A 44-year-old woman presented to the emergency department with a two-day history of lower lip swelling. She had pain and warmth in her lip but no fever, chills, or other symptoms. She had recently completed a course of trimethoprim/sulfamethoxazole for a urinary tract infection. Although she had a history of similar lower lip swelling after angiotensin-converting enzyme inhibitor use, she said she had not taken them recently. She had no history of fillers or other cosmetic treatments to the lip or face.
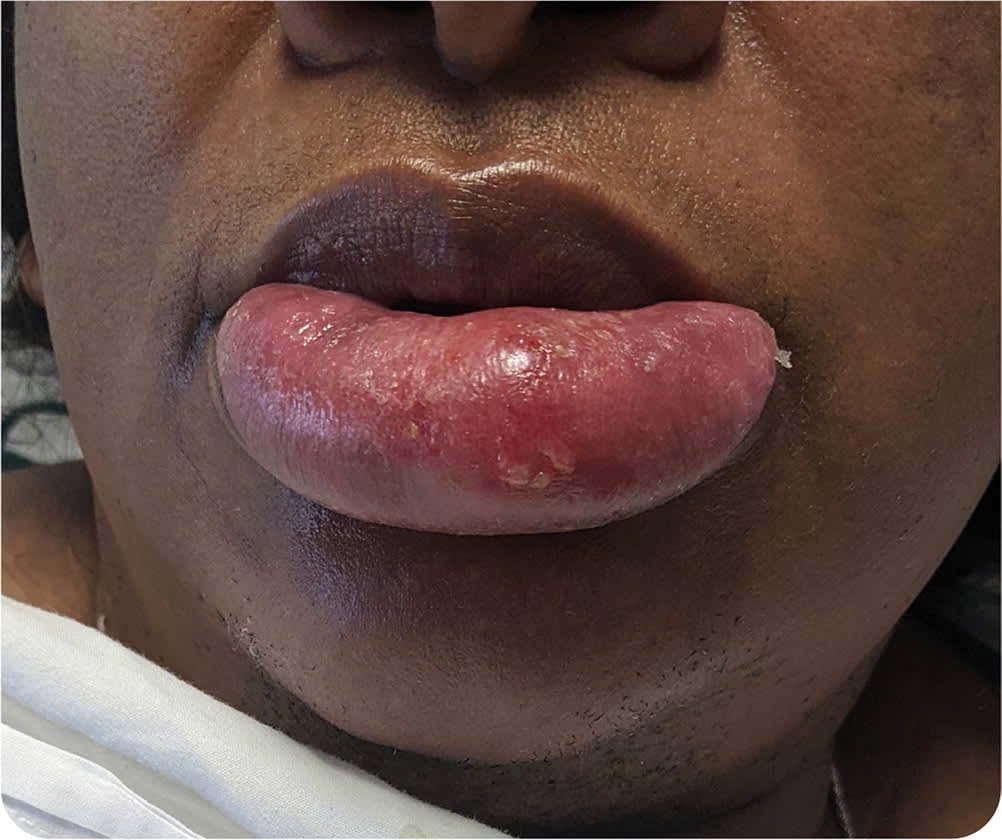
She was afebrile on physical examination. Her lower lip was edematous, and tense and tender to palpation. The exposed mucosa was dry and cracked, with scabbed-over skin just caudal to the vermilion border (Figure 1). Enlarged, mildly tender lymph nodes were palpable in her neck.
FIGURE 1
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Angioedema.
- B. Cutaneous sarcoidosis.
- C. Lip abscess.
- D. Type I hypersensitivity reaction.
Discussion
The answer is C: lip abscess. Abscesses typically present as fluctuant masses with a tract to skin. Purulent material may be expressed from a central punctum. The overlying skin is warm and may be tender to palpation. Abscesses may be secondary to skin trauma, such as at injection sites. Imaging, including ultrasonography, computed tomography, or magnetic resonance imaging, may facilitate diagnosis and identify a foreign body. Treatment typically involves incision and drainage. Antibiotic therapy may not be required for uncomplicated, superficial infections.1
Angioedema typically presents as swelling of the face or upper gastrointestinal tract without urticaria. Lesions appear nonfluctuant and erythematous, without the warmth or pruritus common with other urticarias.2 Angioedema most commonly presents as edema of both lips, and often includes the eyes. Physical examination reveals homogeneous swelling throughout the lips. Hereditary angioedema is typically inherited in an autosomal dominant pattern but can arise as a de novo mutation. Therefore, a lack of family history does not exclude this diagnosis.2 Elevated complement C4 and C1 proteins, C-reactive protein, and erythrocyte sedimentation rate suggest hereditary angioedema. Treatment typically involves steroids, antihistamines, and avoidance of the causative agent.
Cutaneous manifestations of sarcoidosis can be specific or nonspecific and may mimic other skin conditions. Specific cutaneous sarcoidosis may present as maculopapular rash, ulcers, papules, plaques, lichenoid lesions, scars, or nodules. Non-specific cutaneous sarcoidosis usually presents as erythema nodosum.3,4 Patients may report swelling, pruritus, and warmth in the affected region. Because sarcoidosis can affect multiple body systems, especially the lungs, diagnosis of cutaneous sarcoidosis should prompt further testing for multisystem disease.3 Cutaneous sarcoidosis is treated with systemic, intralesional, or topical corticosteroids.
