As physician payment increasingly becomes tied to value, these five habits can help you succeed.

Public and private payers are increasingly shifting the risk of providing health care from payers to physicians and other health care providers by tying reimbursement to value. This shift is part of an effort to achieve the “triple aim” of improving population health, reducing health care costs, and improving the patient care experience. The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) reaffirmed this shift and created new incentives for physicians to transition to value-based, alternative payment models. Also in 2015, the U.S. Department of Health & Human Services (HHS) announced a goal of moving 50 percent of Medicare payments into alternative payment models linked to value by 2018. The HHS announcement came the same week that the Health Care Transformation Task Force, an alliance of major health systems, insurers, and other industry players, announced a goal of placing 75 percent of its business into value-based payment arrangements by 2020.1 The year 2015 also saw the creation of more than 400 Shared Savings Accountable Care Organizations (ACOs) serving nearly 7.2 million beneficiaries, or 14 percent of the Medicare population.2 Medicaid, which covers more than 70 million people, has many states now participating in alternative payment models as well.
Although the market is moving rapidly toward valued-based payment, many physicians understandably feel skeptical, reluctant, or unprepared. A recent survey of primary care physicians across the country showed that only 41 percent felt they know which quality measures apply to their patients under value-based models, 65 percent said they do not have all the health care information they need about their patients, 36 percent said they were satisfied with access to patient data within their existing workflow, and 68 percent felt they do not have the tools to succeed in a value-based system.3 What can be done to help primary care physicians who are already overburdened by administrative tasks? How can they perform well under MACRA? What can physician members of an ACO do to contribute to their organization's success, and their own? The following five principles, which have helped my organization achieve early wins in value-based payment, may assist other physicians in addressing these issues and maximizing their earning potential.
1. Get to know your patients and your data
To accomplish its goal of tying Medicare payments to quality or value, the Centers for Medicare & Medicaid Services (CMS) must know exactly which Medicare patients are yours – and which are not. Attribution models vary. For example, under MACRA's Merit-Based Incentive Payment System (MIPS), patient attribution is retrospective, looking back one year for a plurality of allowed charges for outpatient services only. Each Medicare beneficiary is attributed to a single physician based on his or her National Provider Identifier (NPI)/taxpayer ID number (TIN) or to a group. (See “Patient Attribution: Why It Matters More Than Ever,” FPM, November/December 2016.)
It is important to know how your payers attribute patients and whether their assignments are accurate because this can affect whether you receive payment incentives or penalties and help you to target resources effectively. If you find a discrepancy in patient attribution, designate a staff member to contact a payer representative who can assist in correcting this problem. Of course, given the confusing and imperfect nature of attribution models, you may find that your time is better spent providing the care itself as opposed to analyzing reports and debating which patients are yours.
Once you have a basic understanding of patient attribution, you then need to make sure you are tracking the right data for your patients. Typically quality measures include three categories:
- 1) Activities that contribute to positive health outcomes (e.g., smoking cessation counseling),
- 2) Measures of the effectiveness of care provided (e.g., diabetes control),
- 3) Patient satisfaction.
(This article will discuss specific quality measures in section four.)
Physicians need to have timely access to this patient data and the resources to manage it, and the data itself needs to be accurate. Ideally, your electronic health record (EHR) system will integrate quality metrics. Regardless, you and your staff must know how to capture key data points in the correct portion of the EHR so that they can be tracked and reported. Explore the resources available in your practice to manage and analyze patient data, and utilize these resources to maximize performance. For example, each EHR should have some internal quality reporting options. Make sure these options are turned on and being used. Your EHR data is invariably better than claims data for quality reporting, although for internal purposes looking at both clinical and claims data often provides the most complete picture.
When it comes to claims data, one potentially useful resource is Medicare's Quality and Resource Use Report. This is essentially an annual report card of a practice's performance compared with others, which determines future Medicare reimbursement. Two weaknesses of this report are that the data are not provided at the individual level (except for solo physicians) and are nearly a year old by the time the practice receives the report. (For more on this topic, including how to view your annual report, see “What You Need to Know About Medicare's New ‘Quality and Resource Use Report,’” FPM, November/December 2015.)
2. Surround yourself with a dedicated team
The providers and organizations that are the most successful in value-based payment models not only are invested in information technology systems and data analysis but also have staff dedicated to identifying high-risk patients and monitoring their progress toward quality metrics. Below are several key functions you will need to assign to members of your team:
- Check that the quality metric data is accurately assigned,
- Update any missing metrics that have been met,
- Contact patients who need to be seen to achieve specific quality metrics,
- Order protocol-based labs or studies that patients need to satisfy outcome metrics,
- Review patient satisfaction surveys and provide feedback to the physician and staff on how to improve their scores.
Some groups may already have the capacity to carry out these functions or may be able to create capacity by working smarter. For other groups, adding these functions may mean increasing staff costs with the hope that this investment will pay off down the road.
