“ESTABLISHED” VS. “NEW” PATIENT CODES
I saw a patient who I thought was established but my billing office says was new because the last visit was more than three years ago. I asked to change my CPT 99214 service (level 4 established patient visit) to 99203 (level 3 new patient visit) but was told that the level of history documented was insufficient to support that code. How should I crosswalk between the codes for established and new patients?
Established patient visits require only two of the three key components (history, examination, and medical decision making) to support the level of service reported. New patient codes, on the other hand, require all three. (See the table below.) For example, your 99214 visit may be supported by a detailed examination and medical decision making of moderate complexity but only an expanded problem-focused history. To support 99203, your documentation must support a detailed history. An expanded problem-focused history would limit your service to 99202 (level 2 new patient visit).
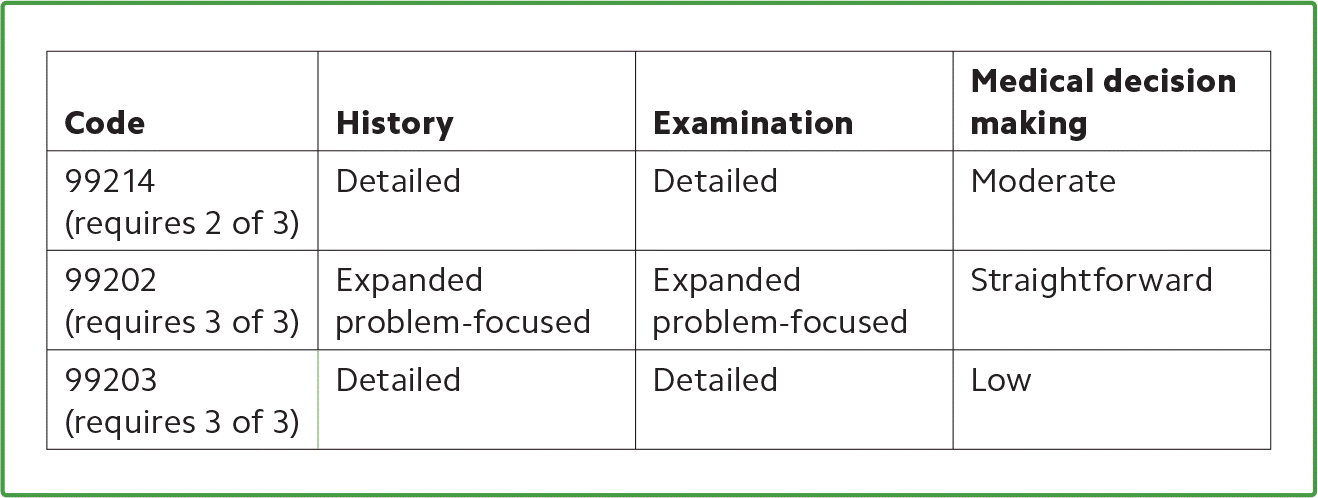
| Code | History | Examination | Medical decision making |
|---|---|---|---|
| 99214 (requires 2 of 3) | Detailed | Detailed | Moderate |
| 99202 (requires 3 of 3) | Expanded problem-focused | Expanded problem-focused | Straightforward |
| 99203 (requires 3 of 3) | Detailed | Detailed | Low |
OFFICE VISITS FOR IMMUNIZATION
Can code 99211, “Office or other outpatient visit for the evaluation and management (E/M) of an established patient that may not require the presence of a physician,” be reported when a patient presents for a flu shot?
Code 99211 is not typically paid in the situation you describe. Payers who use National Correct Coding Initiative (NCCI) edits will deny 99211 if it is billed on the same date as immunization administration (90460–90461 or 90471–90474) even if the nursing assessment (e.g., blood pressure check) is unrelated to the immunization administration and reported with modifier 25. The codes for immunization administration include the clinical staff work of asking about current health and immunization history (e.g., reactions to immunization), providing the vaccine information statement, reviewing benefits and risks of immunization, obtaining informed consent, administering the vaccine/toxoid, and documenting the vaccination in the medical record and immunization registry. Codes 90460–90461 include counseling by the reporting physician or other qualified health care professional (i.e., not clinical staff) regarding the risks and benefits of each component of each vaccine when provided to patients age 18 and younger. You should not report codes 90460–90461 if counseling is limited to supplying the patient with the Vaccine Information Statement.
ADVANCE CARE PLANNING AND TIME
Can I report code 99497 for advance care planning (ACP) when the time of service is 20 minutes rather than the 30 minutes listed in the code descriptor?
Yes, as long as the service was performed as described by CPT, payer regulations, or both. The CPT midpoint rule, which says that “a unit of time is attained when the midpoint is passed,” applies to codes 99497–99498 for Medicare and other payers who follow CPT instruction. You must document the time, and you cannot include any time spent on separately billed services (e.g., time spent to evaluate and manage chronic conditions). Report significant, separately reportable E/M services with modifier 25.If reporting ACP codes on the same date as a Medicare annual wellness visit (G0438 or G0439), be sure to append modifier 33, “Preventive service,” which will avoid out-of-pocket cost to the patient. ACP is an optional element of the Welcome to Medicare physical (G0402), so check your Medicare Part B contractor's payment policy before separately reporting 99497–99498 on the same date as G0402.


