A four-year-old boy presented with a pruritic rash on his hands, forearms, and feet that developed one week earlier. He had nonspecific symptoms of an upper respiratory tract infection with rhinorrhea and a subjective fever. He was initially treated with topical steroids, diphenhydramine (Benadryl), and hydroxyzine (Vistaril), but subsequently developed severe swelling, pain, and blistering on his forearms (the right arm was worse than the left).
On examination, the patient was ill-appearing and irritable, but afebrile. He had numerous large (3- to 6-cm) bullae, some with hemorrhage, on both forearms (Figure 1). The bullae were rapidly evolving on an erythematous base. He had diffuse edema on his right forearm extending to his hand with clawing of the fingers. His pulses and sensation were normal. There was no fluctuance or crepitus with palpation. There was a reticular rash on his right upper arm (Figure 2). His feet were mildly edematous with a faint reticular rash.
Figure 1.
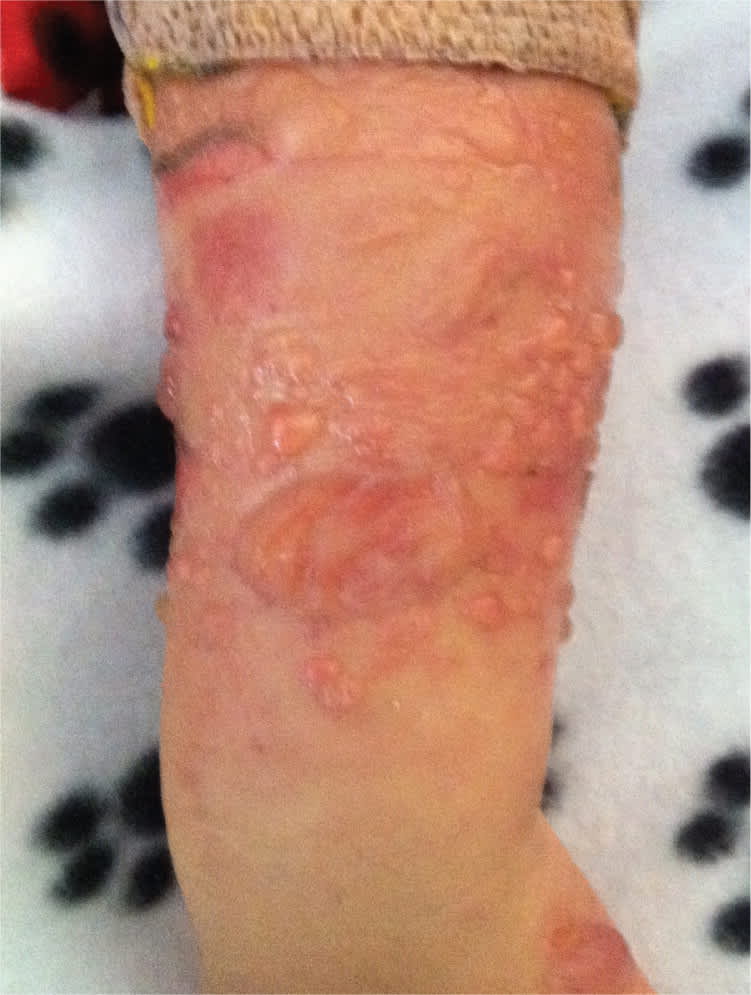
Figure 2.
