Rashes in the newborn period are common and most are benign. Infections should be suspected in newborns with pustules or vesicles, especially in those who are not well-appearing or have risk factors for congenital infection. Congenital cytomegalovirus infection can cause sensorineural hearing loss and neurodevelopmental delay. Skin manifestations of cytomegalovirus may include petechiae due to thrombocytopenia. The most common skin manifestations of early congenital syphilis are small, copper-red, maculopapular lesions located primarily on the hands and feet that peel and crust over three weeks. Erythema toxicum neonatorum and neonatal pustular melanosis are transient pustular rashes with characteristic appearance and distribution. Neonatal acne is self-limited, whereas infantile acne may benefit from treatment. Milia can be differentiated from neonatal acne by their presence at birth. Cutis marmorata and harlequin color change are transient vascular phenomena resulting from inappropriate or exaggerated dilation of capillaries and venules in response to stimuli.
Skin findings in newborns can present a diagnostic challenge in distinguishing common, benign rashes from those associated with infection, malignancy, or systemic syndromes. When clinicians evaluate the newborn rash, the most important skill is to recognize when further evaluation is necessary because early diagnosis and treatment can have a significant impact on morbidity and mortality. Part I of this article reviews the presentation, prognosis, and treatment of the most common rashes and skin changes that present during the first four weeks of life. Part II of this article, which appears in this issue of American Family Physician, discusses the identification and management of birthmarks that appear in newborns.1
