Pharmacologic management of acute pain should be tailored for each patient, including a review of treatment expectations and a plan for the time course of prescriptions. Acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs) are first-line treatment options for most patients with acute mild to moderate pain. Topical NSAIDs are recommended for non–low back, musculoskeletal injuries. Acetaminophen is well tolerated; however, lower doses should be used in patients with advanced hepatic disease, malnutrition, or severe alcohol use disorder. Nonselective NSAIDs are effective but should be used with caution in patients with a history of gastrointestinal bleeding, cardiovascular disease, or chronic renal disease. Selective cyclooxygenase-2 NSAIDs are a more expensive treatment alternative and are used to avoid the gastrointestinal adverse effects of nonselective NSAIDs. Adjunctive medications may be added as appropriate for specific conditions if the recommended dose and schedule of first-line agents are inadequate (e.g., muscle relaxants may be useful for acute low back pain). For severe or refractory acute pain, treatment can be briefly escalated with the use of medications that work on opioid and monoamine receptors (e.g., tramadol, tapentadol) or with the use of acetaminophen/opioid or NSAID/opioid combinations. The opioid epidemic has increased physician and community awareness of the harms of opioid medications; however, severe acute pain may necessitate short-term use of opioids with attention to minimizing risk, including in patients on medication-assisted therapy for opioid use disorder.
Acute pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage. Acute pain lasts from a few days up to 12 weeks and is typically prompted by a specific event and caused by direct tissue damage that is likely to resolve. A person's perception of pain is controlled by biophysical factors, including sensory, emotional, cognitive, and social components.1 Pharmacologic management of acute pain should be tailored for each patient, and effective management may prevent the transition to chronic pain.2
SORT: KEY RECOMMENDATIONS FOR PRACTICE
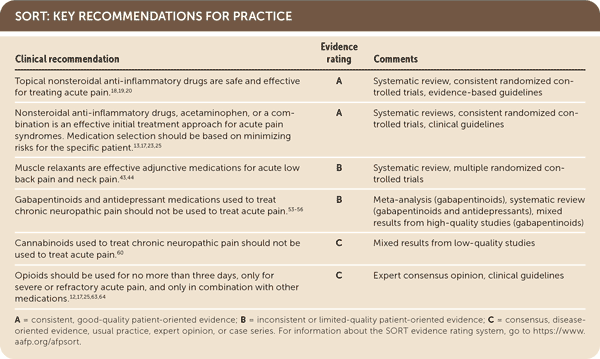
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
This article provides a tiered pharmacologic approach for safe and effective management of acute pain in ambulatory and inpatient settings (Table 13 ). Most data are derived from studies of acute musculoskeletal pain and postoperative pain. Nonpharmacologic management of acute pain, such as nerve blocks,4,5 acupuncture,6 transcutaneous electrical nerve stimulation,7 mindfulness,8 and massage,9 is reviewed elsewhere.
TABLE 1. Common Analgesic Medications for the Treatment of Acute Pain
| Medication/dosing | Pain level | Best use | Risk | Comments | Cost* |
|---|---|---|---|---|---|
| Acetaminophen | |||||
| Orally or rectally: 325 to 1,000 mg every 4 to 6 hours IV: ≥ 50 kg, 650 mg every 4 hours or 1,000 mg every 6 hours; < 50 kg, 12.5 mg per kg every 4 hours or 15 mg per kg every 6 hours Maximum: 75 mg per kg per day, not to exceed 4,000 mg per day | Mild to moderate | Mild osteoarthritis Generalized headache Ankle sprain | Hepatotoxicity | Well tolerated First-line treatment in patients with renal and hepatic impairment and cardiovascular disease ≤ 2,000 mg per day in patients with advanced hepatic disease and severe alcohol use disorder May be combined with NSAIDs for postoperative pain | Tablet: $3 ($5) Suppository: — ($12) IV: NA |
| Nonselective NSAIDs | |||||
| Ibuprofen: 200 to 400 mg every 6 to 8 hours Maximum: 1,200 mg per day | Mild to moderate | Migraine Low back pain Dysmenorrhea Renal colic Postoperative pain | Cardiovascular Gastrointestinal Renovascular Bronchospasm (aspirin) | Anti-inflammatory effects Consider adding proton pump inhibitor or switching to a selective COX-2 NSAID to decrease gastrointestinal risk May have a ceiling analgesic effect | $5 ($10) |
