A 42-year-old man with a history of basal cell carcinoma on his scalp (five years earlier) presented for an annual examination. He reported inconsistent sunscreen use and did not have any new or concerning lesions. He did have a papule on his upper lip that had not changed in shape, size, or color since he first noticed it 10 years earlier. He had nicked it many times while shaving.
Physical examination revealed a solitary, 3.5-mm, skin-colored, dome-shaped, non-tender, firm papule (Figures 1 and 2). On dermoscopy, there was prominent telangiectasia and loss of skin markings within the papule, and no evidence of a pigment network or hair growth.
Figure 1.
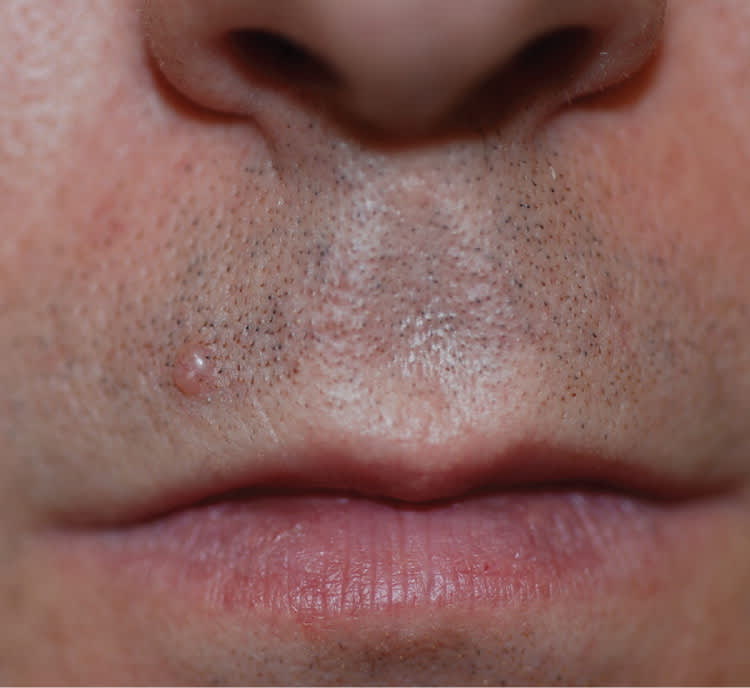
Figure 2.
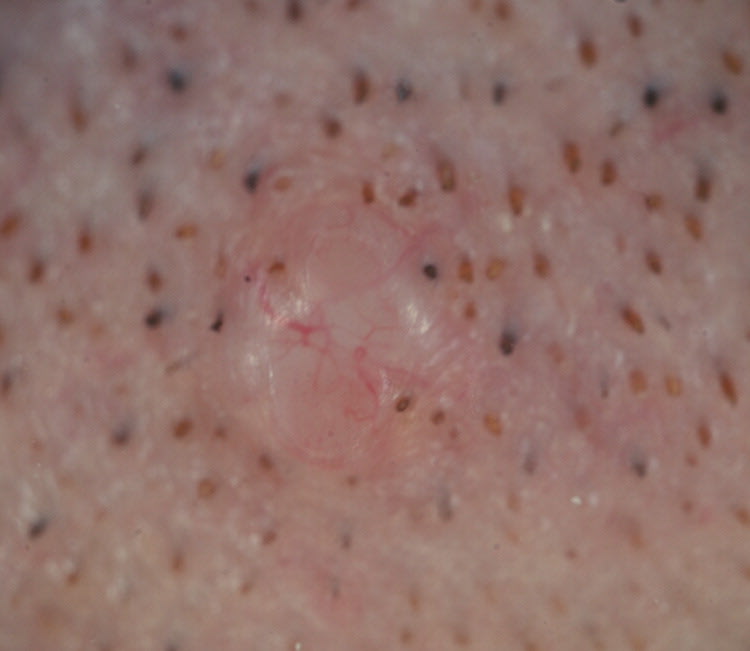
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Basal cell carcinoma.
B. Epidermal inclusion cyst.
C. Intradermal melanocytic nevus.
D. Neurofibroma.
E. Palisaded encapsulated neuroma.
Discussion
The answer is E: palisaded encapsulated neuroma, also known as a solitary circumscribed neuroma. This is a common benign neural tumor that may be misdiagnosed as a carcinoma.1 It presents as a small (2 to 6 mm), asymptomatic, skin-colored, firm, dome-shaped papule. It most often occurs on the mucocutaneous junction of the face in patients between 40 and 60 years of age. Men and women are equally affected.2
Palisaded encapsulated neuromas usually have no hair on the surface and minimal or absent telangiectasia; however, trauma to the area can cause prominent telangiectatic vessels and ulceration.2 Histologically, these neuromas appear as a partially encapsulated dermal nodule. The cause is unknown, but it has been suggested that they are a trauma-induced hyperplasia of the nerve fibers.3 Excision is typically curative.4
The most common form of basal cell carcinoma presents as a dome-shaped papule or nodule that may ulcerate and bleed. The raised, rolled, pearly borders can be accentuated by applying traction to the surrounding skin.5 Telangiectasia forms an arboreal pattern on dermoscopy.6
An epidermal inclusion cyst usually presents as a 1- to 4-cm, solitary, firm, mobile, subcutaneous nodule on the trunk, neck, or face. A white, cheesy material (accumulated keratin debris) can be expressed from the cyst with a surface punctum.7
An intradermal melanocytic nevus is a benign lesion that may or may not be pigmented. It is usually soft with smooth edges and retains skin markings.8 Brown pigment, comma-shaped vessels, and hair are often noted on dermoscopy.9
A solitary neurofibroma presents as a soft sessile or pedunculated papule, usually on the trunk, that invaginates with pressure (“buttonholing”).5 Multiple neurofibromas are associated with von Recklinghausen disease, or neurofibromatosis 1. Other clinical features include café au lait spots, axillary freckling, and iris hamartomas (Lisch nodules).