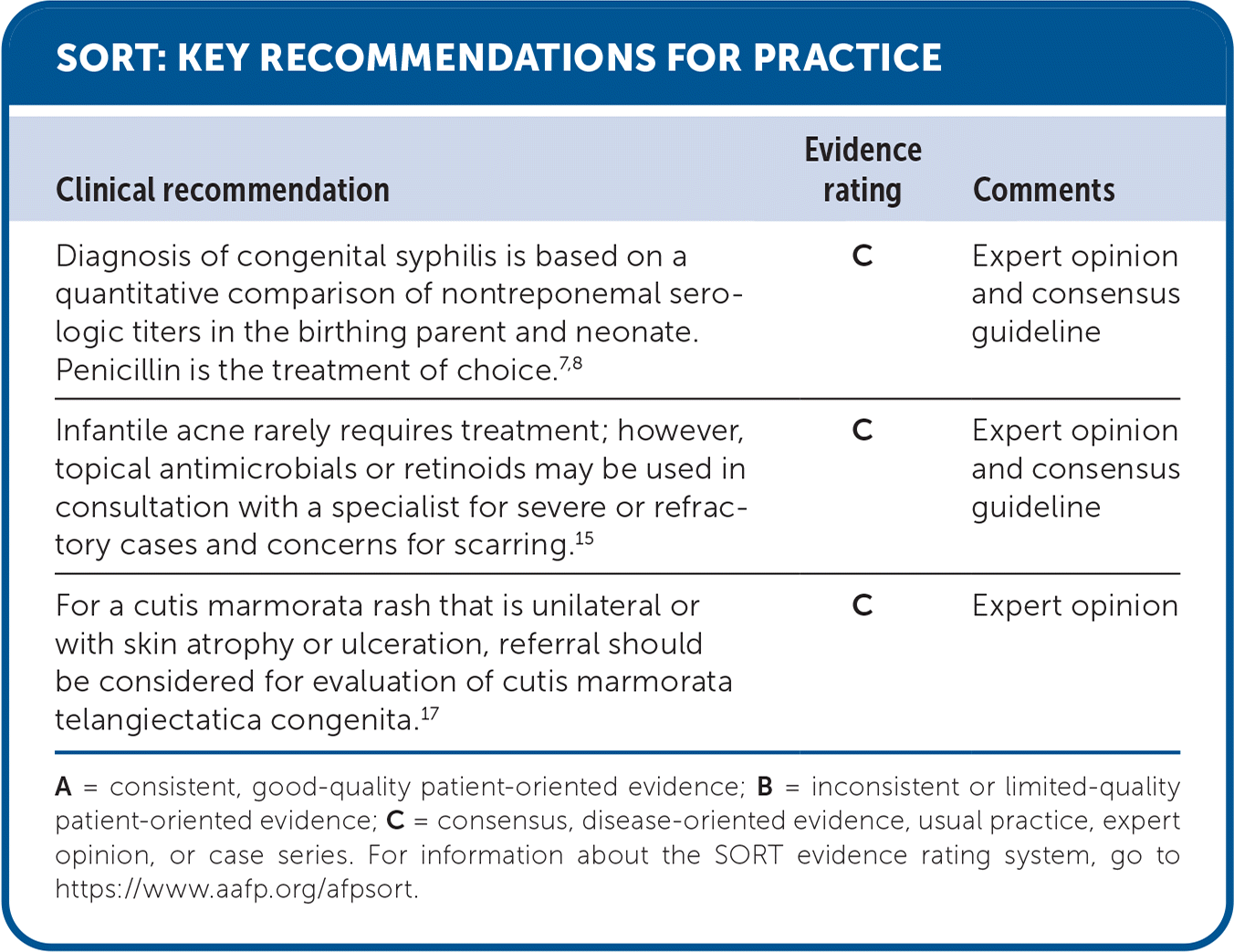
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| Diagnosis of congenital syphilis is based on a quantitative comparison of nontreponemal serologic titers in the birthing parent and neonate. Penicillin is the treatment of choice.7,8 | C | Expert opinion and consensus guideline |
| Infantile acne rarely requires treatment; however, topical antimicrobials or retinoids may be used in consultation with a specialist for severe or refractory cases and concerns for scarring.15 | C | Expert opinion and consensus guideline |
| For a cutis marmorata rash that is unilateral or with skin atrophy or ulceration, referral should be considered for evaluation of cutis marmorata telangiectatica congenita.17 | C | Expert opinion |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Transient Rashes
Infectious causes of transient rashes, such as Candida infections or congenital cytomegalovirus, should be a primary consideration. A rash consistent with one of the classic benign presentations in the well-appearing newborn can be monitored for resolution. Risk factors for congenital infections should be considered before the diagnosis of a benign rash.
INFECTIOUS CAUSES
Congenital infections may present with vesicles or pustules and can generally be distinguished based on presentation (Table 1).2–8 Diffuse papular or vesicular rashes due to bacterial infections will often be associated with clinical signs of sepsis.2
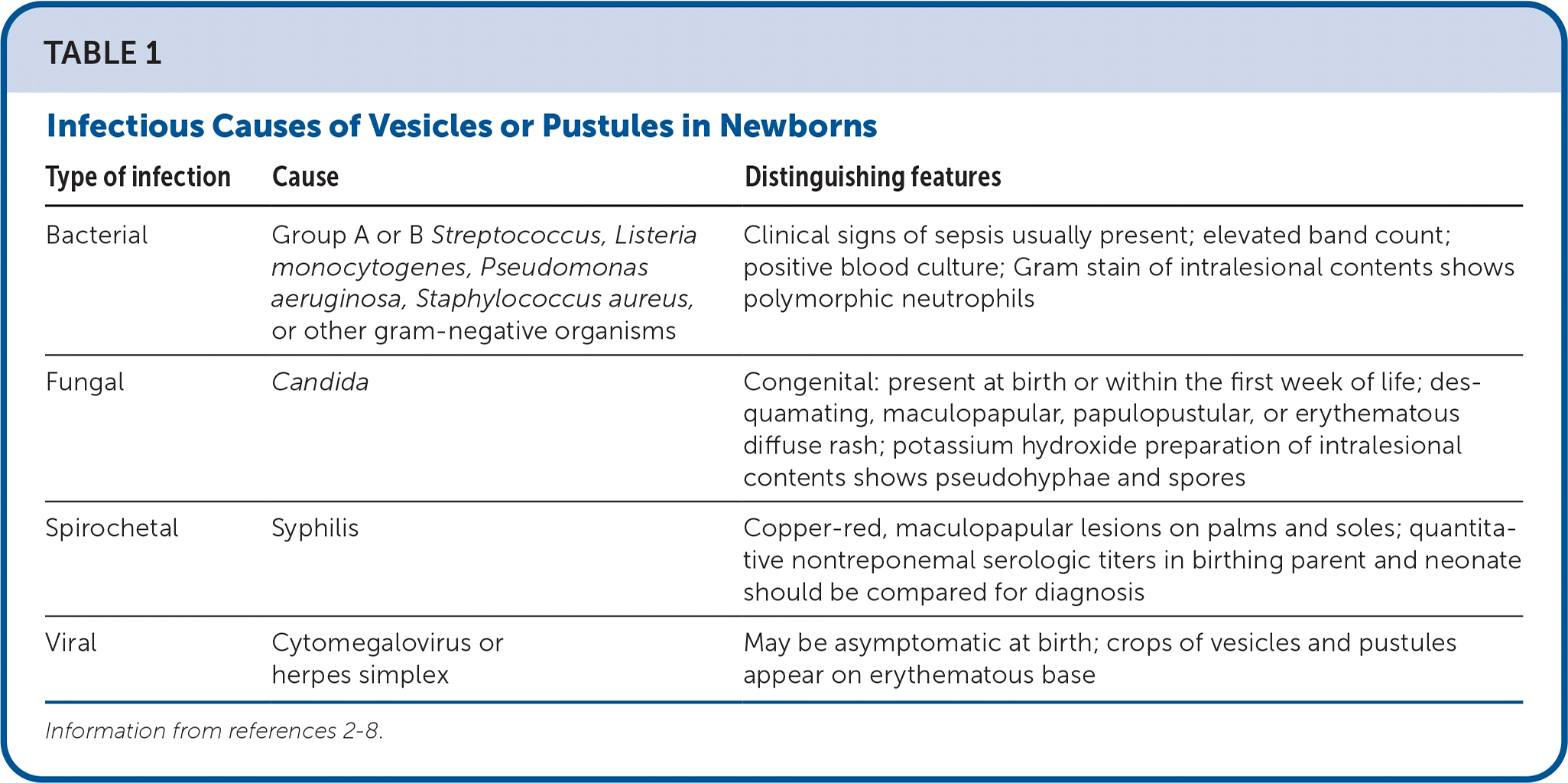
TABLE 1. Infectious Causes of Vesicles or Pustules in Newborns
| Type of infection | Cause | Distinguishing features |
|---|---|---|
