: July 21, 2022
Disclaimer: These recommendations are provided only as assistance for clinicians making clinical decisions regarding the care of their patients. As such, they cannot substitute for the individual judgment brought to each clinical situation. As with all clinical reference resources, they reflect the best understanding of the science of medicine at the time of publication, but they should be used with the clear understanding that continued research may result in new knowledge and recommendations. All AAFP guidelines are scheduled for review five years after completion or earlier if new evidence becomes available.