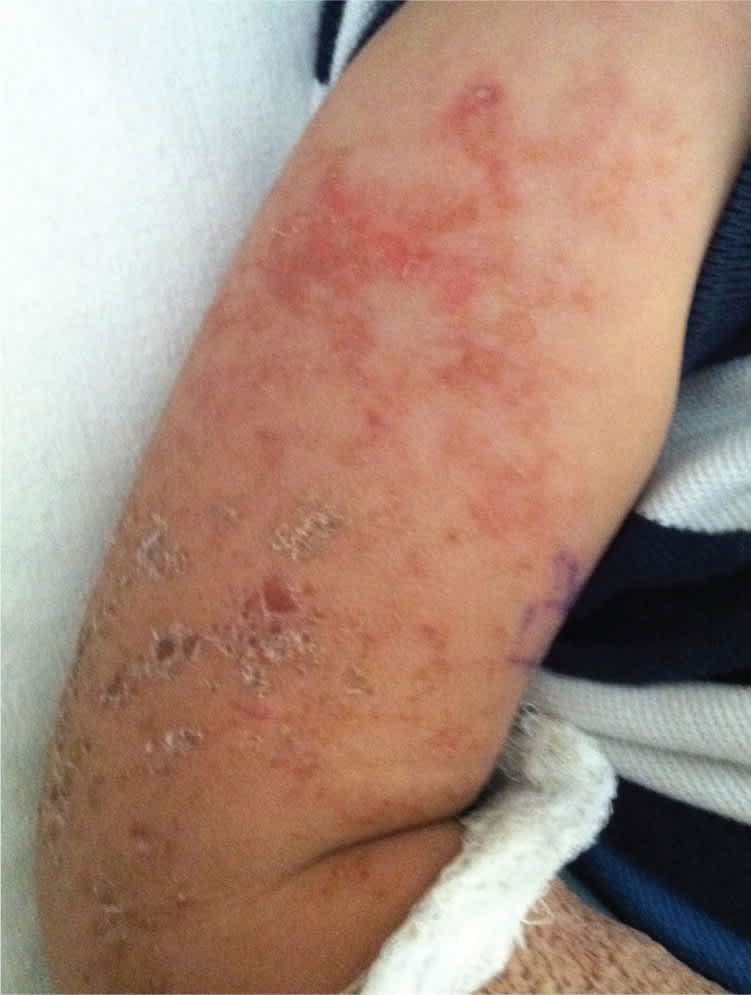
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Compartment syndrome.
B. Contact dermatitis.
C. Juvenile bullous pemphigoid.
D. Necrotizing fasciitis.
E. Parvovirus B19 infection.
Discussion
The answer is E: parvovirus B19 infection. Parvovirus B19 infection (erythema infectiosum) is common in children. It is also associated with papularpurpuric gloves-and-socks syndrome in young adults.
One to four days prior to eruption of the exanthem, patients have a prodromal illness of fever, malaise, rhinorrhea, and nausea. The initial rash is classically described as “slapped cheeks” because it begins as redness of the cheeks. The pruritic rash develops on the distal extremities and evolves into a lacy, reticular appearance.1 In this patient, the edema resulted in bullae formation. Parvovirus B19 infection can also be associated with more serious manifestations including aplastic crisis, arthropathy, chronic pure red cell aplasia, and hydrops fetalis in pregnant women.
The diagnosis of parvovirus B19 infection is made clinically if the pathognomonic slapped cheek rash is present. Serum immunoglobulin M testing can be performed in immunocompetent patients, and viral polymerase chain reaction testing can be performed in immunocompromised patients or in those with transient aplastic crisis. Treatment is usually supportive because the rash is self-limited. However, serious manifestations require medical therapy.
Compartment syndrome occurs after trauma or surgery and is characterized by the six P's: pressure, pain, paresthesia, pallor, paresis, and pulselessness.2
Contact dermatitis may lead to erythema, pruritus, vesicles, and bullae, but no systemic symptoms. Scaling develops in a clearly defined pattern (usually linear).
Juvenile bullous pemphigoid is a rare childhood condition that causes pruritic papules that develop into widespread tense bullae. The rash can be caused by medications or exposure to ultraviolet light. The rash is widespread, but usually affects the face and oral mucosa.3
Necrotizing fasciitis is a serious infection that causes gangrene4 and can lead to rapidly progressing edema, erythema, or necrosis. The rash typically is unilateral and accompanied by systemic symptoms such as fever. On examination, patients have palpable crepitus in the affected areas.
