Splenomegaly can be due to several mechanisms but is almost always a sign of a systemic condition. Patient habits, travel, and medical conditions can increase risk of splenomegaly and suggest etiology. Symptoms can suggest infectious, malignant, hepatic, or hematologic causes. Physical examination will typically reveal splenomegaly, but abdominal ultrasonography is recommended for confirmation. Physical examination should also assess for signs of systemic illness, liver disease, and anemia or other hematologic issues. The most common causes of splenomegaly in the United States are liver disease, malignancy, and infection. Except for apparent causes such as infectious mononucleosis, basic laboratory analysis and ultrasonography are the first-line steps in determining etiology. Malaria and schistosomiasis are common in tropical regions, where as many as 80% of people may have splenomegaly. Management of splenomegaly involves treating the underlying disease process. Splenectomies and spleen reduction therapies are sometimes performed. Any patient with limited splenic function requires increased vaccination and prophylactic antibiotics for procedures involving the respiratory tract. Acute infections, anemia, and splenic rupture are the most common complications of splenomegaly, and people with splenomegaly should refrain from participating in contact sports to decrease risk of rupture.
The spleen is part of the hepatoportal system and is the largest organ of the lymphatic system. Functions of the spleen include removing aging or abnormal blood cells, storing platelets and red blood cells, and producing and distributing immune cells and antibodies.1 The spleen is a major site of blood production outside of the bone marrow, especially during times of stress.1–3 Several general pathophysiologic mechanisms cause splenic enlargement. Hyperplasia and hypertrophy cause splenomegaly due to increased function of the spleen. Infiltrative processes can cause accumulation of abnormal cells in the spleen, which can be malignant, benign, or caused by glycogen storage disorders. Congestive processes result in blood pooling due to blockage of venous outflow.2,3 These mechanisms can lead to transient splenomegaly, such as with blood loss, infection, and during pregnancy, but in these cases the spleen returns to normal size after the condition resolves.2,4
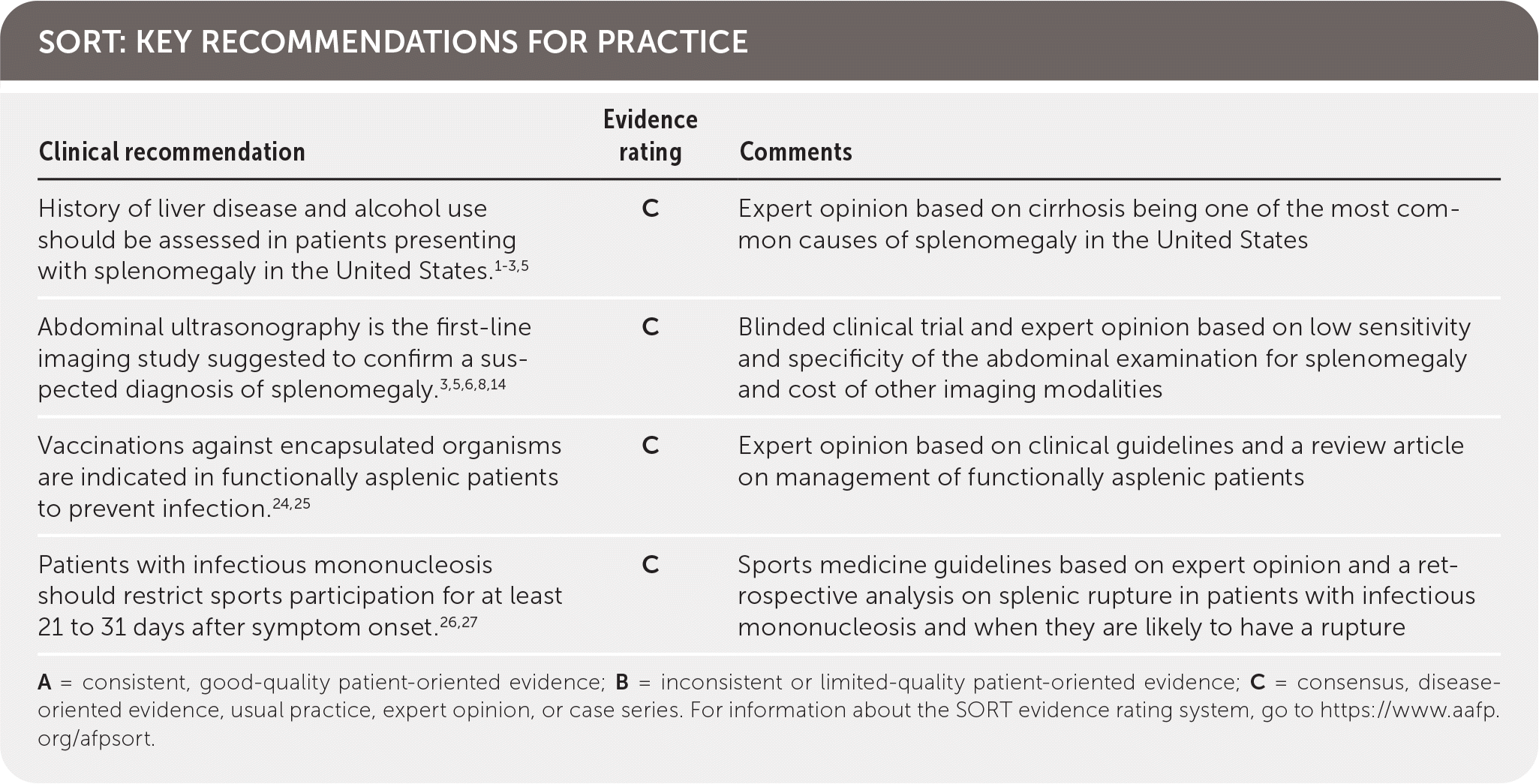
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| History of liver disease and alcohol use should be assessed in patients presenting with splenomegaly in the United States.1–3,5 | C | Expert opinion based on cirrhosis being one of the most common causes of splenomegaly in the United States |
| Abdominal ultrasonography is the first-line imaging study suggested to confirm a suspected diagnosis of splenomegaly.3,5,6,8,14 | C | Blinded clinical trial and expert opinion based on low sensitivity and specificity of the abdominal examination for splenomegaly and cost of other imaging modalities |
