Medical Students
Succeed in medical school and learn more about the family medicine specialty.
Why Choose Family Medicine?
With the broadest spectrum of practice of all the medical specialties, family medicine provides you the unique opportunity to tailor the specialty to fit your own needs and interests. For the past 10 years, family medicine has been the most recruited specialty in the United States. Rising demand has also led to rising salaries. See what makes it so appealing - and find out why family medicine might just be your perfect match!
What is Family Medicine?
9 Reasons to Choose Family Medicine
Discover Family Medicine Career Options
Explore Income & Lifestyle Expectations
Training Requirements for Family Physicians
Did you know the average full-time family physician reported a total compensation of $274,359 in 2022?
Demand for family physicians continues to grow - along with their average income. Learn more with our Career Benchmark Dashboard.
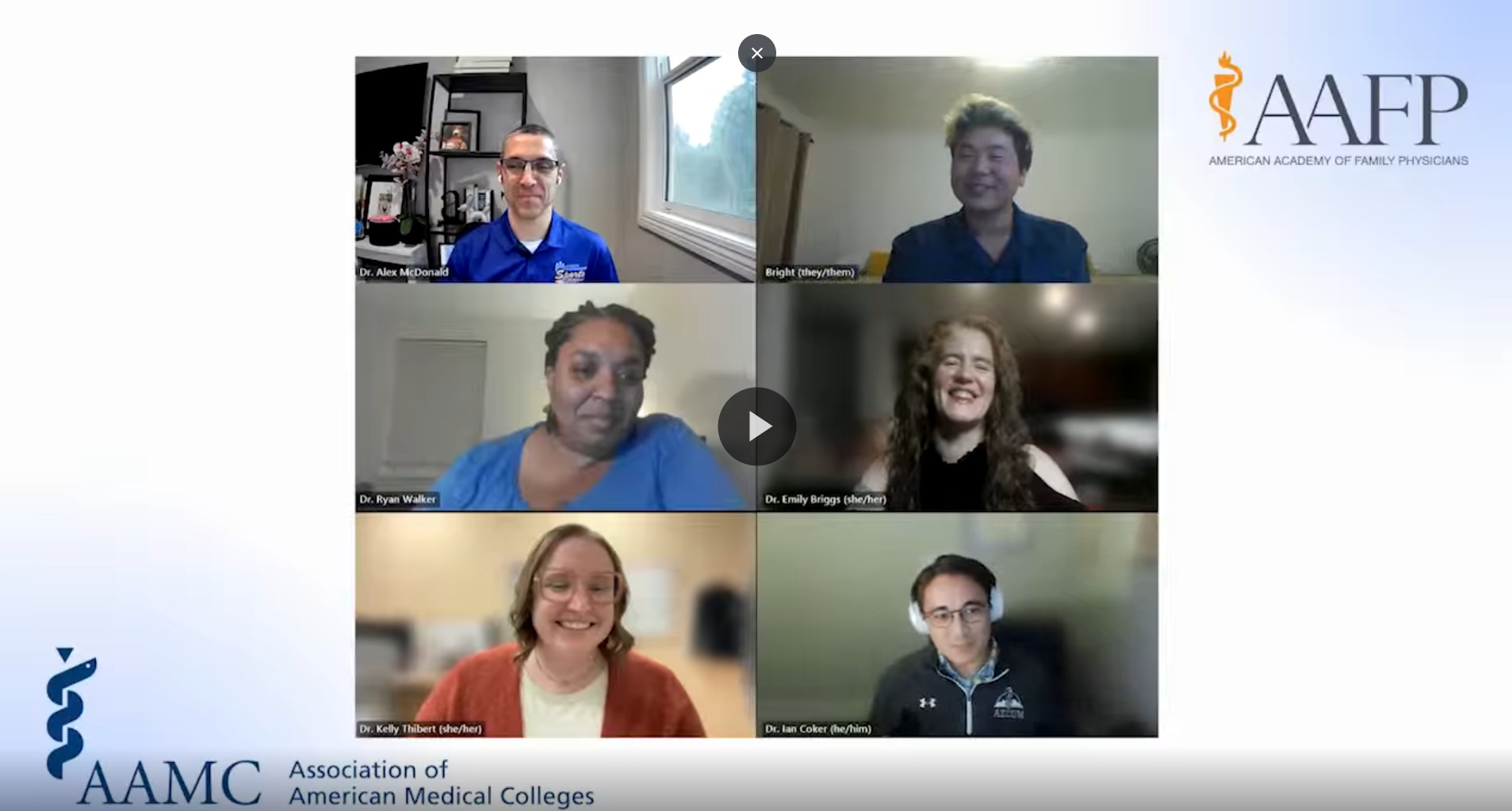
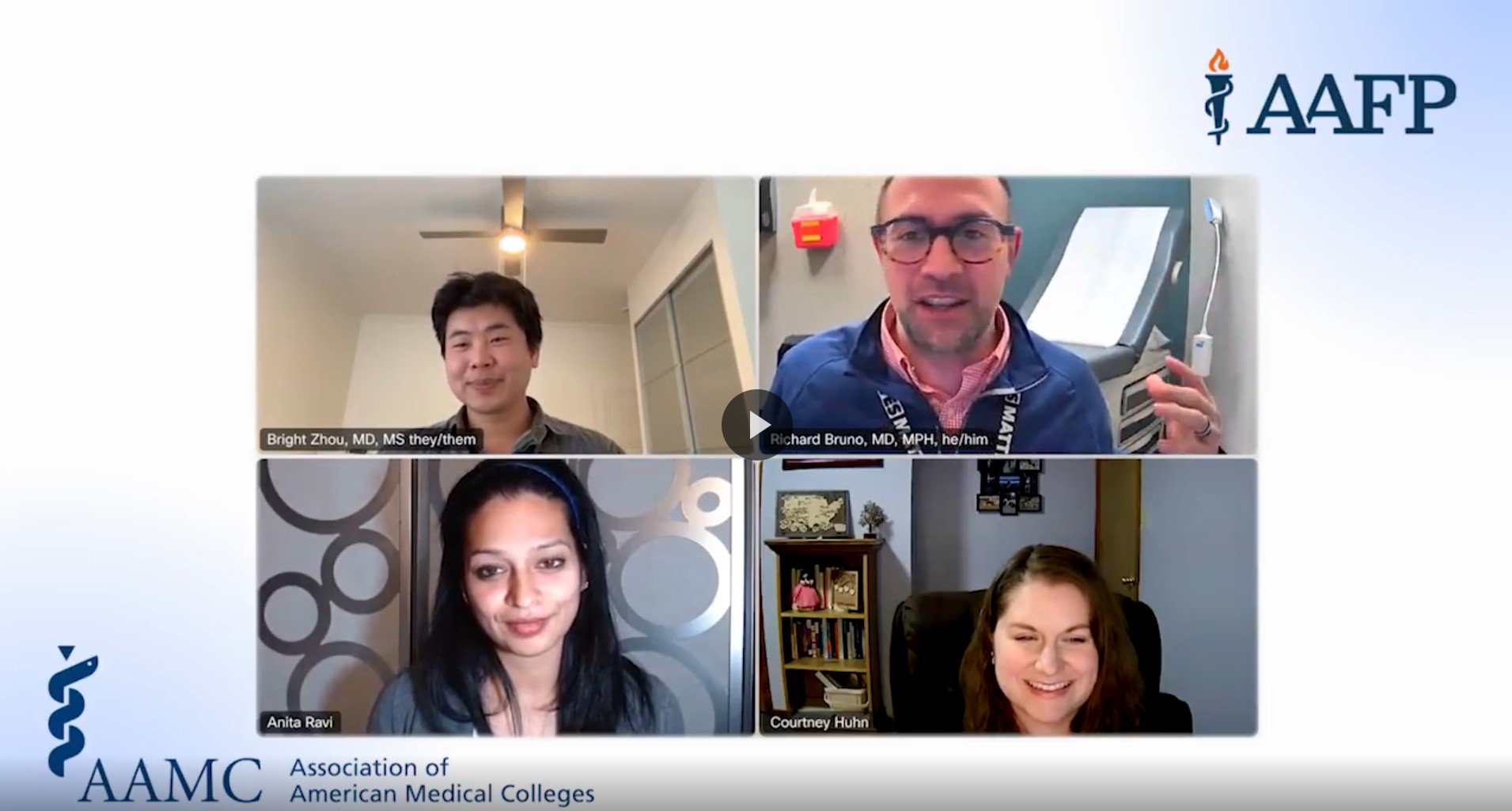
New for Medical Students
This video series, in partnership with AAMC, is focused on helping you choose a meaningful career that matches your values and interests. Hear from dynamic family medicine physicians showcasing diverse career paths and offering inspiration and advice for future physicians.
Not an AAFP member? Medical student membership is free and applying is quick and easy. Join now.
Get Into Medical School
Start your journey toward a career in family medicine. Learn what it takes to get into medical school, and plan for attending and managing medical school debt.
Is a Career in Medicine for You
Get Into Medical School
Plan for Medical School
Manage Medical School Debt
Find a Family Medicine Program
Succeed in Medical School
Medical school isn't easy, but the AAFP's study tools and resources can help you along the way.
