As the U.S. population ages and the prevalence of cardiovascular disease increases, the prevalence of atrial fibrillation (AF) is expected to increase from its current level of 2 million persons. Given the risk of stroke in patients with AF, a reliable risk stratification scheme would help identify patients at high risk, especially those who would benefit from therapies such as warfarin. Current stratification schemes may be based on biased studies. Wang and colleagues tested a classification scheme for patients with AF that focused on stroke risk alone and stroke risk or death as outcomes.
Using data from the Framingham Heart Study, the authors identified 705 eligible persons with new-onset AF who were not treated with warfarin at baseline and were used in the creation of the risk scores. Baseline risk factor data included blood pressure measurements, presence or absence of diabetes, current cigarette smoking, valvular heart disease, and left ventricular hypertrophy. Previous myocardial infarction, congestive heart failure, transient ischemic attack, or stroke also were evaluated in the analysis. Warfarin or aspirin use was determined by self-report. Primary outcomes were stroke alone and stroke or death. Analyses were conducted before and after excluding subjects who had received warfarin.
FIGURE 1. Predicted Five-Year Risk of Stroke
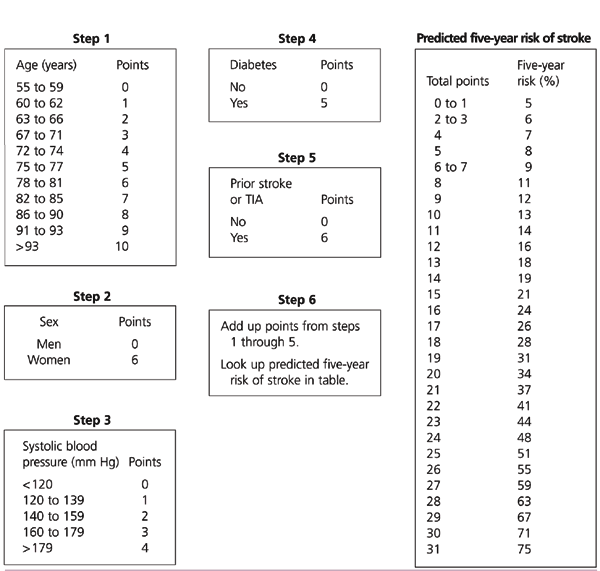
Predicted five-year risk of stroke. The point-based risk estimate approximates the more precise equation-based risk function provided as an Excel spreadsheet available athttp://www.nhlbi.nih/gov/about/framingham/stroke.htm. The point-based risk estimate may differ from the equation-based one, particularly in patients with uncommon combinations of characteristics. (TIA = transient ischemic attack)
Adapted with permission from Wang TJ, Massaro JM, Levy D, Vasan RS, Wolf PA, D'Agostino RB, et al. A risk score for predicting stroke or death in individuals with new-onset atrial fibrillation in the community. The Framingham Heart Study. JAMA 2003;290:1052.
During a mean follow-up of 4.3 years, stroke occurred in 111 persons (13 percent) and stroke or death occurred in 485 persons (56 percent). After excluding those who received warfarin, the analysis yielded 83 strokes and 382 strokes or deaths after 4.0 years. Results of the Cox proportional hazards analyses yielded the following predictors for stroke: female sex, diabetes, and previous stroke or transient ischemic attack. For stroke or death, the following predictors entered the model: smoking, diabetes, previous myocardial infarction or congestive heart failure, heart murmur, and left ventricular hypertrophy. Figures 1 and2 present a scoring system to predict five-year risk of stroke and combined stroke or death.
The results of this study are similar to results of previous studies with regard to risk factors such as diabetes, advancing age, and elevated blood pressure. By deriving clinical risk scores, the current classification scheme can be used to estimate the absolute risk of an adverse event in patients with AF. These results may influence clinical decision-making, particularly in patients who are at especially low or high risk.
FIGURE 2. Predicted Five-Year Risk of Stroke or Death
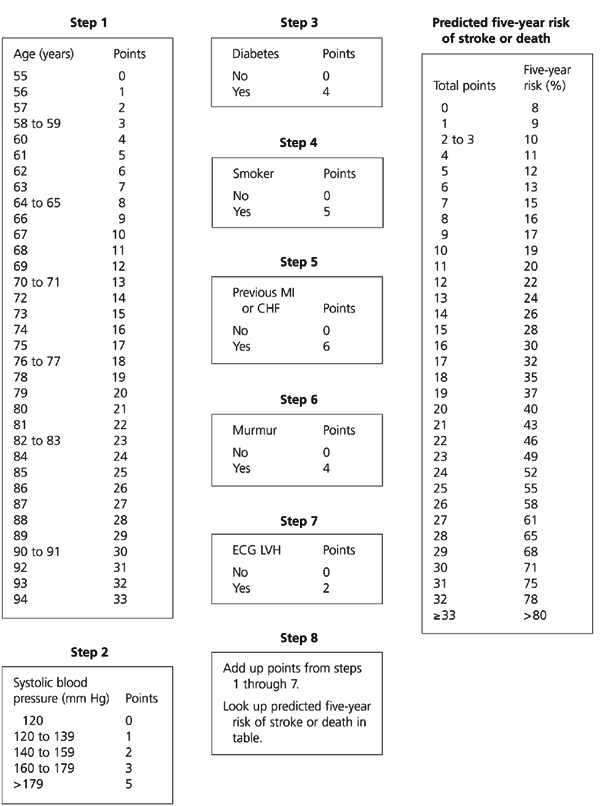
Risk score for stroke or death. The point-based system approximates the more precise equation-based risk function provided as an Excel spreadsheet available athttp://www.nhlbi.nih.gov/about/framingham/stroke.htm. The point-based risk estimate may differ from the equation-based one, particularly in patients with uncommon combinations of characteristics. (MI = myocardial infarction; CHF = congestive heart failure; ECG LVH = electrocardiographic left ventricular hypertrophy)
Adapted with permission from Wang TJ, Massaro JM, Levy D, Vasan RS, Wolf PA, D'Agostino RB, et al. A risk score for predicting stroke or death in individuals with new-onset atrial fibrillation in the community. The Framingham Heart Study. JAMA 2003;290:1053.