| Naproxen: 250 mg every 6 to 8 hours or 500 mg every 12 hours Maximum: 1,000 mg per day | $10 ($200) | ||||
| Diclofenac: 50 mg every 8 hours Maximum: 150 mg per day | $10 ($750) | ||||
| Ketorolac Orally: 10 mg every 4 to 6 hours IM: 30 to 60 mg as a single dose or 15 to 30 mg every 6 hours IV: 10 to 15 mg every 6 hours Maximum: oral 40 mg per day; IM/IV 120 mg per day | Tablets: $20 (—) Syringes: $15 (NA) | ||||
| Meloxicam: 7.5 to 15 mg per day Maximum: 15 mg per day | $10 ($500) | ||||
| Selective COX-2 NSAIDs | |||||
| Meloxicam: 7.5 mg per day | Mild to moderate | Migraine Low back pain Dysmenorrhea Renal colic Postoperative pain | Cardiovascular Renovascular | More expensive than nonselective NSAIDs Celecoxib has a U.S. Food and Drug Administration boxed warning for increased risk of cardiovascular disease | $10 ($300) |
| Celecoxib (Celebrex): 100 to 200 mg per day | $20 ($225) | ||||
| Acetaminophen plus NSAID combinations | |||||
| See individual medications | Mild to moderate May continue use for severe pain | Pain refractory to either agent alone Postoperative pain | See individual medications | Combinations have superior effectiveness vs. single agents Effective for postoperative pain Combining medications has lower risk of adverse effects than high doses of single agents | See individual medications |
| Opioid plus acetaminophen or NSAID combinations | |||||
| Hydrocodone/acetaminophen: 2.5 mg/325 mg to 10 mg/325 mg every 4 to 6 hours Maximum: 4,000 mg per day of acetaminophen | Persistent moderate to severe pain | Pain refractory to other agents Postoperative pain Fracture pain | See individual medications | Superior effectiveness compared with single agent Opioid sparing effect with decreased risk of adverse events | $25 ($150) |
| Hydrocodone/ibuprofen: 2.5 mg/200 mg to 10 mg/ 200 mg every 6 to 8 hours Maximum: 1,200 mg per day of ibuprofen | $40 ($50) | ||||
| Oxycodone/acetaminophen 2.5 mg/325 mg to 10 mg/ 325 mg every 4 to 6 hours Maximum: 4,000 mg per day of acetaminophen | $25 ($800) | ||||
| Dual-action opioid medications | |||||
| Tramadol (Ultram): 25 mg every 4 to 6 hours, titrated to 50 to 100 mg as needed Maximum: 400 mg per day | Persistent moderate to severe pain | Pain refractory to other agents, with goal of limiting more potent opioids | Dizziness, sedation, constipation Opioid use disorder Serotonin syndrome Tramadol decreases the seizure threshold | Adverse effects comparable to full agonists with less pain relief | $10 ($110) |
| Tapentadol (Nucynta): 50 to 100 mg every 4 to 6 hours Maximum: 600 mg per day | — ($215) | ||||
| Full agonist opioids | |||||
| Oxycodone: 5 mg orally every 4 to 6 hours as needed | Persistent severe pain | Short course for severe acute pain Pain refractory to other medications | Nausea, emesis Constipation Sedation Respiratory depression Opioid use disorder | Limit prescription to 3-day course Continue other medication classes as tolerated Higher doses may be required for patients taking chronic opioid therapy or naltrexone (Revia) | $10 ($60) |
| Morphine: 1 to 4 mg IV every 4 hours titrated up as needed; 10 to 15 mg IV every 4 to 6 hours for severe pain Maximum: limited by opioid-related adverse effects | NA | ||||
| Hydromorphone (Dilaudid) Orally: 2 to 4 mg every 4 to 6 hours IV: 0.2 to 1 mg every 2 to 3 hours Maximum: reserve for severe pain; use caution with dosing to prevent oversedation | Tablets: $10 ($125) IV: NA | ||||
COX = cyclooxygenase; IM = intramuscularly; IV = intravenously; NA = cost not available; NSAID = nonsteroidal anti-inflammatory drug.