The composition of the team depends on the practice or organization. One approach is a physician-led “care team” composed of clinicians (nurse practitioners or physician assistants), medical staff, and administrative staff who are fully invested in achieving quality metrics. A larger provider team, as well as effective intra-team communication and problem solving, can help practices engage in data-driven, continuous quality improvement.4
3. Be proactive with previsit planning
There are several ways of putting previsit planning into practice. A first step is to “plan forward” using a checklist to anticipate not only the medical needs of the patient but also any quality measures that can be addressed for the scheduled visit. The provider, the nurse, or a staff member on the care team can do a “look back” at the chart a week or so before the next visit. If needed, the provider (or a staff member using predetermined protocols) can place orders such as labs based on the patient's conditions or medications. The results would then be available for review at the patient's visit. This would serve as an opportunity to capture or satisfy quality metrics that may be needed (such as ordering labs for a patient on ACE-inhibitors). Previsit phone calls for complex patients can be used to reconcile medications, anticipate problems, and screen for fall risks and depression; all of these items would need to be confirmed at the face-to-face visit. A morning mini-huddle involving the provider and the medical assistant/nurse or care team can be helpful to prepare everyone to provide the best possible care to patients. (See “Putting Pre-Visit Planning Into Practice,” FPM, November/December 2015.)
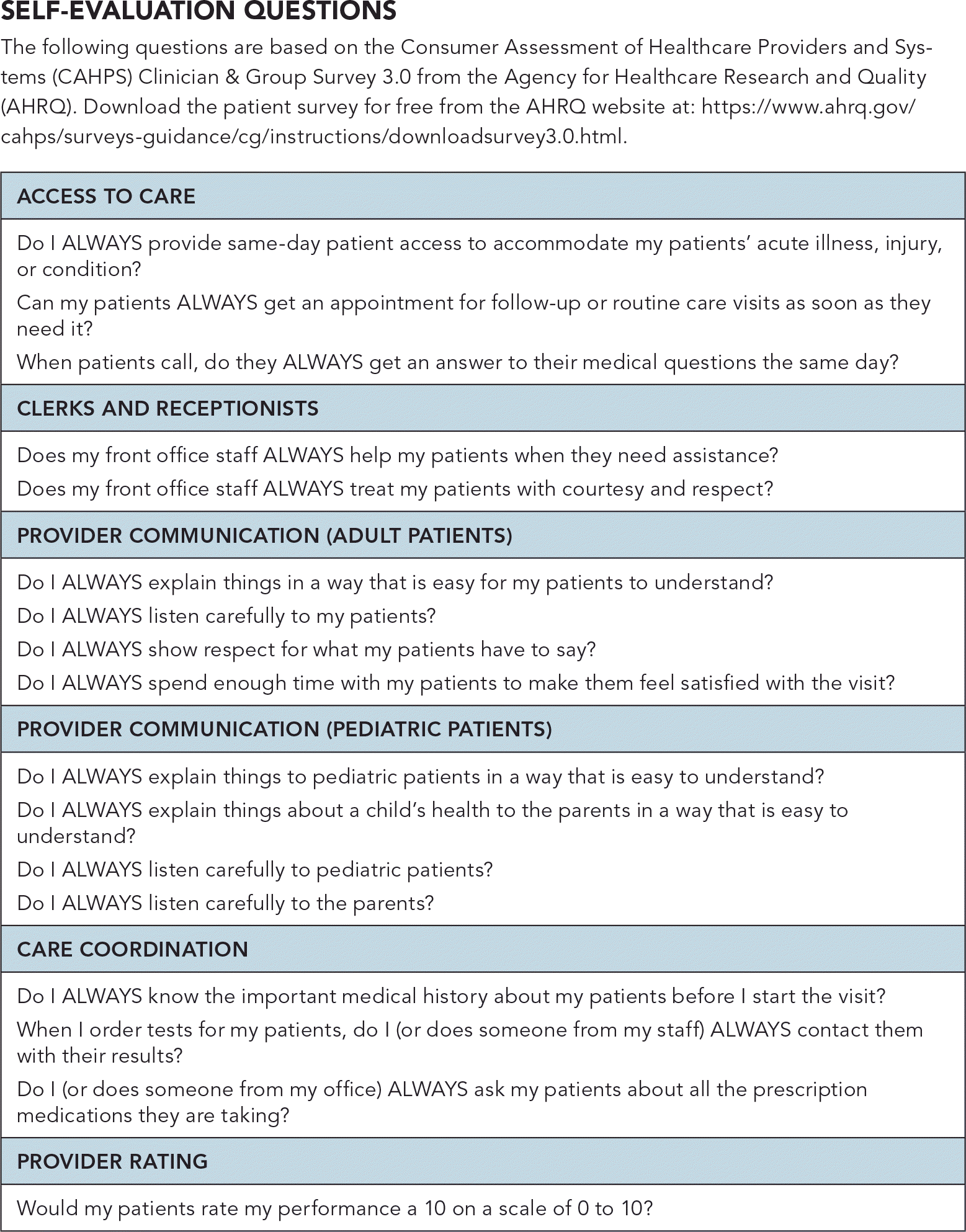
One additional aspect of the visit that providers need to plan for is how the patient will perceive the care he or she receives. The Consumer Assessment of Healthcare Providers and Systems (CAHPS), a program of the Agency for Healthcare Research and Quality, develops standardized patient questionnaires that focus on the patient experience, which can determine CMS payments. CAHPS surveys are used in fee-for-value initiatives and can affect payments to providers. The table below provides “Self-evaluation questions” the provider can ask about his or her accessibility, staff interaction, communication, care coordination, and personal rating. These questions are derived from the CAHPS Clinician & Group Survey 3.0 and written with the adverb “always” because that is the choice the provider should strive for in each area. Knowing what these surveys ask can prepare the provider with the right mindset to deliver a fulfilling patient experience before, during, and after the visit. It can also help raise quality achievement scores tied to compensation.