Type I hypersensitivity reactions classically present as urticaria, flushing, pruritus, nausea, vomiting, and respiratory distress. Use of a new oral medication can cause a localized type I hypersensitivity reaction involving the lip, but diffuse, generalized cutaneous involvement is more common and typically occurs within hours of ingestion. Radioallergosorbent testing, serum tryptase measurement, and skin testing may help to diagnose type I hypersensitivity reactions. Treatment involves steroids, antihistamines, and epinephrine for anaphylaxis.5
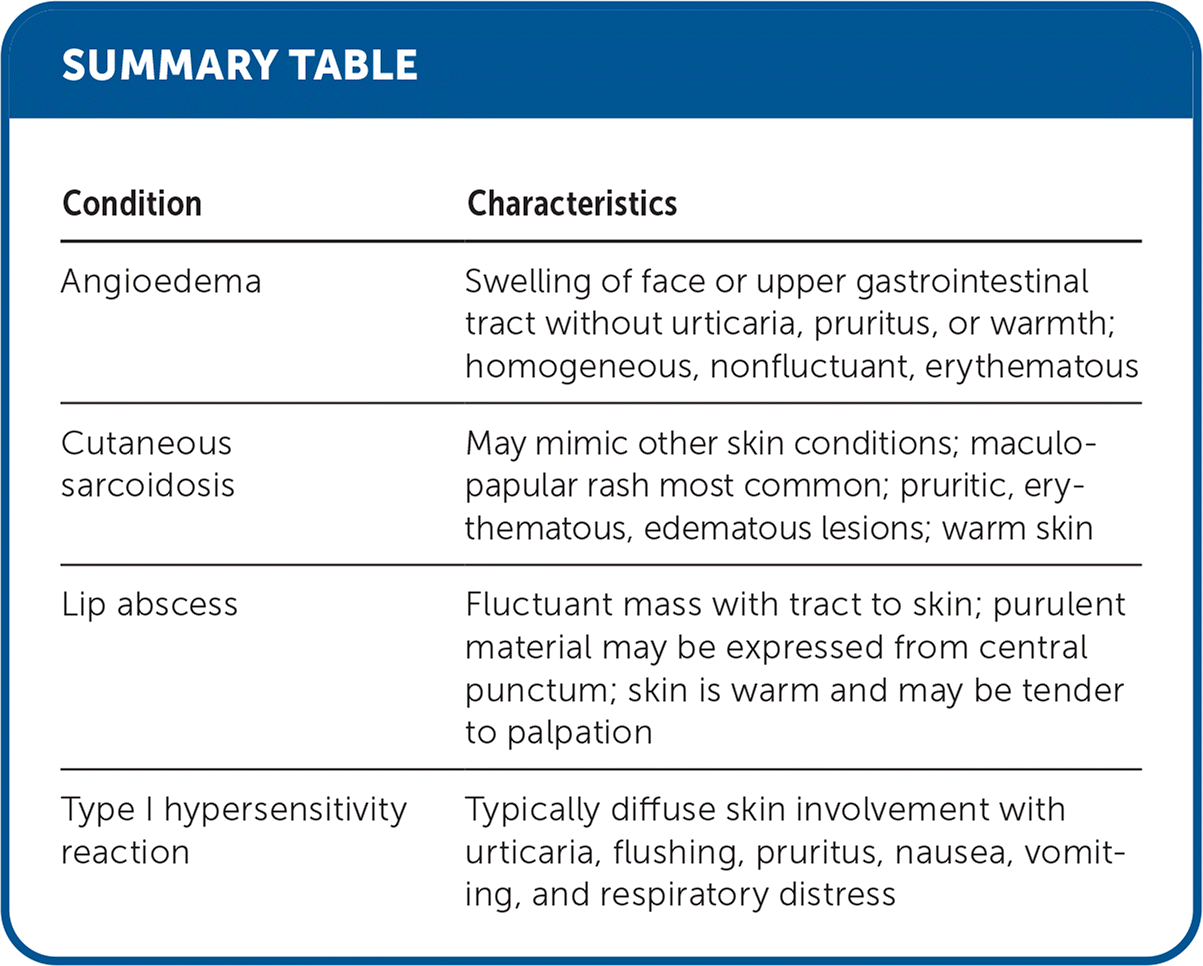
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Angioedema | Swelling of face or upper gastrointestinal tract without urticaria, pruritus, or warmth; homogeneous, nonfluctuant, erythematous |
| Cutaneous sarcoidosis | May mimic other skin conditions; maculo-papular rash most common; pruritic, erythematous, edematous lesions; warm skin |
| Lip abscess | Fluctuant mass with tract to skin; purulent material may be expressed from central punctum; skin is warm and may be tender to palpation |
| Type I hypersensitivity reaction | Typically diffuse skin involvement with urticaria, flushing, pruritus, nausea, vomiting, and respiratory distress |
The views expressed in this work are those of the authors and do not reflect the official policy or position of the Uniformed Services University of the Health Sciences, the U.S. Department of Defense, or the U.S. government.