| Vaccinations against encapsulated organisms are indicated in functionally asplenic patients to prevent infection.24,25 | C | Expert opinion based on clinical guidelines and a review article on management of functionally asplenic patients |
| Patients with infectious mononucleosis should restrict sports participation for at least 21 to 31 days after symptom onset.26,27 | C | Sports medicine guidelines based on expert opinion and a retrospective analysis on splenic rupture in patients with infectious mononucleosis and when they are likely to have a rupture |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
In the United States, the most common etiologies of splenomegaly are chronic liver disease, malignancies, and infections.3 Malignancies—usually leukemia or lymphoma—are common causes of splenomegaly, seen in close to one-third of affected patients.3 As many as one-third of patients with splenomegaly have cirrhosis, where abnormal liver parenchyma leads to congestive splenomegaly.3,5 Several infections can lead to splenomegaly. In the United States, infectious mononucleosis is a common etiology of splenomegaly in adolescents and young adults.3 Splenomegaly is common in patients with HIV, as a response to the virus or because of secondary infections.6 People who are born in tropical regions, global travelers, and military personnel deployed to tropical regions are at risk for parasitic infections that can lead to splenomegaly, most commonly schistosomiasis and chronic malaria.7 Common disorders associated with splenomegaly are shown in Table 1.2,3
TABLE 1. Causes of Splenomegaly

| Type* | Conditions |
|---|---|
| Congestive | Any pathologic process that can cause advanced liver disease, congestive heart failure, portal hypertension, renal failure, splenic vein thrombosis |
| Neoplastic | Essential thrombocytopenia, Hodgkin/non-Hodgkin lymphoma, leukemia (acute lymphoid leukemia, acute myeloid leukemia, chronic lymphoid leukemia, chronic myeloid leukemia, hairy cell), metastatic disease, multiple myeloma, myelofibrosis, polycythemia vera, primary splenic tumors |
| Infectious | Babesiosis; Bartonella; Candida; endocarditis; hepatitis A, B, and C viruses; HIV; mononucleosis (Epstein-Barr virus, cytomegalovirus); splenic abscess; syphilis; tuberculosis |
| Tropical/parasitic considerations | Actinomycosis, brucellosis, leishmaniasis (visceral), malaria, schistosomiasis, typhoid |
| Autoimmune/inflammatory | Collagen vascular disease, hemolytic anemia, immune thrombocytopenia, pernicious anemia, rheumatoid arthritis (Felty syndrome), systemic lupus erythematosus, thyrotoxicosis |
| Hematologic (nonmalignant) | Beta thalassemia major,† sickle cell anemia† |
| Infiltrative (nonmalignant, noninfectious) | Amyloidosis, glycogen storage disorders, sarcoidosis |
*—Listed in order of prevalence.
