Well-coordinated prenatal care that follows an evidence-based, informed process results in fewer hospital admissions, improved education, greater satisfaction, and lower pregnancy-associated morbidity and mortality. Care initiated at 10 weeks or earlier improves outcomes. Identification and treatment of periodontal disease decreases preterm delivery risk. A prepregnancy body mass index greater than 25 kg per m2 is associated with gestational diabetes mellitus, hypertension, miscarriage, and stillbirth. Advanced maternal and paternal age (35 years or older) is associated with gestational diabetes, hypertension, miscarriage, intrauterine growth restriction, aneuploidy, birth defects, and stillbirth. Rho(D) immune globulin decreases alloimmunization risk in a patient who is RhD-negative carrying a fetus who is RhD-positive. Treatment of iron deficiency anemia decreases the risk of preterm delivery, intrauterine growth restriction, and perinatal depression. Ancestry-based genetic risk stratification using family history can inform genetic screening. Folic acid supplementation (400 to 800 mcg daily) decreases the risk of neural tube defects. All pregnant patients should be screened for asymptomatic bacteriuria, sexually transmitted infections, and immunity against rubella and varicella and should receive tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap), influenza, and COVID-19 vaccines. Testing for group B Streptococcus should be performed between 36 and 37 weeks, and intrapartum antibiotic prophylaxis should be initiated to decrease the risk of neonatal infection. Because of the impact of social determinants of health on outcomes, universal screening for depression, anxiety, intimate partner violence, substance use, and food insecurity is recommended early in pregnancy. Screening for gestational diabetes between 24 and 28 weeks is recommended for all patients. People at risk of preeclampsia, including those diagnosed with COVID-19 in pregnancy, should be offered 81 mg of aspirin daily starting at 12 weeks. Chronic hypertension should be treated to a blood pressure of less than 140/90 mm Hg.
Family physicians provide family-centered care for individuals and families before, during, and after the birth of a child. Well-coordinated prenatal care that follows an evidence-based, informed process results in fewer hospital admissions, improved education, greater care satisfaction, improved perinatal outcomes, and mitigates pregnancy-associated morbidity and mortality.1 Family physicians are uniquely positioned to address social determinants of health while ensuring quality of care.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
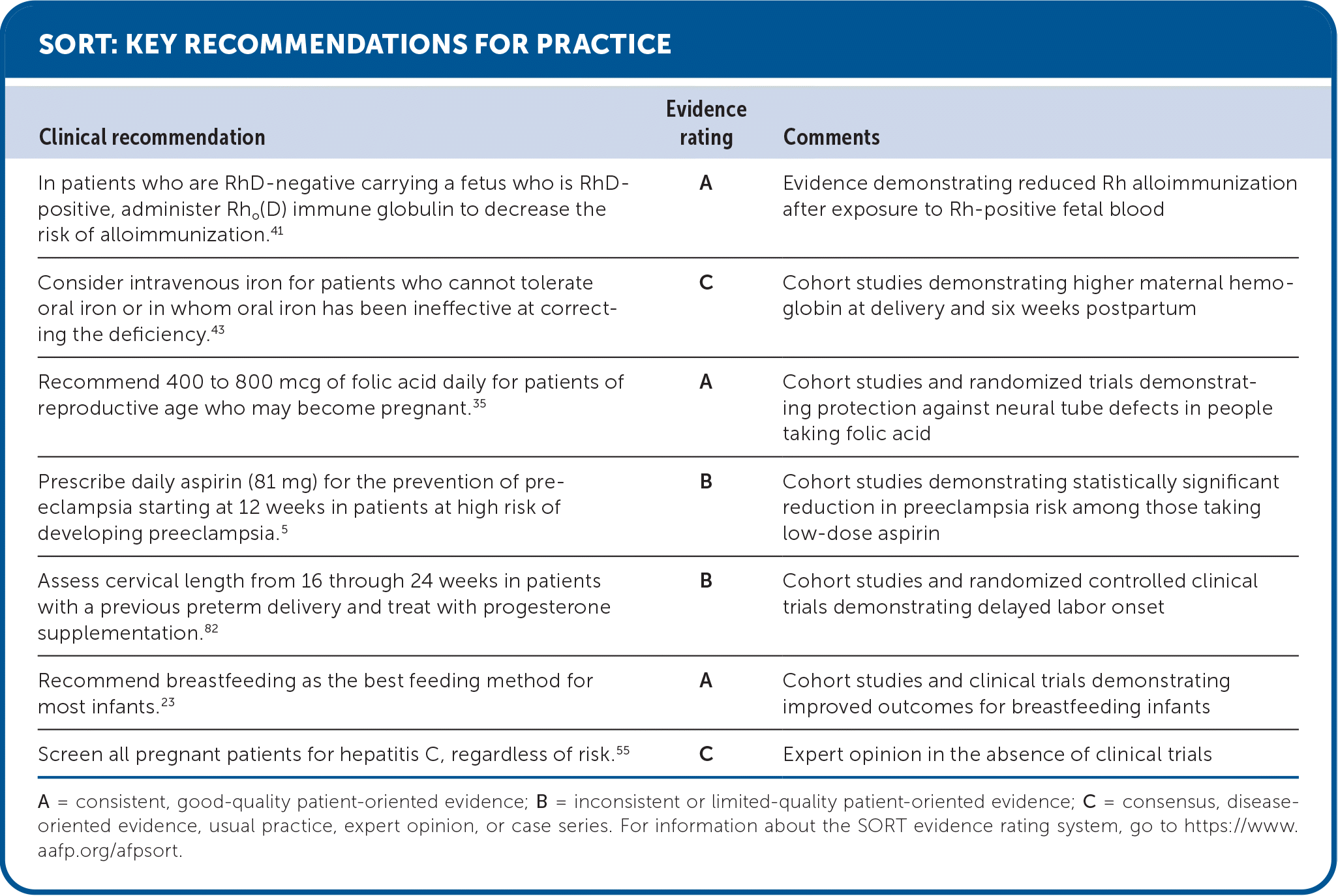
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN MATERNITY CARE

| Recommendation | Sponsoring organization |
|---|---|
| Do not perform maternal serologic studies for cytomegalovirus and toxoplasmosis as part of routine prenatal laboratory studies. | Society for Maternal-Fetal Medicine |
| Do not perform prenatal ultrasonography for nonmedical purposes (e.g., solely to create keepsake videos or photographs). | American College of Obstetricians and Gynecologists |
| Do not perform third trimester group B Streptococcus culture in patients with group B Streptococcus bacteriuria during current pregnancy. | Society for Maternal-Fetal Medicine |
Source: For more information on Choosing Wisely, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/pubs/afp/collections/choosing-wisely.html.
