Analyzing and eliminating physical and procedural barriers to immunization allowed this practice to improve its performance.

The degree to which pediatric patients are up-to-date on recommended immunizations is a key quality metric of well-child care – for both the patient and the practice. Inadequate immunization can increase the risk of acquiring serious infectious diseases. Low rates of immunization can also affect pay-for-performance incentives from insurance plans. In addition, if a practice participates in the Vaccines for Children (VFC) program, poor immunization rates can jeopardize its ability to receive federally subsidized vaccines. For each Medicaid-insured child 6 years old or younger in our urban family medicine practice, we receive about $1,400 worth of vaccines through VFC. The loss of this resource would be devastating for both patients and our practice.
For these reasons, and as part of our pursuit of level-3 patient-centered medical home (PCMH) recognition by the National Committee for Quality Assurance, our practice decided to focus on improving well-child care, and specifically on ensuring up-to-date immunizations, which resulted in dramatic increases in our immunization rates. This article describes what we learned in hopes that other practices might replicate our effort and results.
Our approach
The main metric used by our local health department's VFC program is the completion by age 24 months of four vaccinations for DTaP (diphtheria, tetanus, and pertussis), three for polio, one for MMR (measles, mumps, and rubella), three for Hib (Haemophilus influenzae type B), three for Hepatitis B, one for varicella, and four pneumococcal conjugate vaccinations (PCV7), also known as the “4:3:1:3:3:1:4” series. For children 19 to 35 months of age, the national average for completion of this series in 2012 was 68.4 percent.1 At our combined resident/faculty office, the series completion rate was a disappointing 43 percent in 2010. Meanwhile, chart audits by our department of public health also indicated a high rate (36 percent) of “missed opportunities,” or instances when a child came to the office for some other reason and was not offered the vaccines that were due.
Our PCMH working group, composed of attending physicians, nurses, clinic managers, social workers, residents, pharmacy faculty, medical assistants, and secretarial staff, met weekly, participated in a statewide PCMH residency program collaborative, and underwent quality improvement training.2 Our team gained process improvement skills, including measuring clinical performance, performing rapid PDSA (plan-do-study-act) cycles, conducting stakeholder research and root cause analysis, and developing and testing solutions.3,4 These skills were then applied to improving child immunization rates with the help of tools borrowed from the corporate and manufacturing worlds (these tools are described in the next section),3,4 and all potential solutions were methodically tested.5
What we found
The team's analysis revealed that employees throughout our practice were involved in the immunization process, which increased the complexity of our improvement efforts. Although physicians placed the orders for and sometimes gave the immunizations, medical assistants handled and documented the vaccines, and nurses administered most of the shots. Meanwhile, non-clinical staff members handled the scheduling of patients and addressed the needs of unscheduled walk-in patients.
In our office, we assigned a licensed practical nurse to vaccinate adult and child patients during each clinical session. A spaghetti diagram was created by tracking this nurse's footsteps over the course of a single afternoon. We found that the nurse wasted a lot of time traveling between the two refrigerators where we held the vaccines, one for regular stock and one for vaccines provided by VFC. (See more information about spaghetti diagrams.) We had separated the vaccines because of concerns that patients not eligible for VFC would receive the VFC stock.
We also developed a fishbone diagram to identify potential root causes for missed vaccinations. (See more information about fishbone diagrams.) We identified several broad categories, such as scheduling problems, parent refusal, problems with stock or supply, staffing limitations, poor documentation or missing records, failure to order needed shots, and patients leaving before shots were given.
To determine which causes were the most significant, we performed a clinical chart abstraction and contacted the families of children who were not up-to-date on the vaccination series. We noted the number of times a particular cause was associated with a patient who was not up-to-date. Using Pareto charting (see “Causes of low immunization rates in the practice”), we determined that four causes contributed to more than 80 percent of cases where immunizations were not up-to-date:
- Patients had left the practice but were still being counted in the vaccine series denominator,
- Patients had failed to show for their appointment and not rescheduled,
- Opportunities were missed to immunize during non-preventive visits,
- Staff were giving doses at incorrect intervals or were making other mistakes that made the immunizations medically invalid.
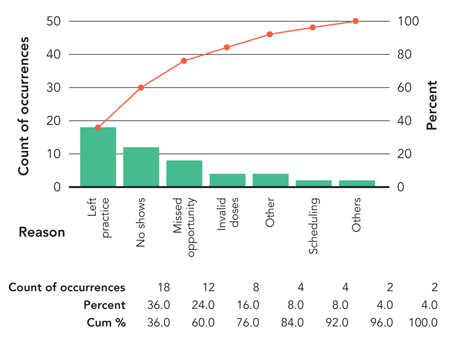
CAUSES OF LOW IMMUNIZATION RATES IN THE PRACTICE
How we responded
As a result of our analysis, we were able to develop potential solutions to the most significant causes of low immunization rates. First, using our electronic health record (EHR) we identified and removed from our immunization roster patients whose insurer no longer listed us as their primary care provider or who had clearly indicated to us that they were leaving the practice, for example, by requesting that their records be transferred. This change proved to be the single most important step to improve our rates and continues to inform how our practice identifies patient panels for population health management.