†—More common in children.
Splenomegaly is a common finding in college freshman in North America, with rates of up to 3%, because of the high prevalence of infectious mononucleosis.3 Splenomegaly can affect up to 80% of people in tropical areas where malaria and schistosomiasis are endemic.7 People who have recently immigrated from overseas, children who are adopted from endemic areas, refugees, and travelers with splenomegaly often have chronic parasitic infections.7
Pertinent History
Personal and family history can suggest the etiology of splenomegaly (Table 23,8–17 ). Early satiety and fullness in the left upper quadrant can be due to an enlarged spleen.2,8 Family history of malignancies, liver disease, lipid storage disorders, or hematologic diseases can suggest an etiology for splenomegaly.2,8 Personal history may contain risk factors for splenomegaly, including alcohol consumption, intravenous drug use, and high-risk sexual behavior. Immigration from or travel to tropical areas increases the risk of infectious diseases such as malaria or schistosomiasis. Medical history of cancer, hematologic disorders, heart failure, or chronic liver disease increases the chance of splenomegaly (Table 12,3 ). Recent flulike symptoms, sore throat, abdominal pain, fever, weight loss, night sweats, and fatigue can suggest infection or malignancies, whereas bleeding, easy bruising, pallor, jaundice, and petechial rashes can be attributable to hematologic etiologies.
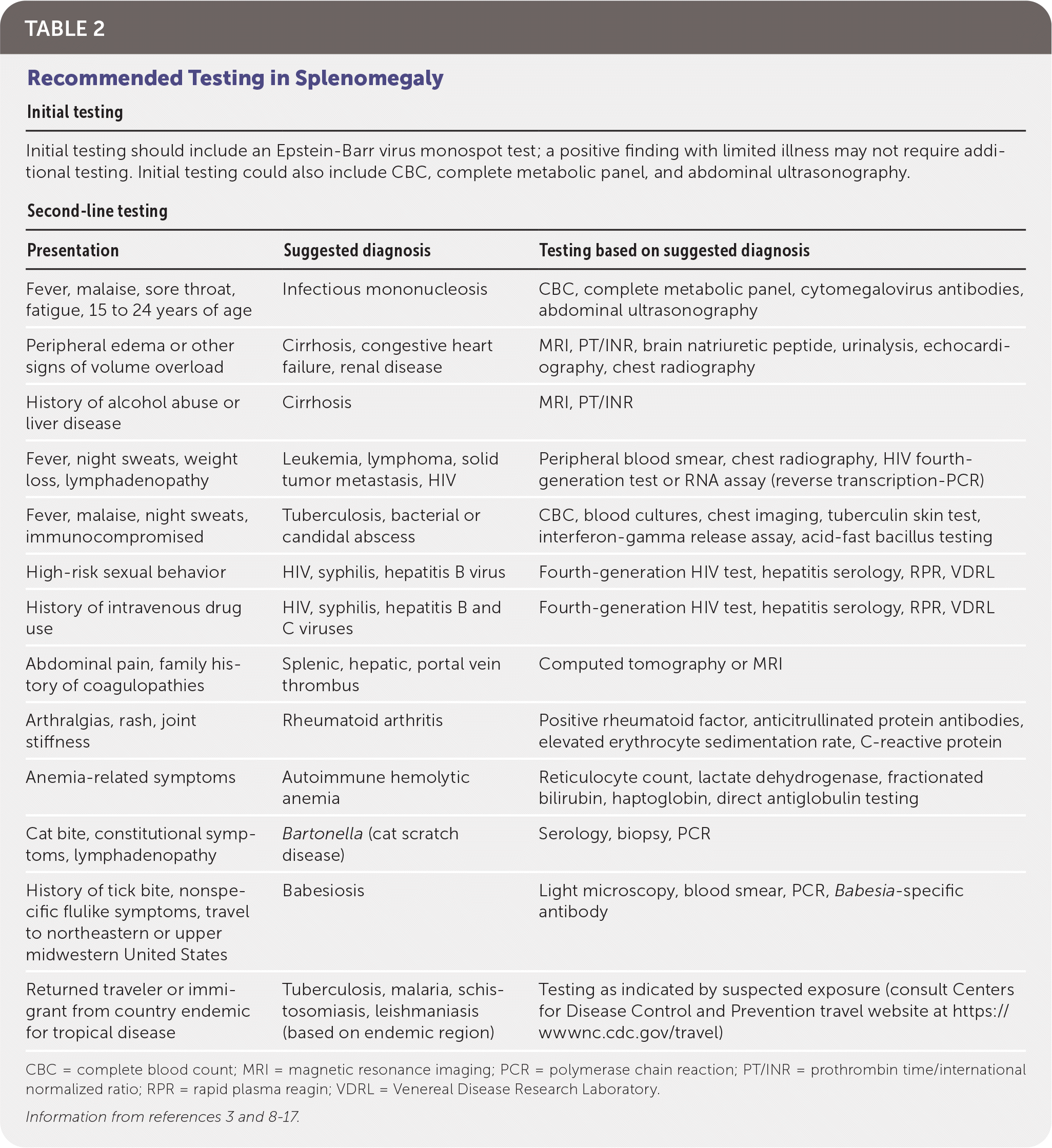
TABLE 2. Recommended Testing in Splenomegaly
| Initial testing | ||
| Initial testing should include an Epstein-Barr virus monospot test; a positive finding with limited illness may not require additional testing. Initial testing could also include CBC, complete metabolic panel, and abdominal ultrasonography. | ||
| Second-line testing | ||
| Presentation | Suggested diagnosis | Testing based on suggested diagnosis |
| Fever, malaise, sore throat, fatigue, 15 to 24 years of age | Infectious mononucleosis | CBC, complete metabolic panel, cytomegalovirus antibodies, abdominal ultrasonography |
