A 26-year-old man presented with a four-year history of exophytic growths on his back and extensive scarring on his chest. The lesions were flesh colored, nontender, and progressively worsening. His medical history was significant for moderate to severe acne, which required treatment with oral isotretinoin. The lesions gradually developed, extending beyond the borders of inflammatory acne cysts. They significantly affected his appearance and caused severe distress.
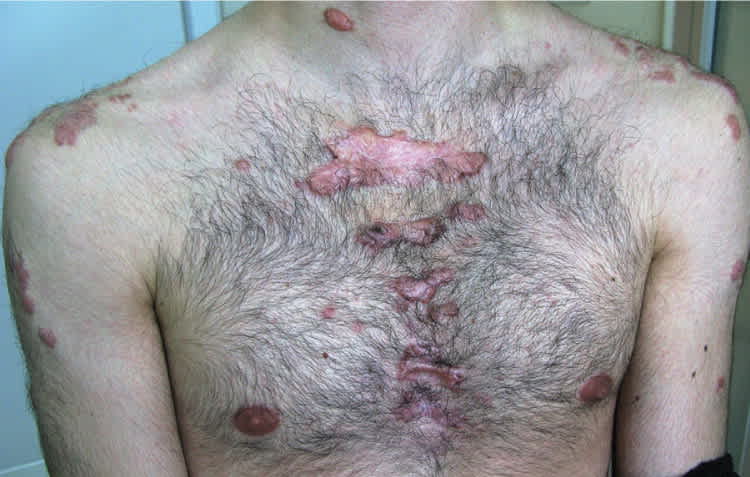
Physical examination revealed multiple oval and round, hypertrophic, nodular tumors on his back (Figure 1). They ranged in size from 2 to 10 cm. On the anterior chest, there were multiple areas of hypertrophic scars (Figure 2).
Figure 1.

Figure 2.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Cutaneous T-cell lymphoma (mycosis fungoides tumors).
B. Lepromatous leprosy.
C. Lobomycosis.
D. Neurofibromatosis 1.
E. Postacne keloids.
Discussion
The correct answer is E: postacne keloids. Keloids are common, benign, flesh-colored dermal tumors that occur during the process of wound healing. They are characterized by excess deposition of collagen and have varying degrees of clinical severity. Keloids and hypertrophic scars are a variation of normal wound healing. Keloids extend beyond the borders of the original trauma and do not spontaneously regress, whereas hypertrophic scars are confined to the borders of the inciting injury, retaining its shape.1 Both can develop after trauma to the deep dermis.
There is no standardized evidence-based treatment for keloids. Preventing them by avoiding unnecessary surgery in patients who are prone to keloids is the most effective approach. Treatment modalities offer minimal improvement, and lesions can recur. This patient was treated unsuccessfully with topical imiquimod (Aldara), cryosurgery in combination with intralesional corticosteroid injections, and excisional surgery.
Cutaneous T-cell lymphoma is a type of non-Hodgkin lymphoma characterized by the presence of neoplastic T lymphocytes in the skin. The two most common types are mycosis fungoides and Sézary syndrome.2 Mycosis fungoides has three stages: patch (atrophic or nonatrophic), plaque, and tumor. The tumors are red, purple, or brown nodules with a smooth surface. They are dome shaped and exophytic, and have a predilection for the face and body folds. The growth rate varies, and they may become ulcerated.
Leprosy is a chronic granulomatous disease caused by Mycobacterium leprae. In lepromatous leprosy, there is a lack of cell-mediated immunity toward M. leprae, which allows dissemination of the infection. Early cutaneous lesions are pale macules with little or no loss of sensation. Later lesions (lepromas) are poorly defined, symmetrically distributed, flesh-colored nodules.3 Leonine facies, a deeply furrowed face with thickened skin, is a classic presentation in leprosy. There is no clinical inflammation. Loss of eyebrow hair is common.
Lobomycosis, also known as Lobo disease or lacaziosis, is a chronic, self-limited, cutaneous fungal infection. It was first reported as keloidal blastomycosis4 and is endemic in rural regions of South and Central America. It is characterized by slow-growing, keloid-like lesions on exposed skin accompanied by pruritus or a burning sensation. The lesions may begin as small papules, plaques, or pustules at sites of minor trauma.5
Neurofibromatosis 1, or von Recklinghausen disease, is an autosomal dominant condition that accounts for 90% of neurofibromatosis cases.6 It is characterized by peripheral or central nervous system neoplasms, pigmented iris hamartomas (Lisch nodules), and various skin lesions such as multiple neurofibromas, café au lait spots, and axillary and inguinal freckling.
