“Virtually every issue [that] relates to drug dependence is suffused with emotion that turns differences of opinion into controversy and leads to distortions, exaggerations, and misunderstandings.”1
This quotation comes from 1971 in the early days of methadone treatment. Policy makers and practitioners were wrestling with a strategy to safely use this effective medication. We are now faced with similar challenges in the use of buprenorphine for opioid use disorder. A buprenorphine-based approach to care is not new and has had international success,2 but its broader implementation in the United States is relatively recent and requires expansion of clinical infrastructure, reimbursement, and patient access. Unlike the HIV/AIDS epidemic, in which primary care and infectious disease subspecialists shared responsibility for treating patients, the current opioid use disorder epidemic relies mostly on the expertise of primary care physicians, who now provide the majority of buprenorphine treatment.3,4 Although many physicians have made substantial efforts to provide care, additional support is needed to increase access to buprenorphine and improve care quality.
Family physicians currently providing buprenorphine treatment have done so largely without clinical infrastructure and reimbursement proportionate to the needs of this complex, vulnerable patient population. In one community sample, patients with opioid use disorder had a mortality rate 10 times higher than the general population.5 This places opioid use disorder among a set of high-risk conditions more similar to cancer or cirrhosis than hypertension or controlled asthma. Primary care for opioid use disorder, however, does not generally have care coordination, peer counseling, and other resources to further allow sustainable quality care. When primary care physicians are asked to better meet the needs of these high-risk patients, they must be given commensurate support through additional reimbursement, education to better understand the chronic nature of addiction, and a team-based approach to treatment.
In addition to this support, health care professionals helping patients with opioid use disorder need ongoing updates of this dynamic field. In this issue of American Family Physician, Drs. Coffa and Snyder address current evidence for care of patients with opioid use disorder.6 In doing so, they provide instruction for the way this treatment can best be achieved. Specifically, they mention crucial areas of updated practice with buprenorphine for opioid use disorder treatment. Four of the article's findings improve on traditional practice. First, home induction of treatment is safe and effective and is often a first-line alternative to office-based induction. Second, the Drug Addiction Treatment Act of 2000 requires that patients can be referred to counseling, not that they actually participate.7 Some patients benefit from dedicated behavioral interventions; however, others need only continued support from their prescribing physician. Third, patients' use of benzodiazepines—licit or illicit— should not obstruct their access to potentially life-saving buprenorphine. And fourth, ongoing, often indefinite, treatment is the standard of care; patients should continue to take buprenorphine as long as they wish and are experiencing benefit.
In a recent publication, we identified these four aspects of care and added three more regarding relapse, the use of toxicology testing, and polysubstance use (Table 1).8 Collectively, these approaches are referred to as low-threshold care.9 Evidence-based and patient-centered low-threshold care uses harm reduction principles that focus on meeting people where they are.10,11 The goal of low-threshold care is to let people more easily come to—and stay in—effective treatment. This is not the historical model of American medicine's care for addiction. We are not far from the days when intentional shaming, confrontation, and ostracization were recognized treatments for substance use disorders.12,13 We need to deliberately question policies and practices in place today and ask ourselves whether they are serving the public well.14 We must continue to refine our care through practice research and epidemiologic findings.