Prenatal Care Visits
Initiation of care between six and 10 weeks allows for identification of preexisting conditions that negatively affect maternal-fetal outcomes (e.g., diabetes mellitus, hypertension, obesity)2; however, 22% of pregnant patients do not receive care during this time.2 The COVID-19 pandemic resulted in a reevaluation of the number of physician visits needed, with an emphasis on increased flexibility, allowing for a combination of virtual and in-person visits depending on risk.3 Table 1 outlines the components of prenatal care.1,4–22 Table 2 provides opportunities for educating pregnant patients during prenatal care visits.6,8,14–19,23–29
TABLE 1. Components of Prenatal Care

| Component | Comments | ||
|---|---|---|---|
| Physical examination | |||
| Abdominal palpation1,4 | Leopold maneuvers can be used to assess fetal presentation beginning at 36 weeks | ||
| Blood pressure measurement5 | Should be assessed at each prenatal visit | ||
| Body mass index6 | Should be determined at first prenatal visit; weight should be measured at all subsequent visits | ||
| Dental health7 | Should be assessed at initial prenatal visit; treatment of periodontal disease can decrease risk of preterm delivery | ||
| Fetal heart rate1,8 | Auscultation should be performed at each prenatal visit to confirm a viable fetus, although there is no evidence of other clinical or predictive value | ||
| Fundal height measurement1,8 | Recommended at each prenatal visit beginning at 20 weeks; should be plotted for monitoring purposes | ||
| Prenatal ultrasonography | |||
| Fetal anatomy screening9 | Should be evaluated with ultrasonography between 18 and 22 weeks | ||
| Dating9,10 | Ultrasonography dating is considered accurate to within: 5 days if less than 8 6/7 weeks 7 days between 9 0/7 and 15 6/7 weeks 10 days between 16 0/7 and 21 6/7 weeks 14 days between 22 0/7 and 27 6/7 weeks 21 days if more than 28 0/7 weeks | ||
| Screening for psychosocial factors | |||
| Depression and anxiety-related disorders11 | Screening is recommended in first and third trimesters using validated tools Anxiety: Generalized Anxiety Scale-7 (sensitivity 73%, specificity 67%) or State-Trait Anxiety Inventory (sensitivity 81%, specificity 78%) Bipolar disorder: screening should occur before initiating treatment for anxiety or depression; Composite International Diagnostic Interview (sensitivity 69% to 100%, specificity 98% to 99%) or Mood Disorder Questionnaire (sensitivity 44% to 90%, specificity 61% to 92%) Depression: Edinburgh Postnatal Depression Scale (sensitivity 81%, specificity 88%) or Patient Health Questionnaire-9 (sensitivity and specificity 88%), which contains questions about anxiety | ||
| Food insecurity12 | Patients should be screened at least once during pregnancy and in the postpartum period; two-item validated Hunger Vital Sign screening tool (sensitivity 97%) | ||
| Intimate partner violence13 | Patients who may become pregnant should be screened and provided with intervention services for positive results | ||
| Substance use14–19 | Pregnant patients should be asked about alcohol consumption, tobacco use, and illicit drug use during the first prenatal visit Use of validated tools to screen for opioid use is encouraged (e.g., 4Ps [parents, partners, past, and pregnancy], NIDA Quick Screen, CRAFFT [car, relax, alone, forget, friends, trouble]) Counseling is effective in decreasing substance use in pregnancy and associated infant morbidity (e.g., intrauterine growth restriction); therefore, individualized, pregnancy-tailored counseling and treatment should be offered | ||
| Antenatal fetal surveillance and delivery timing | |||
| Antenatal fetal surveillance (e.g., non-stress testing, biophysical profile)20 | Recommended in pregnancies complicated by conditions that increase the risk of stillbirth, including: intrauterine growth restriction, hypertension, diabetes mellitus, prepregnancy body mass index greater than 35 kg per m2, five or more alcoholic drinks per week, substance use, gestational age 41 0/7 weeks and greater Timing and frequency of testing should be determined in consultation with perinatology | ||
| Delivery timing21,22 | Can offer elective induction of labor at 39 weeks for low-risk, singleton pregnancies Determination of optimal timing for delivery of pregnancies complicated by high-risk fetal, placental, and maternal conditions should be done in consultation with perinatology | ||
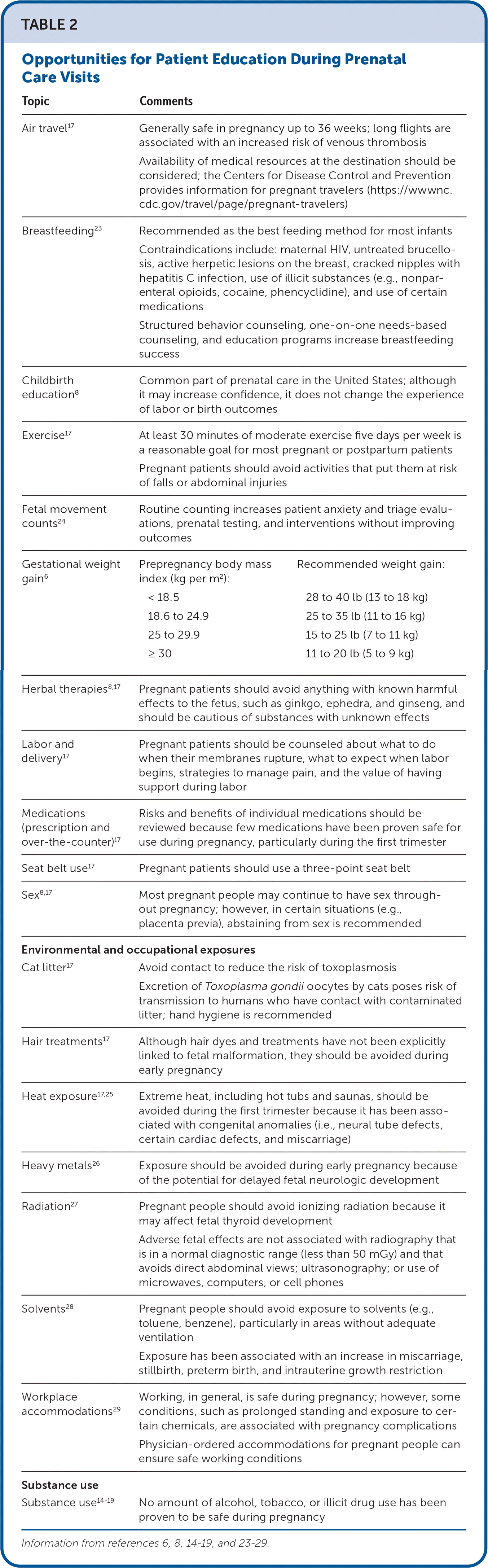
TABLE 2. Opportunities for Patient Education During Prenatal Care Visits