| Bacterial | Group A or B Streptococcus, Listeria monocytogenes, Pseudomonas aeruginosa, Staphylococcus aureus, or other gram-negative organisms | Clinical signs of sepsis usually present; elevated band count; positive blood culture; Gram stain of intralesional contents shows polymorphic neutrophils |
| Fungal | Candida | Congenital: present at birth or within the first week of life; desquamating, maculopapular, papulopustular, or erythematous diffuse rash; potassium hydroxide preparation of intralesional contents shows pseudohyphae and spores |
| Spirochetal | Syphilis | Copper-red, maculopapular lesions on palms and soles; quantitative nontreponemal serologic titers in birthing parent and neonate should be compared for diagnosis |
| Viral | Cytomegalovirus or herpes simplex | May be asymptomatic at birth; crops of vesicles and pustules appear on erythematous base |
Congenital Candida infections are rare and cause a desquamating, maculopapular, papulopustular, or erythematous diffuse rash that presents at birth or in the first week of life. Prompt treatment with systemic antifungals can prevent disseminated candidemia.3
Herpes simplex virus (HSV) is a potentially devastating infection for the newborn and can be effectively treated with prompt recognition. Most newborns who are infected with HSV in the peripartum period have a birthing parent with no known history of HSV. Neonatal HSV can present with disseminated disease, central nervous system disease, or cutaneous infection of the skin, eyes, and mouth. HSV skin vesicles typically present at approximately 12 days of life and are associated with lethargy and fever in an ill-appearing child.4 An evaluation for HSV in these cases should not be delayed.