*—Estimated lowest GoodRx price. Actual cost will vary with insurance and by region. Generic price listed first; brand name price in parentheses. Information obtained at https://goodrx.com (accessed October 27, 2020; zip code: 66211).
Information from reference 3.
Racial and ethnic inequities exist in the management of acute pain. Patients from minority groups are more likely to have their pain underestimated and undertreated compared with White patients.10 African American and Hispanic patients are less likely to receive opioid analgesics despite pain severity.10 African Americans experience both a higher number and magnitude of disparities in pain management than any other group.11 Family physicians should apply the goals and principles of acute pain management to all patients to avoid continued harm to these marginalized groups.
A more detailed discussion of pain management in specific populations, including children and pregnant patients, is beyond the scope of this article. Evidence for specific pain syndromes is highlighted in this article when available.
Goals and Principles
The goal of treating acute pain is to decrease suffering, improve function, and minimize adverse effects. Management should include a review of treatment expectations and a plan for the time course of prescriptions. Treatment of acute pain should include addressing the cause of the pain when appropriate, such as immobilizing a fracture or draining an abscess. The World Health Organization's pain relief ladder provides a framework that was developed to address the need for effective management of cancer-related pain and encourage prompt initiation and appropriate escalation of scheduled opioids for pain that is not relieved with nonopioid medications.12 The use of the pain relief ladder in guiding treatment of acute pain has been called into question.13
Because of the increased recognition of the harm caused by the use of opioids, newer guidelines recommend that opioids be reserved for severe or refractory pain.14,15 Regular reassessments of opioid therapy allow for the addition or discontinuation of pharmacologic and nonpharmacologic treatments as indicated, with a goal of tapering off all medications as quickly as possible.
Combinations of medications may provide maximal benefit and decrease dosage requirements of individual agents. An overview of Cochrane reviews showed that ibuprofen, 200 mg, alone has a number needed to treat (NNT) of 3 to achieve a 50% reduction in pain, whereas the same dose of ibuprofen combined with acetaminophen, 500 mg, has an NNT of 1.6. The NNT of acetaminophen, 1,000 mg, plus ibuprofen, 400 mg, is only marginally better at 1.5.16 The rates of adverse events are sometimes lower when using combination treatments and are low for short-term analgesics. An additional overview of Cochrane reviews reported that the relative risk of any adverse event from a single dose of ibuprofen, 200 mg, is 0.9 (95% CI, 0.7 to 1.02). For the combination of ibuprofen, 200 mg, and acetaminophen, 500 mg, the relative risk is 0.7 (95% CI, 0.6 to 0.9).17
