
Am Fam Physician. 2023;108(3):303-304
Author disclosure: No relevant financial relationships.
An otherwise healthy 69-year-old woman with no significant medical history presented with a facial rash that had appeared three days earlier. The rash had progressed to involve her left eyelid, and she had blurred vision.
Physical examination showed vesicles on erythematous bases around her left eye (Figure 1). Vesicles were present on the upper and lower eyelids, and redness of the eyes was noted. Other eye examination findings were normal. There was no purulent discharge, vesicles, or ulcers appreciated in the cornea. Findings on cranial nerve examination were unremarkable.
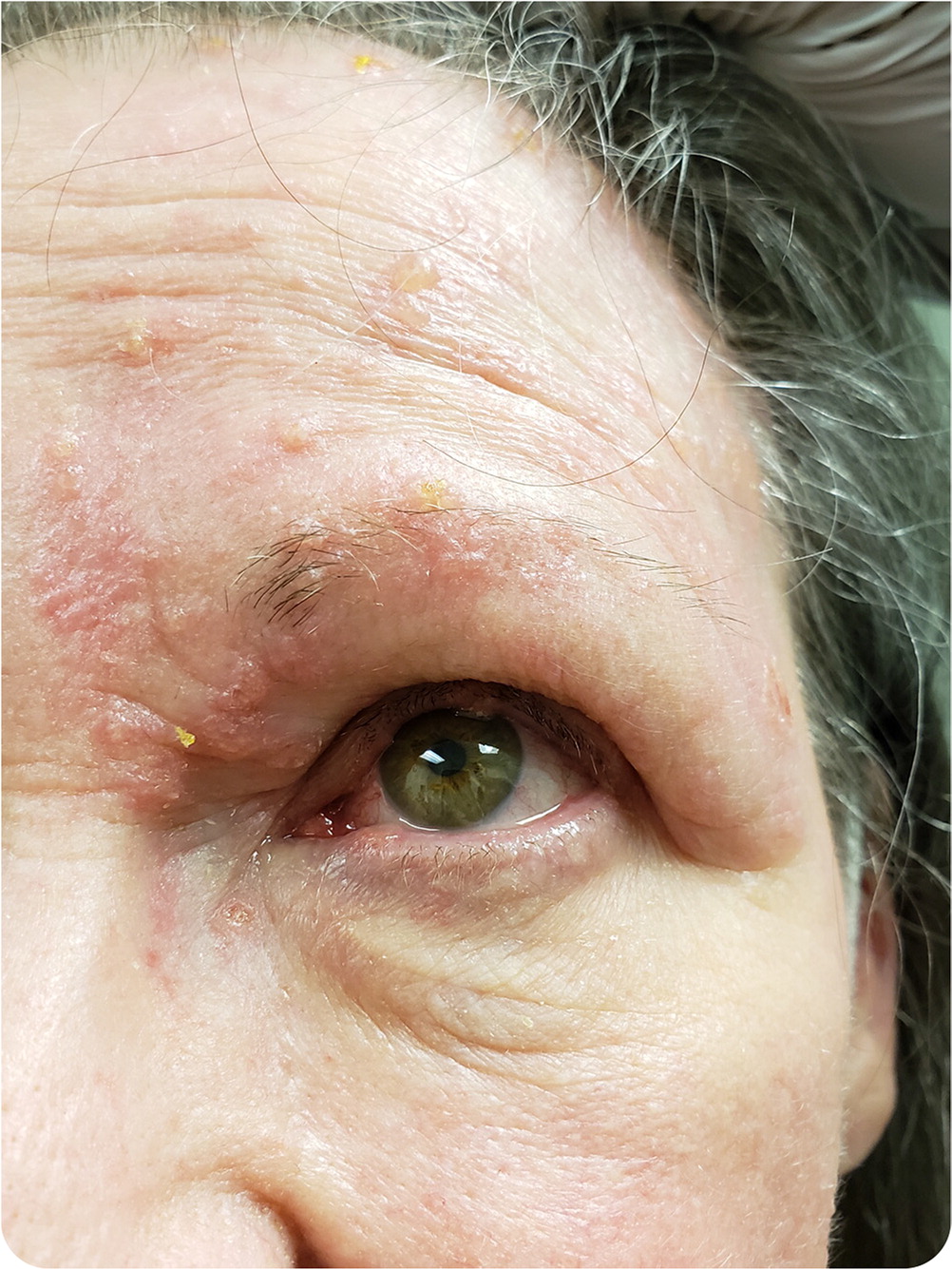
Question
Based on the patient's history and physical examination findings, which one of the following is the most appropriate next step?
A. Start oral antiviral monotherapy.
B. Admit for intravenous antiviral therapy.
C. Start prednisone and oral antiviral
D. Refer urgently to ophthalmology.
Discussion
The answer is D: refer urgently to ophthalmology to evaluate for herpes zoster ophthalmicus. Herpes zoster (shingles) is caused by reactivation of the varicella zoster virus. Herpes zoster ophthalmicus involves the ophthalmic division of the trigeminal nerve and can lead to severe vision-threatening complications.1 About 10% of the approximately 1 million herpes zoster cases per year present as herpes zoster ophthalmicus.2
Since 1995, the incidence of varicella has decreased through the widespread use of the varicella vaccine.3 However, most adults harbor latent virus. An estimated 99% of adults born before 1980 have had varicella infections, even if it was never diagnosed. In 2005, a live, attenuated vaccine became available for herpes zoster.4 The Advisory Committee on Immunization Practices recommends the zoster vaccine for adults older than 50 years to prevent herpes zoster and its complication of postherpetic neuralgia.2 Immunization is also recommended for younger adults with weakened immune systems.
Development of clinical herpes zoster is associated with aging, immunocompromised states, fatigue, or emotional stress. The classic presentation includes malaise, headache, edema, and paresthesia followed by a rash in the affected dermatome. The lesions usually present as erythematous vesicles. Ophthalmic involvement can result in serious complications, including keratitis, uveitis, blindness, orbital inflammation, and acute retinal necrosis.2,4,5
Herpes zoster ophthalmicus is commonly treated with oral antiviral agents; however, urgent referral to ophthalmology is needed for patients with ocular involvement. because prompt intervention reduces the risk of complications from corneal involvement. Treatment during the first 72 hours of the disease course has been shown to reduce pain and decrease vision-threatening complications. A 2022 systematic review of case reports found no significant difference in recovery rates between patients receiving oral and intravenous antiviral therapy.2,6–8
The views in this article are those of the authors and do not necessarily reflect the views or policy of the U.S. Department of the Navy, the U.S. Department of Defense, the U.S. government, or Naval Medical Center Camp Lejeune.
