Guideline source: National Heart, Lung, and Blood Institute
Evidence rating system used? Yes
Literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Published source: Pediatrics, December 2011
Although it is rare for cardiovascular disease (CVD) to manifest in children and adolescents, risk factors and behaviors do start in childhood. Evidence indicates that reducing risk can slow the progression of CVD; therefore, the National Heart, Lung, and Blood Institute (NHBLI) Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents developed guidelines to help health care professionals promote cardiovascular health and to identify and manage risk factors in children and adolescents. These guidelines were based on evidence that atherosclerosis begins, and its risk factors can be identified, in childhood; that atherosclerosis development and progression are associated with these risk factors; that risk factors track from childhood into adulthood; and that there are options for managing these risk factors.
Prevention goals in young persons should be separate from prevention goals in older persons in whom atherosclerosis is well established. Historically, preventing the development of risk factors and preventing CVD through effective management of risk factors have been the two main goals in young persons. Research supports the theory that childhood populations with lower levels of cardiovascular risk factors will have less atherosclerosis and CVD as adults.
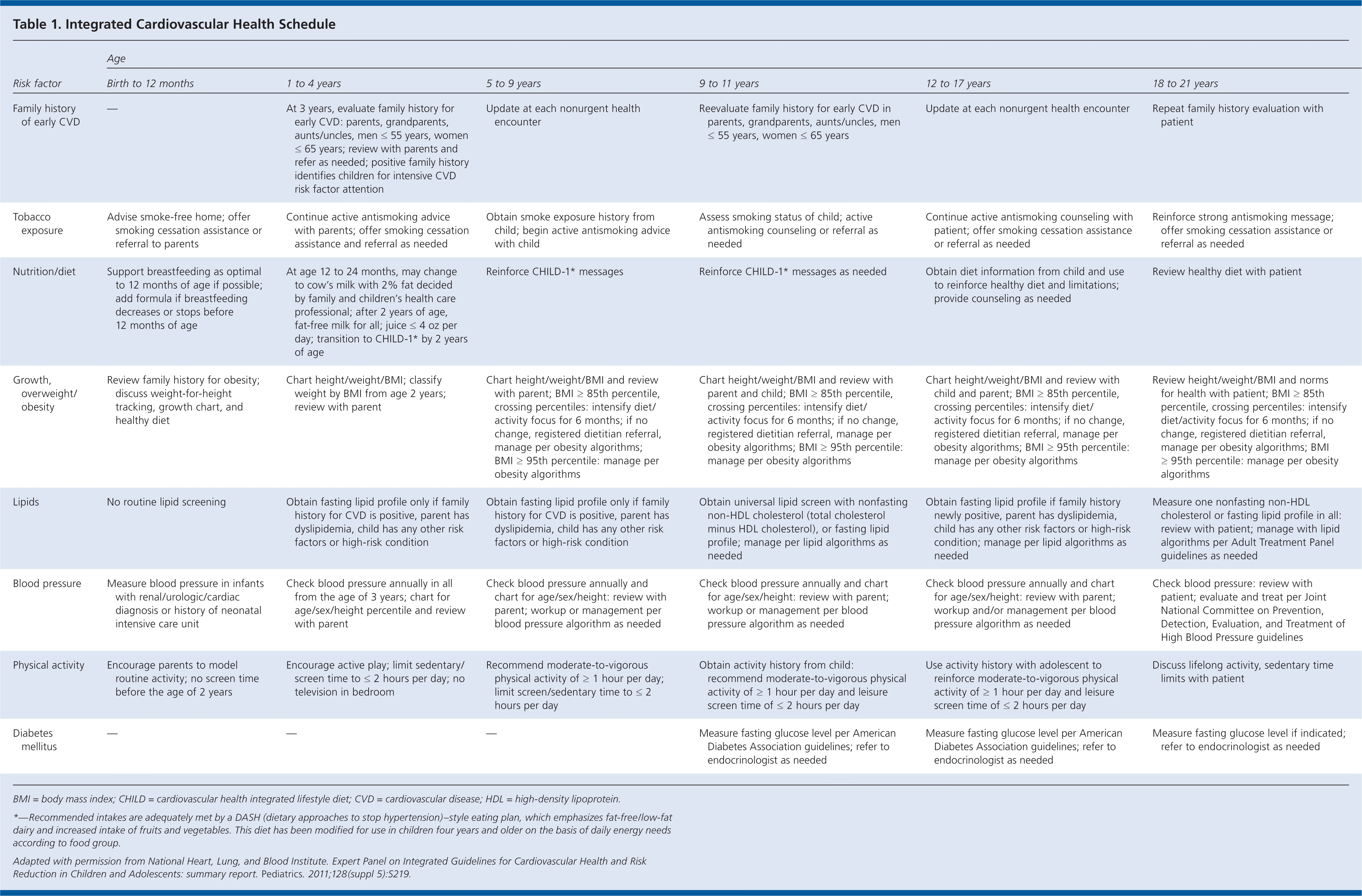
Table 1 provides the integrated cardiovascular health schedule.