Topical Analgesics
Topical nonsteroidal anti-inflammatory drugs (NSAIDs) locally inhibit cyclooxygenase (COX) receptors when absorbed through the skin.18 Topical NSAIDs can be rubbed directly on unbroken skin or applied via a transdermal patch and are effective for acute musculoskeletal strains and sprains.18,19 Topical NSAIDs provide up to 50% pain relief compared with placebo. Diclofenac gel has shown superiority among topical NSAIDs (NNT = 2). The rates of systemic or local adverse events with topical NSAIDs are similar to topical placebo (4.3% and 4.6%, respectively) in the treatment of acute pain.18 Systemic absorption is 1% to 7% across all topical NSAIDs at recommended dosages.18 There is no evidence regarding the rates of adverse cardiovascular events and renal disease when used in the short term. Topical NSAIDs have a low risk of gastrointestinal (GI) bleeding, even with long-term use; however, patients at high risk should be cautious. Guidelines from the American College of Physicians and the American Academy of Family Physicians recommend topical NSAIDs as first-line therapy for acute non–low back, musculoskeletal pain.14
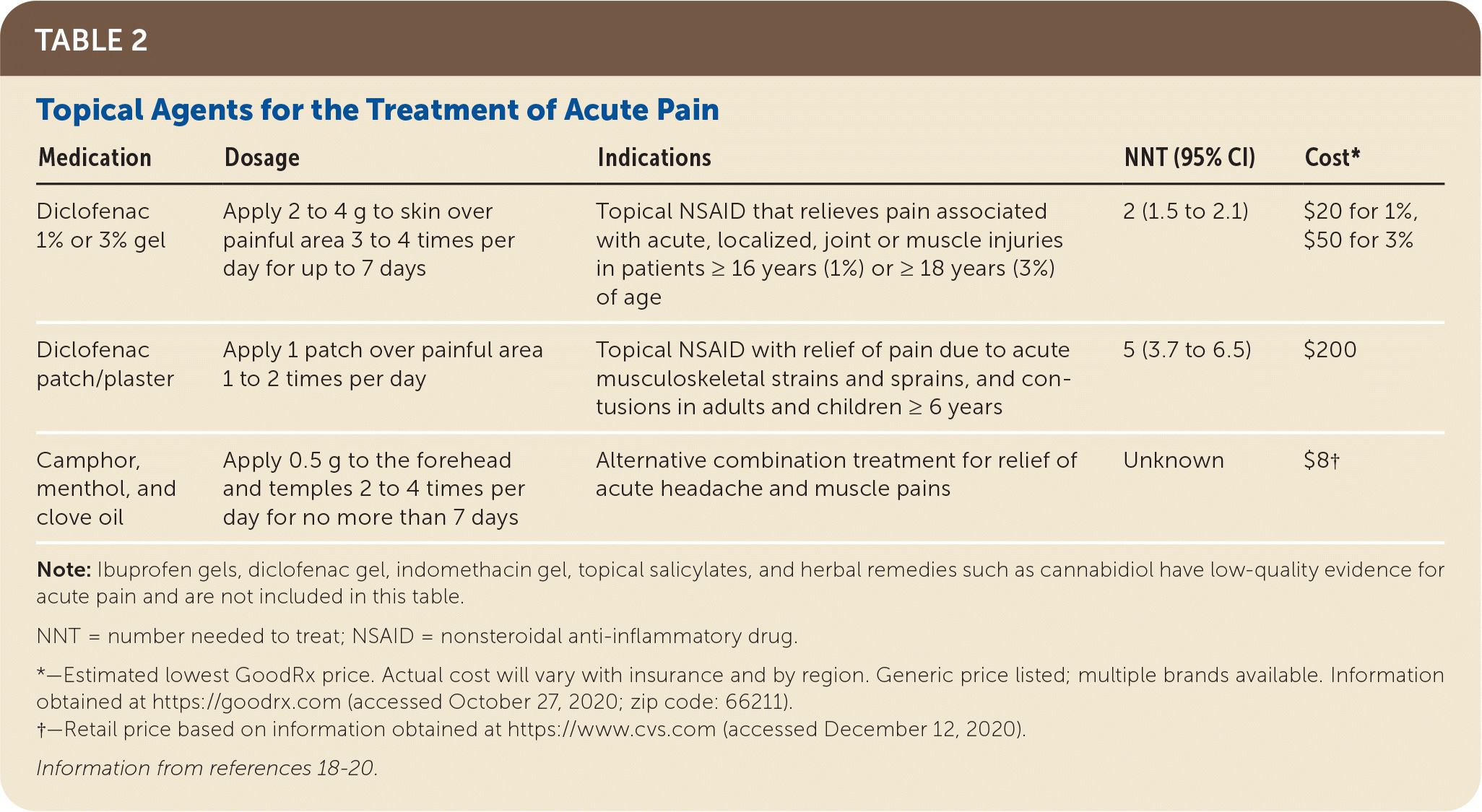
A small randomized controlled trial demonstrated that camphor, menthol, and clove oil applied to the temples can relieve tension headaches comparably to acetaminophen, 1,000 mg, with a moderate risk of adverse skin and allergic reactions.20 There is limited evidence for the use of other topical products, such as capsaicin and lidocaine, for pain relief.19 Table 2 summarizes topical medications for the treatment of acute pain.18–20
TABLE 2. Topical Agents for the Treatment of Acute Pain
| Medication | Dosage | Indications | NNT (95% CI) | Cost* |
|---|---|---|---|---|
| Diclofenac 1% or 3% gel | Apply 2 to 4 g to skin over painful area 3 to 4 times per day for up to 7 days | Topical NSAID that relieves pain associated with acute, localized, joint or muscle injuries in patients ≥ 16 years (1%) or ≥ 18 years (3%) of age | 2 (1.5 to 2.1) | $20 for 1%, $50 for 3% |
| Diclofenac patch/plaster | Apply 1 patch over painful area 1 to 2 times per day | Topical NSAID with relief of pain due to acute musculoskeletal strains and sprains, and contusions in adults and children ≥ 6 years | 5 (3.7 to 6.5) | $200 |
| Camphor, menthol, and clove oil | Apply 0.5 g to the forehead and temples 2 to 4 times per day for no more than 7 days | Alternative combination treatment for relief of acute headache and muscle pains | Unknown | $8† |
Note: Ibuprofen gels, diclofenac gel, indomethacin gel, topical salicylates, and herbal remedies such as cannabidiol have low-quality evidence for acute pain and are not included in this table.
