Clinical Question
Which children with respiratory tract symptoms are likely to have pneumonia?
Evidence Summary
Pneumonia remains a common source of morbidity and mortality in children. A key question in the diagnostic evaluation of children with acute respiratory illness is whether chest radiography should be performed to rule in or rule out the diagnosis of pneumonia. Radiologically, pneumonia is defined as an infiltrate seen on chest radiography in a child with symptoms of an acute respiratory illness. Although there is considerable literature on the diagnosis of pneumonia in children in the developing world, this review focuses on studies in Europe and North America because the clinical presentation, health care system, and microbiology in these settings are more relevant.
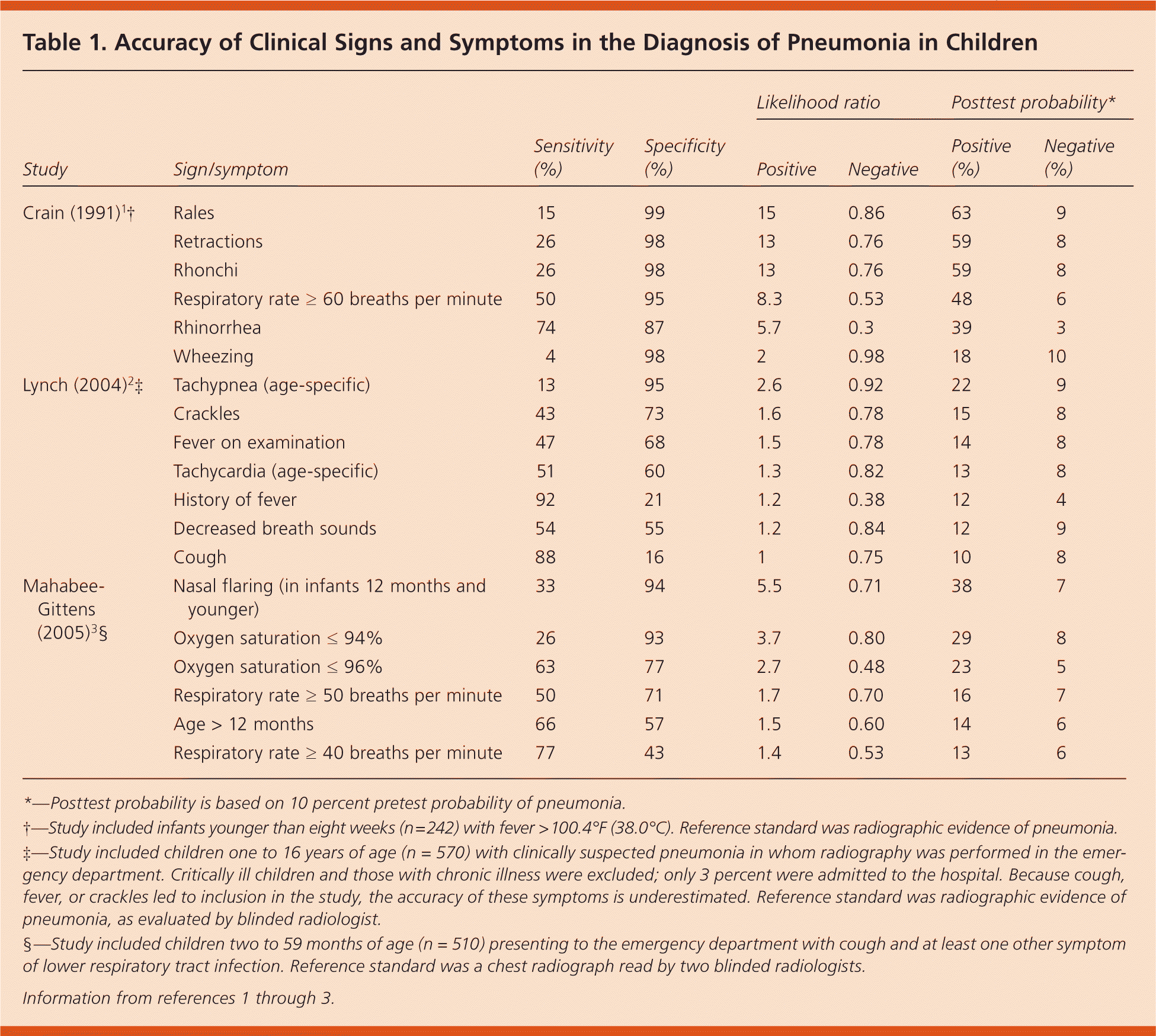
Individual signs and symptoms that are useful in diagnosing pneumonia in different age groups are shown in Table 1.1–3 Fever, tachypnea, nasal flaring (in infants), and reduced oxygen saturation are predictive of pneumonia. These findings, especially in infants, are highly specific and greatly increase the likelihood of pneumonia when present. However, their absence does not rule out pneumonia, and the accuracy of any individual sign or symptom is limited.