Table 1. Integrated Cardiovascular Health Schedule
| Risk factor | Age | |||||
|---|---|---|---|---|---|---|
| Birth to 12 months | 1 to 4 years | 5 to 9 years | 9 to 11 years | 12 to 17 years | 18 to 21 years | |
| Family history of early CVD | — | At 3 years, evaluate family history for early CVD: parents, grandparents, aunts/uncles, men ≤ 55 years, women ≤ 65 years; review with parents and refer as needed; positive family history identifies children for intensive CVD risk factor attention | Update at each nonurgent health encounter | Reevaluate family history for early CVD in parents, grandparents, aunts/uncles, men ≤ 55 years, women ≤ 65 years | Update at each nonurgent health encounter | Repeat family history evaluation with patient |
| Tobacco exposure | Advise smoke-free home; offer smoking cessation assistance or referral to parents | Continue active antismoking advice with parents; offer smoking cessation assistance and referral as needed | Obtain smoke exposure history from child; begin active antismoking advice with child | Assess smoking status of child; active antismoking counseling or referral as needed | Continue active antismoking counseling with patient; offer smoking cessation assistance or referral as needed | Reinforce strong antismoking message; offer smoking cessation assistance or referral as needed |
| Nutrition/diet | Support breastfeeding as optimal to 12 months of age if possible; add formula if breastfeeding decreases or stops before 12 months of age | At age 12 to 24 months, may change to cow's milk with 2% fat decided by family and children's health care professional; after 2 years of age, fat-free milk for all; juice ≤ 4 oz per day; transition to CHILD-1* by 2 years of age | Reinforce CHILD-1* messages | Reinforce CHILD-1* messages as needed | Obtain diet information from child and use to reinforce healthy diet and limitations; provide counseling as needed | Review healthy diet with patient |
| Growth, overweight/obesity | Review family history for obesity; discuss weight-for-height tracking, growth chart, and healthy diet | Chart height/weight/BMI; classify weight by BMI from age 2 years; review with parent | Chart height/weight/BMI and review with parent; BMI ≥ 85th percentile, crossing percentiles: intensify diet/activity focus for 6 months; if no change, registered dietitian referral, manage per obesity algorithms; BMI ≥ 95th percentile: manage per obesity algorithms | Chart height/weight/BMI and review with parent and child; BMI ≥ 85th percentile, crossing percentiles: intensify diet/activity focus for 6 months; if no change, registered dietitian referral, manage per obesity algorithms; BMI ≥ 95th percentile: manage per obesity algorithms | Chart height/weight/BMI and review with child and parent; BMI ≥ 85th percentile, crossing percentiles: intensify diet/activity focus for 6 months; if no change, registered dietitian referral, manage per obesity algorithms; BMI ≥ 95th percentile: manage per obesity algorithms | Review height/weight/BMI and norms for health with patient; BMI ≥ 85th percentile, crossing percentiles: intensify diet/activity focus for 6 months; if no change, registered dietitian referral, manage per obesity algorithms; BMI ≥ 95th percentile: manage per obesity algorithms |