| Topic | Comments | |
|---|---|---|
| Air travel17 | Generally safe in pregnancy up to 36 weeks; long flights are associated with an increased risk of venous thrombosis Availability of medical resources at the destination should be considered; the Centers for Disease Control and Prevention provides information for pregnant travelers (https://wwwnc.cdc.gov/travel/page/pregnant-travelers) | |
| Breastfeeding23 | Recommended as the best feeding method for most infants Contraindications include: maternal HIV, untreated brucellosis, active herpetic lesions on the breast, cracked nipples with hepatitis C infection, use of illicit substances (e.g., nonparenteral opioids, cocaine, phencyclidine), and use of certain medications Structured behavior counseling, one-on-one needs-based counseling, and education programs increase breastfeeding success | |
| Childbirth education8 | Common part of prenatal care in the United States; although it may increase confidence, it does not change the experience of labor or birth outcomes | |
| Exercise17 | At least 30 minutes of moderate exercise five days per week is a reasonable goal for most pregnant or postpartum patients Pregnant patients should avoid activities that put them at risk of falls or abdominal injuries | |
| Fetal movement counts24 | Routine counting increases patient anxiety and triage evaluations, prenatal testing, and interventions without improving outcomes | |
| Gestational weight gain6 | Prepregnancy body mass index (kg per m2): < 18.5 18.6 to 24.9 25 to 29.9 ≥ 30 | Recommended weight gain: 28 to 40 lb (13 to 18 kg) 25 to 35 lb (11 to 16 kg) 15 to 25 lb (7 to 11 kg) 11 to 20 lb (5 to 9 kg) |
| Herbal therapies8,17 | Pregnant patients should avoid anything with known harmful effects to the fetus, such as ginkgo, ephedra, and ginseng, and should be cautious of substances with unknown effects | |
| Labor and delivery17 | Pregnant patients should be counseled about what to do when their membranes rupture, what to expect when labor begins, strategies to manage pain, and the value of having support during labor | |
| Medications (prescription and over-the-counter)17 | Risks and benefits of individual medications should be reviewed because few medications have been proven safe for use during pregnancy, particularly during the first trimester | |
| Seat belt use17 | Pregnant patients should use a three-point seat belt | |
| Sex8,17 | Most pregnant people may continue to have sex throughout pregnancy; however, in certain situations (e.g., placenta previa), abstaining from sex is recommended | |
| Environmental and occupational exposures | ||
| Cat litter17 | Avoid contact to reduce the risk of toxoplasmosis Excretion of Toxoplasma gondii oocytes by cats poses risk of transmission to humans who have contact with contaminated litter; hand hygiene is recommended | |
| Hair treatments17 | Although hair dyes and treatments have not been explicitly linked to fetal malformation, they should be avoided during early pregnancy | |
| Heat exposure17,25 | Extreme heat, including hot tubs and saunas, should be avoided during the first trimester because it has been associated with congenital anomalies (i.e., neural tube defects, certain cardiac defects, and miscarriage) | |
| Heavy metals26 | Exposure should be avoided during early pregnancy because of the potential for delayed fetal neurologic development | |
| Radiation27 | Pregnant people should avoid ionizing radiation because it may affect fetal thyroid development Adverse fetal effects are not associated with radiography that is in a normal diagnostic range (less than 50 mGy) and that avoids direct abdominal views; ultrasonography; or use of microwaves, computers, or cell phones | |
| Solvents28 | Pregnant people should avoid exposure to solvents (e.g., toluene, benzene), particularly in areas without adequate ventilation Exposure has been associated with an increase in miscarriage, stillbirth, preterm birth, and intrauterine growth restriction | |
| Workplace accommodations29 | Working, in general, is safe during pregnancy; however, some conditions, such as prolonged standing and exposure to certain chemicals, are associated with pregnancy complications Physician-ordered accommodations for pregnant people can ensure safe working conditions | |
| Substance use | ||
| Substance use14–19 | No amount of alcohol, tobacco, or illicit drug use has been proven to be safe during pregnancy | |
PHYSICAL EXAMINATION