| Peripheral edema or other signs of volume overload | Cirrhosis, congestive heart failure, renal disease | MRI, PT/INR, brain natriuretic peptide, urinalysis, echocardiography, chest radiography |
| History of alcohol abuse or liver disease | Cirrhosis | MRI, PT/INR |
| Fever, night sweats, weight loss, lymphadenopathy | Leukemia, lymphoma, solid tumor metastasis, HIV | Peripheral blood smear, chest radiography, HIV fourth-generation test or RNA assay (reverse transcription-PCR) |
| Fever, malaise, night sweats, immunocompromised | Tuberculosis, bacterial or candidal abscess | CBC, blood cultures, chest imaging, tuberculin skin test, interferon-gamma release assay, acid-fast bacillus testing |
| High-risk sexual behavior | HIV, syphilis, hepatitis B virus | Fourth-generation HIV test, hepatitis serology, RPR, VDRL |
| History of intravenous drug use | HIV, syphilis, hepatitis B and C viruses | Fourth-generation HIV test, hepatitis serology, RPR, VDRL |
| Abdominal pain, family history of coagulopathies | Splenic, hepatic, portal vein thrombus | Computed tomography or MRI |
| Arthralgias, rash, joint stiffness | Rheumatoid arthritis | Positive rheumatoid factor, anticitrullinated protein antibodies, elevated erythrocyte sedimentation rate, C-reactive protein |
| Anemia-related symptoms | Autoimmune hemolytic anemia | Reticulocyte count, lactate dehydrogenase, fractionated bilirubin, haptoglobin, direct antiglobulin testing |
| Cat bite, constitutional symptoms, lymphadenopathy | Bartonella (cat scratch disease) | Serology, biopsy, PCR |
| History of tick bite, nonspecific flulike symptoms, travel to northeastern or upper midwestern United States | Babesiosis | Light microscopy, blood smear, PCR, Babesia-specific antibody |
| Returned traveler or immigrant from country endemic for tropical disease | Tuberculosis, malaria, schistosomiasis, leishmaniasis (based on endemic region) | Testing as indicated by suspected exposure (consult Centers for Disease Control and Prevention travel website at https://wwwnc.cdc.gov/travel) |
CBC = complete blood count; MRI = magnetic resonance imaging; PCR = polymerase chain reaction; PT/INR = prothrombin time/international normalized ratio; RPR = rapid plasma reagin; VDRL = Venereal Disease Research Laboratory.