Congenital cytomegalovirus infections can cause sensorineural hearing loss and neurodevelopmental delay. Presentation is variable; 90% of newborns affected by cytomegalovirus are asymptomatic. Skin manifestations may include petechiae due to thrombocytopenia. Newborns with symptoms are more likely to suffer permanent sequelae.5 Diagnostic testing in newborns is performed with a saliva sample in the first two to three weeks of life.6
Previously considered a rare disease, congenital syphilis has steadily increased in incidence and geographic distribution since 2013.7 The most common skin manifestations of early congenital syphilis are small, copper-red, maculopapular lesions located primarily on the hands and feet that peel and crust over three weeks.7 Diagnosis is based on a quantitative comparison of nontreponemal serologic titers in the birthing parent and neonate.7 Penicillin is the treatment of choice.8
ERYTHEMA TOXICUM NEONATORUM
Erythema toxicum is a benign rash that may cause a caregiver to have concern that it is a more serious condition (Figure 1). It is the most common pustular newborn rash and affects approximately one-half of newborns; it is more common in those who are full-term.9,10 Lesions may be present at birth but more often appear in the first few days of life.11 Lesions may present as papules, followed by the development of small pustules with a large red base that are not in groups and are located on the face, trunk, and extremities. Lesions are not found on the palms or soles.2 Diagnosis is made clinically in well-appearing newborns, although a peripheral smear that contains eosinophils may help confirm the diagnosis.2 No treatment is required, and the rash should resolve with no scarring in one to two weeks.
FIGURE 1.
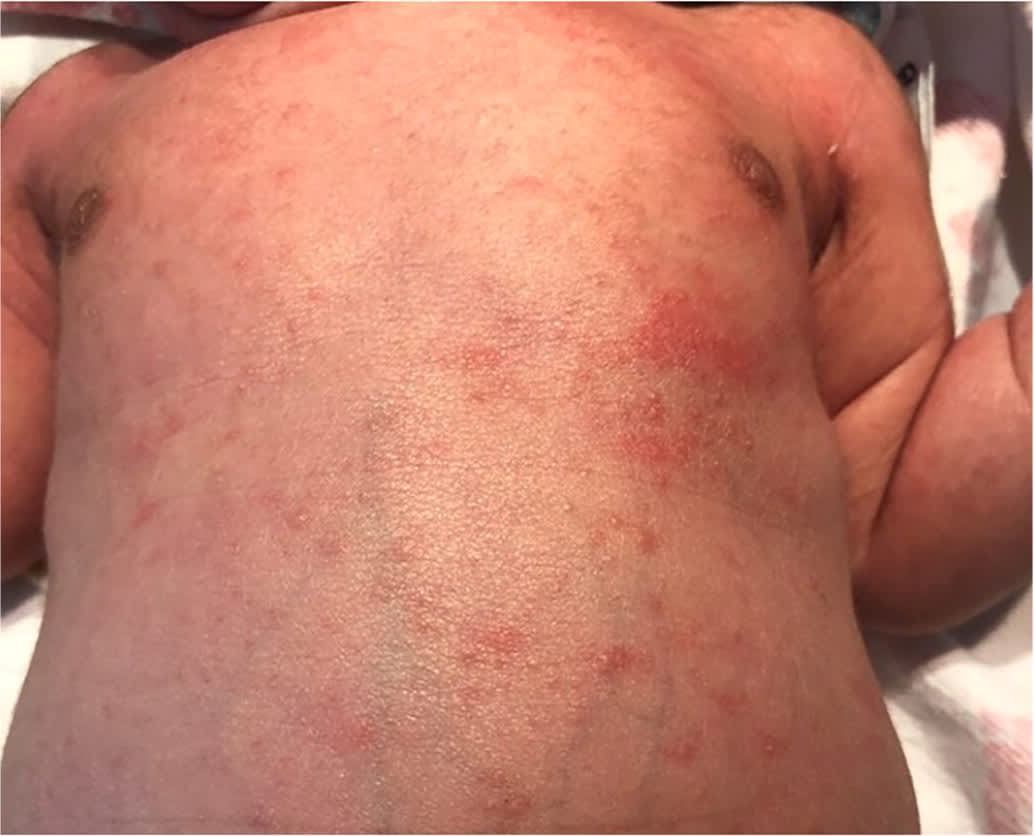
Erythema toxicum neonatorum typically presents as small pustules on a red base that are not grouped.
TRANSIENT NEONATAL PUSTULAR MELANOSIS
Transient neonatal pustular melanosis is more common in newborns with skin containing higher levels of melanin. It is a pustular rash that is present at birth. The pustules rupture and leave a characteristic pigmented macule (Figure 2). The rash is diagnosed clinically by lesions that may appear on the forehead, behind the ears, and on the neck, trunk, and extremities, including the palms and soles.12 Hyperpigmentation may persist for weeks to months before fading.2
FIGURE 2.