Weight, height, and blood pressure should be measured at the first prenatal visit. Early identification of periodontal disease and treatment decreases adverse pregnancy outcomes.7 Treatment may be performed in the second trimester, and emergent treatment may be completed at any time during pregnancy.7 A bimanual pelvic examination has poor predictive value for clinical pelvimetry and screening for disease (i.e., sexually transmitted infections and cancer) but may be used as a diagnostic aid in patients with a discrepancy between uterine size and gestational age, which warrants ultrasonography assessment.30 A pelvic examination is also useful in a symptomatic patient for evaluating spontaneous labor (e.g., cervical dilation, rupture of amniotic membranes). The clinical breast examination is a diagnostic aid in the symptomatic patient and addresses breastfeeding concerns or barriers but does not demonstrate benefit in patients already receiving screening mammograms and does not decrease mortality.31–33
MATERNAL WEIGHT GAIN AND NUTRITION
A prepregnancy body mass index (BMI) greater than 25 kg per m2 is associated with preterm delivery, gestational diabetes, gestational hypertension, and preeclampsia. A BMI greater than 30 kg per m2 is also associated with an increased risk of miscarriage, stillbirth, and obstructive sleep apnea.6 Prepregnancy BMI informs the timing of fetal surveillance, nutritional counseling, and goals for gestational weight gain. Table 3 lists general dietary guidelines for pregnant people.8,17,34,35 For Black and Hispanic people, a prepregnancy BMI greater than 25 kg per m2 and the associated poor outcomes are worse compared with non-Hispanic White people.36
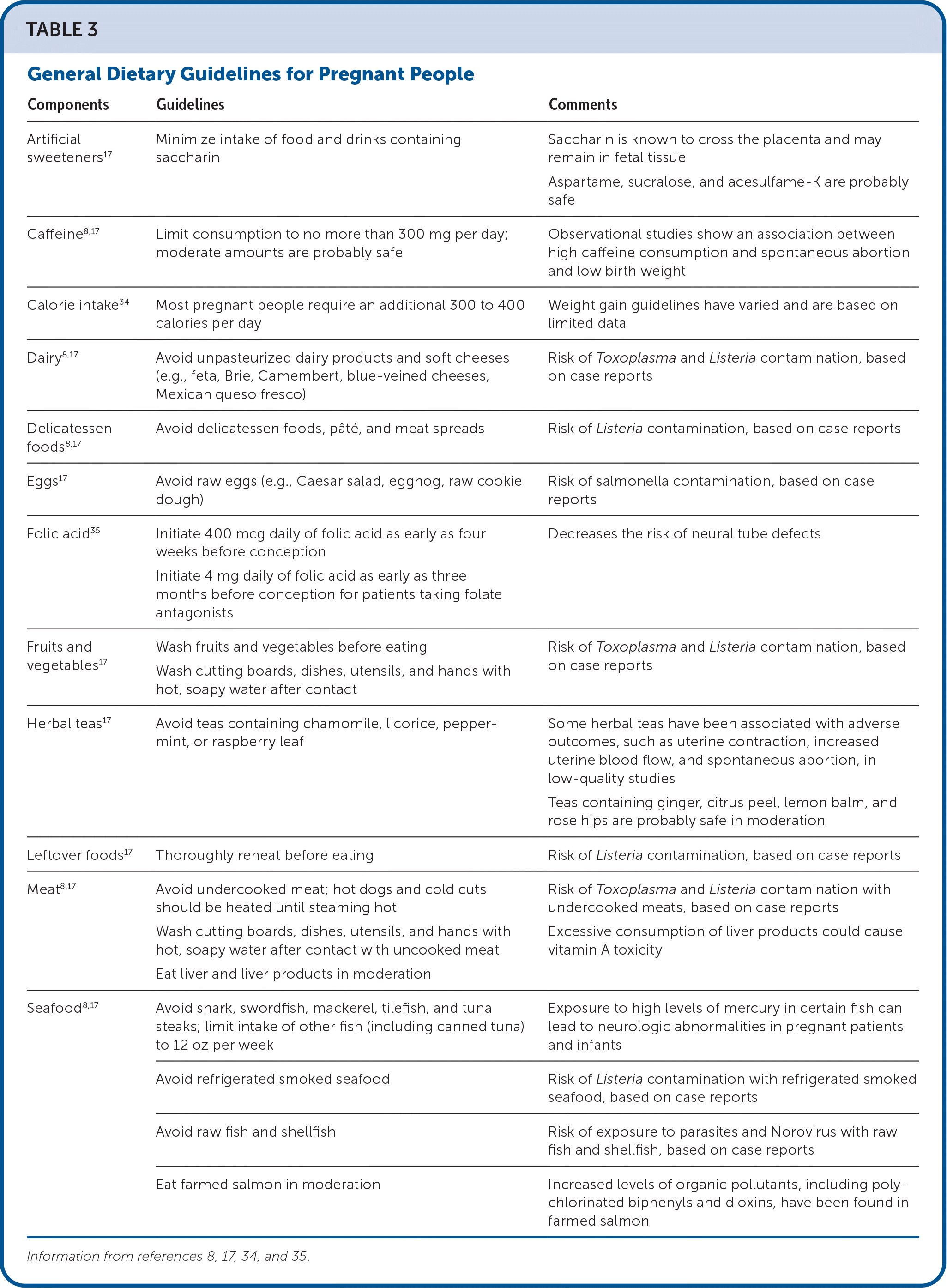
TABLE 3. General Dietary Guidelines for Pregnant People
| Components | Guidelines | Comments |
|---|---|---|
| Artificial sweeteners17 | Minimize intake of food and drinks containing saccharin | Saccharin is known to cross the placenta and may remain in fetal tissue Aspartame, sucralose, and acesulfame-K are probably safe |
| Caffeine8,17 | Limit consumption to no more than 300 mg per day; moderate amounts are probably safe | Observational studies show an association between high caffeine consumption and spontaneous abortion and low birth weight |
| Calorie intake34 | Most pregnant people require an additional 300 to 400 calories per day | Weight gain guidelines have varied and are based on limited data |
| Dairy8,17 | Avoid unpasteurized dairy products and soft cheeses (e.g., feta, Brie, Camembert, blue-veined cheeses, Mexican queso fresco) | Risk of Toxoplasma and Listeria contamination, based on case reports |
| Delicatessen foods8,17 | Avoid delicatessen foods, pâté, and meat spreads | Risk of Listeria contamination, based on case reports |
| Eggs17 | Avoid raw eggs (e.g., Caesar salad, eggnog, raw cookie dough) | Risk of salmonella contamination, based on case reports |
| Folic acid35 | Initiate 400 mcg daily of folic acid as early as four weeks before conception Initiate 4 mg daily of folic acid as early as three months before conception for patients taking folate antagonists | Decreases the risk of neural tube defects |
| Fruits and vegetables17 | Wash fruits and vegetables before eating Wash cutting boards, dishes, utensils, and hands with hot, soapy water after contact | Risk of Toxoplasma and Listeria contamination, based on case reports |
| Herbal teas17 | Avoid teas containing chamomile, licorice, peppermint, or raspberry leaf | Some herbal teas have been associated with adverse outcomes, such as uterine contraction, increased uterine blood flow, and spontaneous abortion, in low-quality studies Teas containing ginger, citrus peel, lemon balm, and rose hips are probably safe in moderation |
| Leftover foods17 | Thoroughly reheat before eating | Risk of Listeria contamination, based on case reports |
| Meat8,17 | Avoid undercooked meat; hot dogs and cold cuts should be heated until steaming hot Wash cutting boards, dishes, utensils, and hands with hot, soapy water after contact with uncooked meat Eat liver and liver products in moderation | Risk of Toxoplasma and Listeria contamination with undercooked meats, based on case reports Excessive consumption of liver products could cause vitamin A toxicity |
| Seafood8,17 | Avoid shark, swordfish, mackerel, tilefish, and tuna steaks; limit intake of other fish (including canned tuna) to 12 oz per week | Exposure to high levels of mercury in certain fish can lead to neurologic abnormalities in pregnant patients and infants |
| Avoid refrigerated smoked seafood | Risk of Listeria contamination with refrigerated smoked seafood, based on case reports | |
