
Am Fam Physician. 2003;67(11):2329-2332
Z-plasty is a plastic surgery technique that is used to improve the functional and cosmetic appearance of scars. With this technique, it is possible to redirect a scar into better alignment with a natural skin fold or the lines of least skin tension. Contracted scars may be lengthened with this technique. Z-plasty involves the creation of two triangular flaps of equal dimension that are then transposed. Basic z-plasty flaps are created using an angle of 60 degrees on each side, which can lengthen a scar by 50 to 70 percent and reorient the direction of the central wound by 90 degrees. Keeping the length and angle of each flap precisely the same is key to avoiding mismatched flaps that may be difficult to close. Some possible complications of z-plasty include flap necrosis, hematoma formation under the flaps, wound infection, trapdoor effect, and sloughing of the flap caused by high wound tension.
Z-plasty is a plastic surgery technique used to improve the functional and cosmetic appearance of scars. It involves the creation of two triangular flaps of equal dimension that are then transposed.1
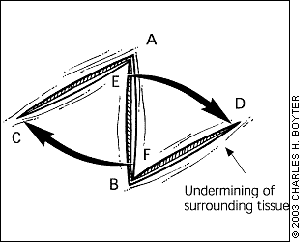
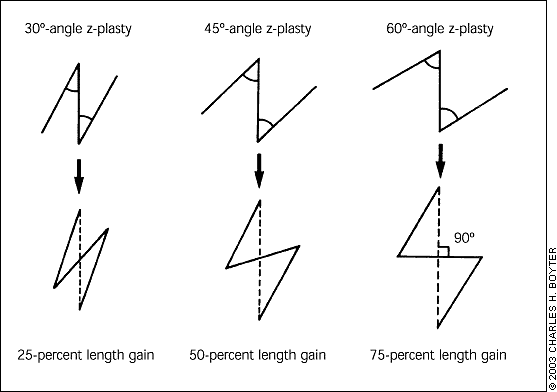
For a basic z-plasty, the triangular flaps are created using an angle of 60 degrees (Figures 1a through 1e). Theoretically, this angle can lengthen a contracted scar by about 75 percent and reorient the direction of the central wound by 90 degrees. In practice, the lengthening and reorientation will be less, owing to increased wound tension.
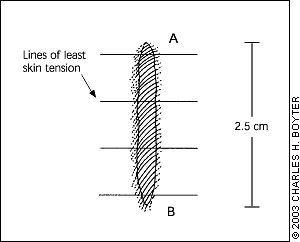
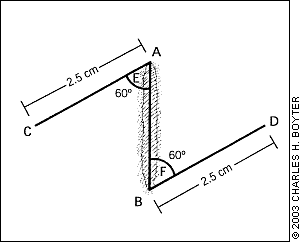
Angles smaller than 60 degrees are easier to transpose but result in less lengthening and realignment of the scar to less than 90 degrees. Angles larger than 60 degrees should be avoided because the force required to transpose the flaps increases markedly, making closure of the wound difficult. The length of each of the lateral limbs of the z-plasty must be precisely equal to the central incision over the original scar, or puckering at the corners will result, and additional undermining and trimming of the flaps will be necessary to obtain proper closure. The multiple variations of the basic z-plasty are beyond the scope of this article.2
In a primary care setting, z-plasty is reserved for improvement of linear, thin scars and is not used as a primary closure technique. The most common situation in which a z-plasty would be used is an unfavorable cosmetic or functional scar that has not improved after waiting for a reasonable length of remodeling time (e.g., one year). More complicated scar situations, such as burn scar contractures, wide scar contractures on fingers, and hypertrophic or keloid scars, typically involve plastic surgery techniques other than basic z-plasty.
Indications
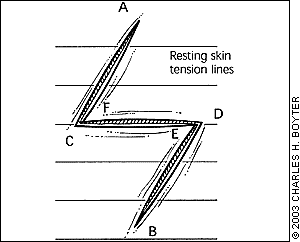
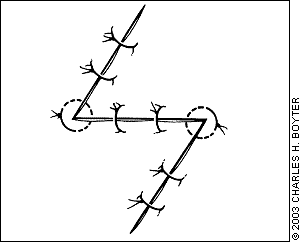
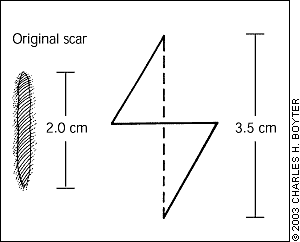
Common indications for z-plasty include (1) lengthening of a contracted linear scar across a flexor crease (Figures 2a and 2b)—flexion contracture is released, and functionality across the scar is improved; and (2) changing the direction of a cosmetically unfavorable scar (Figure 3)—the scar is realigned along a natural skin fold or along the lines of least skin tension, creating less tension on the wound and resulting in a cosmetically superior scar appearance.
Technique
The mechanics of the technique must be clearly understood by the physician before the procedure is attempted. The procedure and its risks and benefits are first explained to the patient, and an informed consent is obtained.
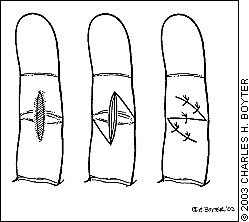
A basic z-plasty is performed using the steps illustrated in Figures 1a through 1e.
The surgical site is prepped with an antibacterial solution, such as povidone-iodine (Beta-dine), and sterile drapes are applied.
Two arms are drawn at each end of the linear scar, inscribing an angle of 60 degrees to the scar. The side arms are exactly equal in length to the central scar and have precisely the same angle.
Local or regional anesthesia is administered. Vertical incisions are made through the skin along the lines, using a no. 15 scalpel blade.
Full-thickness skin flaps are undermined at the level of subcutaneous fat, creating two triangular flaps of equal size and shape. Adequate undermining of surrounding subcutaneous tissue is performed to achieve proper mobilization of the flaps.
The two flaps are then transposed around each other, changing the direction of the original scar.
The flaps are held in place with a few anchoring stitches.
The skin is closed using interrupted sutures. Corner stitches may be used for the flap tips.
Topical antibiotics and a pressure dressing are applied over the wound to minimize the chance of hematoma formation caused by the undermining.
The wound is re-examined in one to two days, and sutures are removed in seven to 14 days.
Complications
Z-plasty may be complicated by flap necrosis, hematoma formation, wound infection, sloughing of the flap caused by high wound tension, and the trapdoor effect (elevation of central tissue resulting from a downward contraction of a surrounding scar).
Most complications may be prevented by meticulous attention to technique.3 When possible, patients should be advised to stop taking anticoagulants before the surgery, and if a hematoma is thought to be present during the postoperative course, large-bore needle aspiration may be performed. Routine wound care instructions are given to the patient, and prophylactic antibiotics may be considered for use in patients with diabetes and in other immunocompromised patients. The trapdoor effect may be avoided by employing sufficient undermining of tissues surrounding the flap site.