Key Points for Practice
• Adenomas on initial colonoscopy affect ongoing follow-up screening recommendations.
• A single normal colonoscopy demonstrates a lifetime CRC mortality risk 68% lower than in the general population.
• Finding more than 10 adenomas confers the highest risk, and repeat colonoscopy is recommended in one year.
• Finding polyps larger than 10 mm, between five and 10 sessile serrated polyps or adenomas, polyps with dysplasia, or traditional serrated adenomas confers high risk, and repeat colonoscopy is recommended in three years.
From the AFP Editors
Screening colonoscopy findings define the future risk of colorectal cancer (CRC) and the need for repeat screening. The U.S. Multi-Society Task Force on Colorectal Cancer updated recommended follow-up intervals after screening colonoscopy in average-risk individuals. This guidance does not apply to people with hereditary syndromes that increase CRC risk, inflammatory bowel disease, serrated polyposis syndrome, or personal or family history of CRC. Although tobacco use, rural living, metabolic syndrome, obesity, and aspirin use affect CRC risk, they do not influence recommended screening intervals.
Adequate Study
The task force defines an adequate study as a high-quality colonoscopy, which requires bowel preparation sufficient to visualize all polyps larger than 5 mm, examination to the cecum, and complete excision of all polyps found. Physicians who perform high-quality colonoscopies should detect adenomas in more than 30% of men and 20% of women who are screened.
Colonoscopy Findings Determine Risk
Common findings on colonoscopy reports include adenomas and polyps. Instead of defining high- and low-risk findings, task force recommendations depend on the number and size of findings.
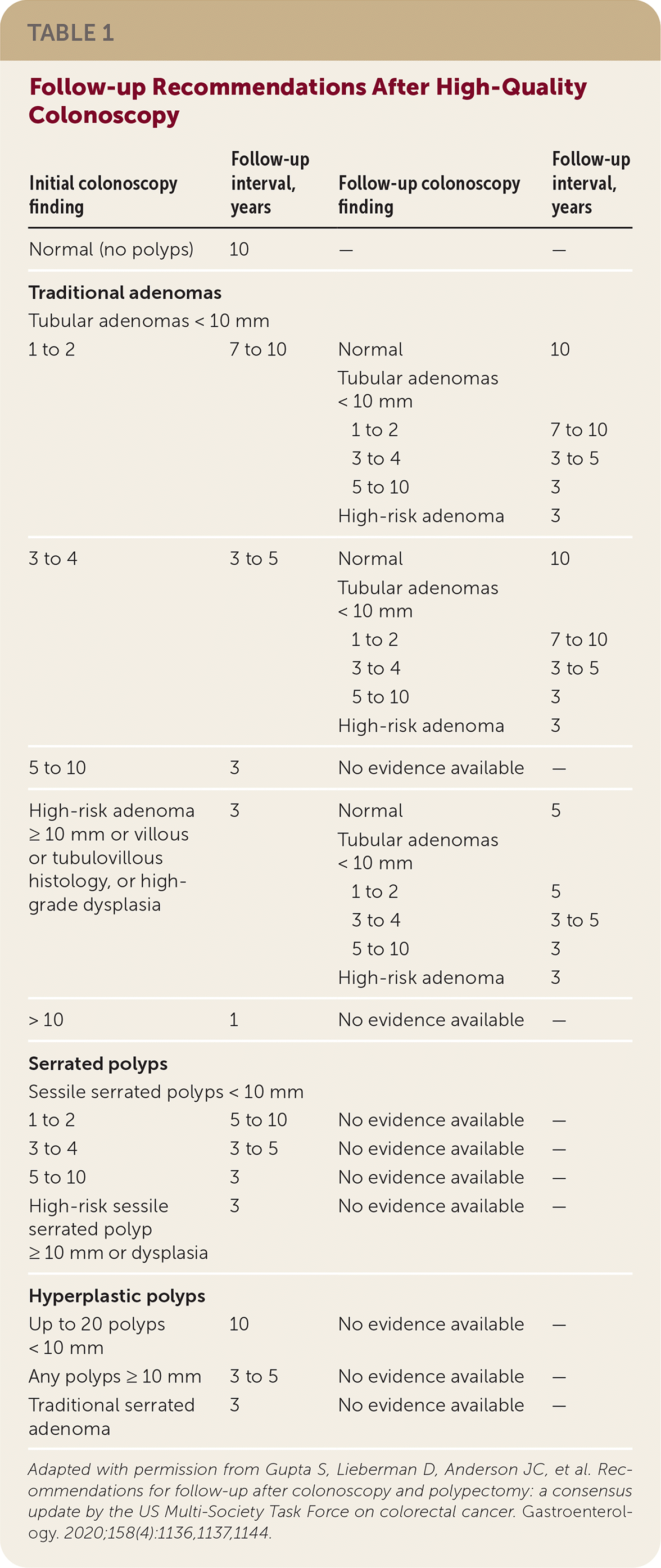
When patients have had more than one colonoscopy, adenomas on initial colonoscopy are the most significant indicator of risk, affecting ongoing follow-up screening recommendations. Recommended intervals for screening based on the current findings may be shortened if a previous colonoscopy showed higher risk. The guideline includes recommendations based on limited evidence for a second follow-up depending on findings of the initial and original follow-up colonoscopies (Table 1).