| Avoid raw fish and shellfish | Risk of exposure to parasites and Norovirus with raw fish and shellfish, based on case reports | |
| Eat farmed salmon in moderation | Increased levels of organic pollutants, including polychlorinated biphenyls and dioxins, have been found in farmed salmon |
PARENTAL AGE AT CONCEPTION
Advanced maternal and paternal age (35 years and older) is associated with poor outcomes (i.e., aneuploidy, birth defects, gestational diabetes, hypertension, intrauterine growth restriction [IUGR], miscarriage, and stillbirth). Activities focused on improving perinatal outcomes for this group, such as a detailed fetal anatomic screening on ultrasonography, may decrease morbidity and mortality.37
PREGNANCY DATING AND ULTRASONOGRAPHY
Accurate gestational age estimation is critical to quality care because it enables more precise timing of interventions (e.g., aspirin for preeclampsia prevention, steroids for fetal lung maturity), screening tests, and delivery. Up to 40% of people estimate their last menstrual period incorrectly; therefore, ultrasonography is recommended if uncertainty exists and for patients with irregular menstrual cycles, irregular bleeding, and discrepancy between uterine size and gestational age.1,38 Ultrasonography before 24 weeks decreases missed multiple gestations and post-term inductions.39 Although routine third-trimester ultrasonography may increase detection of IUGR, it does not improve outcomes.40 If malpresentation is suspected on physical examination, confirmation with ultrasonography is recommended.4
Screening
ALLOIMMUNIZATION
For patients who are RhD-negative and carrying a fetus who is RhD-positive, the alloimmunization risk is 1.5% to 2% in the setting of spontaneous abortion and 4% to 5% with dilation and curettage. The risk is decreased by 80% to 90% with anti-D immune globulin.41 Testing for the ABO blood group and RhD antibodies should be performed early in pregnancy. A 300-mcg dose of anti-D immune globulin is recommended for RhD-negative pregnant patients at 28 weeks and again within 72 hours of delivery if the infant is RhD-positive.41
ANEMIA
Iron deficiency anemia increases the risk of preterm delivery, IUGR, and perinatal depression. The U.S. Preventive Services Task Force found insufficient evidence to assess the benefits and harms of screening for anemia in pregnancy.42 Screening is recommended by the American College of Obstetricians and Gynecologists early in pregnancy, with iron treatment if deficient.43 Intravenous iron should be considered for patients who cannot tolerate oral iron or in whom oral iron has been ineffective at correcting the deficiency.43 Patients with non–iron deficiency anemia, or if iron repletion is ineffective within six weeks, should be referred to a hematologist for further evaluation. Iron supplementation in the first trimester decreases the prevalence of iron deficiency.43
INHERITED CONDITIONS
Pregnant patients should be counseled and offered aneuploidy (extra or missing chromosomes) screening in early pregnancy, regardless of age.44 In the United States, 1 in 150 infants has a chromosomal condition, the most common being trisomy 21 (Down syndrome).44 Table 4 compares screening tests for Down syndrome.1,45,46 If a screening test is positive, amniocentesis at 15 weeks or more or chorionic villous sampling between 11 and 13 weeks is recommended. Both procedures have similar rates of fetal loss.47 At 35 years of age, the risk of Down syndrome (1 in 294 births) is similar to that of fetal loss from amniocentesis.47 Serum and nuchal translucency testing can screen for other trisomies, including 13 and 18, the protocols for which have lower sensitivities and higher specificities compared with screening protocols for trisomy 21 because they are rarer.47
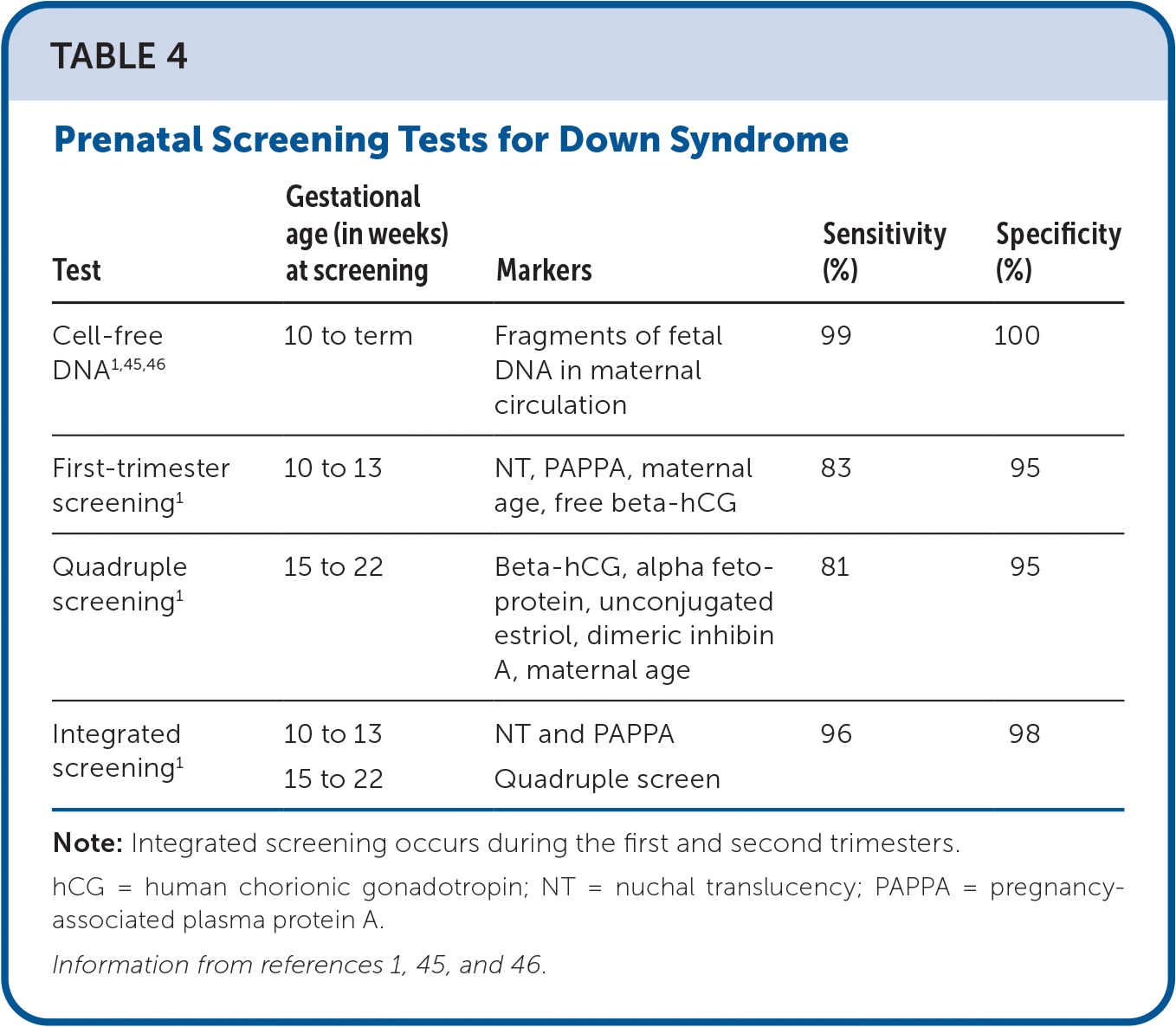
TABLE 4. Prenatal Screening Tests for Down Syndrome
| Test | Gestational age (in weeks) at screening | Markers | Sensitivity (%) | Specificity (%) |
|---|---|---|---|---|
| Cell-free DNA1,45,46 | 10 to term | Fragments of fetal DNA in maternal circulation | 99 | 100 |
| First-trimester screening1 | 10 to 13 | NT, PAPPA, maternal age, free beta-hCG | 83 | 95 |
| Quadruple screening1 | 15 to 22 | Beta-hCG, alpha fetoprotein, unconjugated estriol, dimeric inhibin A, maternal age | 81 | 95 |
| Integrated screening1 | 10 to 13 15 to 22 | NT and PAPPA Quadruple screen | 96 | 98 |
Note: Integrated screening occurs during the first and second trimesters. hCG = human chorionic gonadotropin; NT = nuchal translucency; PAPPA = pregnancy-associated plasma protein A.