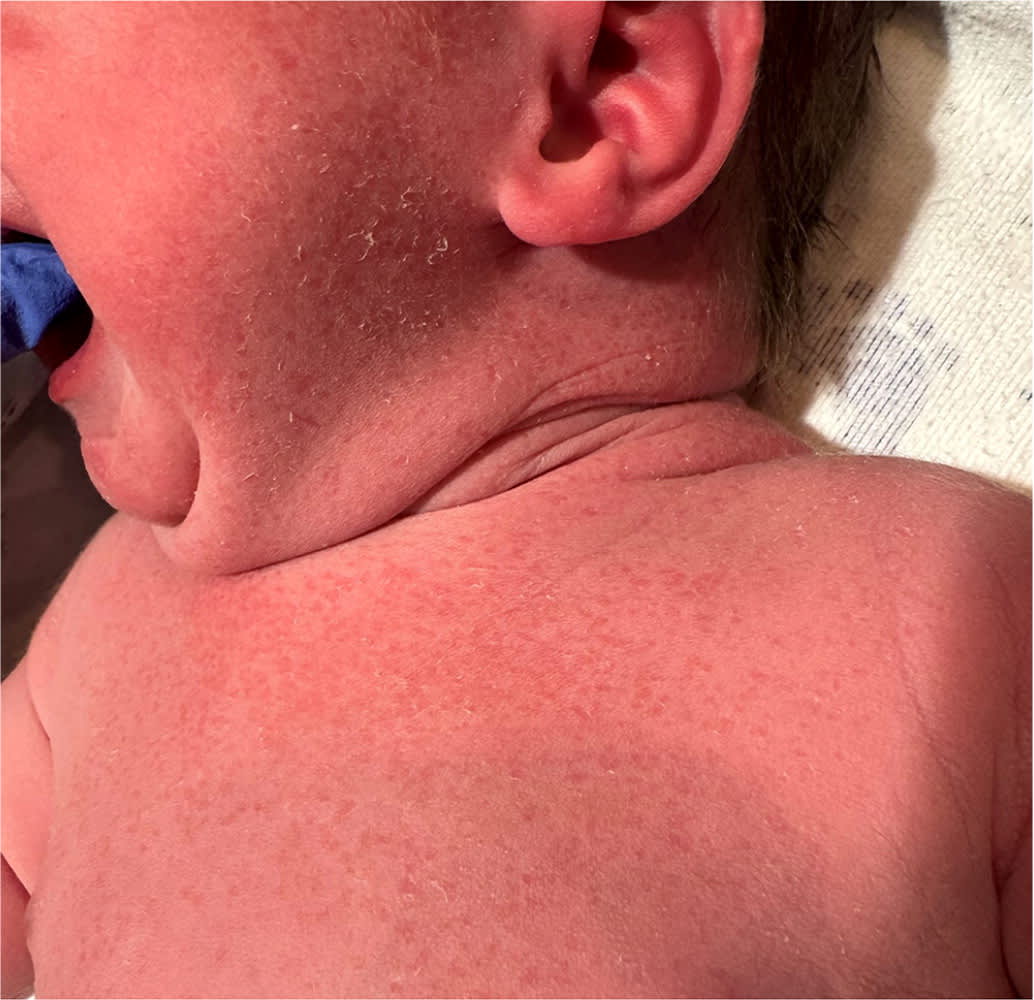
Transient neonatal pustular melanosis is a rash in which pustules rupture and leave characteristic pigmented macules that can last weeks to months. In some newborns, the pustules rupture before delivery and only hyperpigmented macules are visible at birth, as seen on the face, neck, and chest of this newborn.
NEONATAL AND INFANTILE ACNE
Neonatal acne presents with closed comedones on the forehead, nose, and cheeks that may appear pustular (Figure 3). It is not present at birth, but develops in the first four weeks of life.13 Neonatal acne is thought to be a result of sebaceous gland stimulation from newborn exposure to adult levels of endogenous hormones. Infantile acne generally presents after six weeks, lasts for six to 12 months, and may be more inflammatory in nature.14 Infantile acne does not require further evaluation in the absence of other signs of hormonal excess. Infantile acne rarely requires treatment; however, topical antimicrobials or retinoids may be used in consultation with a specialist for severe or refractory cases and concerns for scarring.15
FIGURE 3.