TABLE 1. Buprenorphine Care: Previous Approaches Compared with New Findings and Recommendations
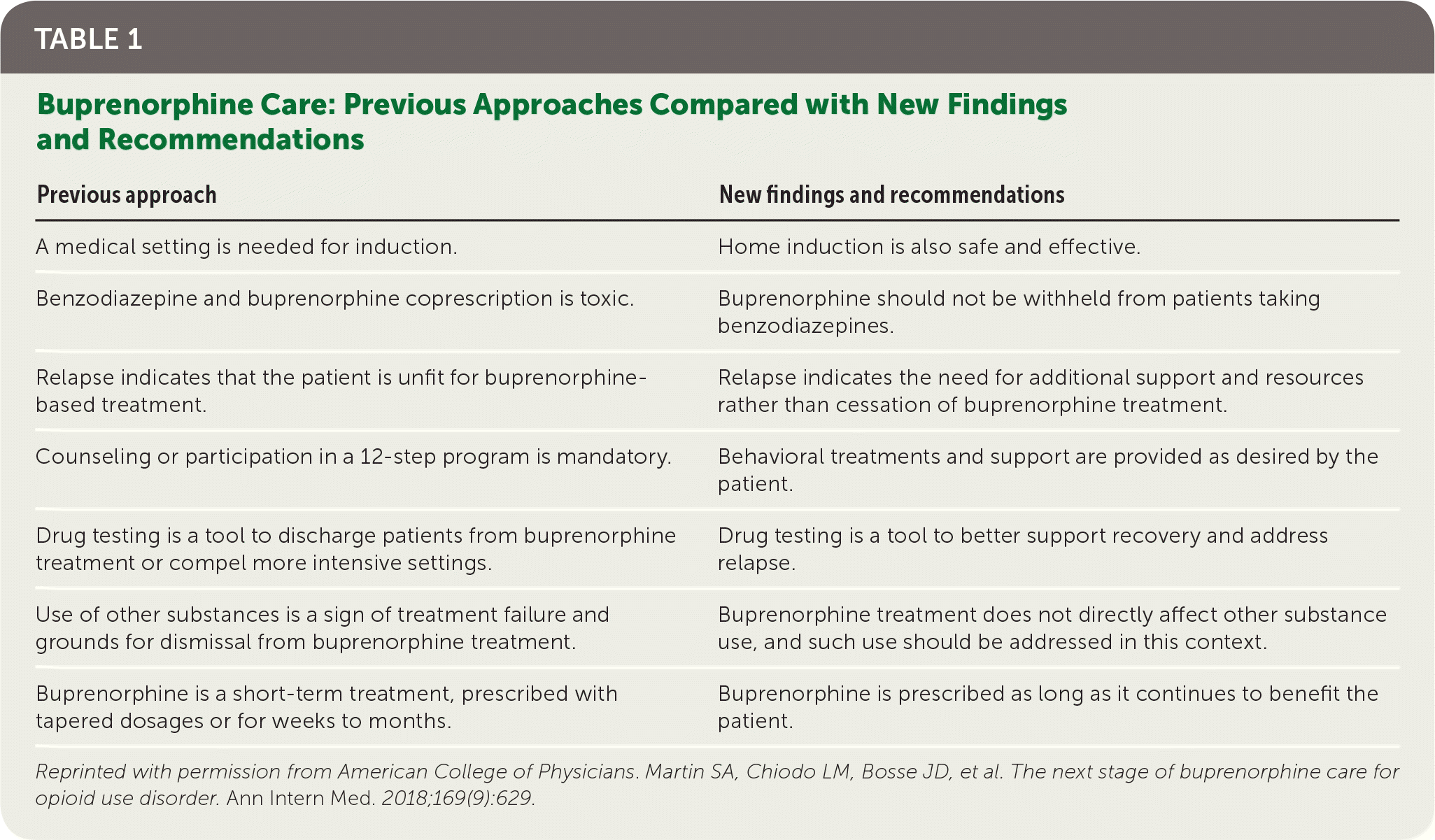
| Previous approach | New findings and recommendations |
|---|---|
| A medical setting is needed for induction. | Home induction is also safe and effective. |
| Benzodiazepine and buprenorphine coprescription is toxic. | Buprenorphine should not be withheld from patients taking benzodiazepines. |
| Relapse indicates that the patient is unfit for buprenorphine-based treatment. | Relapse indicates the need for additional support and resources rather than cessation of buprenorphine treatment. |
| Counseling or participation in a 12-step program is mandatory. | Behavioral treatments and support are provided as desired by the patient. |
| Drug testing is a tool to discharge patients from buprenorphine treatment or compel more intensive settings. | Drug testing is a tool to better support recovery and address relapse. |
| Use of other substances is a sign of treatment failure and grounds for dismissal from buprenorphine treatment. | Buprenorphine treatment does not directly affect other substance use, and such use should be addressed in this context. |
| Buprenorphine is a short-term treatment, prescribed with tapered dosages or for weeks to months. | Buprenorphine is prescribed as long as it continues to benefit the patient. |
Reprinted with permission from American College of Physicians. Martin SA, Chiodo LM, Bosse JD, et al. The next stage of buprenorphine care for opioid use disorder. Ann Intern Med. 2018;169(9):629.
As described in the article by Coffa and Snyder,6 effective treatments for a potentially lethal condition are available. We owe it to patients and others who are affected by this epidemic to find a way forward that avoids potential distortions, exaggerations, and misunderstandings, as quoted previously. The antidote is the thoughtful use of evidence-based medicine and an honest understanding of what we know—and what we don't know—about caring for people with substance use disorders.