Additional genetic screening should be based on maternal and paternal personal and family histories. Race is a social construct, necessitating a shift in genetic risk stratification from race-based to ancestry-based. Sickle cell disease affects up to 100,000 people in the United States, but its inheritance pattern (1:10) is based on people with African ancestry, which includes much of the world.48 Cystic fibrosis is inherited mainly by people of European ancestry (1:25), but ignoring the possibility of European ancestry in certain racial and ethnic groups results in an underestimation of its prevalence: African (1:61), Hispanic (1:40), and Mediterranean (1:29).49
NEURAL TUBE DEFECTS
In the United States, neural tube defects affect approximately 2,600 infants per year, with the highest prevalence in Hispanic populations.35,50 All pregnant patients should be counseled and offered screening with maternal serum alpha fetoprotein.35 Folic acid, 400 to 800 mcg daily, started at least one month before conception and continued until the end of the first trimester, decreases the incidence of neural tube defects by nearly 78%.35 Patients taking folic acid antagonists (e.g., carbamazepine, methotrexate, trimethoprim) or who have a history of carrying a fetus with a neural tube defect should take 4 mg of folic acid daily, starting at least three months before conception.35
THYROID DISORDERS
There is no evidence that screening for thyroid disorders improves pregnancy outcomes. Thyroid-stimulating hormone levels should be measured if there is a history of thyroid disease or symptoms of disease. If the level is abnormal, a free thyroxine test helps determine the etiology.51 Hypothyroidism complicates 1 to 3 per 1,000 pregnancies and increases the risk of fetal loss, preeclampsia, IUGR, and stillbirth. Hyperthyroidism occurs in 2 per 1,000 pregnancies and is associated with miscarriage, preeclampsia, IUGR, preterm delivery, thyroid storm, and congestive heart failure.51 The effect of subclinical hypothyroidism on a child's neurocognitive development is not well understood, and the effectiveness of treatment with levothyroxine is unproven.51
CERVICAL CANCER
Intervals for cervical cancer screening are based on patient age, cytology history, and history of the presence of high-risk human papillomavirus (HPV). Routine screening for people at average risk of cervical cancer should begin at 21 years of age. Screening can be performed with either cytology alone every three years, HPV screening alone every five years, or cytology plus HPV screening every five years starting at 25 years of age. Screening is not indicated for people 65 years and older with negative screening in the previous 10 years, and no history of cervical intraepithelial neoplasia grade 2 or higher in the past 25 years.52 Colposcopy is indicated when the risk of cervical intraepithelial neoplasia grade 3 is greater than 4%. Surveillance of high-grade lesions should be performed every 12 to 24 weeks.52,53 Although colposcopy and cervical biopsy can be safely performed during pregnancy, endocervical sampling should be deferred until postpartum.53
Infectious Disease
BACTERIURIA
Asymptomatic bacteriuria complicates up to 15% of pregnancies in the United States, 30% of which progress to pyelonephritis if untreated.54 All pregnant patients should be screened for bacteriuria at the first prenatal visit.54 A culture from a midstream or clean-catch sample with greater than 100,000 colony-forming units per mL of a single pathogen is considered positive and treated to decrease the risk of pyelonephritis and subsequent preterm delivery.54
SEXUALLY TRANSMITTED INFECTIONS
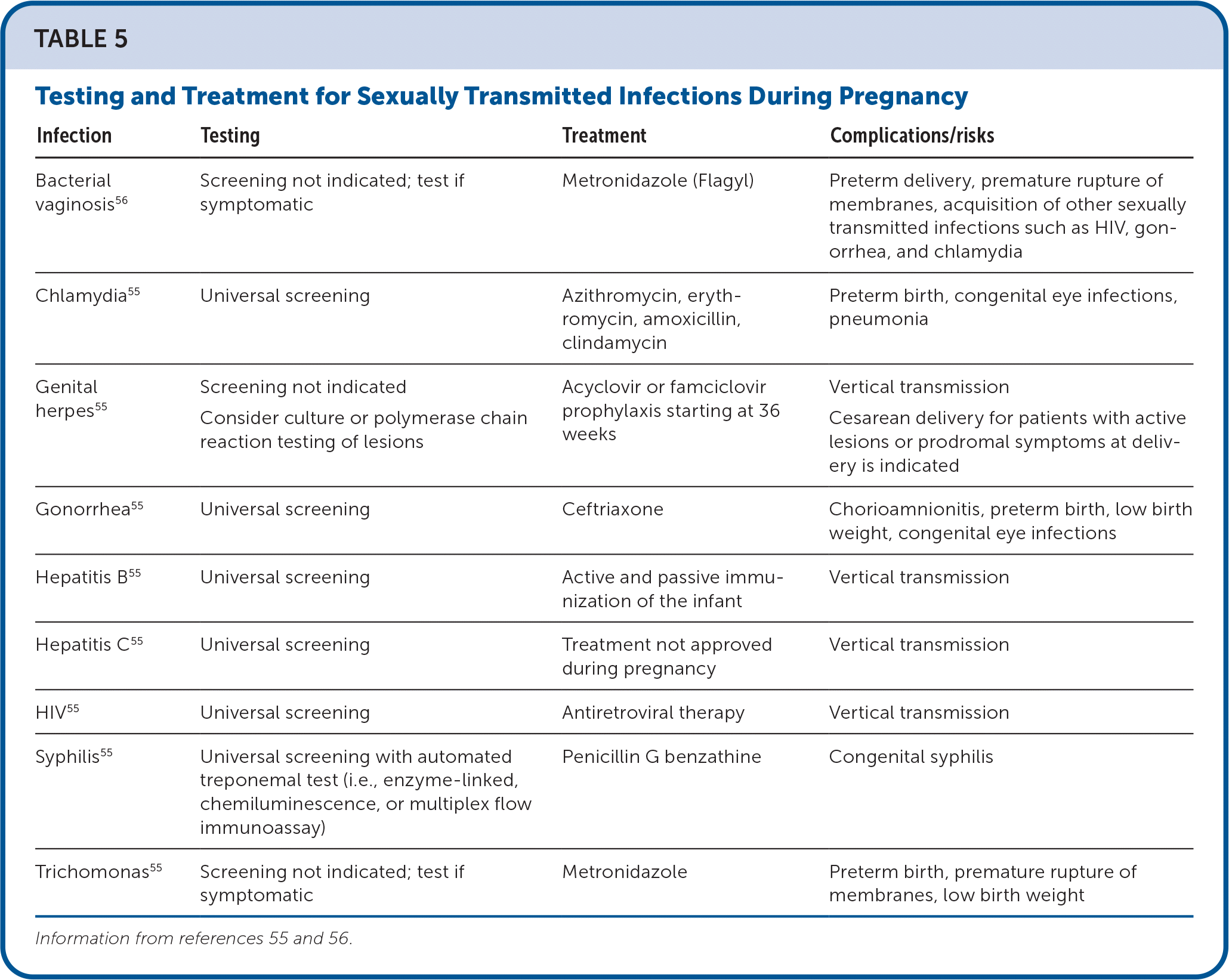
Sexually transmitted infections can affect prenatal outcomes.55–57 Table 5 lists routine screening and treatment for sexually transmitted infections in pregnancy.55,56
TABLE 5. Testing and Treatment for Sexually Transmitted Infections During Pregnancy
| Infection | Testing | Treatment | Complications/risks |
|---|---|---|---|
| Bacterial vaginosis56 | Screening not indicated; test if symptomatic | Metronidazole (Flagyl) | Preterm delivery, premature rupture of membranes, acquisition of other sexually transmitted infections such as HIV, gonorrhea, and chlamydia |
| Chlamydia55 | Universal screening | Azithromycin, erythromycin, amoxicillin, clindamycin | Preterm birth, congenital eye infections, pneumonia |