| Lipids | No routine lipid screening | Obtain fasting lipid profile only if family history for CVD is positive, parent has dyslipidemia, child has any other risk factors or high-risk condition | Obtain fasting lipid profile only if family history for CVD is positive, parent has dyslipidemia, child has any other risk factors or high-risk condition | Obtain universal lipid screen with nonfasting non-HDL cholesterol (total cholesterol minus HDL cholesterol), or fasting lipid profile; manage per lipid algorithms as needed | Obtain fasting lipid profile if family history newly positive, parent has dyslipidemia, child has any other risk factors or high-risk condition; manage per lipid algorithms as needed | Measure one nonfasting non-HDL cholesterol or fasting lipid profile in all: review with patient; manage with lipid algorithms per Adult Treatment Panel guidelines as needed |
| Blood pressure | Measure blood pressure in infants with renal/urologic/cardiac diagnosis or history of neonatal intensive care unit | Check blood pressure annually in all from the age of 3 years; chart for age/sex/height percentile and review with parent | Check blood pressure annually and chart for age/sex/height: review with parent; workup or management per blood pressure algorithm as needed | Check blood pressure annually and chart for age/sex/height: review with parent; workup or management per blood pressure algorithm as needed | Check blood pressure annually and chart for age/sex/height: review with parent; workup and/or management per blood pressure algorithm as needed | Check blood pressure: review with patient; evaluate and treat per Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure guidelines |
| Physical activity | Encourage parents to model routine activity; no screen time before the age of 2 years | Encourage active play; limit sedentary/screen time to ≤ 2 hours per day; no television in bedroom | Recommend moderate-to-vigorous physical activity of ≥ 1 hour per day; limit screen/sedentary time to ≤ 2 hours per day | Obtain activity history from child: recommend moderate-to-vigorous physical activity of ≥ 1 hour per day and leisure screen time of ≤ 2 hours per day | Use activity history with adolescent to reinforce moderate-to-vigorous physical activity of ≥ 1 hour per day and leisure screen time of ≤ 2 hours per day | Discuss lifelong activity, sedentary time limits with patient |
| Diabetes mellitus | — | — | — | Measure fasting glucose level per American Diabetes Association guidelines; refer to endocrinologist as needed | Measure fasting glucose level per American Diabetes Association guidelines; refer to endocrinologist as needed | Measure fasting glucose level if indicated; refer to endocrinologist as needed |
BMI = body mass index; CHILD = cardiovascular health integrated lifestyle diet; CVD = cardiovascular disease; HDL = high-density lipoprotein.
*—Recommended intakes are adequately met by a DASH (dietary approaches to stop hypertension)–style eating plan, which emphasizes fat-free/low-fat dairy and increased intake of fruits and vegetables. This diet has been modified for use in children four years and older on the basis of daily energy needs according to food group.