Summary Table
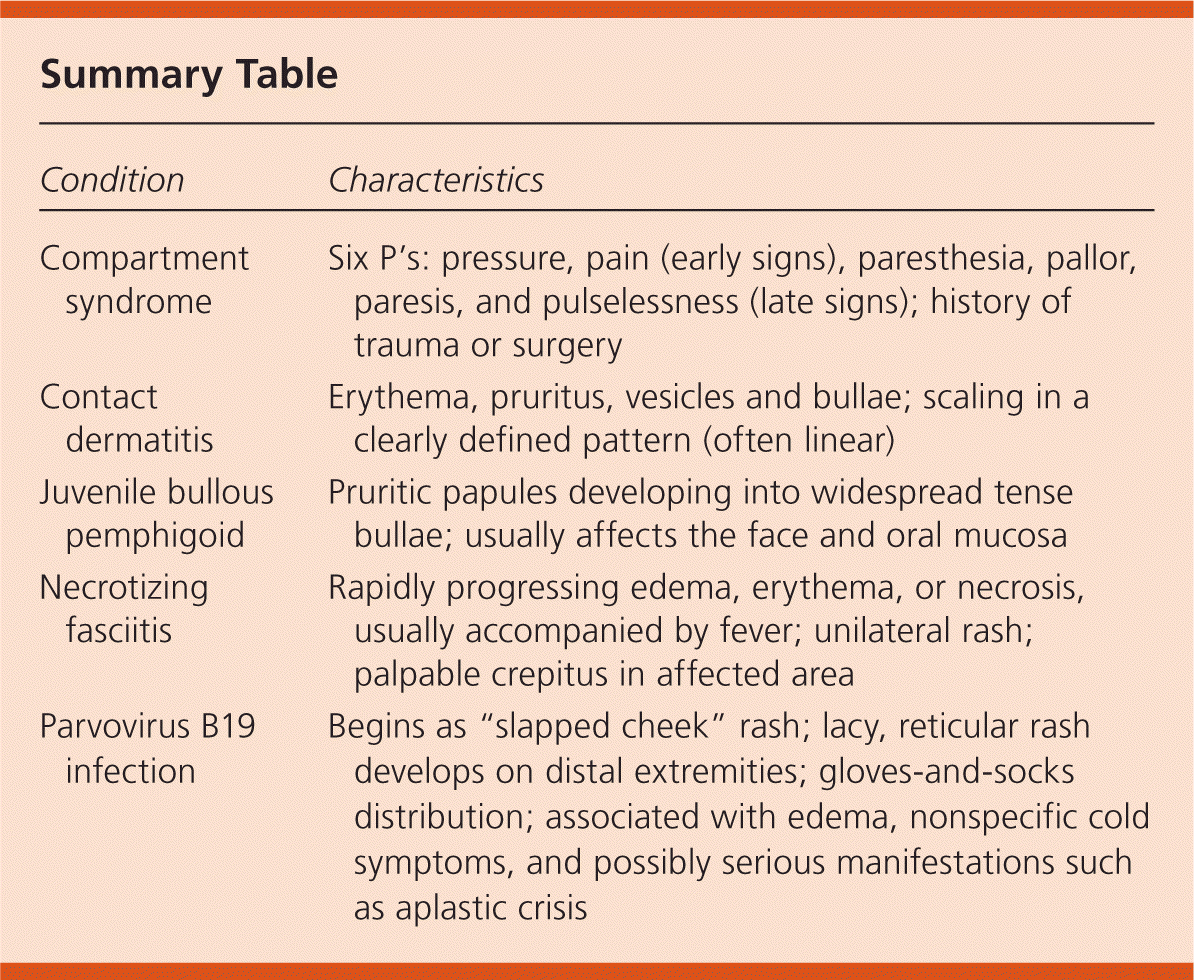
| Condition | Characteristics |
|---|---|
| Compartment syndrome | Six P's: pressure, pain (early signs), paresthesia, pallor, paresis, and pulselessness (late signs); history of trauma or surgery |
| Contact dermatitis | Erythema, pruritus, vesicles and bullae; scaling in a clearly defined pattern (often linear) |
| Juvenile bullous pemphigoid | Pruritic papules developing into widespread tense bullae; usually affects the face and oral mucosa |
| Necrotizing fasciitis | Rapidly progressing edema, erythema, or necrosis, usually accompanied by fever; unilateral rash; palpable crepitus in affected area |
| Parvovirus B19 infection | Begins as “slapped cheek” rash; lacy, reticular rash develops on distal extremities; gloves-and-socks distribution; associated with edema, nonspecific cold symptoms, and possibly serious manifestations such as aplastic crisis |