| Genital herpes55 | Screening not indicated Consider culture or polymerase chain reaction testing of lesions | Acyclovir or famciclovir prophylaxis starting at 36 weeks | Vertical transmission Cesarean delivery for patients with active lesions or prodromal symptoms at delivery is indicated |
| Gonorrhea55 | Universal screening | Ceftriaxone | Chorioamnionitis, preterm birth, low birth weight, congenital eye infections |
| Hepatitis B55 | Universal screening | Active and passive immunization of the infant | Vertical transmission |
| Hepatitis C55 | Universal screening | Treatment not approved during pregnancy | Vertical transmission |
| HIV55 | Universal screening | Antiretroviral therapy | Vertical transmission |
| Syphilis55 | Universal screening with automated treponemal test (i.e., enzyme-linked, chemiluminescence, or multiplex flow immunoassay) | Penicillin G benzathine | Congenital syphilis |
| Trichomonas55 | Screening not indicated; test if symptomatic | Metronidazole | Preterm birth, premature rupture of membranes, low birth weight |
RUBELLA
Rubella immunity screening during the first prenatal visit is recommended. Postpartum vaccination should also be offered if the patient is not immune to prevent congenital rubella syndrome in subsequent pregnancies.1,58 The presence of rubella immunoglobulin G should be interpreted with caution in patients recently migrating from areas where rubella is endemic because this may indicate a recent infection.58 Rubella is a live vaccine and should not be administered during pregnancy but is safe during lactation after delivery.59,60
VARICELLA
Maternal varicella can result in congenital varicella syndrome (i.e., IUGR and limb, ophthalmologic, and neurologic abnormalities) and neonatal varicella; infection can occur from approximately five days before to two days after birth. A negative history of varicella infection or vaccination warrants serologic testing, and if immunoglobulin G is negative, varicella exposure should be avoided. Postpartum vaccination should be offered.61
TDAP
Although tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) vaccination is recommended for anyone in close contact with the infant, only antenatal maternal vaccination ensures increased protection against neonatal pertussis.62 Pregnant patients should receive a Tdap vaccine beginning at 27 weeks to maximize time for passive immunity to the fetus through the placental transfer of maternal antibodies; vaccination is recommended in each subsequent pregnancy.62
INFLUENZA AND COVID-19
Influenza and COVID-19 infection in pregnancy increase the risk of intensive care unit admission, preterm delivery, stillbirth, and maternal death.63,64 COVID-19 infection almost doubles the risk of developing preeclampsia64; therefore, initiating low-dose aspirin (81 mg daily) starting at 12 weeks should be considered.5 Pregnant patients and their household contacts should be vaccinated for influenza and COVID-19.63,64
GROUP B STREPTOCOCCUS
In the United States, group B Streptococcus (GBS) is the leading cause of infection in the first three months of life; 25% of all pregnant patients are GBS carriers.65,66 Screening with a vaginal-rectal swab for culture between 36 and 37 weeks is recommended.67 Intrapartum antibiotic prophylaxis decreases neonatal mortality. Antibiotics are recommended when there is GBS bacteriuria with the current pregnancy, a history of a previous infant affected by GBS (e.g., septicemia, meningitis, pneumonia, death), or unknown GBS status and risk factors (e.g., preterm labor, rupture of membranes more than 18 hours before delivery, GBS in previous pregnancy).67 Patients with GBS bacteriuria in the current pregnancy are assumed to be colonized and do not need subsequent screening.67
Social determinants of health represent up to 80% of the factors that directly affect a person's health.68 Physicians who provide prenatal care play a critical role in mitigating the burden that social determinants of health play on maternal-child health without compromising the quality of care delivered.69 An increased burden from social determinants of health increases the risk of depression, anxiety, intimate partner violence, substance use, and food insecurity70,71; therefore, universal screening is recommended early in pregnancy.