SELF-EVALUATION QUESTIONS
The following questions are based on the Consumer Assessment of Healthcare Providers and Systems (CAHPS) Clinician & Group Survey 3.0 from the Agency for Healthcare Research and Quality (AHRQ). Download the patient survey for free from the AHRQ website.
| ACCESS TO CARE |
| Do I ALWAYS provide same-day patient access to accommodate my patients' acute illness, injury, or condition? Can my patients ALWAYS get an appointment for follow-up or routine care visits as soon as they need it? When patients call, do they ALWAYS get an answer to their medical questions the same day? |
| CLERKS AND RECEPTIONISTS |
| Does my front office staff ALWAYS help my patients when they need assistance? Does my front office staff ALWAYS treat my patients with courtesy and respect? |
| PROVIDER COMMUNICATION (ADULT PATIENTS) |
| Do I ALWAYS explain things in a way that is easy for my patients to understand? Do I ALWAYS listen carefully to my patients? Do I ALWAYS show respect for what my patients have to say? Do I ALWAYS spend enough time with my patients to make them feel satisfied with the visit? |
| PROVIDER COMMUNICATION (PEDIATRIC PATIENTS) |
| Do I ALWAYS explain things to pediatric patients in a way that is easy to understand? Do I ALWAYS explain things about a child's health to the parents in a way that is easy to understand? Do I ALWAYS listen carefully to pediatric patients? Do I ALWAYS listen carefully to the parents? |
| CARE COORDINATION |
| Do I ALWAYS know the important medical history about my patients before I start the visit? When I order tests for my patients, do I (or does someone from my staff) ALWAYS contact them with their results? Do I (or does someone from my office) ALWAYS ask my patients about all the prescription medications they are taking? |
| PROVIDER RATING |
| Would my patients rate my performance a 10 on a scale of 0 to 10? |
4. Review pertinent quality measures before seeing the patient
Because different entities require different quality measures, keeping tracking of them is a serious challenge for physicians and their staff. The measures compiled in this article can serve as “checklists” for physicians to review prior to seeing their patients. The measures are organized into four major categories (Screening, Prevention, & Medication Safety; Acute Care Conditions; Chronic Care Conditions; and Older Adult Care), as well as by age and disease type, and are written in an “active voice” so physicians can take the appropriate action to meet the quality measure.
The tables integrate measures from three sources: the Core Quality Measures Collaborative, the Integrated HealthCare Association's Value Based P4P program, and the National Committee for Quality Assurance's (NCQA's) Healthcare Effectiveness Data and Information Set (HEDIS).