Table 1. Accuracy of Clinical Signs and Symptoms in the Diagnosis of Pneumonia in Children
| Study | Sign/symptom | Sensitivity (%) | Specificity (%) | Likelihood ratio | Posttest probability* | ||
|---|---|---|---|---|---|---|---|
| Positive | Negative | Positive (%) | Negative (%) | ||||
| Crain (1991)1 † | Rales | 15 | 99 | 15 | 0.86 | 63 | 9 |
| Retractions | 26 | 98 | 13 | 0.76 | 59 | 8 | |
| Rhonchi | 26 | 98 | 13 | 0.76 | 59 | 8 | |
| Respiratory rate ≥ 60 breaths per minute | 50 | 95 | 8.3 | 0.53 | 48 | 6 | |
| Rhinorrhea | 74 | 87 | 5.7 | 0.3 | 39 | 3 | |
| Wheezing | 4 | 98 | 2 | 0.98 | 18 | 10 | |
| Lynch (2004)2 ‡ | Tachypnea (age-specific) | 13 | 95 | 2.6 | 0.92 | 22 | 9 |
| Crackles | 43 | 73 | 1.6 | 0.78 | 15 | 8 | |
| Fever on examination | 47 | 68 | 1.5 | 0.78 | 14 | 8 | |
| Tachycardia (age-specific) | 51 | 60 | 1.3 | 0.82 | 13 | 8 | |
| History of fever | 92 | 21 | 1.2 | 0.38 | 12 | 4 | |
| Decreased breath sounds | 54 | 55 | 1.2 | 0.84 | 12 | 9 | |
| Cough | 88 | 16 | 1 | 0.75 | 10 | 8 | |
| Mahabee-Gittens (2005)3 § | Nasal flaring (in infants 12 months and younger) | 33 | 94 | 5.5 | 0.71 | 38 | 7 |
| Oxygen saturation ≤ 94% | 26 | 93 | 3.7 | 0.80 | 29 | 8 | |
| Oxygen saturation ≤ 96% | 63 | 77 | 2.7 | 0.48 | 23 | 5 | |
| Respiratory rate ≥ 50 breaths per minute | 50 | 71 | 1.7 | 0.70 | 16 | 7 | |
| Age > 12 months | 66 | 57 | 1.5 | 0.60 | 14 | 6 | |
| Respiratory rate ≥ 40 breaths per minute | 77 | 43 | 1.4 | 0.53 | 13 | 6 | |
*— Posttest probability is based on 10 percent pretest probability of pneumonia.
†— Study included infants younger than eight weeks (n=242) with fever >100.4°F (38.0°C). Reference standard was radiographic evidence of pneumonia.
‡— Study included children one to 16 years of age (n = 570) with clinically suspected pneumonia in whom radiography was performed in the emergency department. Critically ill children and those with chronic illness were excluded; only 3 percent were admitted to the hospital. Because cough, fever, or crackles led to inclusion in the study, the accuracy of these symptoms is underestimated. Reference standard was radiographic evidence of pneumonia, as evaluated by blinded radiologist.
§— Study included children two to 59 months of age (n = 510) presenting to the emergency department with cough and at least one other symptom of lower respiratory tract infection. Reference standard was a chest radiograph read by two blinded radiologists.
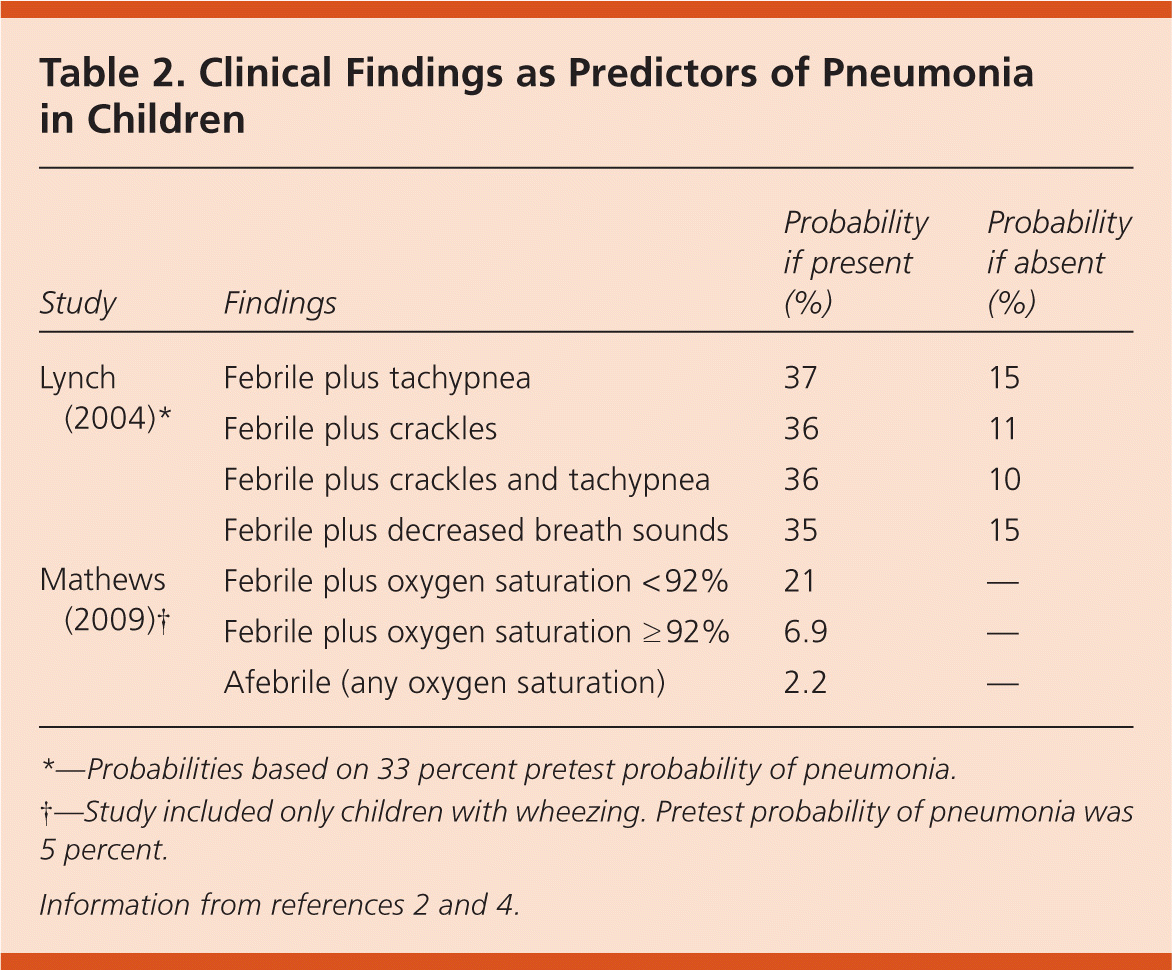