NNT = number needed to treat; NSAID = nonsteroidal anti-inflammatory drug.
*—Estimated lowest GoodRx price. Actual cost will vary with insurance and by region. Generic price listed; multiple brands available. Information obtained at https://goodrx.com (accessed October 27, 2020; zip code: 66211).
†—Retail price based on information obtained at https://www.cvs.com (accessed December 12, 2020).
Oral NSAIDs
Oral NSAIDs inhibit COX enzymes, impairing the conversion of arachidonic acid to prostaglandins and other inflammatory mediators.16 Although systematic reviews have shown that NSAIDs are more effective than acetaminophen for acute pain,21 guidelines suggest that both can improve pain and that NSAIDs are better for functional improvement.14 NSAIDs, acetaminophen, or a combination is an effective initial treatment approach for acute pain syndromes. Medication selection should be based on minimizing risks for the specific patient.3,14,17,22
NSAIDs provide superior pain relief from inflammatory conditions, such as gout flare-ups, renal colic, dysmenorrhea, and postoperative pain, but carry more risks than acetaminophen.17,21 NSAIDs are also preferred over acetaminophen for acute low back pain and migraines.21,23 Low to standard doses of NSAIDs may be considered for short-term treatment of acute pain related to fractures, fracture repair, or other acute musculoskeletal injuries when the risk of bleeding is not significant; however, more studies are needed.24,25 In addition to providing analgesia and improving function, NSAIDs may decrease or eliminate the need for opioids, including for surgical dental pain and kidney stones.14,24,25 Pain relief with NSAIDs is comparable to opioids, particularly when combined with acetaminophen and nonpharmacologic therapies.3,14
There are many NSAIDs with similar clinical properties. Medication choice depends on cost, availability, dosing schedule, and adverse effect profile. Nonselective NSAIDs, such as ibuprofen, naproxen, and diclofenac, inhibit COX-1 and COX-2 enzymes. COX-1 enzymes are present in many organs but specifically play a role in GI protection and platelet aggregation.26 COX-2 enzymes are mainly involved in the inflammatory response.26
Because of COX-1 inhibition, nonselective NSAIDs may cause GI adverse effects, such as dyspepsia, ulcerative disease, and bleeding, especially in older patients and with larger doses or prolonged use.27 Among commonly used NSAIDs, ibuprofen has a lower risk of upper GI complications.27 The GI risk of nonselective NSAIDs can be mitigated by coprescribing a proton pump inhibitor; however, this adds cost and contributes to polypharmacy.28 Nonselective NSAIDs are less expensive and are typically available without a prescription.