Summary Table
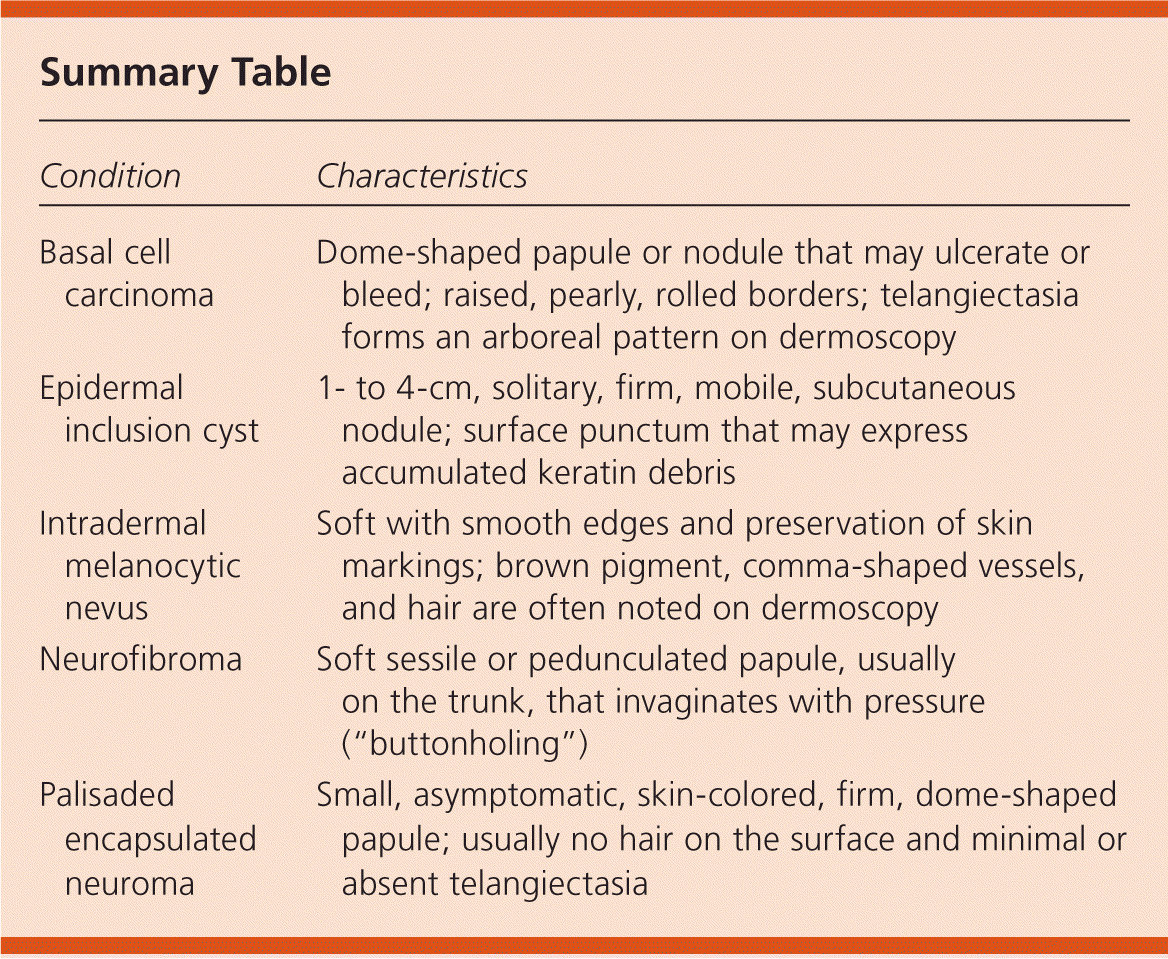
| Condition | Characteristics |
|---|---|
| Basal cell carcinoma | Dome-shaped papule or nodule that may ulcerate or bleed; raised, pearly, rolled borders; telangiectasia forms an arboreal pattern on dermoscopy |
| Epidermal inclusion cyst | 1- to 4-cm, solitary, firm, mobile, subcutaneous nodule; surface punctum that may express accumulated keratin debris |
| Intradermal melanocytic nevus | Soft with smooth edges and preservation of skin markings; brown pigment, comma-shaped vessels, and hair are often noted on dermoscopy |
| Neurofibroma | Soft sessile or pedunculated papule, usually on the trunk, that invaginates with pressure (“buttonholing”) |
| Palisaded encapsulated neuroma | Small, asymptomatic, skin-colored, firm, dome-shaped papule; usually no hair on the surface and minimal or absent telangiectasia |