Deciding on a Specialty
Research Clinical Topics & Procedures
Plan Your Clerkships & Electives
Global Health Opportunities
Finding a Mentor
Attend Family Medicine Conferences
Listen to the AFP Podcast

Become a Resident
Once you approach the end of your medical school education, the next step is matching with a family medicine residency program. Find out more about the Match process, preparing for residency interviews, and finding a residency program that's right for you.
Understand the Match Process
Choosing a Residency Program
Find a Residency Program
Preparing your Residency Application
Residency Interview Guide
Supplemental Offer and Acceptance Program Tips
Student Wellness Resources
Maintaining your overall wellness during medical school is critical for your success. Check out our collection of videos, articles and other tools to help you prevent burnout, care for yourself and lead change as you grow your career.
NEW: Managing Perfectionism in Medical Students
This webinar explores strategies to overcome perfectionism, including self-compassion techniques and tools to prioritize personal health.
Managing Perfectionism
Lead Your Family Medicine Interest Group
Make the most of your school's Family Medicine Interest Group (FMIG). Discover new programming ideas, apply for funding, and create a forum for others interested in family medicine.
Discover FMIG Resources
Join the FMIG Network Online Community
Get Free Student Membership
Explore family medicine with a free student membership in the AAFP, and access benefits and resources you can use in medical school.
Ace Your Exams
Master family medicine topics and prep for your family med shelf exam with our board review questions, which are free for AAFP members.
Connect with Your Peers
Join an exclusive community just for medical student members, and explore other online communities organized by topic and interest.