Summary Table
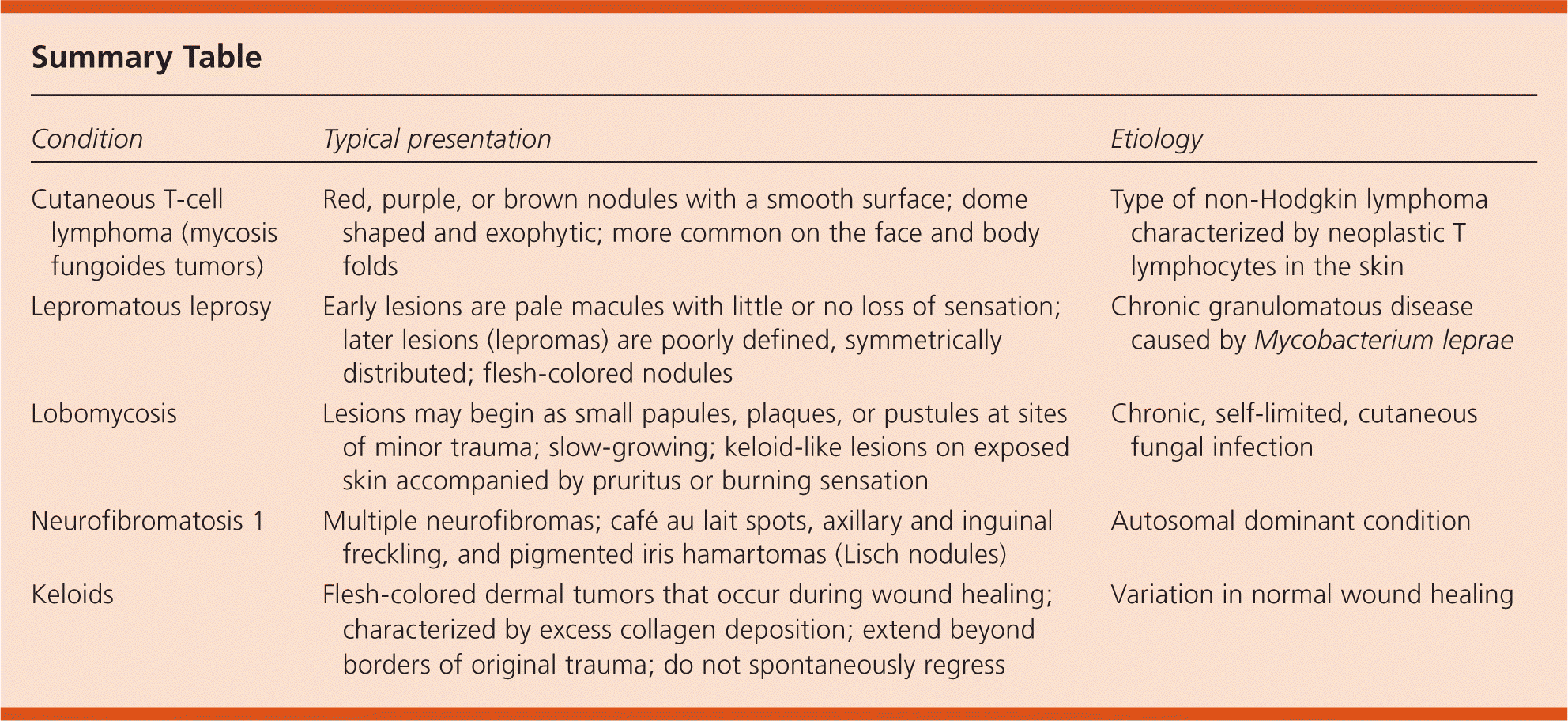
| Condition | Typical presentation | Etiology |
|---|---|---|
| Cutaneous T-cell lymphoma (mycosis fungoides tumors) | Red, purple, or brown nodules with a smooth surface; dome shaped and exophytic; more common on the face and body folds | Type of non-Hodgkin lymphoma characterized by neoplastic T lymphocytes in the skin |
| Lepromatous leprosy | Early lesions are pale macules with little or no loss of sensation; later lesions (lepromas) are poorly defined, symmetrically distributed; flesh-colored nodules | Chronic granulomatous disease caused by Mycobacterium leprae |
| Lobomycosis | Lesions may begin as small papules, plaques, or pustules at sites of minor trauma; slow-growing; keloid-like lesions on exposed skin accompanied by pruritus or burning sensation | Chronic, self-limited, cutaneous fungal infection |
| Neurofibromatosis 1 | Multiple neurofibromas; café au lait spots, axillary and inguinal freckling, and pigmented iris hamartomas (Lisch nodules) | Autosomal dominant condition |
| Keloids | Flesh-colored dermal tumors that occur during wound healing; characterized by excess collagen deposition; extend beyond borders of original trauma; do not spontaneously regress | Variation in normal wound healing |

