Key Points for Practice
• Although insulin has the best evidence for maintaining glycemic control in hospitalized patients, dipeptidyl-peptidase-4 inhibitors may be equivalent for patients with type 2 diabetes.
• Corrective insulin alone only slightly increases average blood glucose levels vs. basal-bolus insulin and may reduce the risk of hypoglycemia.
• Carbohydrate counting has minimal impact on glycemic control compared with fixed mealtime insulin dosing.
• Diabetes education during hospitalization can improve outpatient glycemic control and reduce readmissions.
From the AFP Editors
One-fourth of hospitalized patients have diabetes mellitus, and up to one-third of those without diabetes experience glucose levels greater than 140 mg per dL (7.77 mmol per L) during their hospital stay. Diabetes and hyperglycemia are associated with prolonged hospitalizations. The Endocrine Society released updated guidelines for glycemic management during hospitalization with noncritical illnesses.
Monitoring Hospitalized Patients
For patients without diabetes and those with diabetes controlled without insulin, point-of-care blood glucose testing is recommended.
Based on low- or very low-quality evidence, continuous glucose monitoring for patients with insulin-treated diabetes may be more effective than point-of-care blood glucose monitoring alone at preventing hyperglycemia. Based on four randomized trials, continuous glucose monitoring decreases mean daily glucose levels. Continuous glucose monitoring may increase the detection of hypoglycemic events and reduce the time spent in hypoglycemia.
Medications to Control Hyperglycemia
Insulin is recommended to maintain glycemic control during hospitalizations, although some oral medications may offer similar control for patients with type 2 diabetes. Three randomized controlled trials suggest that daily dipeptidylpeptidase-4 inhibitors can maintain glycemic control similar to that of insulin and may reduce hypoglycemic events. Although glucagon-like peptide-1 receptor agonists also slightly reduce hypoglycemia compared with insulin, they increase the risk of nausea and vomiting. Metformin, sulfonylureas, thiazolidinediones, and sodium-glucose cotransporter-2 inhibitors have not been studied during hospitalization.
When insulin is used during hospitalization, regimens containing neutral protamine Hagedorn and basal-bolus insulin appear equivalent in preventing hyperglycemia and hypoglycemia.
Glycemic Control Regimens
Based on very low-quality evidence of benefit, the guideline recommends that corrective insulin be used to lower blood glucose levels of 140 mg per dL or greater in patients with hyperglyce-mia but not diabetes. In patients with diabetes not treated with insulin, corrective insulin or basal-bolus insulin can be initiated. Basal-bolus insulin is defined as a basal rate of long-acting insulin with boluses for mealtime and correction, whereas corrective insulin is only provided in response to hyperglycemia. In these patients, corrective insulin alone only slightly increases the average blood glucose level vs. basal-bolus insulin and may reduce the risk of hypoglycemia. For patients already treated with insulin, basal-bolus regimens are recommended.
For patients using insulin pump therapy before admission, continuing that therapy reduces hyperglycemia and hypoglycemia compared with shifting to an insulin regimen. Insulin pump therapy requires that patients have a sufficient level of consciousness to maintain their insulin pump settings, and it is not appropriate for patients with diabetic ketoacidosis or hyperosmolar hyperglycemic states. Hospitals must have sufficient expertise in managing insulin pump therapy.
Carbohydrate counting during hospitalization has little impact on glycemic control compared with fixed mealtime insulin doses. The Endocrine Society recommends not using carbohydrate counseling in patients not already treated with insulin therapy and using it in insulin-treated patients only if it is beneficial to model an outpatient routine.
Perioperative Glycemic Control
In patients with diabetes who are scheduled for elective surgery, a preoperative A1C level of less than 7% reduces the risk of postoperative infections and neurologic complications. Because this control can be overly challenging, an A1C level of 8% and random glucose level of 100 to 180 mg per dL (5.55 to 9.99 mmol per L) is recommended from one to four hours before surgery.
Diabetes Education During Hospitalization
Providing diabetes education during hospitalization through diabetes educators reduces A1C levels at six months by 0.8% (95% CI, 0.5% to 1.1%) and reduces readmissions by a number needed to treat of 24 (95% CI, 17 to 56).