DEPRESSION AND ANXIETY-RELATED DISORDERS
After the COVID-19 pandemic, rates of perinatal depression and anxiety have increased. People who are non-White, 24 years or younger, or who have 12 years or less of education, lower socioeconomic status, or a history of intimate partner violence or sexual trauma are at higher risk.11,72,73 If untreated, depression and anxiety-related disorders increase the risk of preeclampsia, preterm delivery, IUGR, substance use, maternal suicide, infanticide, psychosis, and homicide.11
INTIMATE PARTNER VIOLENCE
Intimate partner–related homicide is the leading cause of death in the United States in pregnancy. Screening is recommended at the first prenatal visit and once per trimester.13 Intimate partner violence increases the risk of miscarriage, placental abruption, premature rupture of membranes, IUGR, and preterm delivery.13 Family physicians should be aware of the signs of intimate partner violence (e.g., frequent sexually transmitted infections, repeated requests for pregnancy tests when pregnancy is not desired, fear of asking a partner to use a condom), the effect of violence on health, and the increased risk of child abuse after delivery.13
SUBSTANCE USE
Substance use during pregnancy increases the risk of IUGR, preterm delivery, stillbirth, fetal malformations, and maternal death.74 The use of prescription opioids complicates 7% of pregnancies in the United States; of these, 20% of patients report misuse.75 Opioid use in pregnancy increased by 131% from 2010 to 2017 in the United States, and the incidence of babies born with withdrawal symptoms in that time increased by 82%.76 Fetal alcohol exposure is the leading cause of preventable neurodevelopmental disorders in the United States.14 However, 14% of pregnant patients report current drinking, and 5% report binge drinking in the past 30 days.77 Exposure to cigarette smoking in utero increases the risk of sudden intrauterine and infant death.15
FOOD INSECURITY
Maternal food insecurity increases the risk of poor outcomes (e.g., IUGR, preterm delivery, gestational diabetes, hypertension, depression, anxiety). However, few patients disclose this due to concerns about social stigma; therefore, a universal approach to screening is encouraged. The Hunger Vital Sign tool may be used.12
Complications of Pregnancy
GESTATIONAL DIABETES
Gestational diabetes complicates up to 14% of U.S. pregnancies, with up to 67% of patients developing type 2 diabetes later in life.78 Racial and ethnic minorities are at the highest risk.79 Gestational diabetes is associated with hypertension, macrosomia, shoulder dystocia, and cesarean deliveries.80 Screening for undiagnosed type 2 diabetes at the initial prenatal visit is recommended for people at increased risk80 (Table 65,80 ). Universal screening for gestational diabetes should occur between 24 and 28 weeks with a one-hour (50-g) glucose tolerance test and, if results are abnormal, should be followed by a confirmatory, fasting, three-hour (100-g) test.80
TABLE 6. Risk Factors for Developing Gestational Diabetes Mellitus and Preeclampsia

| Gestational diabetes risk factors80 |
| Body mass index > 25 kg per m2 plus at least one of the following: First-degree relative with diabetes mellitus High-risk race/ethnicity (i.e., Black, Hispanic, Native American, Asian, or Pacific Islander) Hypertension Personal history of gestational diabetes |
| Preeclampsia risk factors5 |
| Assisted reproductive technology |
| Autoimmune disease (e.g., systemic lupus erythematosus, rheumatoid arthritis, antiphospholipid syndrome) |
| Diabetes (gestational and pregestational) |
| Either parents' birth was complicated by preeclampsia |
| Hypertension before 20 weeks (chronic hypertension) |
| Maternal age ≥ 35 years |
| Multifetal gestation |
| Obstructive sleep apnea |
| Polycystic ovary syndrome |
| Prepregnancy body mass index > 25 kg per m2 |
| Renal disease |
Note: Maternity care physicians should carefully review the medical, social, and family histories of pregnant people and their partners to determine appropriateness of daily low-dose aspirin (81 mg) for the prevention of preeclampsia.5
HYPERTENSION
Blood pressure should be monitored at each prenatal visit, and education should be provided on preeclampsia warning signs.5 Patients at increased risk of preeclampsia should be screened for thrombocytopenia, transaminitis, and renal insufficiency, including proteinuria, during the first or second trimester and started on prophylactic daily low-dose aspirin (81 mg) between 12 and 16 weeks5,85 (Table 65,80 ). [Updated] Screening for proteinuria in isolation has little predictive value for detecting preeclampsia.5 Chronic hypertension (hypertension before 20 weeks) is treated to less than 140/90 mm Hg.81
PRETERM DELIVERY
Preterm delivery (between 20 and 37 weeks) is a significant cause of neonatal morbidity and mortality, complicating 10.5% of U.S. pregnancies.2 Modifiable risk factors include prepregnancy BMI (less than 18.5 kg per m2 and greater than 25 kg per m2), substance use, and short interval between pregnancies (i.e., less than 18 months).82 Several options are available for the prevention of preterm labor in a singleton pregnancy.82 Patients with a previous preterm delivery before 34 weeks should have a cervical length assessment starting at 16 weeks through 24 weeks.82 These patients should be treated with progesterone supplementation (vaginal or intramuscular). In the asymptomatic patient with a short cervix and without a history of spontaneous birth before 34 weeks, vaginal progesterone (200 mg) started between 16 and 20 weeks and continued through 36 weeks is recommended.82
POST-TERM DELIVERY
Stillbirth complicates 3 per 1,000 post-term (42 weeks or greater) pregnancies.20 Antenatal testing should be initiated at 41 weeks; if the results are not reassuring, induction of labor is recommended.20,21
Cultural Considerations
Maternity care improves outcomes; however, vulnerable populations (i.e., racial, ethnic, and religious minorities) are less likely to engage in care if it is not culturally centered, which acknowledges the effect of culture on health conditions (e.g., depression) and enhances patient-physician trust.83 Addressing cultural needs (e.g., doula, community health workers, interpreters) throughout pregnancy helps mitigate barriers and improves outcomes.
This article updates previous articles on this topic by Zolotor and Carlough1; Kirkham, et al.17; and Kirkham, et al.84
Data Sources: A search was completed using the key terms prenatal care, COVID-19, oral health, pelvic examination, prepregnancy body mass index, pregnancy dating and ultrasound, maternal and paternal age and impact on pregnancy outcomes, aneuploidy screening, inheritance patterns of sickle cell disease and cystic fibrosis, anemia, cell-free DNA analysis, thyroid disease, cervical cancer screening, management of abnormal cervical cytology, screening guidelines for sexually transmitted infections in pregnancy, group B Streptococcus screening, social determinants of health and prenatal outcomes, intimate partner violence, polysubstance abuse, food insecurity, maternity care deserts, hypertension in pregnancy, progesterone for preterm birth prevention, post-term delivery, and preconception care. Also searched were PubMed, Essential Evidence Plus, the Cochrane database, U.S. Preventive Services Task Force, American College of Obstetricians and Gynecologists, American Cancer Society, American Family Physician, and reference lists of retrieved articles. Search dates: July 1, 2022; February 19, 2023; and June 16, 2023.


Social Determinants of Health