The Core Quality Measures Collaborative was formed in 2014, and it included federal, state, and commercial insurance plan leaders, CMS and National Quality Forum leaders, and national physician organizations. The goal was to establish broadly agreed upon core quality measures that could be used across payers, reducing the reporting complexity for physicians. The core measure sets were released in early 2016. The American Academy of Family Physicians has recommended that payers offering alternative payment models for primary care incorporate the core measure set for “Accountable Care Organizations, Patient Centered Medical Homes, and Primary Care.”5
Because implementation of the core quality measures is just beginning, it is helpful to look at an older model as well. The California-based Integrated HealthCare Association's Value Based P4P program is the largest alternative payment program in the United States with participation of 10 health plans and more than 200 physician organizations caring for 9.6 million patients enrolled in HMO and point of service plans. The program's measure set has been used across multiple health plans since 2010.
Last but not least are the HEDIS measures. This is the most widely used set of performance measures in the managed care industry.
QUALITY MEASURES FOR PRIMARY CARE
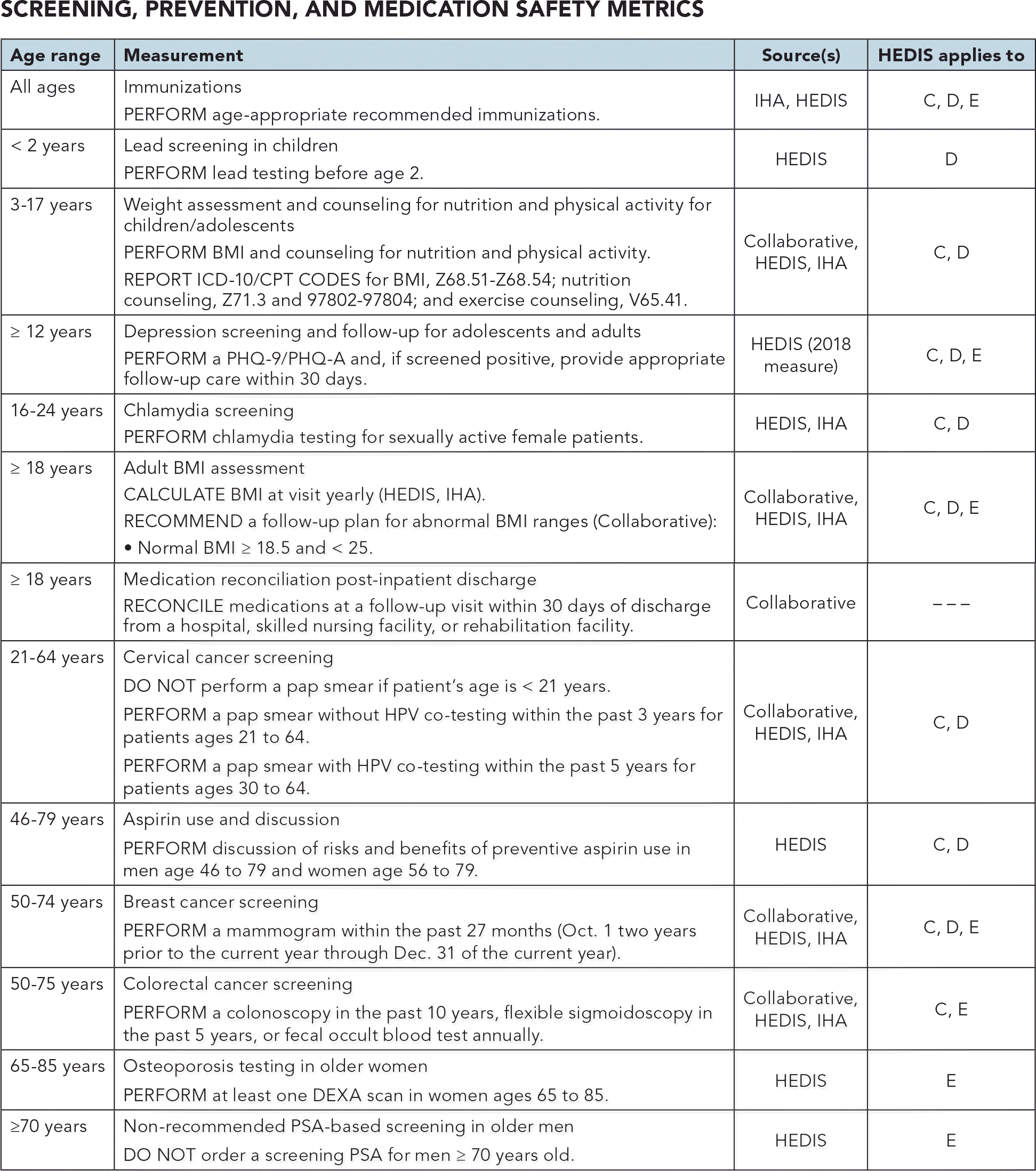
The following metrics should be used as general guidelines. To review details and exclusions to each measure (available for purchase from NCQA), visit http://bit.ly/2oG7ufl. Key: C = Commercial, D = MedicaiD, and E = MedicarE.
SCREENING, PREVENTION, AND MEDICATION SAFETY METRICS
| Age range | Measurement | Source(s) | HEDIS applies to |
|---|---|---|---|
| All ages | Immunizations PERFORM age-appropriate recommended immunizations. | IHA, HEDIS | C, D, E |
| < 2 years | Lead screening in children PERFORM lead testing before age 2. | HEDIS | D |
| 3–17 years | Weight assessment and counseling for nutrition and physical activity for children/adolescents PERFORM BMI and counseling for nutrition and physical activity. REPORT ICD-10/CPT CODES for BMI, Z68.51-Z68.54; nutrition counseling, Z71.3 and 97802–97804; and exercise counseling, V65.41. | Collaborative, HEDIS, IHA | C, D |
| ≥ 12 years | Depression screening and follow-up for adolescents and adults PERFORM a PHQ-9/PHQ-A and, if screened positive, provide appropriate follow-up care within 30 days. | HEDIS (2018 measure) | C, D, E |
| 16–24 years | Chlamydia screening PERFORM chlamydia testing for sexually active female patients. | HEDIS, IHA | C, D |
| ≥ 18 years | Adult BMI assessment CALCULATE BMI at visit yearly (HEDIS, IHA). RECOMMEND a follow-up plan for abnormal BMI ranges (Collaborative):
| Collaborative, HEDIS, IHA | C, D, E |