G-TRUST GUIDELINE SCORECARD
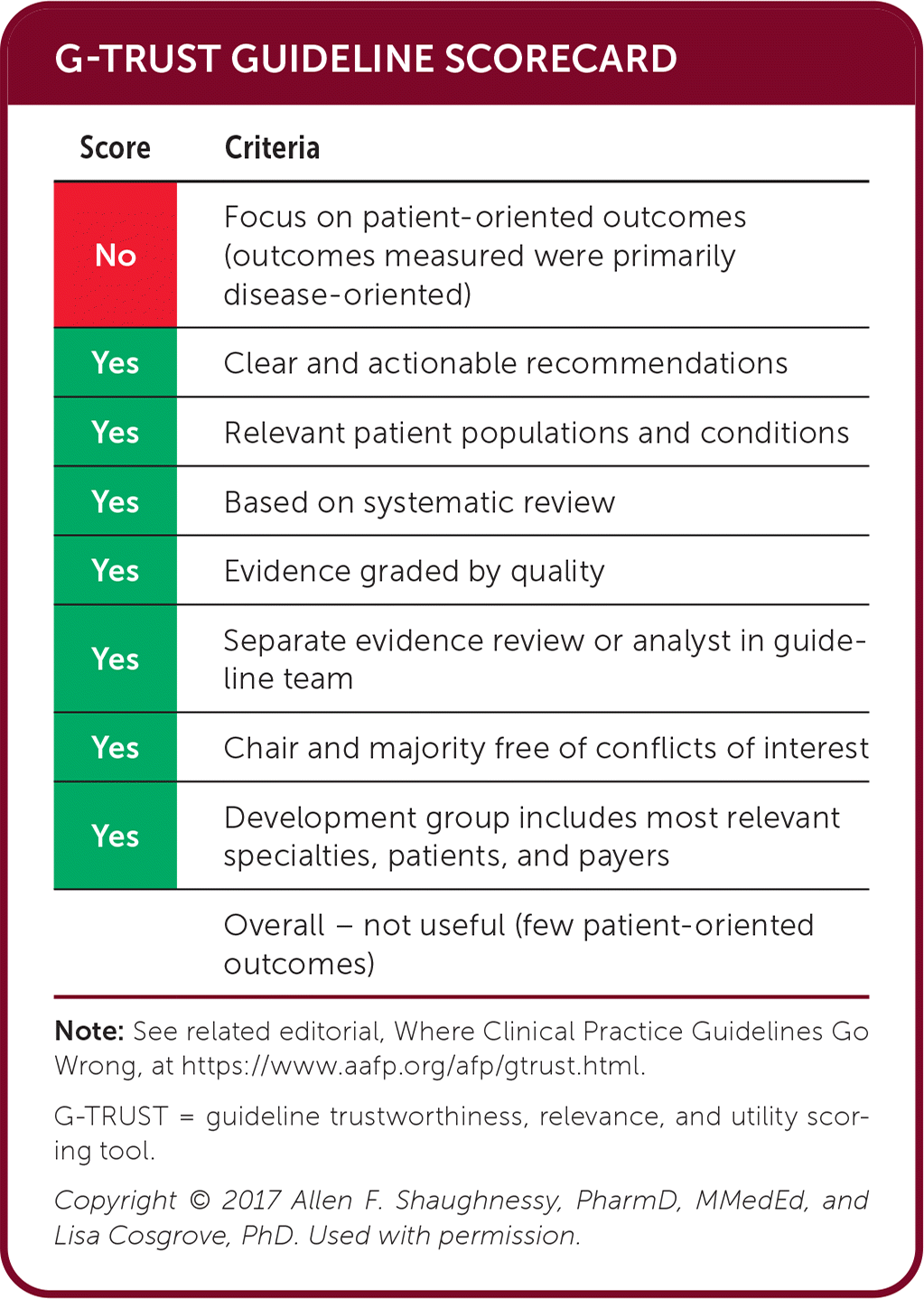
| Score | Criteria |
|---|---|
| No | Focus on patient-oriented outcomes (outcomes measured were primarily disease-oriented) |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analyst in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| Yes | Development group includes most relevant specialties, patients, and payers |
| Overall – not useful (few patient-oriented outcomes) |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
The views expressed are those of the author and do not necessarily reflect the official policy or position of the Uniformed Services University of the Health Sciences, U.S. Navy, U.S. Department of Defense, or U.S. government.
Editor's Note: Despite the limited and primarily disease-oriented evidence that leads to this guideline’s poor evaluation by G-TRUST, I find this guidance useful because it disproves some things I have been taught. For example, I fell into the guidance about a decade ago that corrective, or sliding scale insulin, was harmful for patients, and good physicians used only basal-bolus regimens. Yet, corrective insulin only increases average glucose levels slightly and appears to reduce hypoglycemia risk. Similarly, the limited benefit of carbohydrate counting can simplify orders and the nursing workload. —Michael J. Arnold, MD, Assistant Medical Editor
The number needed to treat and related CI reported in this Practice Guideline were calculated based on data from the Endocrine Society guideline.
Guideline source: Endocrine Society
Published source: Korytkowski MT, et al. Management of hyperglycemia in hospitalized adult patients in non-critical care settings. J Clin Endocrinol Metab. 2022;107(8):2101–2128