Physical Examination
Splenomegaly is often found on physical examination, but detection depends on the patient's habitus and the degree of enlargement of the spleen.5 The spleen is best evaluated with the patient supine with knees bent and feet on the table to relax the abdominal wall musculature. Percussion and palpation can determine splenomegaly because the spleen cannot be detected by either technique if it is not enlarged. Dullness to percussion in the lowest intercostal space at the left axillary line has an 82% sensitivity for splenomegaly.18 The overall sensitivity of palpation is 58%.18 Up to 16% of palpable spleens are found to be normally sized on imaging, so splenomegaly should be confirmed with ultrasonography.8 Normal spleens tend to be larger in men and taller people.19 Although there is no accepted definition of splenomegaly, a splenic diameter larger than 10 cm (3.9 in) is generally considered enlarged.19
Splenomegaly is considered massive when the lower pole is located in the left lower quadrant or right side of the abdomen.20 Massive splenomegaly can be missed on examination if the lower edge of the spleen is not recognized.
Splenic tenderness on examination can indicate infection, rupture, or infarct.5 Physical examination findings such as lymphadenopathy, peripheral edema, ruddy complexion, splinter hemorrhages, or elevated temperature can suggest infectious etiologies, whereas hepatomegaly, caput medusae, ascites, pallor, bruising, or petechiae can suggest liver or hematologic diseases (Table 23,8–17 ).
Diagnostic Approach
Evaluation of splenomegaly is guided by history and examination, focusing on the common etiologies of liver disease, malignancy, and infection.3 Not all patients warrant an extensive evaluation. For example, in a young adult with splenomegaly, constitutional symptoms, and a sore throat, testing for heterophile antibodies can often confirm the diagnosis.21 Without an obvious cause, imaging and further laboratory evaluation are often necessary.
BLOOD TESTS
A complete metabolic panel and complete blood count provide an initial evaluation for hepatic and hematologic etiologies of splenomegaly. A peripheral blood smear should be ordered when hematologic abnormalities are found or suspected. Prompt referral to oncology is necessary when blasts or abnormal red cell morphology or composition is identified. Abnormal liver function tests should lead the physician to evaluate for causes of liver disease and refer the patient to hepatology if indicated. Further testing should be guided by initial evaluation; recommended blood tests are found in Table 2.3,8–17
IMAGING
Sonographic measurements of the spleen length can estimate spleen volume within 2% of calculations based on computed tomography.22 The accuracy, cost-effectiveness, and lack of radiation make abdominal ultrasonography a first-line step for confirmation of size.3,5,6,8,14 In addition, ultrasonography may reveal splenic lesions or hepatobiliary pathology.8 When attempting to evaluate the spleen and nearby organs with more detail or when there is concern for malignancy, contrast-enhanced computed tomography is recommended.8,23 If portal vein thrombosis is suspected, then contrast-enhanced computed tomography is indicated. If peripheral edema or cirrhosis occurs or a focal lesion is suspected, magnetic resonance imaging may be needed.8
In a patient with pulmonary symptoms, chest imaging can help identify pulmonary or mediastinal masses suggesting malignancy, cavitary lesions suggesting tuberculosis, or bilateral hilar adenopathy suggesting sarcoidosis.
FURTHER EVALUATION
When initial evaluation does not point to the cause of splenomegaly, specialty referral is warranted to evaluate for malignancies and other hematologic disorders. Asymptomatic young adults with mild splenomegaly and no risk factors or apparent illness can be monitored over the course of weeks to months.8 In these cases, repeat laboratory evaluation and imaging can reveal occult conditions. Some causes of splenomegaly are ultimately revealed by splenic biopsy or diagnostic splenectomy.8
Management
Management of splenomegaly involves treating the underlying disease process. Depending on the level of experience of each physician, hepatology or hematology referrals may be warranted for definitive diagnosis and management.