TABLE 1. Follow-up Recommendations After High-Quality Colonoscopy
| Initial colonoscopy finding | Follow-up interval, years | Follow-up colonoscopy finding | Follow-up interval, years |
|---|---|---|---|
| Normal (no polyps) | 10 | — | — |
| Traditional adenomas | |||
| Tubular adenomas < 10 mm | |||
| 1 to 2 | 7 to 10 | Normal | 10 |
| Tubular adenomas < 10 mm | |||
| 1 to 2 | 7 to 10 | ||
| 3 to 4 | 3 to 5 | ||
| 5 to 10 | 3 | ||
| High-risk adenoma | 3 | ||
| 3 to 4 | 3 to 5 | Normal | 10 |
| Tubular adenomas < 10 mm | |||
| 1 to 2 | 7 to 10 | ||
| 3 to 4 | 3 to 5 | ||
| 5 to 10 | 3 | ||
| High-risk adenoma | 3 | ||
| 5 to 10 | 3 | No evidence available | — |
| High-risk adenoma ≥ 10 mm or villous or tubulovillous histology, or high-grade dysplasia | 3 | Normal | 5 |
| Tubular adenomas < 10 mm | |||
| 1 to 2 | 5 | ||
| 3 to 4 | 3 to 5 | ||
| 5 to 10 | 3 | ||
| High-risk adenoma | 3 | ||
| > 10 | 1 | No evidence available | — |
| Serrated polyps | |||
| Sessile serrated polyps < 10 mm | |||
| 1 to 2 | 5 to 10 | No evidence available | — |
| 3 to 4 | 3 to 5 | No evidence available | — |
| 5 to 10 | 3 | No evidence available | — |
| High-risk sessile serrated polyp ≥ 10 mm or dysplasia | 3 | No evidence available | — |
| Hyperplastic polyps | |||
| Up to 20 polyps < 10 mm | 10 | No evidence available | — |
| Any polyps ≥ 10 mm | 3 to 5 | No evidence available | — |
| Traditional serrated adenoma | 3 | No evidence available | — |
Adapted with permission from Gupta S, Lieberman D, Anderson JC, et al. Recommendations for follow-up after colonoscopy and polypectomy: a consensus update by the US Multi-Society Task Force on colorectal cancer. Gastroenterology. 2020;158(4):1136, 1137, 1144.
Normal Colonoscopy
A normal colonoscopy report can include hyperplastic polyps less than 10 mm in diameter, but no other findings. A single normal colonoscopy denotes a lifetime CRC mortality risk 68% lower than the general population. Although there is no direct evidence of benefit, the group recommends a 10-year follow-up after a normal study.