Adapted with permission from National Heart, Lung, and Blood Institute. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents: summary report. Pediatrics. 2011;128(suppl 5):S219.
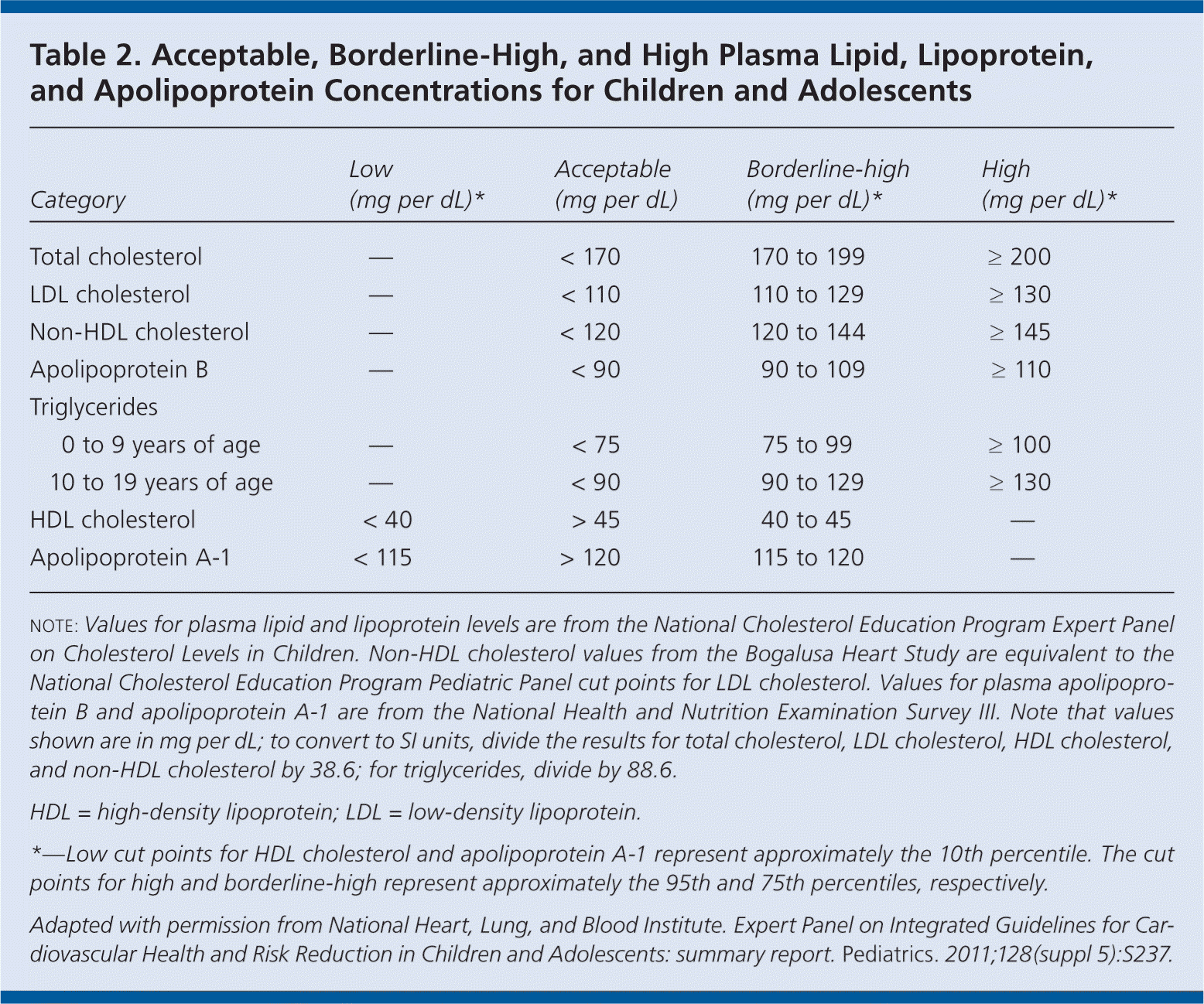
Lipid and lipoprotein levels in childhood are predictive of levels in adulthood, with the strongest relationship occurring between levels in late childhood and at age 20 to 40 years. Table 2 lists normal lipid and lipoprotein distributions in children and adolescents. Total and low-density lipoprotein (LDL) cholesterol levels can decrease by 10 to 20 percent or more during puberty. Based on this, a stable time for lipid evaluation would be 10 years of age, which is before puberty in most children.
Table 2. Acceptable, Borderline-High, and High Plasma Lipid, Lipoprotein, and Apolipoprotein Concentrations for Children and Adolescents
| Category | Low (mg per dL)* | Acceptable (mg per dL) | Borderline-high (mg per dL)* | High (mg per dL)* | |
|---|---|---|---|---|---|
| Total cholesterol | — | < 170 | 170 to 199 | ≥ 200 | |
| LDL cholesterol | — | < 110 | 110 to 129 | ≥ 130 | |
| Non-HDL cholesterol | — | < 120 | 120 to 144 | ≥ 145 | |
| Apolipoprotein B | — | < 90 | 90 to 109 | ≥ 110 | |
| Triglycerides | |||||
| 0 to 9 years of age | — | < 75 | 75 to 99 | ≥ 100 | |
| 10 to 19 years of age | — | < 90 | 90 to 129 | ≥ 130 | |
| HDL cholesterol | < 40 | > 45 | 40 to 45 | — | |
| Apolipoprotein A-1 | < 115 | > 120 | 115 to 120 | — | |
note: Values for plasma lipid and lipoprotein levels are from the National Cholesterol Education Program Expert Panel on Cholesterol Levels in Children. Non-HDL cholesterol values from the Bogalusa Heart Study are equivalent to the National Cholesterol Education Program Pediatric Panel cut points for LDL cholesterol. Values for plasma apolipoprotein B and apolipoprotein A-1 are from the National Health and Nutrition Examination Survey III. Note that values shown are in mg per dL; to convert to SI units, divide the results for total cholesterol, LDL cholesterol, HDL cholesterol, and non-HDL cholesterol by 38.6; for triglycerides, divide by 88.6.
HDL = high-density lipoprotein; LDL = low-density lipoprotein.
*—Low cut points for HDL cholesterol and apolipoprotein A-1 represent approximately the 10th percentile. The cut points for high and borderline-high represent approximately the 95th and 75th percentiles, respectively.
Adapted with permission from National Heart, Lung, and Blood Institute. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents: summary report. Pediatrics. 2011;128(suppl 5):S237.
To reduce total and LDL cholesterol levels, children should eat a diet made up of 25 to 30 percent of calories from fat, with less than 10 percent from saturated fat, and less than 300 mg of cholesterol per day (e.g., CHILD-1 [cardiovascular health integrated lifestyle diet]). Some evidence indicates that this type of diet also reduces total and LDL cholesterol levels if started in infancy and continued through adolescence. A diet that has no more than 7 percent of calories from saturated fat and less than 200 mg of cholesterol per day (CHILD-2-LDL) has been shown to decrease LDL cholesterol levels in children diagnosed with hypercholesterolemia and an elevated LDL cholesterol level. Table 3 briefly summarizes the various recommended diets.