| ≥ 18 years | Medication reconciliation post-inpatient discharge RECONCILE medications at a follow-up visit within 30 days of discharge from a hospital, skilled nursing facility, or rehabilitation facility. | Collaborative | – – – |
| 21–64 years | Cervical cancer screening DO NOT perform a pap smear if patient's age is < 21 years. PERFORM a pap smear without HPV co-testing within the past 3 years for patients ages 21 to 64. PERFORM a pap smear with HPV co-testing within the past 5 years for patients ages 30 to 64. | Collaborative, HEDIS, IHA | C, D |
| 46–79 years | Aspirin use and discussion PERFORM discussion of risks and benefits of preventive aspirin use in men age 46 to 79 and women age 56 to 79. | HEDIS | C, D |
| 50–74 years | Breast cancer screening PERFORM a mammogram within the past 27 months (Oct. 1 two years prior to the current year through Dec. 31 of the current year). | Collaborative, HEDIS, IHA | C, D, E |
| 50–75 years | Colorectal cancer screening PERFORM a colonoscopy in the past 10 years, flexible sigmoidoscopy in the past 5 years, or fecal occult blood test annually. | Collaborative, HEDIS, IHA | C, E |
| 65–85 years | Osteoporosis testing in older women PERFORM at least one DEXA scan in women ages 65 to 85. | HEDIS | E |
| ≥70 years | Non-recommended PSA-based screening in older men DO NOT order a screening PSA for men ≥ 70 years old. | HEDIS | E |
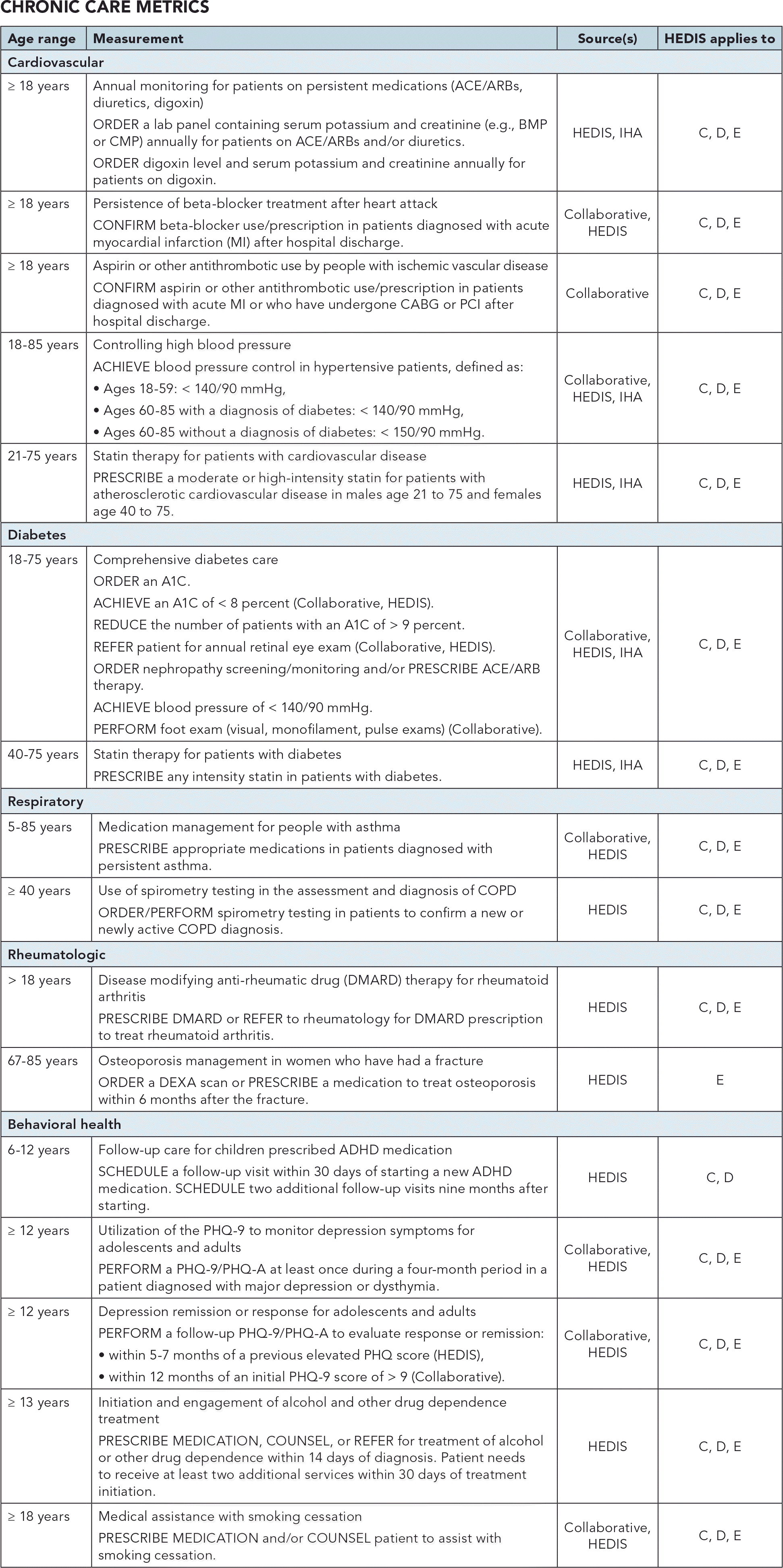
CHRONIC CARE METRICS
| Age range | Measurement | Source(s) | HEDIS applies to |
|---|---|---|---|
| Cardiovascular | |||
| ≥ 18 years | Annual monitoring for patients on persistent medications (ACE/ARBs, diuretics, digoxin) ORDER a lab panel containing serum potassium and creatinine (e.g., BMP or CMP) annually for patients on ACE/ARBs and/or diuretics. ORDER digoxin level and serum potassium and creatinine annually for patients on digoxin. | HEDIS, IHA | C, D, E |
| ≥ 18 years | Persistence of beta-blocker treatment after heart attack CONFIRM beta-blocker use/prescription in patients diagnosed with acute myocardial infarction (MI) after hospital discharge. | Collaborative, HEDIS | C, D, E |
| ≥ 18 years | Aspirin or other antithrombotic use by people with ischemic vascular disease CONFIRM aspirin or other antithrombotic use/prescription in patients diagnosed with acute MI or who have undergone CABG or PCI after hospital discharge. | Collaborative | C, D, E |
| 18–85 years | Controlling high blood pressure ACHIEVE blood pressure control in hypertensive patients, defined as:
| Collaborative, HEDIS, IHA | C, D, E |
| 21–75 years | Statin therapy for patients with cardiovascular disease PRESCRIBE a moderate or high-intensity statin for patients with atherosclerotic cardiovascular disease in males age 21 to 75 and females age 40 to 75. | HEDIS, IHA | C, D, E |
| Diabetes | |||
