A 63-year-old man presented with an asymptomatic rash that began four days earlier, one day after he was treated for an abscess on his right abdomen. The abscess was treated by incision and drainage, and he was prescribed trimethoprim/sulfamethoxazole because he had a history of methicillin-resistant Staphylococcus aureus infection.
Physical examination revealed multiple large, erythematous, sharply demarcated circular plaques, some with tense bullae in the center, on his trunk and extremities (Figures 1 and 2). There was no mucosal involvement.
Figure 1.
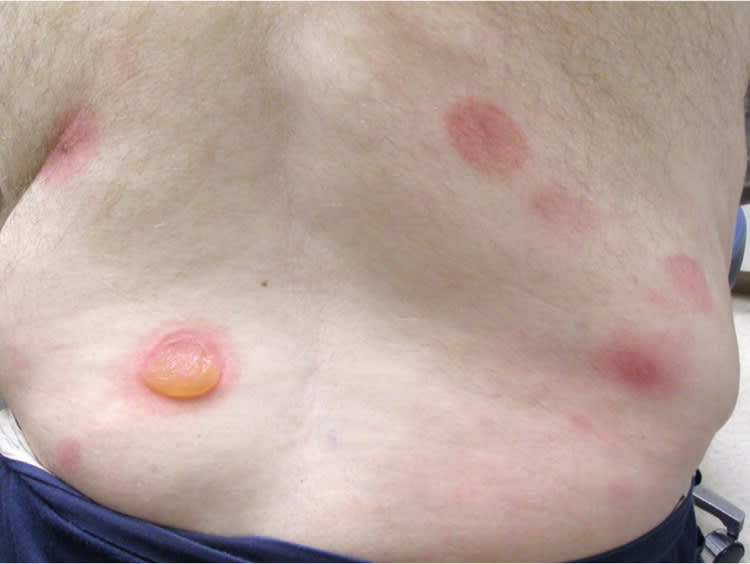
Figure 2.
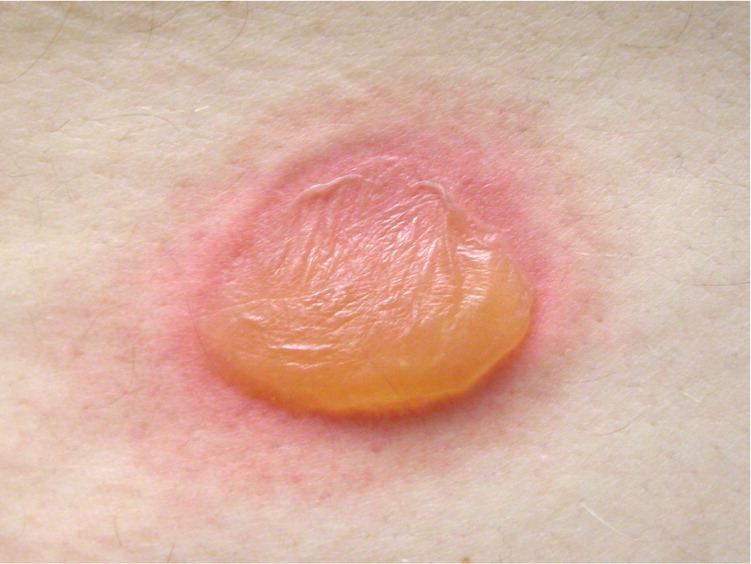
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
A. Bullous impetigo.
B. Bullous pemphigoid.
C. Erythema multiforme.
D. Pemphigus vulgaris.
Discussion
The answer is C: erythema multiforme. Erythema multiforme minus is a self-limited hypersensitivity reaction. It most commonly occurs in response to an antecedent herpes simplex virus infection but may also be triggered by medications, including sulfonamides, barbiturates, penicillins, and phenytoin (Dilantin).1–3 Erythema multiforme majus is a more severe form of the condition also known as Stevens-Johnson syndrome. The diagnosis of erythema multiforme is clinical. Lesions may have a target appearance, and usually begin on the distal extremities and progress proximally.3 Vesicles and bullae sometimes form centrally.3
Erythema multiforme usually causes minimal symptoms and resolves over several weeks without treatment.2 Suspected causal medications should be withdrawn as soon as possible. Oral antihistamines or topical steroids may be used for itching.2 A short course of oral corticosteroids may be helpful in severe cases; however, this is controversial.3 Recurrent cases may be treated with antiviral agents or other immunosuppressant drugs.3
Bullous impetigo is caused by toxin-producing staphylococcal strains and is most common in infants and children.2 Vesicles enlarge rapidly to form bullae containing clear or cloudy fluid. The lesions may expand and rupture, leaving a collarette of moist scale and an erythematous base.2 There is typically little to no surrounding erythema. Diagnosis is usually clinical but may require a culture of fluid from the lesion.4
Bullous pemphigoid is an autoimmune disease characterized by tense bullae on an erythematous, urticarial, or noninflammatory base.5 The bullae are commonly pruritic and may be preceded by a prodromal phase with eczematous, papular, or urticarial skin lesions lasting for weeks.6 Diagnosis is made through biopsy of the lesion and perilesional tissue, with subsequent microscopic evaluation using standard histology and direct immunofluorescent techniques.
