Currently, a gap of more than $135,000 separates the median annual subspecialist income from that of a primary care physician, yielding a $3.5 million difference in expected income over a lifetime. These income disparities dissuade medical students from selecting primary care and should be addressed to ensure sufficient patient access to primary care.
The income gap between primary care physicians and subspecialists has grown steadily since 1979.1 At the extreme, nearly $250,000 separated the median annual income of primary care physicians from the incomes of physicians in diagnostic radiology and orthopedic surgery in 2004 (see accompanying figure).1 Over the past 30 years, the growth of this income gap reduced the odds of medical students choosing primary care or family medicine by nearly one half. It also reduced the odds of students working in a federally qualified health center or rural health center by 30 percent, and of practicing in a rural area by almost 20 percent.1
Figure.
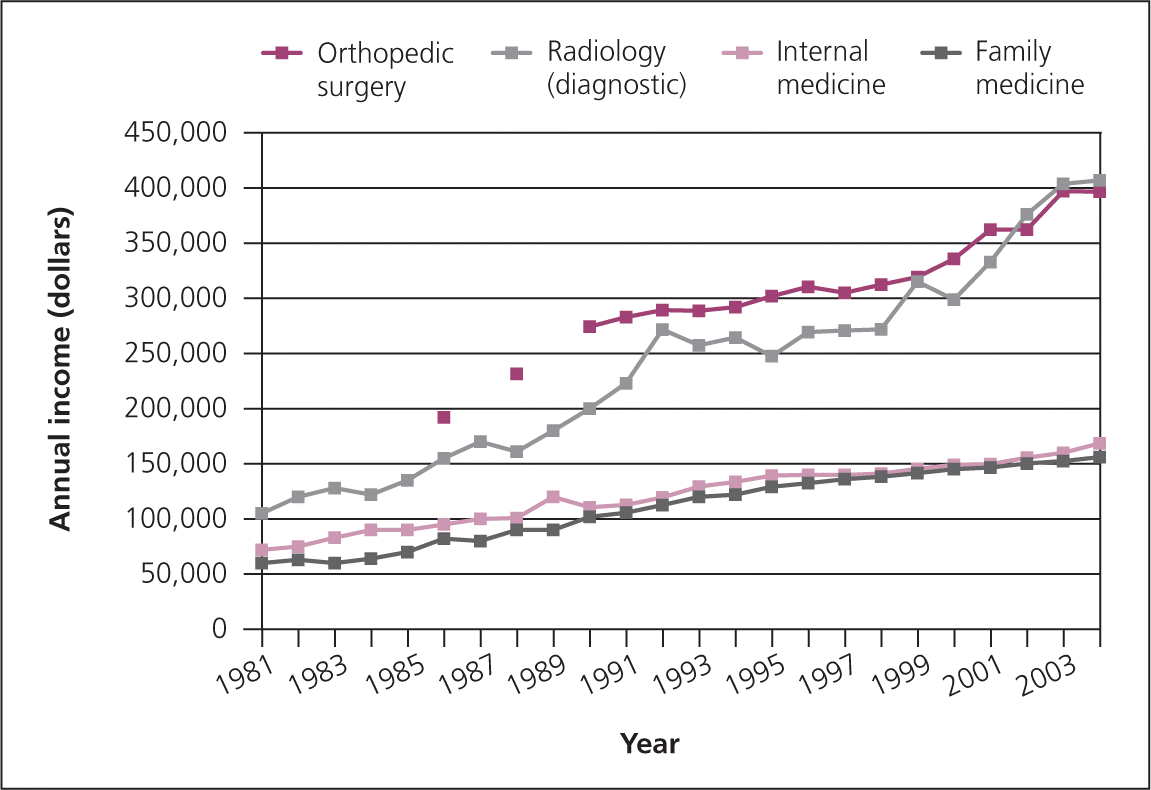
Comparison of annual income (median compensation) by physician subspecialty.
Adapted with permission from Phillips RL Jr, et al.; Robert Graham Center. Specialty and geographic distribution of the physician workforce: what influences medical student and resident choices? March 2009. https://www.graham-center.org/online/graham/home/publications/monographs-books/2009/rgcmo-specialty-geographic.html. Accessed January 4, 2010.
The resulting difference in expected income over the average physician career is impressive. Data from the Department of Labor Statistics and the Medical Group Management Association show that primary care physicians earn a cumulative average lifetime net income of nearly $6.5 million compared with more than $10 million for subspecialists.1
Medical students who select non–primary-care specialties stand to reap considerable financial benefits over those who choose primary care, despite the limited additional training time and expense involved in subspecializing. Even students who select business, law, and dentistry—careers with lower opportunity costs than medicine—can also expect greater relative financial rewards; the lifetime return on investment for each was greater than for primary care in the 1990s, and likely remains as such.2 Policies reversing the growth of payment disparities could attract more students to primary care and secure access to an adequate primary care workforce.