| 18–75 years | Comprehensive diabetes care ORDER an A1C. ACHIEVE an A1C of < 8 percent (Collaborative, HEDIS). REDUCE the number of patients with an A1C of > 9 percent. REFER patient for annual retinal eye exam (Collaborative, HEDIS). ORDER nephropathy screening/monitoring and/or PRESCRIBE ACE/ARB therapy. ACHIEVE blood pressure of < 140/90 mmHg. PERFORM foot exam (visual, monofilament, pulse exams) (Collaborative). | Collaborative, HEDIS, IHA | C, D, E |
| 40–75 years | Statin therapy for patients with diabetes PRESCRIBE any intensity statin in patients with diabetes. | HEDIS, IHA | C, D, E |
| Respiratory | |||
| 5–85 years | Medication management for people with asthma PRESCRIBE appropriate medications in patients diagnosed with persistent asthma. | Collaborative, HEDIS | C, D, E |
| ≥ 40 years | Use of spirometry testing in the assessment and diagnosis of COPD ORDER/PERFORM spirometry testing in patients to confirm a new or newly active COPD diagnosis. | HEDIS | C, D, E |
| Rheumatologic | |||
| > 18 years | Disease modifying anti-rheumatic drug (DMARD) therapy for rheumatoid arthritis PRESCRIBE DMARD or REFER to rheumatology for DMARD prescription to treat rheumatoid arthritis. | HEDIS | C, D, E |
| 67–85 years | Osteoporosis management in women who have had a fracture ORDER a DEXA scan or PRESCRIBE a medication to treat osteoporosis within 6 months after the fracture. | HEDIS | E |
| Behavioral health | |||
| 6–12 years | Follow-up care for children prescribed ADHD medication SCHEDULE a follow-up visit within 30 days of starting a new ADHD medication. SCHEDULE two additional follow-up visits nine months after starting. | HEDIS | C, D |
| ≥ 12 years | Utilization of the PHQ-9 to monitor depression symptoms for adolescents and adults PERFORM a PHQ-9/PHQ-A at least once during a four-month period in a patient diagnosed with major depression or dysthymia. | Collaborative, HEDIS | C, D, E |
| ≥ 12 years | Depression remission or response for adolescents and adults PERFORM a follow-up PHQ-9/PHQ-A to evaluate response or remission:
| Collaborative, HEDIS | C, D, E |
| ≥ 13 years | Initiation and engagement of alcohol and other drug dependence treatment PRESCRIBE MEDICATION, COUNSEL, or REFER for treatment of alcohol or other drug dependence within 14 days of diagnosis. Patient needs to receive at least two additional services within 30 days of treatment initiation. | HEDIS | C, D, E |
| ≥ 18 years | Medical assistance with smoking cessation PRESCRIBE MEDICATION and/or COUNSEL patient to assist with smoking cessation. | Collaborative, HEDIS | C, D, E |
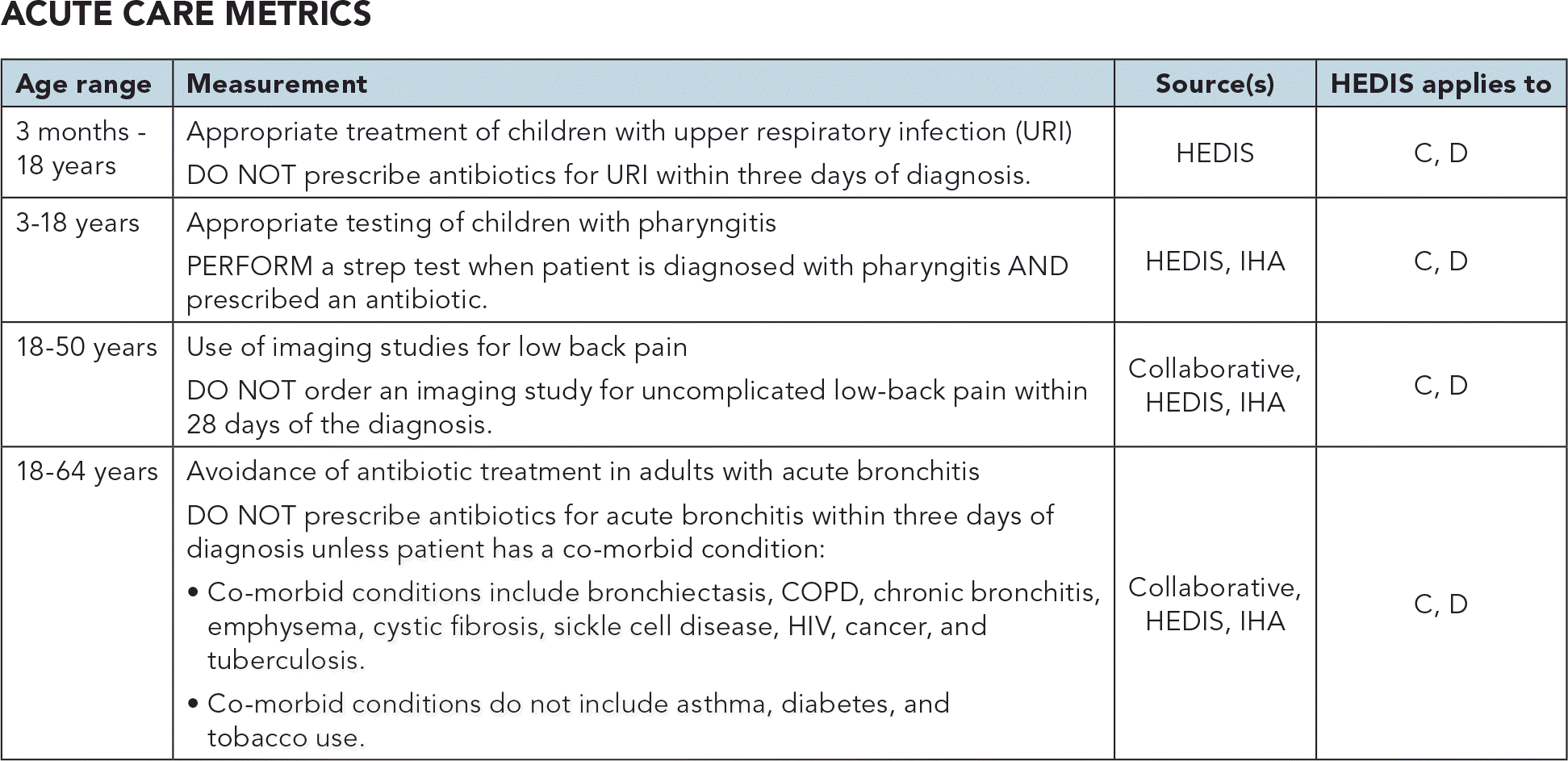
ACUTE CARE METRICS
| Age range | Measurement | Source(s) | HEDIS applies to |
|---|---|---|---|
| 3 months - 18 years | Appropriate treatment of children with upper respiratory infection (URI) DO NOT prescribe antibiotics for URI within three days of diagnosis. | HEDIS | C, D |