Pemphigus vulgaris is an autoimmune disease characterized by flaccid blisters on the skin and mucosal surfaces that rupture easily, leaving painful erosions.7 Diagnosis is made through biopsy of the lesion and perilesional tissue.
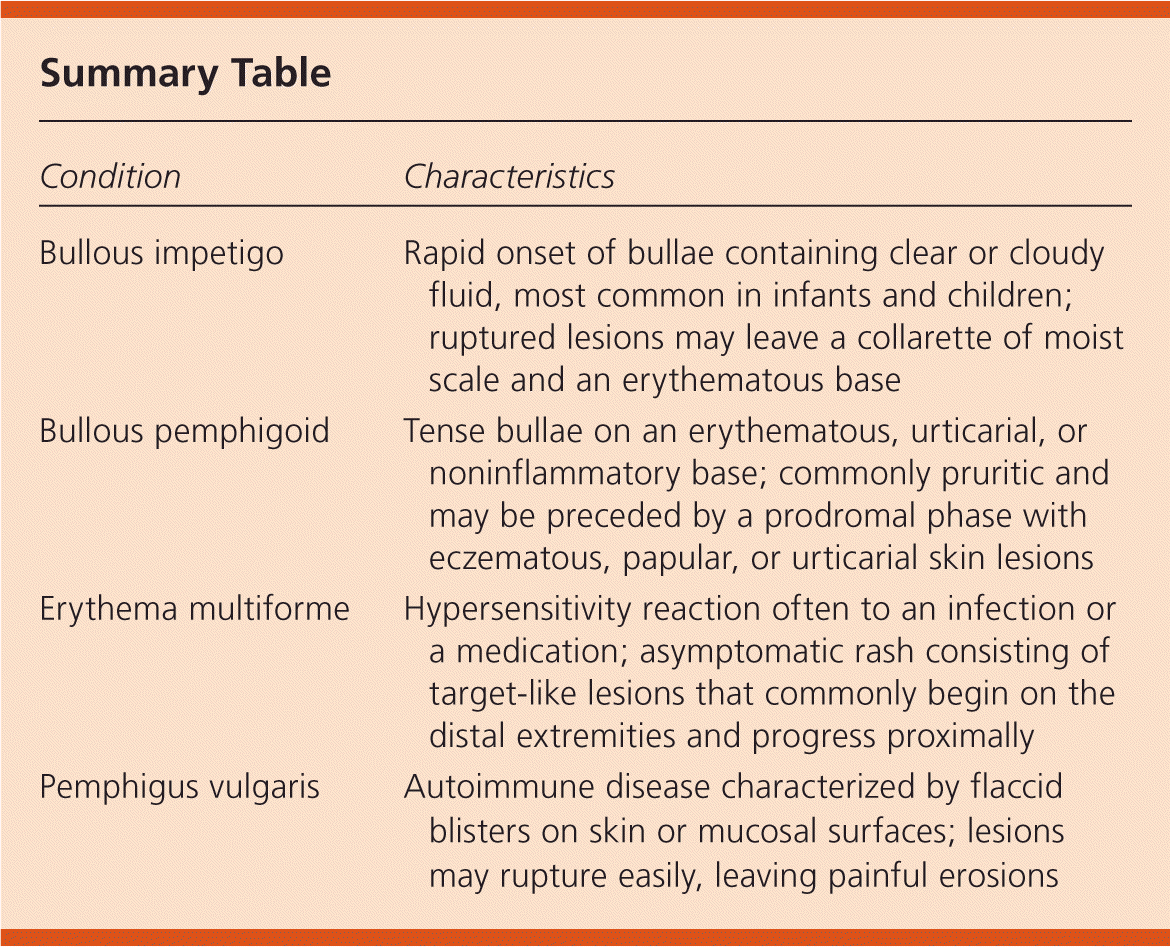
Summary Table
| Condition | Characteristics |
|---|---|
| Bullous impetigo | Rapid onset of bullae containing clear or cloudy fluid, most common in infants and children; ruptured lesions may leave a collarette of moist scale and an erythematous base |
| Bullous pemphigoid | Tense bullae on an erythematous, urticarial, or noninflammatory base; commonly pruritic and may be preceded by a prodromal phase with eczematous, papular, or urticarial skin lesions |
| Erythema multiforme | Hypersensitivity reaction often to an infection or a medication; asymptomatic rash consisting of target-like lesions that commonly begin on the distal extremities and progress proximally |
| Pemphigus vulgaris | Autoimmune disease characterized by flaccid blisters on skin or mucosal surfaces; lesions may rupture easily, leaving painful erosions |