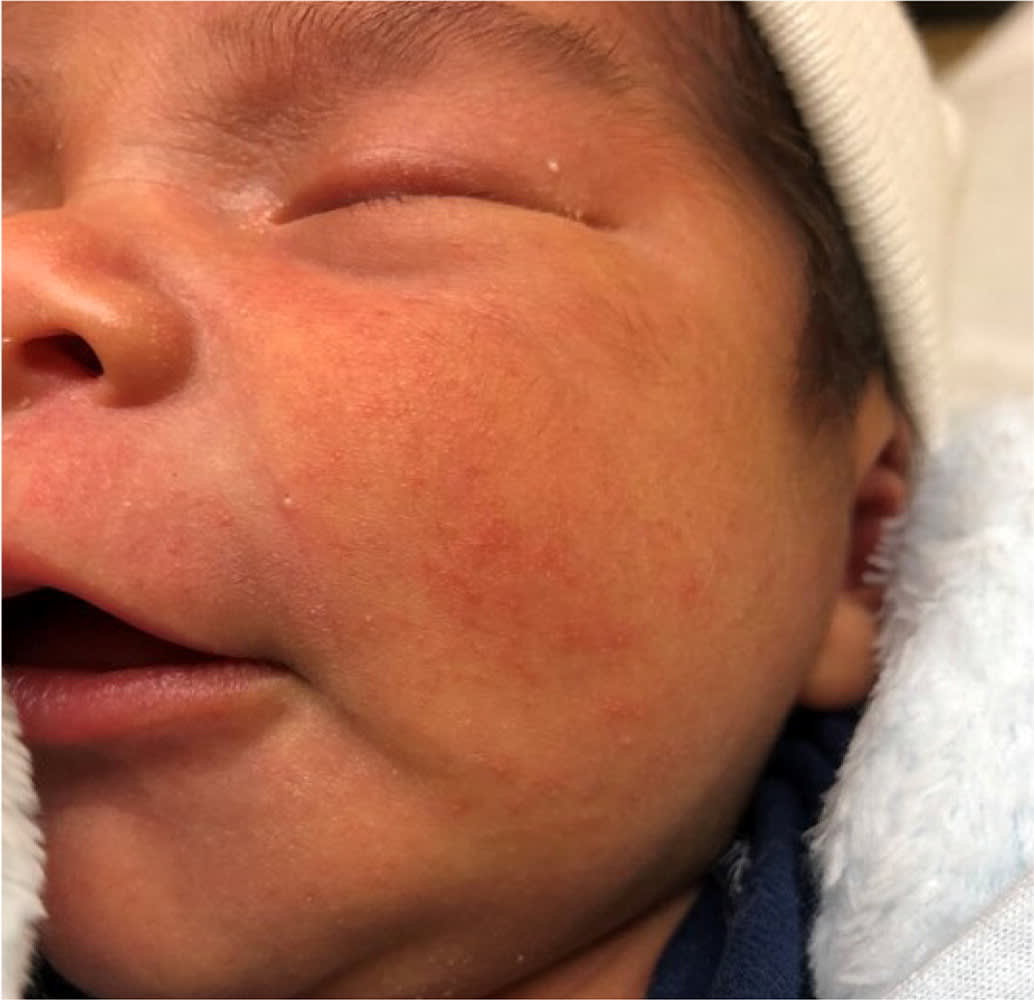
Neonatal acne most commonly presents as closed comedones on the forehead, nose, and cheeks.
MILIA
Milia consists of tiny, pearly white to yellow cysts located on the forehead, nose, and cheeks, although they can appear in other locations (Figure 4). They are secondary to retained keratin and present at birth in up to one-half of newborns. Treatment is not needed.2,16
FIGURE 4.