Table 3. Evidence-Based Recommendations for Pharmacologic Treatment of Dyslipidemia

| Age | Recommendation | Grade and recommendation levels | ||||
|---|---|---|---|---|---|---|
| Birth to 10 years | Pharmacologic treatment is limited to children with severe primary hyperlipidemia (homozygous familial hypercholesterolemia, primary hypertriglyceridemia*), a high-risk condition, or evident cardiovascular disease, all under the care of a lipid specialist | C; recommend | ||||
| ≥ 10 to21 years | Detailed family history and risk factor assessment required before initiation of drug therapy† | C; strongly recommend | ||||
| LDL cholesterol: | ||||||
| B; strongly recommend | |||||
| A; strongly recommend | ||||||
| Repeat fasting lipid profile: | ||||||
| A; strongly recommend | |||||
| A; strongly recommend | |||||
| B; recommend | |||||
| B; recommend | |||||
| B; recommend | |||||
| A; strongly recommend | |||||
| ≥ 10 to 21 years | Detailed family history and risk factor/condition assessment required before initiation of drug therapy†¶ | C; strongly recommend | ||||
| Triglycerides: | ||||||
| B; recommend | |||||
| B; recommend | ||||||
| Repeat fasting lipid profile: | ||||||
| B; strongly recommend | |||||
| C; recommend | |||||
| D; recommend | |||||
| Non-HDL cholesterol: | ||||||
| D; optional | |||||
note: Grades reflect the findings of the evidence review, and recommendation levels reflect the consensus opinion of the expert panel. When medication is recommended, it should always be in the context of the complete cardiovascular risk profile of the patient and in consultation with the patient and the family.
Evidence grading system:
A = Well-designed randomized controlled trials or diagnostic studies performed on a population similar to the guideline's target population.
B = Randomized controlled trials or diagnostic studies with minor limitations; genetic natural history studies; overwhelmingly consistent evidence from observational studies.
C = Observational studies (case-control and cohort design).
D = Expert opinion, case reports, or reasoning from first principles (bench research or animal studies).
CHILD = cardiovascular health integrated lifestyle diet; HDL = high-density lipoprotein; LDL = low-density lipoprotein; TG = triglyceride.
*—Triglyceride level ≥ 500 mg per dL.
†—Consideration of drug therapy is based on the average of at least two fasting lipid profiles, obtained at least 2 weeks but no more than 3 months apart.
‡—Recommended intakes are adequately met by a DASH (dietary approaches to stop hypertension)–style eating plan, which emphasizes fat-free/low-fat dairy and increased intake of fruits and vegetables. This diet has been modified for use in children four years and older on the basis of daily energy needs according to food group.
§—For children with elevated LDL cholesterol. Diet consists of 25 to 30 percent of calories from fat, no more than 7 percent from saturated fat, and approximately 10 percent from monounsaturated fat; less than 200 mg per day of cholesterol; and avoidance of trans fats.
||—If average LDL cholesterol ≥ 190 mg per dL after CHILD-2–LDL and child is 8 to 9 years of age with a positive family history or at least one high-level risk factor/condition or at least two moderate-level risk factors/conditions, statin therapy may be considered.
¶—If the child is obese, nutrition therapy should include calorie restriction and increased activity beyond that recommended for all children.
**—For children with elevated triglycerides or non-HDL cholesterol. Diet consists of 25 to 30 percent of calories from fat, no more than 7 percent from saturated fat, and approximately 10 percent from monounsaturated fat; less than 200 mg per day of cholesterol; avoidance of trans fat; decreased sugar intake; and increased fish intake (to increase omega-3 fatty acids).
Adapted with permission from National Heart, Lung, and Blood Institute. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents: summary report. Pediatrics. 2011;128(suppl 5):S244.
In children with familial hypercholesterolemia, up to 20 g per day of a dietary supplement (e.g., plant sterol or stanol esters) can augment LDL cholesterol–lowering effects in the short term. Long-term trials have not been performed; therefore, these types of dietary supplements are typically used only for children in whom LDL cholesterol goals cannot be achieved with dietary therapy alone, with the hope that they may lower LDL cholesterol levels enough to avoid using medication. Consuming a diet with fewer simple carbohydrates (and with more complex carbohydrates and less saturated fat) and losing weight are associated with lower triglyceride levels. Children with elevated triglyceride levels and obesity should eat fewer calories, with the CHILD-2–TG being the recommended diet. It is also important that these children get more physical activity.
Table 3 provides the recommendations for pharmacologic treatment of dyslipidemia.

