
Am Fam Physician. 2023;107(4):353-354
Author disclosure: No relevant financial relationships.
Clinical Question
Can magnetic resonance imaging (MRI) accurately diagnose acute appendicitis?
Evidence-Based Answer
In pregnant patients, children, and adults with clinical signs and symptoms of appendicitis, MRI has an overall sensitivity of 95% and specificity of 96%. The posttest probability of having appendicitis after a positive MRI is 90% and 2% after a negative MRI, assuming a median pretest probability of 25%.1 (Strength of Recommendation: B, inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
Appendicitis is the most common abdominal surgical emergency, leading to more than 300,000 appendectomies in the United States each year.2 Timely diagnosis and treatment of acute appendicitis based on clinical findings and radiographic imaging reduce the risk of complications, including perforation, sepsis, peritonitis, and death.3 Ultrasonography is an appropriate option in some circumstances.4,5 If MRI is accurate in the diagnosis of appendicitis, avoiding ionizing radiation exposure makes it an attractive option, especially in pregnant patients and children. The authors of the Cochrane review sought to assess the accuracy of MRI in diagnosing acute appendicitis in all patients, with subgroup analysis of pregnant patients, children, and adults, as a secondary outcome.
The review included 58 studies with a total of 7,462 patients from 12 countries (35 studies were conducted in the United States). All studies were observational (cohort or cross-sectional) or randomized test accuracy studies. Case-control studies and studies with fewer than 10 patients were excluded. Most studies (39) were retrospective. Studies included children (n = 2,794), pregnant patients (n = 2,282), and adults (n = 1,088) presenting to an acute or emergency setting who underwent MRI for clinical suspicion of appendicitis. Radiographic findings were compared with histologic analysis of appendix specimens following surgery. Appendicitis was considered not present in patients who underwent surgery without appendectomy due to a normal appearing appendix or who were discharged without treatment and had an uneventful follow-up.1
Among patients in the meta-analysis, 27% met criteria for acute appendicitis. Pooled analysis showed that MRI is highly sensitive (95%; 95% CI, 94% to 97%) and specific (96%; 95% CI, 95% to 97%). At an estimated median prevalence of 25%, the posttest probability of acute appendicitis was 90% (95% CI, 85% to 93%) following a positive MRI and 2% (95% CI, 1% to 3%) following a negative MRI. This suggests that in a theoretical cohort of 1,000 patients with suspected appendicitis who have an MRI, 250 patients would be diagnosed with suspected appendicitis. Of those with a positive MRI who had an appendectomy, 12 (5%) would not have appendicitis. Of the 750 patients with a negative MRI, 30 (4%) would have appendicitis.1
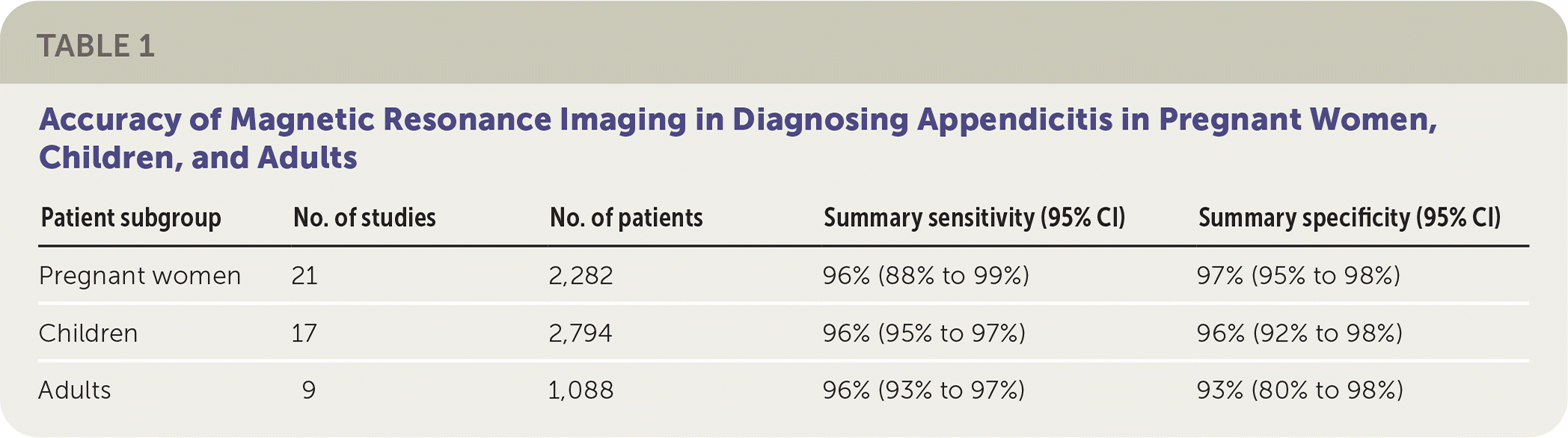
Secondary outcomes examined subgroups of pregnant patients, children, and adults (Table 1). Sensitivity and specificity of MRI for the diagnosis of acute appendicitis remained high in each subgroup. Only three studies compared MRI protocols, mainly assessing MRI with or without intravenous or oral contrast; a meta-regression analysis found no difference.1
| Patient subgroup | No. of studies | No. of patients | Summary sensitivity (95% CI) | Summary specificity (95% CI) |
|---|---|---|---|---|
| Pregnant women | 21 | 2,282 | 96% (88% to 99%) | 97% (95% to 98%) |
| Children | 17 | 2,794 | 96% (95% to 97%) | 96% (92% to 98%) |
| Adults | 9 | 1,088 | 96% (93% to 97%) | 93% (80% to 98%) |
The included studies reported methodologic weaknesses in study designs and low standards of reporting. The review was limited because it included mostly retrospective studies that relied on chart review as the reference standard for patients with a negative MRI who did not undergo surgery. The design cannot account for patients diagnosed with appendicitis after discharge if presenting to another medical facility for follow-up. Given the low incidence of false-negative results, this may overestimate sensitivity even if a small number of such events occurred. In practice, access, cost, and patient challenges in tolerating imaging may affect the use of MRI for acute appendicitis.
A meta-analysis of computed tomography suggests that at an estimated pretest prevalence of 43%, the sensitivity ranges from 91% to 96% and specificity ranges from 93% to 95% depending on the use of contrast.6 Small studies suggest that ultrasonography is not as useful, with a sensitivity of 84% and specificity of 83%.7 The American College of Radiology Appropriateness Criteria recommends imaging with computed tomography as the first-line modality in most cases of suspected appendicitis in nonpregnant adults and MRI as a second-line alternative in most patients.4 In line with the Cochrane review, MRI is recommended as a first-line option in pregnant patients due to the absence of ionizing radiation. The American College of Radiology recommends initial imaging in children based on the level of clinical risk; when there is intermediate clinical risk, ultra-sonography is labeled “usually appropriate,” whereas MRI “may be appropriate.”5 MRI would be considered “usually appropriate” as the next step in the setting of nondiagnostic ultrasonography.5
The practice recommendations in this activity are available at https://www.cochrane.org/CD012028.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force, the U.S. Department of Defense, or the U.S. government.