Selective COX-2 inhibitors (e.g., celecoxib [Celebrex]) have a significantly safer GI adverse effect profile but may be cost prohibitive. Relatively selective COX-2 inhibitors (e.g., meloxicam, nabumetone) inhibit the activity of COX-2 enzymes at low doses (e.g., meloxicam, 7.5 mg) but are less selective at higher doses (e.g., meloxicam, 15 mg). Relatively selective COX-2 inhibitors have a similar GI adverse effect profile to selective COX-2 inhibitors but cost less and are dosed once per day.26,27
NSAIDs increase the risk of cardiovascular events, including myocardial infarction, stroke, and death, by about 30%.29,30 Even short-term NSAID use is cautioned in patients with a high baseline risk of cardiovascular disease; however, selecting an NSAID associated with a lower cardiovascular risk (e.g., naproxen) may be considered.30 Selective COX-2 inhibitors carry a U.S. Food and Drug Administration boxed warning because of a higher incidence of thrombotic cardiovascular events; the risk is dose-dependent.31 NSAIDs may also cause acute kidney injury as a result of reduced renal blood flow.29,32,33 The use of NSAIDs is cautioned in patients with chronic renal disease, older age, or volume-depleted states.
NSAIDs deliver dose-dependent anti-inflammatory effects, which may prompt the use of higher daily dosages (e.g., 3,200 mg of ibuprofen) when treating conditions such as rheumatoid arthritis; however, there is a ceiling analgesic effect.29 When used for acute pain, lower daily dosages should be used (e.g., 1,200 mg of ibuprofen); higher dosages increase the risk of adverse effects. Over-the-counter medications are appropriately labeled to treat acute pain while avoiding NSAID-related harm.
Aspirin irreversibly inhibits COX-1 and COX-2 enzymes in a dose-dependent manner. A low daily dosage of aspirin (75 mg to 81 mg) inhibits COX-1–dependent platelet function, producing its antithrombotic effect. At higher daily dosages (approximately 1,000 mg), aspirin inhibits COX-1 and COX-2 enzymes, resulting in anti-inflammatory and analgesic effects.34 Aspirin increases the risk of bronchospasm in patients with asthma.35
Acetaminophen
Acetaminophen is well tolerated and is the most widely used medication for pain. The exact mechanism of action is unknown, but it likely affects the serotonergic system and other pain pathways.36 Acetaminophen possesses analgesic and antipyretic properties but lacks the anti-inflammatory properties of NSAIDs. Although acetaminophen is often the safest medication for treating acute pain, caution is necessary. Unintentional acetaminophen overdose is the leading cause of acute liver failure in the United States, often attributed to accidental supratherapeutic use.37 In one study, 38% of patients admitted to tertiary care centers with unintentional overdoses took two or more acetaminophen preparations simultaneously, and 63% used compounds that also contained opioids.37 In many patients, using more than the maximum daily dosage of acetaminophen (3,000 mg) may cause significant elevations in alanine transaminase levels (i.e., greater than three times the upper limit of normal).38
Patients with severe alcohol use disorder, malnutrition, or advanced hepatic disease may use acetaminophen but at daily dosages of 2,000 mg or lower. Acetaminophen is still preferable to NSAIDs in this setting because NSAIDs may cause more serious complications, such as mucosal bleeding, diuretic-resistant ascites, or hepatorenal syndrome in patients who are at risk.39
Intravenous acetaminophen offers no advantage in pain control compared with oral formulations. It should be reserved for patients unable to take medication orally or rectally, such as in the postoperative setting.40
Adjunctive Medications
Adjunctive medications are a broad category of medications that do not primarily treat pain but can augment analgesics.
Nonbenzodiazepine muscle relaxants demonstrate effectiveness for acute low back pain and neck pain.41–44 No single agent is superior; therefore, treatment decisions can be made based on the dosing schedule and patient preference.43 Sedation is a common adverse effect that can be mitigated by reducing the dose or limiting administration to the evening. Muscle relaxants are not recommended for older adults.
Caffeine, an adenosine receptor antagonist, is an effective adjunctive medication for several pain syndromes, including tension headaches, migraines, and postoperative pain, with an NNT of 14 at a dose equivalent to one cup of coffee.45,46
Intravenous ketamine (Ketalar), a phencyclidine analogue and dissociative anesthetic agent that is used in subanesthetic doses for acute pain, has some evidence of benefit when used with opioids.47 Intravenous ketamine has been used as an adjunctive and stand-alone agent for perioperative pain in patients who are opioid tolerant or at high risk of respiratory depression.48,49 Intranasal ketamine has been used to treat acute pain in the emergency department,50,51 but larger studies are needed before routine use can be recommended.