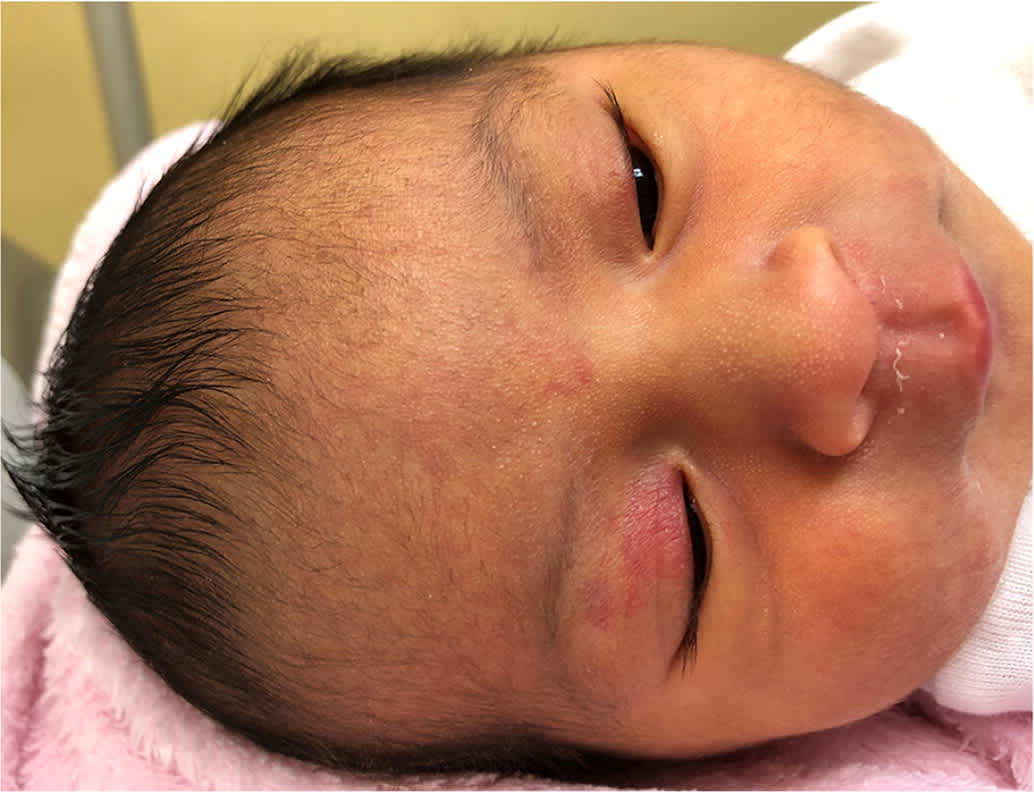
Milia are tiny, pearly white to yellow, keratin-filled cysts shown on this newborn's nose and forehead. Also note the nevus simplex on the forehead and upper eyelids.
Transient Vascular Phenomena
Transient vascular phenomena are visual representations of inappropriate or exaggerated dilation of normally formed blood vessels in response to an environmental stimulus.
CUTIS MARMORATA
Cutis marmorata is a physiologic phenomenon that presents as a reticular, bluish rash with symmetrical distribution on the trunk and extremities (Figure 5). It is caused by the dilation of capillaries and venules in response to cold temperatures. It can occur for weeks after birth and will disappear in warm temperatures.17
FIGURE 5.