Several clinical decision rules have been developed that combine signs and symptoms to predict the likelihood of pneumonia in children. Lynch and colleagues identified fever, decreased breath sounds, crackles, and tachypnea as independent predictors of pneumonia in a group of 570 children one to 16 years of age presenting to the emergency department (ED) with clinical suspicion of pneumonia.2 Findings of fever plus decreased breath sounds, crackles, or tachypnea; or fever, crackles, and tachypnea had excellent sensitivity (93 to 97 percent) but poor specificity (11 to 19.4 percent). The positive predictive value for these findings is shown in Table 2.2,4
Table 2. Clinical Findings as Predictors of Pneumonia in Children
| Study | Findings | Probability if present (%) | Probability if absent (%) |
|---|---|---|---|
| Lynch (2004)* | Febrile plus tachypnea | 37 | 15 |
| Febrile plus crackles | 36 | 11 | |
| Febrile plus crackles and tachypnea | 36 | 10 | |
| Febrile plus decreased breath sounds | 35 | 15 | |
| Mathews (2009)† | Febrile plus oxygen saturation < 92% | 21 | — |
| Febrile plus oxygen saturation ≥ 92% | 6.9 | — | |
| Afebrile (any oxygen saturation) | 2.2 | — |
*— Probabilities based on 33 percent pretest probability of pneumonia.
†— Study included only children with wheezing. Pretest probability of pneumonia was 5 percent.
A second rule was proposed by Mahabee-Gittens and colleagues, who studied 510 children two to 59 months of age presenting to the ED with cough and at least one other symptom of lower respiratory tract infection.3 Age older than 12 months, a respiratory rate of at least 50 breaths per minute, oxygen saturation of 96 percent or less, and nasal flaring (in infants 12 months and younger) were the best independent predictors of pneumonia in a multivariate model. However, this rule is too complex to use at the point of care and has not been prospectively validated.
In a study of 526 children in whom chest radiography was performed after they presented to the ED with wheezing, only fever and oxygen saturation of less than 92 percent were used to develop a model predicting infiltrates on radiography.4 Afebrile children (temperature of less than 100.4°F [38.0°C]) had a 2.2 percent risk of pneumonia (seven out of 317), whereas febrile children with oxygen saturation of 92 percent or greater had a 6.9 percent risk of pneumonia (12 out of 175), and febrile children with oxygen saturation less than 92 percent had a 21 percent risk of pneumonia (seven out of 34)4 (Table 2).2,4
Although none of these rules has been prospectively validated, there is good consistency between the signs and symptoms identified by each. Two out of three rules include fever, tachypnea, and reduced oxygen saturation. The absence of all three signs makes pneumonia unlikely, whereas the presence of at least two of the signs is associated with a high risk of pneumonia.