| 3–18 years | Appropriate testing of children with pharyngitis PERFORM a strep test when patient is diagnosed with pharyngitis AND prescribed an antibiotic. | HEDIS, IHA | C, D |
| 18–50 years | Use of imaging studies for low back pain DO NOT order an imaging study for uncomplicated low-back pain within 28 days of the diagnosis. | Collaborative, HEDIS, IHA | C, D |
| 18–64 years | Avoidance of antibiotic treatment in adults with acute bronchitis DO NOT prescribe antibiotics for acute bronchitis within three days of diagnosis unless patient has a co-morbid condition: • Co-morbid conditions include bronchiectasis, COPD, chronic bronchitis, emphysema, cystic fibrosis, sickle cell disease, HIV, cancer, and tuberculosis. • Co-morbid conditions do not include asthma, diabetes, and tobacco use. | Collaborative, HEDIS, IHA | C, D |
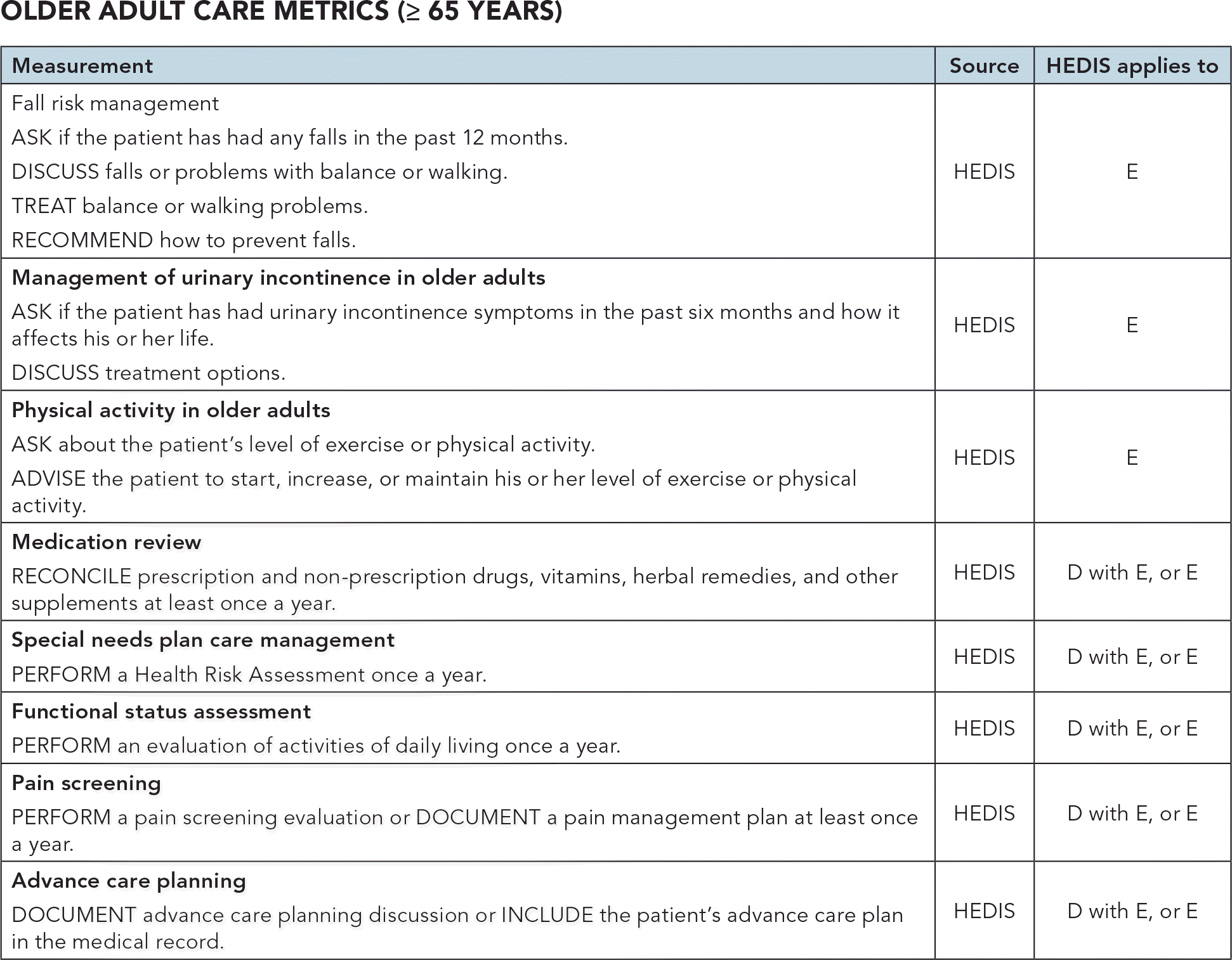
OLDER ADULT CARE METRICS (≥ 65 YEARS)
| Measurement | Source | HEDIS applies to |
|---|---|---|
| Fall risk management ASK if the patient has had any falls in the past 12 months. DISCUSS falls or problems with balance or walking. TREAT balance or walking problems. RECOMMEND how to prevent falls. | HEDIS | E |
| Management of urinary incontinence in older adults ASK if the patient has had urinary incontinence symptoms in the past six months and how it affects his or her life. DISCUSS treatment options. | HEDIS | E |
| Physical activity in older adults ASK about the patient's level of exercise or physical activity. ADVISE the patient to start, increase, or maintain his or her level of exercise or physical activity. | HEDIS | E |
| Medication review RECONCILE prescription and non-prescription drugs, vitamins, herbal remedies, and other supplements at least once a year. | HEDIS | D with E, or E |
| Special needs plan care management PERFORM a Health Risk Assessment once a year. | HEDIS | D with E, or E |
| Functional status assessment PERFORM an evaluation of activities of daily living once a year. | HEDIS | D with E, or E |
| Pain screening PERFORM a pain screening evaluation or DOCUMENT a pain management plan at least once a year. | HEDIS | D with E, or E |
| Advance care planning DOCUMENT advance care planning discussion or INCLUDE the patient's advance care plan in the medical record. | HEDIS | D with E, or E |
5. Code correctly to get credit for the work you're doing
If you do not understand the basics of coding, you will miss opportunities to capture, get credit for, and bill for medically necessary services you provide to Medicare beneficiaries and other patients. Your documentation should match the services performed, of course, and your code selection should follow CPT, ICD-10, and Medicare guidelines.