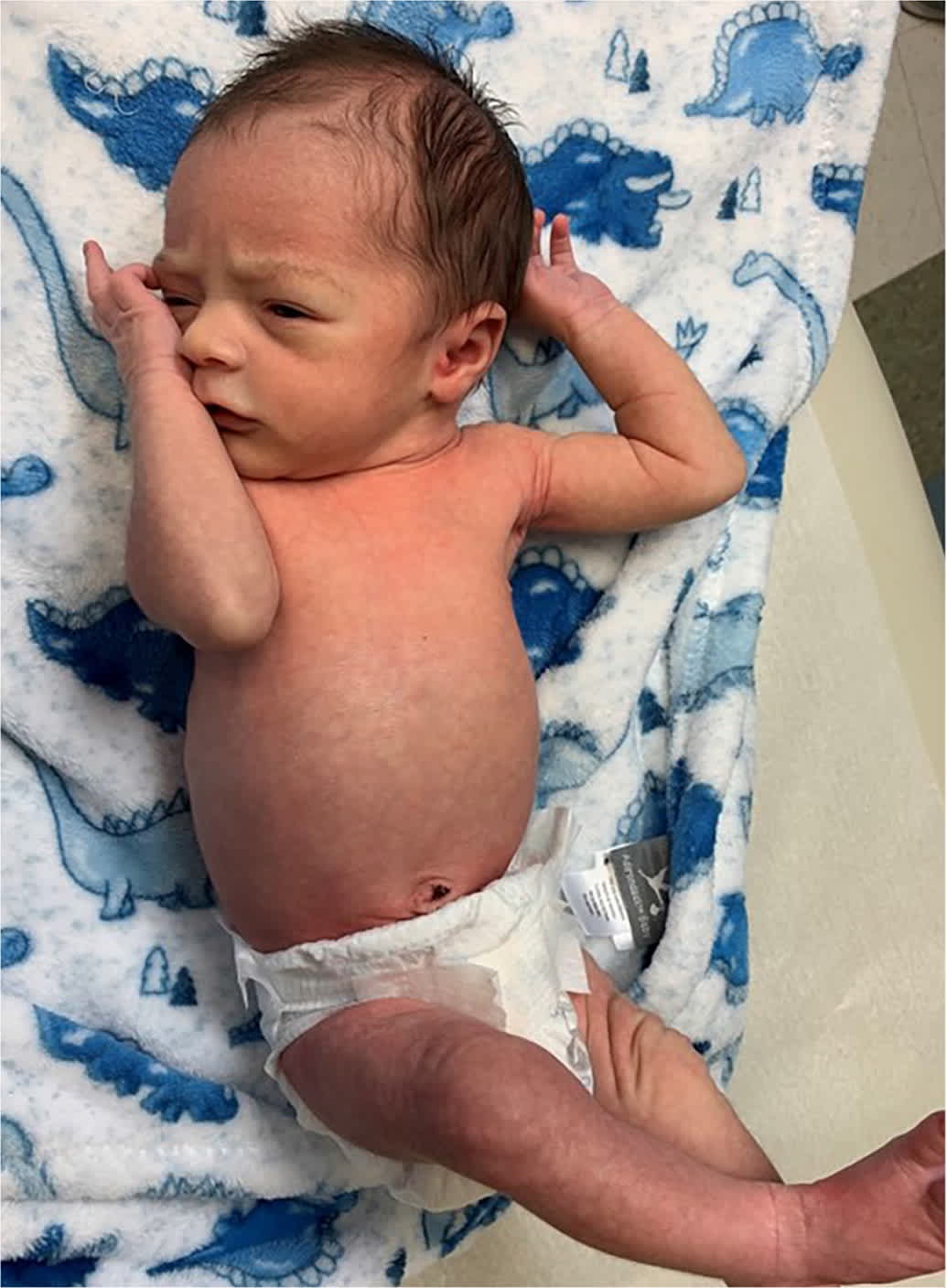
Cutis marmorata is a physiologic phenomenon in response to cold that presents as a reticular, bluish, symmetrical rash on the trunk and extremities.
Cutis marmorata telangiectatica congenita is a serious vascular anomaly that mimics physiologic cutis marmorata. Although the rash may appear similar in both conditions, cutis marmorata telangiectatica congenita should be considered if there is skin atrophy, ulceration, or unilateral distribution.17 Referral is indicated when the diagnosis is uncertain.
HARLEQUIN COLOR CHANGE
Harlequin color change affects up to 10% of newborns, especially those who are preterm or small for gestational age.18 It presents as transient, clearly demarcated areas in which one-half of the body is pale, and the other is plethoric. It generally appears between the third and fifth day of life, can persist from 30 seconds to 20 minutes, and may disappear when the newborn cries.19 It is a benign, cutaneous condition that is thought to be secondary to vasomotor instability from an immature hypothalamus. It requires no specific evaluation or treatment.19,20
This article updates a previous article on this topic by O’Connor, et al.2
Data Sources: A PubMed search was completed using the terms congenital infections, erythema toxicum neonatorum, transient neonatal pustular melanosis, neonatal and infantile acne, milia, cutis marmorata, harlequin color change, and key terms for diagnosis and management. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. The Cochrane database, UpToDate, Essential Evidence Plus, and the TRIP database were also searched. Search dates: November 2022 to February 2023, May to June 2023, and December 2023.
The authors thank the patients’ families who allowed their newborns to be photographed for this article.