Tubular Adenomas
Tubular adenomas include all nonserrated lesions. Adenomas that are at least 10 mm in diameter or that have pathology reported as tubulovillous, villous, or high-grade dysplasia are at high risk of neoplasia at follow-up. For these lesions, repeat colonoscopy is recommended at three years. For large adenomas, repeat colonoscopy leads to lower future CRC risk.
Without high-risk findings, recommendations depend on the number of adenomas. For one to two adenomas, a seven- to 10-year follow-up interval is recommended. Recent studies have shown that these patients have CRC risks similar to patients with normal colonoscopy. For three to four adenomas, a three- to five-year follow-up is recommended because studies suggest risk is only slightly higher than with one or two adenomas. For five to 10 adenomas, a three-year follow-up is recommended because of higher neoplasia risk in this population.
When more than 10 adenomas are found, a hereditary polyposis syndrome is likely, and repeat colonoscopy is recommended in one year. In one study, people with this finding had about a 25% risk of developing advanced neoplasia at four years.
Serrated Lesions
Serrated lesions have a similar histologic appearance and are identified as sessile serrated polyps, traditional serrated adenomas, and hyperplastic polyps on pathology reports. The neoplasia risk after finding serrated lesions is not as well defined as the risk with tubular adenomas.
SESSILE SERRATED POLYPS
The neoplasia risk after finding sessile serrated polyps appears to be less than for tubular adenomas. When sessile serrated polyps are at least 10 mm in diameter or have dysplasia, risk appears to be high and a three-year follow-up is recommended. Without these features, follow-up depends on the number of lesions. For one to two polyps, a five- to 10-year follow-up colonoscopy is recommended. This interval is three to five years with three to four sessile serrated polyps and three years with five to 10 polyps.
TRADITIONAL SERRATED ADENOMAS
Traditional serrated adenomas confer a higher neoplasia risk than tubular adenomas, so a three-year follow-up colonoscopy is recommended when they are found.
HYPERPLASTIC POLYPS
Hyperplastic polyps smaller than 10 mm do not increase risk and can be part of a normal colonoscopy. A three- to five-year follow-up colonoscopy is recommended for a hyperplastic polyp 10 mm or larger because any large serrated polyp increases risk of neoplasia. Finding more than 20 hyperplastic polyps suggests a serrated polyposis syndrome, which indicates higher risk requiring individualized follow-up. Fewer than 20 hyperplastic polyps smaller than 10 mm indicates a low risk for neoplasia.
Editor's Note: The U.S. Multi-Society Task Force on Colorectal Cancer includes members from the American Gastroenterological Association, the American College of Gastroenterology, and the American Society for Gastrointestinal Endoscopy. These multisociety guidelines for repeating colonoscopy based on findings contain several changes from previous guidance. Finding more than 10 adenomas demonstrates high risk, so three-year follow-up is recommended. The guidelines suggest follow-up at seven to 10 years instead of five to 10 years after finding only one or two adenomas. These guidelines consider colonoscopy results alone and do not evaluate the role of flexible sigmoidoscopy, fecal immunochemical testing or other stool-based tests, or computed tomography colonography, which are recommended CRC screening strategies by the U.S. Preventive Services Task Force. CRC screening is discussed in previous AFP summaries of the American College of Physicians (https://www.aafp.org/afp/2020/0815/p250.html) and the BMJ (https://www.aafp.org/afp/2020/0815/p253.html) guidelines.—Michael J. Arnold, MD, Contributing Editor
The views expressed are those of the author and do not necessarily reflect the official policy or position of the Department of the Navy, Uniformed Services University of the Health Sciences, Department of Defense, or the U.S. government.
Guideline source: U.S. Multi-Society Task Force on Colorectal Cancer
Evidence rating system used? Yes
Systematic literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Recommendations based on patient-oriented outcomes? Yes
Published source: Gastroenterology. March 2020;158(4):1131–1153.e5