There is no convincing evidence that antiepileptics have a role in the treatment of acute neuropathic pain or the prevention of chronic pain.52 The use of gabapentinoids has been studied as a strategy to decrease the use of opioids in the perioperative period with mixed results.53–55 Although national guidelines recommend gabapentinoids as part of a multimodal treatment plan for patients undergoing major surgeries,56 concerns about sedation and addiction limit their use.57
Medical-grade cannabis is effective for the treatment of chronic pain58,59; however, neither marijuana nor cannabidiol has evidence of benefit for acute pain.60,61
Other proposed adjunctive medications with low evidence of benefit for the management of acute pain include benzodiazepines, corticosteroids, and antidepressants.41,62,63
Opioids
Opioids activate mu opioid receptors in the central nervous system and are potent analgesics.64 Up to 6.5% of patients who are opioid-naive and prescribed opioids for surgery are still taking opioids one year later, and 0.6% of patients prescribed an opioid medication will develop an opioid use disorder.65 Unused opioids prescribed for acute pain may be diverted for recreational use by others, contributing to the opioid crisis.65,66
Opioids are effective for acute pain but carry substantial risks, such as neurologic and GI adverse effects. The American College of Physicians/American Academy of Family Physicians guidelines recommend against the use of opioids for acute musculoskeletal conditions except in severe or refractory cases.14,67 When opioids are indicated, a prescription drug monitoring program (https://www.cdc.gov/drugoverdose/pdmp/states.html) should be checked before prescribing to identify patients who may have an opioid use disorder or who are engaged in diversion.64 All patients should be educated on the risks and goals of therapy, as well as the safe storage and disposal of opioids.12,64
Patients with severe or refractory acute pain who receive opioids should continue first-line medications and use the lowest effective dose of opioids for the shortest duration possible.12 Studies have shown that hydrocodone, 5 mg, is as effective as oxycodone, 5 mg, and oral oxycodone is as effective as intravenous morphine for acute musculoskeletal injuries.68,69 Patients should be provided no more than three days of opioids. Authorizing more than one week of opioid medications or providing a prescription refill is associated with two times the risk of continuing to need opioids one year later.65 Long-acting opioids are not indicated for opioid-naive patients with acute pain.64 Opioid combinations with NSAIDs or acetaminophen are superior to any agent alone.70,71
Patients receiving chronic opioid therapy for pain or opioid use disorder, including buprenorphine and methadone, should continue their current medication with adjunctive nonopioid pain medications.72,73 Buprenorphine and methadone can be dosed every eight hours if needed for pain control.72,74 Short-acting opioids can be added if required.
For patients taking naltrexone (Revia), nonopioid treatment such as ketamine or regional blocks should be attempted before opioids because very high-dose opioids may be required to overcome naltrexone's opioid blockade, especially in patients receiving the long-acting injectable formulation and in patients who decide not to taper because of concerns of relapse.74
Dual-Action Medications
Dual-action medications, such as tapentadol (Nucynta) and tramadol, are weak opioids that also target norepinephrine and/or serotonin pathways. Dual-action medications have been studied mostly in cancer-related or chronic pain but may be useful in acute pain when first-line agents are not effective, tolerated, or safe. They carry the same risks as full agonist opioids (e.g., constipation, sedation, addiction) but are less potent analgesics.75–77
Caution must be used when coprescribing serotonergic agents because of the risk of serotonin syndrome. Tramadol lowers the seizure threshold and may be prescribed in combination with acetaminophen or as an extended-release formulation.75,78 Cost often limits the use of tapentadol.76
This article updates a previous article on this topic by Blondell, et al.79
Data Sources: A PubMed search was completed in Clinical Queries using the key terms pain, acute pain, postoperative pain, musculoskeletal pain, headache, pain pregnancy, acetaminophen, NSAIDs, ketamine, caffeine, gabapentinoids, cannabinoids, buprenorphine, and topical analgesics. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality, Clinical Evidence, the Cochrane database, Essential Evidence Plus, and the National Guideline Clearing-house database. Search dates: February 4, 2020, to August 1, 2020.