With guidance from the Centers for Disease Control and Prevention or infectious disease consultants, many of the infectious causes of splenomegaly can be managed by family physicians.8
Spleen reduction therapies (e.g., irradiation, chemotherapy, transfusions) and splenectomy are occasionally used for painful splenomegaly or in malignancies. Splenectomy can be performed to control esophageal varices in liver disease or to control pain and other symptoms caused by massive splenomegaly.8 In some cases, splenectomy can also improve thrombocytopenia and leukopenia.2
In impaired splenic function caused by conditions such as sickle cell, HIV, splenic infarct, malignancy, or splenectomy, risk of infection with encapsulated organisms and influenza increases.24,25 Fevers are particularly concerning in these patients because progression to sepsis occurs more rapidly compared with individuals who have functioning spleens. Febrile patients with impaired splenic function should receive empiric antibiotic therapy. Daily antibiotic prophylaxis is indicated for one to two years after splenectomy, before respiratory tract procedures, and in any asplenic patient who has developed sepsis.
Oral penicillin twice daily is typically used for antibiotic therapy after splenectomy and before procedures (levofloxacin [Levaquin] can be used in penicillin-allergic patients). If an asplenic patient develops a fever but does not appear ill, immediate administration of ceftriaxone (Rocephin) is recommended. Patients who appear ill or who have laboratory results consistent with infection should be treated with cefepime and vancomycin (adults). Asplenic patients should be prescribed an emergency oral dose of antibiotics to take in the case of a fever if they are unable to get to a medical facility that can administer intravenous antibiotics within two hours. Amoxicillin or levofloxacin (if penicillin allergic) are the preferred agents.25
Vaccination against Streptococcus pneumoniae, Neisseria meningitidis, Haemophilus influenzae type b, and influenza virus lowers the risk of infections.24 A dose of 13-valent pneumococcal conjugate vaccine followed by 23-valent pneumococcal polysaccharide (PPSV23) vaccine eight weeks later, H. influenzae type b conjugate vaccination, and MenACWY should be given at least two weeks before planned splenectomy if the patient has not been previously vaccinated with an age-appropriate regimen. Booster doses of PPSV23 and MenACWY will be needed (see https://www.cdc.gov/vaccines/schedules/hcp/imz/adult.html for more information). If the splenectomy was emergent, see https://www.cdc.gov/vaccines/adults/rec-vac/health-conditions/asplenia.html for the vaccine schedule. All patients with functional asplenia should receive the inactivated flu vaccine yearly.
Complications
Acute infections, anemia, and splenic rupture are the most common complications of splenomegaly.2 Any trauma to an enlarged spleen carries the risk of rupture with significant blood loss. Up to one in every 200 cases of infectious mononucleosis is complicated by splenic rupture, highlighting the importance of counseling young and active patients.26 Current recommendations are to restrict contact activity for at least 21 days after symptom onset, regardless of a palpated spleen on examination.26 A small retrospective study of 42 cases shows that a significant number of ruptures occur between days 21 and 31, suggesting that return-to-play guidelines may need to be extended to 31 days.27 It is important to note that splenic rupture has been reported beyond even this cutoff.26,27 For this reason, in cases where splenomegaly was diagnosed at mononucleosis presentation, a follow-up examination after 31 days is suggested to ensure that the spleen is no longer palpable and for return-to-play shared decision-making.27 A risk of atraumatic splenic rupture also occurs in patients with underlying splenic pathology; this occurs most commonly with malignancies and infectious processes.9 Although return-to-play guidelines do not exist for splenomegaly, it would be prudent to recommend avoidance of strenuous activity or participation in contact sports in patients with any spleen pathology, including splenomegaly.
Data Sources: A Search of PubMed was completed using the key terms spleen, splenomegaly, enlarged spleen, and massive splenomegaly. The Cochrane Database of Systematic Reviews and the Essential Evidence Plus summary were also searched. Only references published in English were reviewed. Search dates were 2000 to 2020, with an expansion to 1990 to 2000 for a few additional studies. Search dates: April 2020 through February 2021.