Under value-based care, it is increasingly important to manage high-risk patients, helping them avoid costly care, and to document what you've done. To address the multiple, complex medical issues of older or sicker patients during their visits, practices need to consider creating adequate appointment time slots, perhaps 30 to 40 minutes rather than the standard 15 to 20 minutes in some cases.
Chronic care management and transitional care management codes are relatively new ways to get paid for managing high-risk patients. (See “Four Coding and Payment Opportunities You Might Be Missing,” FPM, May/June 2016.) In addition, the annual wellness visit (AWV) benefit for Medicare beneficiaries can be billed along with a significant, separately identifiable, medically necessary evaluation and management (E/M) service if you document both services and attach modifier 25 to the E/M service. (See “Medicare Annual Wellness Visits: How to Get Patients and Physicians on Board,” FPM, March/April 2017.) Performing these visits with a team approach using a two-part visit workflow can be helpful. (See “Making Medicare Wellness Visits Work in Practice,” FPM, September/October 2012.)
When you review and address chronic medical conditions for Medicare Advantage patients, this provides yet another opportunity to accurately capture Hierarchical Condition Category codes to drive “risk adjustment factor” scores, earn shared savings, and avoid shared loss when taking care of higher risk patients. (See “HCC Coding, Risk Adjustment, and Physician Income: What You Need to Know,” FPM, September/October 2016.)
A complete list of Medicare preventive services with accompanying HCPCS/CPT codes can be found online.
Final words
Your performance this year will affect your Medicare payments in 2019 when MACRA takes full effect. Physicians in MIPS will receive payment increases or penalties based on their performance relative to other physicians in the same track. Qualified physicians in an advanced alternative payment model (AAPM) will receive a lump sum bonus annually, and in 2026 will receive an annual update of 0.75 percent under the Medicare physician fee schedule. (See “Making Sense of MACRA, Part 2: Value-Based Payment and Your Future,” FPM, January/February 2017.)
Although physicians may be justified in feeling skeptical or overwhelmed by the shift to value-based payment, inaction will not serve us well. We cannot ignore the changes occurring as health care transitions from fee-for-service to fee-for-value. We must begin to embrace quality measures to achieve the triple aim of improving population health, reducing health care costs, and improving the patient care experience. Perhaps, with the right team in place to provide support and the right resources in place to achieve the desired metrics, practices can go beyond the triple aim and achieve the quadruple aim, improving the work life of physicians as well.