On the clinical front, we implemented a number of strategies:
- Provider and staff education. We held an education session on childhood immunization schedules for faculty, residents, and staff. The session was led by a local guest physician from the American Academy of Pediatrics, and clinical hours were blocked to maximize participation in the session.
- Previsit planning. A nurse reviews the immunization history of every patient age 18 or under before his or her scheduled appointment, reconciling that history with the city's online immunization registry and Centers for Disease Control and Prevention (CDC) guidelines. An immunization recommendation note is placed in the EHR to help the medical assistant or other provider see what vaccines are needed at the time of the visit. While not always possible for same-day or next-day appointments, this previsit planning has proven useful for the majority of our pediatric appointments.
- Vaccine order “smart sets.” Correctly ordering vaccines within the EHR can be challenging, especially when so many different vaccines are involved. We created pediatric vaccine order “smart sets” to simplify the process within our EHR, with orders organized by the age at which the shots are typically given. This required technical assistance from our EHR support staff.
- Vaccine accessibility. We reorganized the vaccine refrigerators so that both VFC and non-VFC stock were available at both wings of our large office suite. This minimized wasted steps for support staff, reduced wait times for patients, and decreased the number of patients leaving before getting their shots. We use color-coordinated plastic bins to keep the refrigerators organized and to address concerns about mixing VFC and non-VFC stock.
- No-show reminder letters. Clinic staff review all pediatric no-show appointments. When a child who is due for immunizations misses an appointment, a letter is generated and mailed, letting the family know that the appointment was missed and that shots are due. The letter provides instructions for scheduling a make-up appointment or returning for a shots-only nurse visit. (See “Immunization reminder letter.”)
- No-show reminder phone calls. In addition to the letters, staff called families after missed appointments to let them know shots were overdue.
- Walk-in immunizations. For standard CDC-recommended immunizations, we no longer require scheduled appointments, assuming the patient has an existing relationship with us. Patients who need a physician exam or have other needs are still encouraged to make an appointment, but those who only need to catch up on shots can have a nurse visit on a walk-in basis. Standing order protocols are in place so that nurses may act quickly to provide the needed immunizations.
IMMUNIZATION REMINDER LETTER
Patient's name:
DOB:
Dear Parent or Guardian:
Our records show that your child is due for his/her shots.
Immunizations are an important way to keep your child healthy and free from disease. Remember that immunizations work best when they are given on time.
Please come by our office for (PATIENT'S FIRST NAME) to get his/her shots.
We recommend that you come in next week to take care of these very important immunizations before you forget. No appointment is needed for routine shots. Please see below for our office walk-in hours for immunizations. If your child also needs a physical, that can be scheduled at another time.
We hope to see you soon!
Sincerely,
(PHYSICIAN)
(PRACTICE NAME and HOURS OF OPERATION)
How it worked
Even after just six months of implementation, we began to notice improvements, which continued over the following year. Our vaccine series completion rates increased from 43 percent to 71 percent, and our missed opportunity percentage dropped to the single digits (see “Results of interventions”). We found that we were able to sustain the positive changes seen in our early efforts over time because they were integrated into our general workflow. The only strategy we stopped using, largely for staffing reasons, was making reminder phone calls to the families of patients who missed appointments. We determined that we were able to achieve acceptable follow-up immunization rates with reminder letters alone.
It is hard for us to quantify what financial impact these changes have had in terms of additional revenue or costs. But it is clear that if we had not improved our performance we would be at risk of losing the VFC vaccines because of program eligibility requirements.
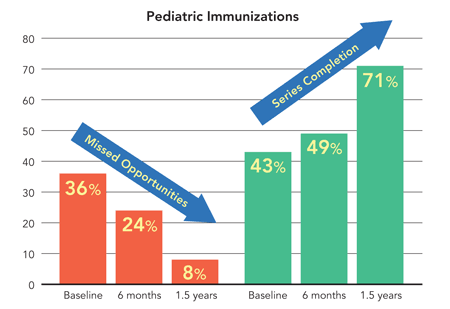
RESULTS OF INTERVENTIONS
The practice found that over time, as missed opportunities declined, the percentage of patients completing the pediatric 4:3:1:3:3:1:4 vaccine series increased. Note that the national average series completion percentage in 2012 was 68.4 percent.
Keys to success
Our keys to success included developing and sustaining an interdisciplinary team focused on improving the care of our patients. We have gained valuable experience with quality improvement tools we can use to identify root causes and create feasible and sustainable solutions for many other clinically important issues. Realizing the potential that team-based approaches have for achieving clinical quality improvement in our busy primary care practice continues to motivate us.

